Académique Documents
Professionnel Documents
Culture Documents
SF-36 QUESTIONNAIRE Bariatric Vaznooo
Transféré par
Dusan OrescaninCopyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
SF-36 QUESTIONNAIRE Bariatric Vaznooo
Transféré par
Dusan OrescaninDroits d'auteur :
Formats disponibles
J Appl Physiol 119: 37–46, 2015.
First published April 30, 2015; doi:10.1152/japplphysiol.00092.2015.
Females have a blunted cardiovascular response to one year
of intensive supervised endurance training
Erin J. Howden,1,2 Merja Perhonen,1 Ronald M. Peshock,2 Rong Zhang,1,2 Armin Arbab-Zadeh,1
Beverley Adams-Huet,2 and Benjamin D. Levine1,2
1
Institute for Exercise and Environmental Medicine, Dallas, Texas; and 2University of Texas Southwestern Medical Center,
Dallas, Texas
Submitted 4 February 2015; accepted in final form 23 April 2015
Howden EJ, Perhonen M, Peshock RM, Zhang R, Arbab- studies of endurance athletes suggest that females have a lower
Zadeh A, Adams-Huet B, Levine BD. Females have a blunted maximal oxygen uptake (V̇O2max) and cardiac output (Qc) and
cardiovascular response to one year of intensive supervised endurance smaller left ventricular (LV) dimensions and wall thickness
training. J Appl Physiol 119: 37– 46, 2015. First published April 30,
compared with similar male athletes (12, 34, 40). Confounding
2015; doi:10.1152/japplphysiol.00092.2015.—Cross-sectional studies
in athletes suggest that endurance training augments cardiovascular the interpretation of sex differences is the effect that body size
structure and function with apparently different phenotypes in athletic has on cardiovascular anatomic and physiological variables
(11). Typically studies have scaled cardiovascular variables to
Downloaded from http://jap.physiology.org/ by 10.220.33.1 on October 30, 2017
males and females. It is unclear whether the longitudinal response to
endurance training leads to similar cardiovascular adaptations be- body size or lean body mass, which eliminates some, but not
tween sexes. We sought to determine whether males and females all, of the differences between sexes.
demonstrate similar cardiovascular adaptations to 1 yr of endurance Cross-sectional studies are also limited by the different
training, matched for training volume and intensity. Twelve previ- sports played by male and female athletes and different training
ously sedentary males (26 ⫾ 7, n ⫽ 7) and females (31 ⫾ 6, n ⫽ 5)
completed 1 yr of progressive endurance training. All participants
performed, which may alter the magnitude of the effect on the
underwent a battery of tests every 3 mo to determine maximal oxygen cardiovascular adaptations observed. Longitudinal studies
uptake (V̇O2max) and left ventricle (LV) function and morphology comparing the cardiovascular response in males and females
(cardiac magnetic resonance imaging). Pulmonary artery catheteriza- with a comparable endurance training program is lacking.
tion was performed before and after 1 yr of training, and pressure- We have recently demonstrated in previously sedentary
volume and Starling curves were constructed during decreases (lower- young subjects that 1 yr of intensive endurance training in-
body negative pressure) and increases (saline infusion) in cardiac creases cardiac mass to levels similar to elite endurance ath-
volume. Males progressively increased V̇O2max, LV mass, and mean letes, results in favorable cardiac remodeling, and improves LV
wall thickness, before reaching a plateau from month 9 to 12 of
training. In contrast, despite exactly the same training, the response in
compliance (3). In this secondary analysis of the same study,
females was markedly blunted, with V̇O2max, LV mass, and mean wall we sought to determine whether males and females demon-
thickness plateauing after only 3 mo of training. The response of LV strate similar cardiovascular adaptations to 1 yr of endurance
end-diastolic volume was not influenced by sex (males ⫹20% and training, matched for training volume and intensity. We hy-
females ⫹18%). After training Starling curves were shifted upward pothesized that the response to training would be similar in
and left, but the effect was greatest in males (interaction P ⫽ 0.06). males and females, evidenced by a similar change in V̇O2max,
We demonstrate for the first time clear sex differences in response to cardiac morphology, and function in response to training. To
1 yr of matched endurance training, such that the development of test this hypothesis, we prescribed a progressive training plan,
ventricular hypertrophy and increase in V̇O2max in females is markedly
blunted compared with males. identical between males and females, based on a strategy
derived from optimal training by competitive athletes; this
cardiac magnetic resonance imaging; exercise training; gender study design allowed us to collect time-dependent measures of
metabolic and LV structure parameters in response to 1 yr of
REGULAR EXERCISE TRAINING leads to changes in the structure and training.
function of cardiac and skeletal muscle, which is fundamen-
tally influenced by the type of exercise performed (endurance METHODS
vs. strength training) (36). Physiological skeletal muscle hy- Subjects
pertrophy is associated with strength training, whereas endur-
ance training is a more potent stimulus to induce physiological This study is a secondary analysis of 12 healthy previously seden-
cardiac hypertrophy. Clear sex differences are observed be- tary males (n ⫽ 7) and females (n ⫽ 5), who completed 1 yr of
tween strength-trained athletes, such that males demonstrate a intensive endurance training. The primary findings from this study
greater magnitude of skeletal muscle mass compared with have been published recently (3). One subject completed all of the
females (1), primarily due to the profound anabolic effect of initial testing but became pregnant in the second quarter of training
testosterone on protein synthesis within the skeletal muscle (9). and was excluded from the study. Participants were not eligible for the
study if they had engaged in any regular endurance training defined as
It is less clear whether the cardiovascular response to en-
⬎30 min/day more than three times per week. All participants were
durance training is also influenced by sex. Cross-sectional carefully screened and underwent a physical examination, electrocar-
diogram (ECG), and echocardiogram. None of the subjects smoked,
Address for reprint requests and other correspondence: B. D. Levine, used recreational drugs, or had significant chronic medical problems.
Institute for Exercise and Environmental Medicine, 7232 Greenville Ave., Ste. All female subjects were eumenorrheic when they commenced train-
435, Dallas, TX 75321 (e-mail: BenjaminLevine@Texashealth.org). ing and remained so for the duration of the study.
http://www.jappl.org 8750-7587/15 Copyright © 2015 the American Physiological Society 37
38 Sex Differences in Response to Endurance Training • Howden EJ et al.
Ethical Approval
3200 Males
Females
All subjects signed an informed consent, which was approved by
Monthly TRIMP, arbitary units
the Institutional Review Boards of the University of Texas South- 2800
western Medical Center at Dallas and Texas Health Resources Pres-
2400
byterian Hospital of Dallas.
2000
Exercise Training
1600
Endurance training was designed to enable subjects to complete a
marathon at the end of the 1-yr period. All subjects performed an 1200
incremental treadmill test for determination of V̇O2max at baseline and
every 3 mo to document exercise performance and for optimal 800
training prescription. A detailed description of the exercise interven-
tion has been previously described (3, 18). Training zones for optimal 400
training prescription were individualized by heart rate (HR) and 0
0 1 2 3 4 5 6 7 8 9 10 11 12 13 14
lactate response to incremental treadmill exercise. “Maximal steady
Month of Training
state” was first estimated from the ventilatory and lactate threshold
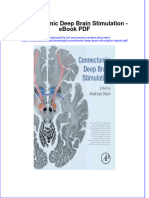
according to standard criteria (18). The HR at maximal steady state Fig. 1. Average training impulse (TRIMP) scores per month in males and
and maximum HR were then used to calculate training zones for each females. Individual sex values are presented as means ⫾ SD.
Downloaded from http://jap.physiology.org/ by 10.220.33.1 on October 30, 2017
subject; five training zones were determined for individualized train-
ing prescription as follows: zone 1, recovery, zone 2, base pace, zone
3, maximal steady state or “threshold,” zone 4, race pace/critical Study Protocol
power, and zone 5, intervals. During the early phase of the training
program, the subjects trained three to four times per week for 30-45 All measurements were performed before training (baseline) and
min/session at base pace by brisk walking, slow jogging, swimming, repeated after 3, 6, 9, and 12 mo of training. Pressure/volume studies
or cycling. As subjects became fitter, the duration of the base training were completed pre- and posttraining.
sessions was prolonged, including the addition of one long run per Exercise Testing
week, which was performed at the lower end of base pace HR range.
