Académique Documents
Professionnel Documents
Culture Documents
Pediatric Journal
Transféré par
michael halimTitre original
Copyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
Pediatric Journal
Transféré par
michael halimDroits d'auteur :
Formats disponibles
Paediatrica Indonesiana
p-ISSN 0030-9311; e-ISSN 2338-476X; Vol.58, No.3(2018). p. 146-50; doi: http://dx.doi.org/10.14238/pi58.3.2018.146-50
Case Report
West syndrome and mosaic trisomy 13: a case report
Hechmi Ben Hamouda1, Habib Soua1, Mohamed Dogui2, Hassine Hamza3,
Mohamed Tahar Sfar1
T
risomy 13, or Patau syndrome, is a rare chromosomal
disorder characterized by a triad of cleft lip and palate,
The Case
postaxial polydactyly, and microphthalmia, with an
incidence ranging between 1/5,000 and 1/20,000 A 4-month-old girl followed from birth for mosaic
births.1 Most patients (80%) with Patau syndrome have complete trisomy 13 developed repetitive flexor spasms, and was
trisomy 13. Mosaic trisomy 13 is very rare; it occurs in only 5% hospitalized in the Department of Paediatrics. She
of all patients with the trisomy 13 phenotype.2 Trisomy 13 is
a clinically severe entity, and 90 to 95% of patients born with was the seventh child of healthy, non-consanguineous
this syndrome do not survive beyond one year of life. However, parents with 3 girls and 3 boys in good health. Her
patients with mosaic trisomy 13 usually have longer survival mother was 39 year old, the course of pregnancy
and less severe phenotype compared to patients with complete was normal, and antenatal ultrasounds showed
trisomy 13. Malformations mainly affect midline development,
with a high frequency of central nervous system involvement. The no anomalies. She was delivered vaginally at 42
presence of central nervous system malformations is important weeks of gestation without incident. Apgar scores
as a predictive factor of survival.1,3 It is well known that the at l and 5 min were 8 and 9, respectively. She had
incidence of epilepsy is higher in children with Patau syndrome
dysmorphic features suggesting Patau syndrome with
than in the general population, and West syndrome or infantile
spasms have been rarely reported in these children.1,4,5 Prior to our microcephaly, hypertelorism, upslanting palpebral
report, there has been no case report of West syndrome associated fissures, epicanthal folds, broad nasal bridge, bilateral
with mosaic trisomy 13. The association of West syndrome with cleft lip and palate, and short neck (Figure 1).
trisomy 13 is considered a symptomatic West syndrome because
of preexisting psychomotor development delay and the poor
Transfontanellar ultrasound, abdominal ultrasound,
prognosis in most of these children.6 We report here the first case and echocardiogram were normal. The cytogenetic
of West syndrome in a girl with mosaic trisomy 13 and discuss the examination of lymphocytes demonstrated a mosaicism
clinical characteristics and prognosis of this association.[Paediatr of 47, XX, + 13 [6] /46, XX [10].
Indones. 2018;58:146-50; doi: http://dx.doi.org/10.14238/
pi58.3.2018.146-50 ].
Keywords: West syndrome; Patau syndrome;
mosaic trisomy 13; prognosis
From the Department of Pediatrics and Neonatology, Tahar Sfar University
Hospital, 5111 Mahdia1, Department of Neurophysiology, Sahloul
University Hospital, 4000 Sousse2, and Department of Radiology, Tahar
Sfar University Hospital, 5111 Mahdia3, Tunisia.
Reprint requests to: DR. Hechmi Ben Hamouda, Department of
Pediatrics and Neonatology, Tahar Sfar University Hospital, 5111 Mahdia,
Tunisia. Tel. 00 216 98 688 475 ; Fax. 00 216 73 671 579; E-mail: hechmi.
benhamouda@rns.tn.