In addition, during the second and third quarters of the training A modified Astrand-Saltin incremental treadmill protocol (individ-
program, sessions of increased intensity (maximal steady-state and ualized treadmill speed, with changes in grade of 2% every 2 min) was
interval sessions) were added first one time and then two times and used to determine maximal exercise capacity. Measures of ventilatory
occasionally three times per week. Interval sessions were followed the gas exchange were made by use of the Douglas bag technique. Gas
next day by a recovery session to maximize performance gains. By the fractions were analyzed by mass spectrometry (Marquette MGA
end of the year-long training program, subjects were exercising for 1100), and ventilatory volume was measured by a dry-gas meter
7–9 h/wk, including long runs of up to 3 h, plus regular interval (Collins). V̇O2max was defined as the highest oxygen uptake measured
sessions on the track and races. The purpose of this template was to from ⱖ40 s Douglas bag. In nearly all cases, a plateau in V̇O2 was
maximize training efficiency and to provide a periodization of the observed with increasing work rate, confirming the achievement of
training program. This strategy of varying intensity and duration of V̇O2max. Qc was measured with the acetylene rebreathing method,
training session within any given week (microcycles) applying peri- which has been previously validated in this laboratory (19). HR was
ods of increasing stress followed by recovery from month to month monitored continuously via ECG (Polar). Systemic arteriovenous
(mesocycle) with an ultimate goal of a specific competition (macro- oxygen difference (a-vO2 diff) was calculated from the Fick equation
cycle) is a classic training routine used by competitive athletes and is (a-vO2 diff ⫽ V̇O2/Qc) while stroke volume (SV) was calculated as
widely considered the optimal approach to training (37). Although the Qc/HR. SV and Qc were scaled relative to baseline body surface area
majority of subjects chose to complete a marathon at completion of [stroke index (SI) and cardiac index (QI)] by clinical convention to
the intervention, one female subject completed a 100-mile endurance reduce the confounding effect of body size and composition (11).
cycling race, and one male subject completed an Olympic distance Body Composition
triathlon. We followed the principles of training specificity; thus, the
subjects completing the marathon performed predominantly running Body density and composition were determined by underwater
and the cyclist cycled while the triathlete performed a combination of weighing with correction for residual lung volume (41). Each partic-
swimming, cycling, and running. ipant performed at least three adequate measurements defined as a
HR was recorded during each training session using a HR monitor definite plateau in underwater weight, and the mean value was
provided to each participant. This approach was an important aspect calculated.
of the study and gave us the ability to match and quantify training load
Plasma, Blood Volume, and Hematocrit
throughout the intervention. To quantify the training stimulus, we
calculated the training impulse (“TRIMP”) (5). This method multi- At baseline and at each quarter testing session, all subjects under-
plies the duration of a training session by the average HR achieved went measurement of plasma volume using Evans Blue dye indicator
during that session, weighted for exercise intensity as a function of dilution technique. The methods from this technique have been
HR reserve. With the use of this method, exercise sessions of longer published (14). Briefly, individuals rested in the supine position for at
duration and/or greater intensity such as interval workouts are as- least 30 min after which a known quantity of Evans Blue dye was
signed relatively higher TRIMP values (higher HR and higher weight- injected through a peripheral intravenous catheter, and venous blood
ing factor) than sessions of shorter duration and/or lower intensity. was drawn at 10, 20, and 30 min after injection for the measurement
The average TRIMP for the male and female subjects is presented in of absorbance at 620 and 740 nm via spectrophotometry (DU 600;
Fig. 1. Note the oscillations in TRIMP score throughout the training Beckman). Hematocrit was measured via microcapillary centrifuge,
period, i.e., micro- and macrocycles of training in Fig. 1 and the and blood volume was estimated by dividing plasma volume by 1 ⫺
remarkably similar training load between sexes. hematocrit using appropriate corrections for trapped plasma and
J Appl Physiol • doi:10.1152/japplphysiol.00092.2015 • www.jappl.org
Sex Differences in Response to Endurance Training • Howden EJ et al. 39
peripheral sampling. To reduce the confounding effect of body size Data were used to construct Frank-Starling (SV/PCWP) and pres-
and composition on blood volume (11), absolute values were scaled sure-volume (PCWP/LVEDV) curves. For the purpose of the present
relative to total body mass (ml/kg) and fat-free mass (FFM; ml/kg study, we characterized two explicitly different but related mechanical
FFM). properties of the heart during diastole: 1) static stiffness or overall
chamber stiffness referred to as the stiffness constant, S, of the
Cardiac Magnetic Resonance Imaging logarithmic equation describing the pressure-volume curve (see be-
low); and 2) distensibility, which is used to mean the absolute
Cardiac morphometric parameters were assessed by a cardiac LVEDV at a given distending pressure, independent of dP/dV, or S.
magnetic resonance imaging (cMRI) 1.5-tesla Phillips NT MRI Scan- To characterize the LV pressure-volume relation, we modeled the
ner (Phillips Medical Systems, Best, The Netherlands). Short-axis, data in the present experiment according to the equation described by
gradient echo, and cine magnetic resonance imaging (MRI) sequences Nikolic et al. (28):
with a temporal resolution of 39 ms were obtained to calculate
ventricular volumes as previously described (17). Ventricular mass P ⫽ ⫺S ln关共Vm ⫺ V兲 ⁄ (Vm ⫺ Vo)兴
was computed as the difference between epicardial and endocardial
areas multiplied by the density of heart muscle, 1.05 g/ml (21). The where P is PCWP, V is LVEDV, V0 is equilibrium volume or the
Simpson’s rule technique was used to measure LV mass, which has volume at which P ⫽ 0, Vm is the maximal volume obtained by this
been demonstrated to be accurate and reproducible in our laboratory chamber, and S is a stiffness constant that describes the shape of the
(21) and by others (15). curve. In addition, pressure-volume curves were also calculated using the
For LV volumes, the endocardial border of each slice was identified difference between PCWP and right atrial (RA) pressure (PCWP ⫺ RA)
manually at end diastole and end systole, and volumes were counted as an index of transmural filling pressure (8) to assess the contribution of
by summation (31). Mean wall thickness (MWT) for the entire LV, pericardial constraint.
Downloaded from http://jap.physiology.org/ by 10.220.33.1 on October 30, 2017
including the papillary muscle, was calculated as previously described Statistics
(30). For each short-axis slice, the epicardial area (LV chamber plus
myocardial wall) and endocardial area (chamber area) were deter- Continuous data are expressed as means ⫾ SD except for in Figs.
mined using software on the imaging device. The “average” radius for 2–7 in which SE is used. Baseline sex differences were compared with
each area was calculated by approximating the cross section as a circle Student’s t-test. Continuous variables measured over the 12-mo study
and using the equation for the area of a circle (area ⫽ r2). To reduce duration were analyzed longitudinally using linear mixed-effects
the confounding effects of body size and lean mass on LV and right model repeated-measures analysis. The repeated-measures model had
ventricle (RV) mass, measures were scaled to FFM (7). five repeated measurements (time points at baseline and 3, 6, 9, and 12
mo), and the study participant was modeled as a random effect. The
Cardiac Catheterization and Experimental Protocol covariance structure was selected based on Akaike’s Information
Cardiac catheterization was performed at baseline and after the
completion of the training period. Participants were studied in the Table 1. Baseline characteristics, body size and
resting supine position. A 6-Fr balloon-tipped fluid-filled catheter composition, and total blood volume after endurance
(Swan-Ganz; Baxter) was placed using fluoroscopic guidance through training
an antecubital vein in the pulmonary artery. All intracardiac pressures
were referenced to atmospheric pressure with the pressure transducer P Value (sex difference
(Transpac IV; Abbott) zero reading set at 5 cm below the sternal Males Females at baseline)
angle. The wedge position of the catheter tip was confirmed using Age, yr
fluoroscopy, as well as the presence of an appropriate pulmonary Baseline 26 ⫾ 7 31 ⫾ 6 0.21
capillary wedge pressure (PCWP) waveform. The mean PCWP was Height, cm
determined visually at end expiration and was used as an estimation of Baseline 177 ⫾ 2 169 ⫾ 6 0.031
LV end-diastolic pressure. Weight, kg
Qc was measured, and SV was calculated from Qc/HR measured Baseline 78 ⫾ 6 60 ⫾ 3 ⬍0.0001
during rebreathing. Left ventricular end-diastolic volume (LVEDV) 12 Months 77 ⫾ 6 60 ⫾ 4
was measured with two-dimensional echocardiography using standard BSA, m2
Baseline 1.96 ⫾ 0.07 1.67 ⫾ 0.07 0.0006
views and formulas as described by the American Society of Echo-
12 Months 1.93 ⫾ 0.07 1.69 ⫾ 0.08
cardiography (27). Images were obtained with an annular phased- FFM, kg
array transducer using a frequency of 2.5–3.5 MHZ (Interspec Apogee Baseline 62 ⫾ 5 47 ⫾ 5 0.0007
CX) and stored on VCR tapes for off-line analysis by a skilled 12 Months 65 ⫾ 4 50 ⫾ 3**
technician. For calculation of LVEDV for each subject, either the Body fat, %
modified Simpson’s rule method, the area length method, or the bullet Baseline 19 ⫾ 6 23 ⫾ 4 0.270
model (cylinder hemiellipsoid) was chosen on the basis of which 12 Months 15 ⫾ 3* 16 ⫾ 4*
views provided the most optimal endocardial definition (39). The Hematocrit, %
same formula was used for each individual subject throughout the Baseline 44 ⫾ 3 39 ⫾ 3 0.0089
12 Months 42 ⫾ 2** 41 ⫾ 4
study.
TBV, ml/kg
Testing protocol. Resting supine measures (baseline 1) were col- Baseline 66 ⫾ 9 63 ⫾ 4 0.493
lected after ensuring hemodynamic stability (⬃20 min of quiet rest), 12 Months 67 ⫾ 12 67 ⫾ 4*
and then cardiac filling was decreased using lower-body negative TBV, ml/kg FFM
pressure (LBNP) as previously described (26). Measurements of Baseline 82 ⫾ 7 82 ⫾ 8 0.947
PCWP, Qc (and therefore SV), LVEDV, HR, and blood pressure were 12 Months 79 ⫾ 15 80 ⫾ 5
made after 5 min each of ⫺15 and ⫺30 mmHg LBNP. The LBNP was PV, ml/kg
then released. After repeat baseline measurements to confirm a return Baseline 40 ⫾ 5 42 ⫾ 2 0.513
to hemodynamic steady state (usually 20 –30 min), cardiac filling was 12 Months 42 ⫾ 8 43 ⫾ 3
increased by rapid (200 ml/min) infusion of warm (37°C), isotonic Values are means ⫾ SD. BSA, body surface area; FFM, fat-free mass; TBV,
saline. Measurements were repeated after 15 and 30 ml/kg had been total blood volume; PV, plasma volume. *P ⬍ 0.05 and **P ⬍ 0.01 vs.
infused. baseline.
J Appl Physiol • doi:10.1152/japplphysiol.00092.2015 • www.jappl.org
40 Sex Differences in Response to Endurance Training • Howden EJ et al.
A B
Fig. 2. A and B: effect of 1 yr of endurance 60 4.0
training on maximal oxygen uptake (V̇O2max) Male *†‡ * †‡ *† †
*†
indexed to baseline body mass in males and 55 Female
*
VO2 max, ml·kg·min-1
* * *
LV mass, g/kg FFM
females (left), significant sex ⫻ time interac-
*
3.5 * *
tion P ⫽ 0.084 and changes in left ventricle 50
(LV) mass measured by magnetic resonance
imaging (MRI) scaled to baseline fat-free
mass, significant sex ⫻ time interaction P ⫽
45
* * * * 3.0
0.031 (right). Both measured every 3 mo dur-
ing the training program. FFM, fat-free mass. 40
Post hoc comparison with baseline (*), with 2.5
month 3 (†), and with month 6 (‡) for P ⬍ 0.05 35
•
from linear mixed model.
30 2.0
Baseline 3 mo 6 mo 9 mo 12 mo Baseline 3 mo 6 mo 9 mo 12 mo
Criteria and model parsimony. Our analysis was unadjusted, and the or 100-mile endurance cycling race (n ⫽ 1 female). One male
analysis was by available data (last observation was not varied subject had a metal implant and was unable to undergo MRI,
forward). To test our primary hypothesis whether previously seden-
Downloaded from http://jap.physiology.org/ by 10.220.33.1 on October 30, 2017
but completed all other testing. The baseline characteristics and
tary healthy young males and females differ in response to 1 yr of
endurance training, the sex ⫻ time interaction was used, with a P
effect of training on body size, composition, and blood volume
value of ⬍0.10 declared significant. Similar regression models were are summarized in Table 1. Comparison between the sexes
used to assess pressure-volume curves with the addition of a fixed showed that females had smaller body size, less FFM and
effect to test for the difference and response interactions between the higher percent body fat (P ⱕ 0.031), and lower hematocrit
baseline and training curves and sex. To express the dose-response levels (P ⫽ 0.009) before training than males. After training
relationship between the exercise training stimulus and changes in LV there was no difference between sexes for hematocrit, body fat,
mass, the relationship between the quarterly training impulse and indexed blood volume. There was a significant sex ⫻ time
(monthly TRIMP) and cardiac adaptations at baseline and 3, 6, 9, and
12 mo was estimated with quadratic polynomial regression models.
interaction (P ⫽ 0.081) for percent body fat. Females demon-
Statistical analysis was performed using commercially available soft- strated a reduction in body fat after 6 mo of training (22.8 ⫾
ware (IBM SPSS, SAS version 9.3; SAS Institute, Cary, NC). Statis- 4.5 vs. 18.1 ⫾ 2.1%, P ⫽ 0.048); a further 6 mo of training
tical significance was declared at a P value of ⬍0.05. sustained the reduction in body fat (P ⫽ 0.006, month 12
compared with baseline, 16.2 ⫾ 4.2%). In males, percent body
RESULTS
fat did not decrease significantly until month 12 of training
At 1 yr, all subjects completed either a marathon (n ⫽ 10, 4 (19.3 ⫾ 6.1 vs. 15.0 ⫾ 3.4%, P ⫽ 0.026). The effect of the
females and 6 males), Olympic distance triathlon (n ⫽ 1 male), intervention on lean body mass was similar between sexes
Table 2. Effect of 1 yr of endurance training on maximal exercise response
Month
P Value (main P Value
Baseline 3 6 9 12 effect of time) (sex ⫻ time)
V̇O2, l/min
Males 3.36 ⫾ 0.44 3.75 ⫾ 0.43* 3.85 ⫾ 0.35* 4.07 ⫾ 0.43*†‡ 4.09 ⫾ 0.47*†‡ ⬍0.001 0.013
Females 2.19 ⫾ 0.14 2.48 ⫾ 0.16* 2.57 ⫾ 0.18* 2.48 ⫾ 0.21*† 2.51 ⫾ 0.12*†
V̇O2, ml/kg FFM
Males 53.6 ⫾ 5.0 59.9 ⫾ 4.9* 61.4 ⫾ 3.6* 64.9 ⫾ 4.9*†‡ 65.3 ⫾ 5.6*† ⬍0.001 0.094
Females 47.0 ⫾ 3.5 53.3 ⫾ 5.8* 55.2 ⫾ 5.4* 53.1 ⫾ 4.5* 54.2 ⫾ 7.1*
Heart rate, beats/min
Males 200 ⫾ 12 189 ⫾ 7 189 ⫾ 10 190 ⫾ 12 188 ⫾ 12 ⬍0.001 0.56
Females 192 ⫾ 7 185 ⫾ 9 185 ⫾ 6 183 ⫾ 6 186 ⫾ 8
Cardiac index, l·m⫺2·min⫺1
Males 12.2 ⫾ 1.3 13.6 ⫾ 1.3 12.5 ⫾ 1.3 12.0 ⫾ 1.9 12.9 ⫾ 1.6 0.029 0.32
Females 8.9 ⫾ 1.1 9.9 ⫾ 1.5 8.9 ⫾ 0.8 10.3 ⫾ 2.1 10.4 ⫾ 1.4
Stroke index, ml/m2
Males 60.8 ⫾ 5.2 72.5 ⫾ 6.8 66.6 ⫾ 9.3 63.7 ⫾ 12.6 69.1 ⫾ 12.0 0.002 0.37
Females 46.2 ⫾ 5.8 53.9 ⫾ 9.8 48.1 ⫾ 3.9 56.3 ⫾ 10.9 55.7 ⫾ 5.9
a-vO2 diff, ml/100 ml
Males 14.2 ⫾ 1.6 14.2 ⫾ 1.4 15.9 ⫾ 2.0 17.6 ⫾ 2.0*† 16.4 ⫾ 1.8 0.021 0.009
Females 14.8 ⫾ 1.5 15.1 ⫾ 2.7 17.2 ⫾ 1.3* 14.6 ⫾ 2.4‡ 14.6 ⫾ 1.8‡
Lactate, mmol/l
Males 10.4 ⫾ 1.6 10.6 ⫾ 3.2 10.6 ⫾ 1.4 9.3 ⫾ 1.0 9.2 ⫾ 1.7 0.55 0.59
Females 9.9 ⫾ 3.4 9.0 ⫾ 1.9 10.6 ⫾ 2.9 10.1 ⫾ 1.7 9.2 ⫾ 2.7
Values are means ⫾ SD. a-vO2 diff, systemic arteriovenous oxygen difference. The P value within the table represents the main effect of time. Post hoc
comparisons are indicated from the linear mixed-effects model where there was a statistically significant, P ⬍ 0.10 sex ⫻ time interaction; P ⬍ 0.05 vs. baseline
(*), 3 mo (†), and 6 mo (‡).
J Appl Physiol • doi:10.1152/japplphysiol.00092.2015 • www.jappl.org
Sex Differences in Response to Endurance Training • Howden EJ et al. 41
(sex ⫻ time P ⫽ 0.38), with training resulting in a similar increase in V̇O2max occurring during the initial 3 mo of training
significant increase (main effect of time P ⫽ 0.019). (13% increase from baseline) plateauing thereafter despite the
further increases in training load. In both sexes, training de-
Training Impulse creased maximal HR and increased QI, which resulted in a
The amount of training performed was virtually identical significant increase in SI after completion of 1 yr of training
between sexes (males total TRIMP ⫽ 19,919 ⫾ 8,687 vs. (Table 2). There was a significant sex ⫻ time interaction for
females total TRIMP ⫽ 19,989 ⫾ 2,695, P ⫽ 0.98; Fig. 1). a-vO2 diff (P ⫽ 0.026; Table 2), where males increased a-vO2
after 9 mo of training while females increased after 6 mo of
Maximal Exercise Response training before decreasing back to baseline levels.