146 • Paediatr Indones, Vol. 58, No. 3, May 2018
Hechmi Ben Hamounda et al.: A case report of West syndrome and mosaic trisomy 13
Her psychomotor development at 3 months developmental delay, and tetraparesia. Her spasms
was abnormal with hypotonia and poor head control. disappeared with Vigabatrin. She died of pneumonia
Thyroid function was normal. At 4 months, she at the age of 26 months.
had flexor spasms several times a day, occurring in
series, psychomotor developmental delay, and axial
hypotonia. The EEG showed hypsarrhythmia. She
was diagnosed as having West syndrome, and treated
with Vigabatrin at a dose of 150 mg/kg/day. Vigabatrin
therapy was immediately effective with good clinical
control of spasms, but the EEG monitoring after
one month was unchanged showing persistent
hypsarrhythmia. Brain magnetic resonance imaging
(MRI) showed lobar holoprosencephaly and callosal
agenesis (Figure 2).
Because of her severe psychomotor delay, she Figure 2. Brain MRI showing (A) holoprosencephaly
and (B) callosal agenesis
received nasogastric tube feedings at home and
the cleft lip and palate were untreatable. The first
intervention of the cleft lip and palate was made at Discussion
16 months of age, but the post-operative course was
marked by dropping of sutures. After a follow-up of 2 Mosaic trisomy 13, or mosaic Patau syndrome occurs
years, the patient had hypotonia, feeding difficulties, when there is a portion of trisomic cells for an entire
severe growth retardation, microcephaly, severe chromosome 13, while the remaining body cells are
euploid.7 The typical phenotype of complete trisomy
13 is usually associated with characteristic physical
anomalies such as microcephaly, scalp defects,
holoprosencephaly, microphthalmia, orofacial clefting,
congenital heart defects, polydactyly, and profound
mental retardation.3 However, the phenotype of
mosaic trisomy 13 varies widely, which renders clinical
diagnosis difficult. Some patients may have the
typical phenotype of trisomy 13 with neonatal death,
while others may have few dysmorphic features and
prolonged survival. The reason for this variation is that
the phenotype changes according to the distribution
of abnormal cells in specific tissues.7 We clinically
diagnosed our patient as having complete trisomy 13
by typical features, but chromosomal analysis revealed
mosaic trisomy 13.
In the general population of children, the
incidence of West syndrome ranges from 0.6 to 4.5
per 10,000 live births.6,8 However, this incidence is
much higher in children with Patau syndrome. It has
been reported that 25 to 70% of patients with Patau
syndrome have epilepsy, and 62.5% of these patients
have epileptic spasms. They may present at an early
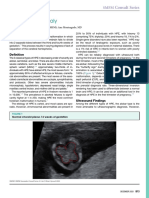
Figure 1. Facial view of the patient at birth showing age with myoclonic jerks and/or infantile spasms.1,3,7
hypertelorism with a large nasal bridge and a bilat- Spagnoli et al. reported that the age at onset of infantile
eral cleft lip and palate. spasms in 8 patients with trisomy 13 ranged from 2
Paediatr Indones, Vol. 58, No. 3, May 2018 • 147
Hechmi Ben Hamounda et al.: A case report of West syndrome and mosaic trisomy 13
months to 3 years and 9 months. West syndrome began axial contraction, predominantly in the upper limbs,
during the first year of life in 50% of these patients.1 with upper deviation of the eyes. In their cohort of 8
Our patient had infantile spasms at 4 months. patients with Patau syndrome, Spagnoli et al. found
The higher risk of West syndrome in Patau a high prevalence of spasms and photic-induced
syndrome is shared with numerous other chromosomal myoclonic jerks and confirmed that photosensitivity
abnormalities as in Down syndrome, 9 but the manifested at an unusually early age of onset.1 In our
mechanism is not yet clear. According to the literature, patient, West syndrome was clinically diagnosed from
two different hypotheses have been established.1 the flexor spasms that occurred several times a day,
The first hypothesis is based on the presence of which began at an early age.