The effect of the 1 yr of training on V̇O2max indexed to body Effect of Sex on Left Ventricular Adaptations to Training
mass is shown in Fig. 2A. Endurance training increased V̇O2max
by 22% in males and 15% in females. There was a significant The adaptations in LV structure to the intervention are
sex ⫻ time interaction for absolute (P ⫽ 0.018; our primary presented in Figs. 2–5 and Table 3. Similar to the response of
outcome variable) and V̇O2max scaled to body mass (P ⫽ 0.084) V̇O2max, we detected a significant sex ⫻ time interaction for LV
and FFM (P ⫽ 0.094), which resulted in the males demon- mass indexed to FFM (P ⫽ 0.031). The pattern in LV mass
strating a progressive increase in V̇O2max over the first 9 mo of relative to FFM remodeling is shown in Fig. 2B. In males, LV
endurance training and then plateauing from months 9 to 12 mass increased by 11 ⫾ 2% (P ⬍ 0.05) during the first 3 mo
(Fig. 2A and Table 2). The response of V̇O2max in the females of training and 9 ⫾ 2 (P ⬍ 0.01) between 3 and 6 mo, with the
Downloaded from http://jap.physiology.org/ by 10.220.33.1 on October 30, 2017
was blunted compared with the males, with the majority of the total increase during the first 6 mo being 20 ⫾ 2% (P ⬍ 0.01).
Table 3. Effect of 1 yr of endurance training on left and right ventricle morphology and function measured by cardiac MRI
P Value (main P Value
Baseline Month 3 Month 6 Month 9 Month 12 effect of time) (sex ⫻ time)
MWT, cm
Males 1.00 ⫾ 0.13 1.19 ⫾ 0.13* 1.27 ⫾ 0.11*† 1.23 ⫾ 0.12* 1.23 ⫾ 0.06* ⬍0.001 ⬍0.001
Females 1.00 ⫾ 0.05 1.11 ⫾ 0.05* 1.12 ⫾ 0.02* 1.05 ⫾ 0.05†‡ 1.07 ⫾ 0.07*
LV mass, g
Males 192 ⫾ 31 212 ⫾ 27* 230 ⫾ 24*† 234 ⫾ 23*† 238 ⫾ 26*† ⬍0.001 0.001
Females 140 ⫾ 15 158 ⫾ 13* 160 ⫾ 12* 157 ⫾ 13*‡ 164 ⫾ 12*
LV EDV, ml
Males 132 ⫾ 10 136 ⫾ 11 143 ⫾ 11 151 ⫾ 14 158 ⫾ 13 ⬍0.001 0.39
Females 98 ⫾ 10 99 ⫾ 9 104 ⫾ 10 118 ⫾ 14 116 ⫾ 15
LV ESV, ml
Males 43 ⫾ 8 40 ⫾ 6 41 ⫾ 7 44 ⫾ 8 44 ⫾ 8 ⬍0.001 0.79
Females 30 ⫾ 6 28 ⫾ 4 31 ⫾ 3 32 ⫾ 5 34 ⫾ 6
LV SV, ml
Males 89 ⫾ 3 96 ⫾ 5* 102 ⫾ 5*† 107 ⫾ 7*†‡ 113 ⫾ 7*†‡§ ⬍0.001 0.035
Females 68 ⫾ 5 71 ⫾ 6 74 ⫾ 6* 85 ⫾ 10*†‡ 81 ⫾ 9*†‡
LV ejection fraction, %
Males 68 ⫾ 4 71 ⫾ 3 71 ⫾ 3 71 ⫾ 3 72 ⫾ 3 0.001 0.28
Females 69 ⫾ 4 72 ⫾ 2 71 ⫾ 1 72 ⫾ 2 70 ⫾ 2
LV mass/volume
Males 1.45 ⫾ 0.19 1.56 ⫾ 0.16* 1.61 ⫾ 0.13* 1.55 ⫾ 0.11* 1.51 ⫾ 0.08‡ ⬍0.001 0.008
Females 1.42 ⫾ 0.04 1.60 ⫾ 0.03* 1.54 ⫾ 0.14* 1.34 ⫾ 0.11† 1.34 ⫾ 0.11†‡
RV EDV, ml
Males 156 ⫾ 9 180 ⫾ 8 188 ⫾ 11 193 ⫾ 10 198 ⫾ 17 ⬍0.001 0.20
Females 112 ⫾ 13 126 ⫾ 9 128 ⫾ 10 146 ⫾ 16 144 ⫾ 14
RV ESV, ml
Males 70 ⫾ 6 82 ⫾ 5 86 ⫾ 6 86 ⫾ 6 88 ⫾ 12 ⬍0.001 0.26
Females 46 ⫾ 7 53 ⫾ 5 54 ⫾ 5 63 ⫾ 11 61 ⫾ 9
RV SV, ml
Males 87 ⫾ 4 98 ⫾ 5 103 ⫾ 5 107 ⫾ 7 110 ⫾ 7 ⬍0.001 0.31
Females 66 ⫾ 7 73 ⫾ 4 74 ⫾ 7 85 ⫾ 9 82 ⫾ 7
RV mass, g
Males 69 ⫾ 7 78 ⫾ 7* 83 ⫾ 7* 86 ⫾ 8*† 91 ⫾ 9*†‡ ⬍0.001 0.066
Females 56 ⫾ 6 62 ⫾ 5 61 ⫾ 5 63 ⫾ 14 69 ⫾ 11*‡
RV ejection fraction, %
Males 56 ⫾ 2 55 ⫾ 1 55 ⫾ 1 55 ⫾ 2 55 ⫾ 2 0.70 0.82
Females 59 ⫾ 2 58 ⫾ 2 58 ⫾ 2 58 ⫾ 2 58 ⫾ 2
RV mass/vol
Males 0.44 ⫾ 0.05 0.44 ⫾ 0.04 0.45 ⫾ 0.04 0.45 ⫾ 0.02 0.46 ⫾ 0.05 0.037 0.019
Females 0.51 ⫾ 0.03 0.48 ⫾ 0.03 0.46 ⫾ 0.05* 0.42 ⫾ 0.06*†‡ 0.49 ⫾ 0.06§
Values are means ⫾ SD; n ⫽ 6 male and 5 female subjects for all parameters. All variables were measured by cardiac magnetic resonance imaging (MRI).
MWT, mean wall thickness; RV, right ventricle; LV, left ventricle; EDV, end-diastolic volume; ESV, end-systolic volume; SV, stoke volume. The P value within
the table represents the main effect of time. Post hoc comparisons are indicated from the linear mixed-effects model where there was a statistically significant,
P ⬍ 0.10 sex ⫻ time interaction; P ⬍ 0.05 vs. baseline (*), 3 mo (†), 6 mo (‡), and 9 mo (§).
J Appl Physiol • doi:10.1152/japplphysiol.00092.2015 • www.jappl.org
42 Sex Differences in Response to Endurance Training • Howden EJ et al.
A B
250 250
LV mass, g
LV mass, g
Fig. 3. A and B: quadratic regression analysis
between average quarterly TRIMP values as 200 200
measure of training stimulus and LV mass.
Light gray lines, individual curves; solid
black line, curves for males and females.
150 150
0 2000 4000 6000 8000 0 2000 4000 6000 8000
TRIMP TRIMP
Downloaded from http://jap.physiology.org/ by 10.220.33.1 on October 30, 2017
In females, the greatest increase in LV mass indexed to FFM mass-to-volume ratio decreased to below baseline values, sug-
(13 ⫾ 2%, P ⬍ 0.01) occurred during the first 3 mo of training. gesting even greater eccentric remodeling.
In contrast to the males, there was no further statistically
significant increase in LV mass indexed to FFM in the females Effect of Sex on Right Ventricular Adaptations to Training
(Fig. 2B). When the mean quarterly values for LV mass were
The RV volumetric adaptations that occurred during the 1 yr
compared with the average TRIMP values obtained for each
of training were similar between sexes (Fig. 4B and Table 3).
quarter in males and females, we observed a strong positive
There was a sex ⫻ time (P ⫽ 0.066) interaction for RV mass
relationship in the males such that as training impulse in-
(Table 3), demonstrating again that males have a more pro-
creased LV mass was markedly augmented, whereas in the
nounced hypertrophic response to training compared with fe-
females the effect of increased training impulse was markedly
males. There was a significant sex ⫻ time interaction for RV
attenuated with a small gradual increase in mass with increas-
mass-to-volume ratio (Table 3). Interestingly, males main-
ing training stimulus (Fig. 3, A and B).
tained a similar mass-to-volume ratio throughout the interven-
MWT was increased by training and paralleled the increase
tion. However, the ratio decreased in females as the training
in LV mass in both sexes (Table 3). In males, MWT increased
progressed.
by 27 ⫾ 3% during the first 6 mo of training. In females the
increase in MWT was 11 ⫾ 2% during the first 3 mo. Pressure-Volume Curves
The effect of endurance training on LVEDVI was similar
between sexes (sex ⫻ time P ⫽ 0.34; Fig. 4A). The overall The LV pressure-volumes curves constructed from group
increase in LVEDVI was 20% for males and 18% for females. mean data in males and females are shown in Fig. 5, A and B,
The pattern of concentric and eccentric modelling was over- respectively. Both Vm and V0 increased in the males and
all similar between males and females; however, the time females consistent with significant physiological remodeling.
course of change was different (sex ⫻ time P ⫽ 0.008, Table The response to endurance training for the pressure-volume
3). Both sexes demonstrated an initial increase in mass and curves was similar between sexes (sex ⫻ time P ⫽ 0.18), with
wall thickness, consistent with concentric remodeling. The LV both males (P ⫽ 0.039) and females (P ⬍ 0.001) demonstrat-
mass-to-volume ratio returned to near baseline levels in the ing a significant rightward shift. LV pressure-volume curves
males at completion of the study, whereas in the females the (Fig. 6, A and B) constructed using transmural pressure dem-
A B
Fig. 4. A and B: effect of 1 yr of endurance Male
training on left ventricle end-diastolic vol- 100 100
Female
ume (LVEDV, A) and right ventricle end-
diastolic volume (RVEDV, B) scaled to
RVEDVI, ml/m2
LVEDVI, ml/m2
baseline total body surface area, measured
by MRI every 3 mo during the 1-yr training 80 80
program. For left ventricular end-diastolic
volume index (LVEDVI) and right ventricu-
lar end-diastolic volume index (RVEDVI),
males and females responded in a similar 60 60
manner to the training (LVEDVI sex ⫻ time
P ⫽ 0.48 and RVEDVI sex ⫻ time P ⫽
0.22).
40 40
Baseline 3 mo 6 mo 9 mo 12 mo Baseline 3 mo 6 mo 9 mo 12 mo
J Appl Physiol • doi:10.1152/japplphysiol.00092.2015 • www.jappl.org
Sex Differences in Response to Endurance Training • Howden EJ et al. 43
A B 25
25
Pre Pre
S= 8.1 S= 7.7
20
20
Vmax= 81 Vmax= 59
Fig. 5. A and B: group mean pressure-volume
PCWP, mmHg
PCWP, mmHg
V0= 23 V0= 22
curves for male (A) and female (B) subjects
15 15
with data points derived from baseline, low-
er-body negative pressure (LBNP), and rapid
10 Post 10 saline infusion, similar to Fig. 6. Each data
Post
S= 8.8 S= 8.4 point represents the mean ⫾ SE of males or
5 Vmax= 84 5 females, pre vs. post (sex ⫻ time P ⫽ 0.18).
Vmax= 67
V0= 35 V0= 28
0 0
30 40 50 60 70 80 90 30 40 50 60 70 80 90
LVEDVI, mL/m 2
LVEDVI, mL/m2
onstrated a significant interaction (sex ⫻ time P ⫽ 0.07), with anism has been shown to be a hallmark characteristic of
females demonstrating a significant shift in the pressure-vol- endurance athletes (26).
ume curve posttraining (P ⫽ 0.02), but not males (P ⫽ 0.75).
Downloaded from http://jap.physiology.org/ by 10.220.33.1 on October 30, 2017
Effect of One Year of Endurance Training on Exercise
Frank-Starling Curves
Performance and Cardiac Morphology
Frank-Starling curves are shown in Fig. 7, A and B, for
This is the first study to demonstrate that healthy previously
males and females, respectively. There was a significant sex ⫻
time interaction (P ⫽ 0.06). The training effect in females was sedentary males have a markedly greater increase in LV mass
⬃7.1 ml less than in the males. and V̇O2max compared with the response in females to 1 yr of
identical endurance training. To that end, we recorded each
DISCUSSION heart beat during exercise to carefully quantify the amount of
training performed using the TRIMP method (6). As can be
The main new findings from the present study were clear seen from Fig. 1, males and females received a nearly identical
differences in the time course and magnitude of cardiovascular training stimulus. However, there was a divergent response in
adaptation between previously sedentary males and females in the observed adaptations to training. Surprisingly V̇O2max pla-
response to identical endurance training loads. Males had more teaued after only 3 mo of training in females, but continued to
pronounced LV hypertrophy throughout the 1 yr of training, increase progressively in males until month 9, resulting in an
whereas females reached the maximal LV mass after only 3 mo
⬃7% greater increase in V̇O2max at month 12. Indeed, as
of training. The LV hypertrophic response closely paralleled
training intensity increased in the males, we observed a pro-
the increase in V̇O2max in both sexes, which was blunted in
females. We found that ventricular remodeling and increased gressive increase in LV mass that was not evident in the
compliance were similar between sexes, but endurance training females (Fig. 2B). To our knowledge no endurance training
resulted in greater augmentation of the Frank-Starling mecha- studies have compared sex differences in healthy young sub-
nism in the males compared with females. The greater effect of jects beyond 3 mo of training. Therefore, until now, important
endurance training on the Frank-Starling mechanism (relation- differences in the cardiovascular response to training may have
ship between LV filling pressures and SV) in the males been missed. Indeed 90 days of intense endurance training in
means that males had a greater diastolic reserve after 1 yr of female and male rowers resulted in no significant differences
training. This adaptation to training is extremely beneficial between sexes for change in any cardiovascular variables (4).
for performing exercise, allowing individuals to generate a Thus it seems likely that cardiovascular sex differences have
higher SV and cardiac output in response to an increase in been underestimated due to the duration of prior training
filling pressure. Indeed, an enhanced Frank-Starling mech- studies.
A B
8 8
Pre Pre
S= 1.9 S= 2.5
6 Vmax= 80 6 Vmax= 60 Fig. 6. A and B: group mean transmural pres-
TMP, mmHg
V0= 1.208e-16 V0 = 8 sure (TMP)-volume curves for male (A) and
female (B) subjects with data points derived
TMP
4 4 from baseline, LBNP, and rapid saline infu-
Post Post sion. Each data point represents the mean ⫾
S= 2.4 S= 2.3 SE of males or females, pre vs. post (sex ⫻
2
Vmax= 86
2
Vmax= 69
time P ⫽ 0.07).
V0= 1.208e-16 V0= 2.6
0 0
30 40 50 60 70 80 90 30 40 50 60 70 80 90
LVEDVI, mL/m2 LVEDVI, mL/m2
J Appl Physiol • doi:10.1152/japplphysiol.00092.2015 • www.jappl.org
44 Sex Differences in Response to Endurance Training • Howden EJ et al.
A B
80 80
Fig. 7. A and B: group mean Frank-Starling
curves representing pulmonary capillary
wedge pressure (PCWP) as an index of LV
end-diastolic pressure vs. stroke volume in- POST
POST
SI (ml/m2)
SI (ml/m2)
dex (SI), over a range of LV filling produced
by lower-body negative pressure (two lowest 60 60
levels of PCWP), quiet baseline (two middle
values of PCWP), and rapid saline infusion
(two highest values of PCWP) as described in PRE
text. Each data point represents the mean ⫾ SE PRE
of males or females, pre vs. post (sex ⫻ time 40 40
P ⫽ 0.06).
0 5 10 15 20 25 0 5 10 15 20 25
PCWP (mmHg) PCWP (mmHg)
Consistent with the sex difference observed in the LV, the Moreover, diet also influences cardiac adaptation in mice and
RV also increased in mass in response to training. The re- must be considered when using this model to assess sex
sponse in males was again more prominent than the females, differences (23). The present study suggests that endurance
Downloaded from http://jap.physiology.org/ by 10.220.33.1 on October 30, 2017
who did not demonstrate a significant increase in RV mass training has an early anabolic effect on female hearts while the
until completion of the study. Few prospective studies have increase in male heart size is more progressive possibly due to
assessed the degree of RV hypertrophy with endurance train- small elevations in androgens.
ing, due to the difficulty in reliably assessing morphology It should be noted that we observed a marked reduction in
using echocardiography. Recent evidence from cross-sectional body fat in female participants from month 6 of training
studies with cMRI suggests that the mass of RV is increased to onward. This reduction in fat mass coincided with an increase
match the increased work of the LV and maintain a balanced in training impulse (Fig. 1), since both intensity and duration of
ratio to enhance function in male and female athletes (32, 33). training were dramatically increased. We did not observe
Transient increases in pulmonary artery pressure during exer- similar changes in body fat in the males in response to the
cise likely contribute to the enlargement of the RV. Endurance increase in training load. Our intervention provided only gen-
athletes have greater RV enlargement and wall thickening, eral dietary advice. Thus a possible explanation for the lack of
which is thought to be due to the disproportionate increase in effect of endurance training on V̇O2max and cardiac mass in
hemodynamic load placed on the RV during endurance exer- females may be partially explained by a suboptimal energy
cise (25). Given these prior findings, our results raise the intake. The American College of Sports Medicine recognizes
possibility that the male participants may have been under a that female athletes are plagued by low energy intake (2). A
greater hemodynamic stress during training, which is reflected reduced energy intake will result in the utilization of fat and
by the greater increase in RV mass. In the present studies, the lean tissue stores to fuel the body during exercise and may
increase in RV and LV mass in females was attenuated com- impair muscle protein synthesis (35).
pared with the changes observed in the LV and in the males, Alternatively, other aspects of the subject’s lives may have
but still reached levels comparable with female athletes (29). influenced the lack of adaptation observed in the female sub-
jects, including lack of appropriate recovery or other life-
Potential Underlying Mechanisms Regulating Sex related stressors (e.g., sleep, work, and emotional upheavals).
Differences in Response to Training Indeed all subjects showed some signs of overtraining toward
Sex differences in the endogenous androgens play a key role the end of the study. We have previously reported that pro-
in the development of both skeletal muscle and cardiac hyper- longed intense training does not necessarily result in greater
trophy. In male rats who have undergone orchiectomy ventric- enhancement of dynamic regulation of HR or blood pressure
ular mass is decreased, while testosterone administration in- (18). In our prior study, we demonstrated a bell-shaped relation
duces myocellular hypertrophy (22). Regular exercise training with late changes in autonomic control of the circulation,
is a strong stimulus to increase circulating endogenous testos- possibly due to the effects of overtraining. Unfortunately, we
terone levels, which promotes muscle growth, through protein did not collect information on the subject’s quality of life
synthesis and inhibits protein degradation (38). Circulating throughout the study or indicators of overtraining. Future
estrogen levels influence cardiac hypertrophy by preventing the studies should plan to include specific dietary advice as would
development of pathological cardiac hypertrophy in premeno- be recommended to male and female athletes performing such
pausal females, with the benefit reduced in the postmenopausal a high volume of endurance training, and include assessments
state (16). It remains unclear whether estrogen also influences of quality of life.
exercise-induced cardiac hypertrophy. Indeed, rodent studies Another possible explanation for the observed sex differ-
suggest an enhanced cardiac hypertrophic response to training ences in cardiac hypertrophy may relate to differences in
in females compared with males (24). However, key differ- signaling events that mediate hypertrophy. Cardiac hypertro-
ences in animal and human female reproductive physiology, phy due to exercise is mediated by peptide growth factors and
namely estrous vs. menstrual cycle, limit the interpretation of signaling through the phosphatidylinositol 3-kinase/Akt path-
the influence of sex hormones on cardiac adaptations in mice way (13). Premenopausal females have a fivefold increase in
and must be considered when interpreting animal studies. Akt when compared with age-matched males (10). We specu-
J Appl Physiol • doi:10.1152/japplphysiol.00092.2015 • www.jappl.org
Sex Differences in Response to Endurance Training • Howden EJ et al. 45
late that young females may be somewhat protected from measures of sex hormones, although all females experienced
marked increases in ventricular hypertrophy by the increased normal menstrual cycles at all times during the study. Future
levels of Akt. Evidence from animal studies also provides studies should include these measures. Although we observed
some support for this hypothesis. Endurance-trained female a divergent response between sexes for a-vO2 diff, this finding
mice have been shown to have higher levels of phosphorylated seems to be driven by the response of one female, a further
glycogen synthase kinase-3beta (GSK) in isolated cardiac tis- limitation of our small sample size.
sue compared with male mice (24). GSK is a downstream
target of Akt kinase and negative regulator of cardiac hyper- Conclusion
trophy. Thus the hypertrophic response to endurance training In summary, the cardiovascular adaptation to 1 yr of endur-
in young females may be blunted by a combination of in- ance training has a different time course and magnitude of
creased levels of Akt and GSK. effect in males and females, even when performing identical
endurance training. Males had a more prominent increase in
Ventricular Remodeling LV mass throughout the study, whereas females reached max-
The superior athletic ability of the elite athlete is partially imal LV hypertrophy in 3 mo, although the intensity of training
due to a large compliant LV and enhanced ability to utilize the was similar in both sexes. Aerobic power was clearly related to
Frank-Starling mechanism to increase SV during exercise (26). LV hypertrophy. Ventricular compliance and distensibility
Endurance athletes have a greater augmentation in SV for any improved similarly in males and females, but males demon-
given filling pressure and increased diastolic reserve, meaning strate greater enhancement in the Frank-Starling mechanism
Downloaded from http://jap.physiology.org/ by 10.220.33.1 on October 30, 2017
their LVs are more compliant and distensible compared with compared with the females, emphasizing the divergent sex
sedentary subjects (26). We recently demonstrated that 1 yr of response to endurance training.
training resulted in a significant improvement in ventricular ACKNOWLEDGMENTS
distensibility and possible reduction in pericardial constraint in
healthy young individuals (3). In the present study, we extend We thank Matthew J. Morrow for work in training the subjects, Fatima
Franco for assistance with MRI analysis, and Julie H. Zuckerman for nursing
these findings to examine whether the response to training care during the invasive studies and performance of the ultrasound measure-
differs in males and females. Despite clear sex differences in ments.
the hypertrophic response to endurance training, both males
and females had a similar augmentation in end-diastolic vol- GRANTS
ume and LV compliance and distensibility. The Frank-Starling This study was supported by National Aeronautic and Space Administration
mechanism was augmented to a greater extent in males com- Specialized Center for Research and Training Grant NGW-3582, the S. Finley
Ewing Chair for Wellness at Texas Health Presbyterian Hospital, and the Harry
pared with females, which is likely due to the greater amount S. Moss Heart Chair for Cardiovascular Research.
of hypertrophy in the males and therefore larger SV (26). An
increase in wall thickness of the ventricle results in a reduction DISCLOSURES
in wall stress and afterload. This in turn allows for a smaller The authors declare no conflict of interest.
end-systolic volume and thus larger SV. In addition, ventricu-
lar remodeling occurs in response to endurance training, which AUTHOR CONTRIBUTIONS
increases muscle mass and results in greater ventricular com- Author contributions: E.J.H., M.P., R.M.P., A.A.-Z., B.A.-H., and B.D.L.
pliance. Therefore, for a given filling pressure, the males were analyzed data; E.J.H., M.P., R.M.P., R.Z., A.A.-Z., B.A.-H., and B.D.L.
able to generate a greater end-diastolic volume. We speculate interpreted results of experiments; E.J.H. prepared figures; E.J.H. and M.P.
drafted manuscript; E.J.H. and B.D.L. edited and revised manuscript; E.J.H.,
that even more prolonged training (e.g., years), or the com- M.P., R.M.P., R.Z., A.A.-Z., B.A.-H., and B.D.L. approved final version of
mencement of training during developmental years, may be manuscript; M.P., R.M.P., R.Z., A.A.-Z., and B.D.L. performed experiments;
required to improve LV compliance to levels similar to endur- R.Z. and B.D.L. conception and design of research.
ance athletes (26). Long-term follow-up is also required to
determine whether maintenance of this training frequency REFERENCES
through middle age and beyond will indeed maintain LV 1. Alway SE, Grumbt WH, Gonyea WJ, Stray-Gundersen J. Contrasts in
compliance. muscle and myofibers of elite male and female bodybuilders. J Appl
Physiol 67: 24 –31, 1989.
Limitations 2. American Dietetic Association, Dietitians of the American College of
Sports Medicine, Rodriguez NR, Di Marco NM, Langley S. American
The primary limitation with this study is its small sample College of Sports Medicine position stand Nutrition and athletic perfor-
mance Med Sci Sports Exerc 41: 709 –731, 2009.
size, a direct reflection of the intensive and invasive nature of 3. Arbab-Zadeh A, Perhonen M, Howden E, Peshock RM, Zhang R,
the training and assessment tools. Few studies have reported Adams-Huet B, Haykowsky MJ, Levine BD. Cardiac remodeling in
the effects of sex on cardiac adaptations to exercise training. response to 1 year of intensive endurance training. Circulation 130:
Thus, while our sample size is small, these results are highly 2152–2161, 2014.
4. Baggish AL, Wang F, Weiner RB, Elinoff JM, Tournoux F, Boland A,
novel in the field of exercise physiology. The small sample size Picard MH, Hutter AM Jr, Wood MJ. Training-specific changes in
is also offset by our observations of significant sex ⫻ time cardiac structure and function: a prospective and longitudinal assessment
interactions, and our within-subject design, which minimized of competitive athletes. J Appl Physiol 104: 1121–1128, 2008.
important sources of error. It is also notable that MRI is 5. Banister EW, Morton RH, Fitz-Clarke J. Dose/response effects of
substantially more precise in terms of cardiac morphological exercise modeled from training: physical and biochemical measures. Ann
Physiol Anthropol 11: 345–356, 1992.
assessment than echocardiography (20). LV pressure-volume 6. Bannister EW, Hamilton CL. Monitoring training. In: Physiological
curves were evaluated by use of mean PCWP as a surrogate for Testing of the Elite Athlete, edited by MacDougall JD, Wenger HA.
LV end-diastolic pressure. Unfortunately we do not have direct Ottawa, Canada: Canadian Association of Sport Sciences, 1982.
J Appl Physiol • doi:10.1152/japplphysiol.00092.2015 • www.jappl.org
46 Sex Differences in Response to Endurance Training • Howden EJ et al.
7. Batterham AM, George KP. Modeling the influence of body size and 24. Konhilas JP, Maass AH, Luckey SW, Stauffer BL, Olson EN, Lein-
composition on M-mode echocardiographic dimensions. Am J Physiol wand LA. Sex modifies exercise and cardiac adaptation in mice. Am J
Heart Circ Physiol 274: H701–H708, 1998. Physiol Heart Circ Physiol 287: H2768 –H2776, 2004.
8. Belenkie I, Kieser TM, Sas R, Smith ER, Tyberg JV. Evidence for left 25. La Gerche A, Heidbuchel H, Burns AT, Mooney DJ, Taylor AJ,
ventricular constraint during open heart surgery. Can J Cardiol 18: Pfluger HB, Inder WJ, Macisaac AI, Prior DL. Disproportionate
951–959, 2002. exercise load and remodeling of the athlete’s right ventricle. Med Sci
9. Brown M. Skeletal muscle and bone: effect of sex steroids and aging. Adv Sports Exerc 43: 974 –981, 2011.
Physiol Ed 32: 120 –126, 2008. 26. Levine BD, Lane LD, Buckey JC, Friedman DB, Blomqvist CG. Left
10. Camper-Kirby D, Welch S, Walker A, Shiraishi I, Setchell KD, ventricular pressure-volume and Frank-Starling relations in endurance
Schaefer E, Kajstura J, Anversa P, Sussman MA. Myocardial Akt athletes. Implications for orthostatic tolerance and exercise performance.
activation and gender: increased nuclear activity in females versus males. Circulation 84: 1016 –1023, 1991.
Circ Res 88: 1020 –1027, 2001. 27. Nagueh SF, Appleton CP, Gillebert TC, Marino PN, Oh JK, Smiseth
11. Carrick-Ranson G, Hastings JL, Bhella PS, Shibata S, Fujimoto N, OA, Waggoner AD, Flachskampf FA, Pellikka PA, Evangelista A.
Palmer D, Boyd K, Levine BD. The effect of age-related differences in Recommendations for the evaluation of left ventricular diastolic function
body size and composition on cardiovascular determinants of VO2max. J by echocardiography. J Am Soc Echocardiogr 22: 107–133, 2009.
Gerontol A Biol Sci Med Sci 68: 608 –616, 2013. 28. Nikolic S, Yellin EL, Tamura K, Vetter H, Tamura T, Meisner JS,
12. D’Andrea A, Riegler L, Cocchia R, Scarafile R, Salerno G, Gravino R, Frater RW. Passive properties of canine left ventricle: diastolic stiffness
Golia E, Vriz O, Citro R, Limongelli G, Calabro P, Di Salvo G, Caso and restoring forces. Circ Res 62: 1210 –1222, 1988.
P, Russo MG, Bossone E, Calabro R. Left atrial volume index in highly 29. Pelliccia A, Maron BJ, Culasso F, Spataro A, Caselli G. Athlete’s heart
trained athletes. Am Heart J 159: 1155–1161, 2010. in women. Echocardiographic characterization of highly trained elite
13. Dorn GW, 2nd. The fuzzy logic of physiological cardiac hypertrophy. female athletes. J Am Med Assoc 276: 211–215, 1996.
Hypertension 49: 962–970, 2007. 30. Perhonen MA, Franco F, Lane LD, Buckey JC, Blomqvist CG,
Downloaded from http://jap.physiology.org/ by 10.220.33.1 on October 30, 2017
14. Foldager N, Blomqvist CG. Repeated plasma volume determination with Zerwekh JE, Peshock RM, Weatherall PT, Levine BD. Cardiac atrophy
the Evans Blue dye dilution technique: the method and a computer after bed rest and spaceflight. J Appl Physiol 91: 645–653, 2001.
program. Comput Biol Med 21: 35–41, 1991. 31. Peshock RM, Willett DL, Sayad DE, Hundley WG, Chwialkowski
15. Germain P, Roul G, Kastler B, Mossard JM, Bareiss P, Sacrez A. MC, Clarke GD, Parkey RW. Quantitative MR imaging of the heart.
Inter-study variability in left ventricular mass measurement. Comparison Magn Reson Imaging Clin N Am 4: 287–305, 1996.
between M-mode echography and MRI. Eur Heart J 13: 1011–1019, 32. Petersen SE, Hudsmith LE, Robson MD, Doll HA, Francis JM,
1992. Wiesmann F, Jung BA, Hennig J, Watkins H, Neubauer S. Sex-
16. Haines CD, Harvey PA, Leinwand LA. Estrogens mediate cardiac specific characteristics of cardiac function, geometry, and mass in young
hypertrophy in a stimulus-dependent manner. Endocrinology 153: 4480 – adult elite athletes. J Magn Res Imaging 24: 297–303, 2006.
4490, 2012. 33. Scharhag J, Schneider G, Urhausen A, Rochette V, Kramann B,
17. Hundley WG, Li HF, Willard JE, Landau C, Lange RA, Meshack Kindermann W. Athlete’s heart: right and left ventricular mass and
BM, Hillis LD, Peshock RM. Magnetic resonance imaging assessment of function in male endurance athletes and untrained individuals determined
the severity of mitral regurgitation. Comparison with invasive techniques. by magnetic resonance imaging. J Am Coll Cardiol 40: 1856 –1863, 2002.
Circulation 92: 1151–1158, 1995. 34. Sun B, Ma JZ, Yong YH, Lv YY. The upper limit of physiological
18. Iwasaki K, Zhang R, Zuckerman JH, Levine BD. Dose-response cardiac hypertrophy in elite male and female athletes in China. Eur J Appl
relationship of the cardiovascular adaptation to endurance training in Physiol 101: 457–463, 2007.
healthy adults: how much training for what benefit? J Appl Physiol 95: 35. Tipton KD, Witard OC. Protein requirements and recommendations for
1575–1583, 2003. athletes: relevance of ivory tower arguments for practical recommenda-
19. Jarvis SS, Levine BD, Prisk GK, Shykoff BE, Elliott AR, Rosow E, tions. Clin Sports Med 26: 17–36, 2007.
Blomqvist CG, Pawelczyk JA. Simultaneous determination of the accu- 36. Utomi V, Oxborough D, Whyte GP, Somauroo J, Sharma S, Shave R,
racy and precision of closed-circuit cardiac output rebreathing techniques. Atkinson G, George K. Systematic review and meta-analysis of training
J Appl Physiol 103: 867–874, 2007. mode, imaging modality and body size influences on the morphology and
20. Jenkins C, Bricknell K, Chan J, Hanekom L, Marwick TH. Compar- function of the male athlete’s heart. Heart 99: 1727–1733, 2013.
ison of two- and three-dimensional echocardiography with sequential 37. Vigil J. Road To The Top. Albuquerque, NM: Creative Designs, 1995.
magnetic resonance imaging for evaluating left ventricular volume and 38. Vingren JL, Kraemer WJ, Ratamess NA, Anderson JM, Volek JS,
ejection fraction over time in patients with healed myocardial infarction. Maresh CM. Testosterone physiology in resistance exercise and training:
Am J Cardiol 99: 300 –306, 2007. the up-stream regulatory elements. Sports Med 40: 1037–1053, 2010.
21. Katz J, Milliken MC, Stray-Gundersen J, Buja LM, Parkey RW, 39. Vuille C, Weyman A. General considerations, assessment of chamber
Mitchell JH, Peshock RM. Estimation of human myocardial mass with size and function. In: Principles and Practices of Echocardiography,
MR imaging. Radiology 169: 495–498, 1988. edited by Weyman AE. Philadelphia, PA: Lea and Febiger, 1994, p.
22. Koenig H, Goldstone A, Lu CY. Testosterone-mediated sexual dimor- 575–624.
phism of the rodent heart. Ventricular lysosomes, mitochondria, and cell 40. Whyte GP, George K, Sharma S, Firoozi S, Stephens N, Senior R,
growth are modulated by androgens. Circ Res 50: 782–787, 1982. McKenna WJ. The upper limit of physiological cardiac hypertrophy in
23. Konhilas JP, Chen H, Luczak ED, McKee LA, Regan J, Watson PA, elite male and female athletes: the British experience. Eur J Appl Physiol
Stauffer BL, Khalpey ZI, McKinsey TA, Horn TR, LaFleur B, Lein- 92: 592–597, 2004.
wand LA. Diet and sex modify exercise and cardiac adaptation in the 41. Wilmore JH, Behnke AR. An anthropometric estimation of body density
mouse. Am J Physiol Heart Circ Physiol 308: H135–H145, 2015. and lean body weight in young men. J Appl Physiol 27: 25–31, 1969.
J Appl Physiol • doi:10.1152/japplphysiol.00092.2015 • www.jappl.org
Vous aimerez peut-être aussi
- Shoe Dog: A Memoir by the Creator of NikeD'EverandShoe Dog: A Memoir by the Creator of NikeÉvaluation : 4.5 sur 5 étoiles4.5/5 (537)
- Eagle Syndrome Managed by Pulsed Radiofrequency TreatmentDocument11 pagesEagle Syndrome Managed by Pulsed Radiofrequency TreatmentDusan OrescaninPas encore d'évaluation
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeD'EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeÉvaluation : 4 sur 5 étoiles4/5 (5794)
- Covid19 Rapid Guideline Pneumonia in Adults in The CommunityDocument15 pagesCovid19 Rapid Guideline Pneumonia in Adults in The CommunityDusan OrescaninPas encore d'évaluation
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceD'EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceÉvaluation : 4 sur 5 étoiles4/5 (895)
- Inhaled Budesonide in The Treatment of Early COVID-19Document10 pagesInhaled Budesonide in The Treatment of Early COVID-19Dusan OrescaninPas encore d'évaluation
- The Yellow House: A Memoir (2019 National Book Award Winner)D'EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Évaluation : 4 sur 5 étoiles4/5 (98)
- Prescribing Tables To Guide Decision Making About AntibioticDocument2 pagesPrescribing Tables To Guide Decision Making About AntibioticDusan OrescaninPas encore d'évaluation
- Grit: The Power of Passion and PerseveranceD'EverandGrit: The Power of Passion and PerseveranceÉvaluation : 4 sur 5 étoiles4/5 (588)
- Patient Pathway OPD CLINICS - COVID-19 MAR 2020 PDFDocument1 pagePatient Pathway OPD CLINICS - COVID-19 MAR 2020 PDFDusan OrescaninPas encore d'évaluation
- The Little Book of Hygge: Danish Secrets to Happy LivingD'EverandThe Little Book of Hygge: Danish Secrets to Happy LivingÉvaluation : 3.5 sur 5 étoiles3.5/5 (400)
- BR J Sports Med-2005-Pigozzi-527-31Document6 pagesBR J Sports Med-2005-Pigozzi-527-31Dusan OrescaninPas encore d'évaluation
- The Emperor of All Maladies: A Biography of CancerD'EverandThe Emperor of All Maladies: A Biography of CancerÉvaluation : 4.5 sur 5 étoiles4.5/5 (271)
- Exercise and Bariatric SurgeryDocument9 pagesExercise and Bariatric SurgeryDusan OrescaninPas encore d'évaluation
- Never Split the Difference: Negotiating As If Your Life Depended On ItD'EverandNever Split the Difference: Negotiating As If Your Life Depended On ItÉvaluation : 4.5 sur 5 étoiles4.5/5 (838)
- Daniel Medina BarselonaDocument24 pagesDaniel Medina BarselonaDusan OrescaninPas encore d'évaluation
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyD'EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyÉvaluation : 3.5 sur 5 étoiles3.5/5 (2259)
- Article Citation Cardio Testovi Kod MraDocument1 pageArticle Citation Cardio Testovi Kod MraDusan OrescaninPas encore d'évaluation
- On Fire: The (Burning) Case for a Green New DealD'EverandOn Fire: The (Burning) Case for a Green New DealÉvaluation : 4 sur 5 étoiles4/5 (74)
- SOAP Notes Format in EMR: SOAP Stands For Subjective, Objective, Assessment, and PlanDocument2 pagesSOAP Notes Format in EMR: SOAP Stands For Subjective, Objective, Assessment, and PlanNick Jacob100% (7)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureD'EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureÉvaluation : 4.5 sur 5 étoiles4.5/5 (474)
- Sudden Cardiac Death IRELANDDocument8 pagesSudden Cardiac Death IRELANDDusan OrescaninPas encore d'évaluation
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryD'EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryÉvaluation : 3.5 sur 5 étoiles3.5/5 (231)
- Exercise Prescription Obesity VaznoooDocument4 pagesExercise Prescription Obesity VaznoooDusan OrescaninPas encore d'évaluation
- Team of Rivals: The Political Genius of Abraham LincolnD'EverandTeam of Rivals: The Political Genius of Abraham LincolnÉvaluation : 4.5 sur 5 étoiles4.5/5 (234)
- Physical Therapy After Bariatric Surgery VaznooooooooooooDocument1 pagePhysical Therapy After Bariatric Surgery VaznooooooooooooDusan OrescaninPas encore d'évaluation
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaD'EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaÉvaluation : 4.5 sur 5 étoiles4.5/5 (266)
- Mental HealthDocument10 pagesMental Healthleydi nina100% (2)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersD'EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersÉvaluation : 4.5 sur 5 étoiles4.5/5 (345)
- ECR 2022 ProgrammeDocument1 126 pagesECR 2022 ProgrammejbmbritoPas encore d'évaluation
- Francis N. Ramirez, MDDocument9 pagesFrancis N. Ramirez, MDPridas GidPas encore d'évaluation
- The Unwinding: An Inner History of the New AmericaD'EverandThe Unwinding: An Inner History of the New AmericaÉvaluation : 4 sur 5 étoiles4/5 (45)
- Rosuvastatin: Role in Secondary Prevention of Cardiovascular DiseaseDocument5 pagesRosuvastatin: Role in Secondary Prevention of Cardiovascular Diseasenasir uddinPas encore d'évaluation
- Chapter 09 - Aortic StenosisDocument9 pagesChapter 09 - Aortic StenosisAndrada CatrinoiuPas encore d'évaluation
- Bloodstream Infection MBDocument47 pagesBloodstream Infection MBDarshan Koirala100% (1)
- Lequesne Knee ScoreDocument3 pagesLequesne Knee ScoreBagus PutraPas encore d'évaluation
- Position S: Pratiksha RaiDocument49 pagesPosition S: Pratiksha RaiJoanne Cristie TolopiaPas encore d'évaluation
- Full Download Book Connectomic Deep Brain Stimulation PDFDocument41 pagesFull Download Book Connectomic Deep Brain Stimulation PDFgeorge.redfield696100% (15)
- G.R. No. 165279, June 7, 2011.: Consent Rubi Li vs. SolimanDocument17 pagesG.R. No. 165279, June 7, 2011.: Consent Rubi Li vs. SolimanJOAHNNA PAULA CORPUZPas encore d'évaluation
- UELS NIH Research Plan CompressedDocument36 pagesUELS NIH Research Plan CompressedKunal JaisinghaniPas encore d'évaluation
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreD'EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreÉvaluation : 4 sur 5 étoiles4/5 (1090)
- ESPEN Practical Guideline Clinical Nutrition in SurgeryDocument17 pagesESPEN Practical Guideline Clinical Nutrition in SurgeryMaríaJoséVegaPas encore d'évaluation
- Beximco PharmaDocument8 pagesBeximco PharmaShakilfunkyPas encore d'évaluation
- Jurnal NeuroDocument6 pagesJurnal NeuroSiti WahyuningsihPas encore d'évaluation
- Atrial FlutterDocument16 pagesAtrial Flutterapi-527603714100% (1)
- Use of Liquid ParaffinDocument7 pagesUse of Liquid ParaffinNada Milic - PavlicevicPas encore d'évaluation
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)D'EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Évaluation : 4.5 sur 5 étoiles4.5/5 (121)
- Pathophysiology of Upper Gastrointestinal BleedingDocument1 pagePathophysiology of Upper Gastrointestinal BleedingkimmybapkiddingPas encore d'évaluation
- Multidimensional Effects of Shirodhara On Psycho-Somatic Axis in The Management of Psycho-Physiological DisordersDocument9 pagesMultidimensional Effects of Shirodhara On Psycho-Somatic Axis in The Management of Psycho-Physiological DisordersMatt AldridgePas encore d'évaluation
- 01.classification and Causes of Animal DiseasesDocument16 pages01.classification and Causes of Animal DiseasesDickson MahanamaPas encore d'évaluation
- Bangalore International Academy N.S.V.K.®: Name: Class: SubectDocument18 pagesBangalore International Academy N.S.V.K.®: Name: Class: SubectAjay RajPas encore d'évaluation
- WTG Morton PDFDocument7 pagesWTG Morton PDFrkPas encore d'évaluation
- FIQ - Proliferative Diabetic RetinopathyDocument35 pagesFIQ - Proliferative Diabetic RetinopathyHikban FiqhiPas encore d'évaluation
- VEAL CHOP With Interventions and OutcomesDocument1 pageVEAL CHOP With Interventions and Outcomesayngn13Pas encore d'évaluation
- Her Body and Other Parties: StoriesD'EverandHer Body and Other Parties: StoriesÉvaluation : 4 sur 5 étoiles4/5 (821)
- 5.case Study: Effects of Homeopathic Medicines in AdultsDocument2 pages5.case Study: Effects of Homeopathic Medicines in AdultsAMEEN ARTSPas encore d'évaluation
- 9 - Clinical Management (STRATOG 2015 SBAs)Document12 pages9 - Clinical Management (STRATOG 2015 SBAs)w yPas encore d'évaluation
- NCP ShockDocument5 pagesNCP ShockJanina Patricia BuddlePas encore d'évaluation
- Piet AlDocument6 pagesPiet AlKiara NurmathiasPas encore d'évaluation
- DDB Board Reg No. 7, S. 2019Document72 pagesDDB Board Reg No. 7, S. 2019keith tanueco100% (1)
- IV. Antiarrhythmic Drugs: PHRM 537 Summer 2020Document19 pagesIV. Antiarrhythmic Drugs: PHRM 537 Summer 2020SaulPas encore d'évaluation
- Ectopic PregnancyDocument7 pagesEctopic PregnancyDeepshikha MahapatraPas encore d'évaluation