malformations of cortical development in these Medical treatment of infantile spasms should
conditions of mosaic trisomy 13. Malformations mainly be effective and initiated as early as possible.
affect midline development, with a high frequency of Evaluation of treatment effectiveness includes
central nervous system involvement, including corpus cessation of spasms, resolution of hypsarrhythmia
callosum anomalies, ventriculomegaly, neural tube on the EEG, and reduction of the cognitive decline
defects, hydrocephalus, holoprosencephaly, cerebellar associated with epilepsy. Currently, vigabatrin and
dysplasia, olfactory aplasia, and cortical dysplasia. adrenocorticotropic hormone (ACTH) are the only
Interestingly, co-existing reflex and spontaneous drugs approved to suppress clinical spasms and abolish
seizures have been described in the setting of cortical hypsarrhythmia. Past studies have reported different
malformations.3,10,11 Brain MRI is recommended to treatment protocols, but the large majority of children
facilitate the etiologic diagnosis of infantile spasms with infantile spasms received vigabatrin as first line
in patients with Patau syndrome.4,6 In our patient, treatment and ACTH as second line treatment.6,14
the brain MRI showed lobar holoprosencephaly and Epileptic spasms in children with Patau syndrome were
callosal agenesis. The second hypothesis involves genes described as well-controlled with anticonvulsants.5
on chromosome 13 for epilepsy and photosensitivity, However, Spagnoli et al. presented evidence of
and is supported by past research studies.1,12 Of difficult seizure control in two patients: one patient
interest is the recent indication of glypican-5 (GPC5) who needed multi-drug therapy and another patient
as a candidate gene for epilepsy inside the 13q31.3 who at clinical follow-up at 2 years of age experienced
locus. Speculation has been made about a contribution around 20 episodes of myoclonic seizures/day, despite
of disrupted axon guidance and synaptic formation high doses of sodium valproate. Neither of these
in the genesis of epilepsy and/or brain malformations patients underwent brain imaging.1 In our patient,
in trisomy 13. However, at present, this hypothesis vigabatrin was immediately effective, with a complete
remains unproven.1,12 resolution of clinical spasms during the first two years.
The diagnosis of West syndrome is often easy The response to treatment has been shown to be
when infantile spasms are associated with arrest significantly better when initiated less than 6 weeks
or regression of psychomotor development, and a after the diagnosis of infantile spasms.15 These results
specific EEG pattern of hypsarrhythmia.8 The clinical suggest that early diagnosis and rapid treatment can
symptoms of infantile spasms are very different from improve longer-term prognosis of infantile spasms in
any other type of seizure because of the absence of children with Patau syndrome.
paroxysmal motor phenomena, such as convulsions Despite early diagnosis and rapid initiation of
or loss of consciousness. This lack of typical seizure effective treatment, West syndrome in children is still
phenomena may lead to initial misdiagnosis of associated with a poor, long-term prognosis. Long-
infantile spasms by pediatricians at the first medical term follow-up showed that 60% of the children had
consultation. Auvin et al. reported that approximately drug-resistant epilepsy and that 75% had delayed
one-third of infants with infantile spasms were not psychomotor development.16 Children with West
suspected of having epilepsy during the first medical syndrome and evidence of pre-existing developmental
consultation.13 Infantile spasms in infants are usually delay or neurological abnormalities, as in our patient,
symmetrical and manifest as repetitive flexor, extensor, have a worse prognosis, poorer response to treatment,
or flexor–extensor spasms, with sudden and brief and less favorable developmental outcome.6
148 • Paediatr Indones, Vol. 58, No. 3, May 2018
Hechmi Ben Hamounda et al.: A case report of West syndrome and mosaic trisomy 13
It is important to acknowledge that the prognosis Funding acknowledgment
of Patau syndrome is very poor and most patients die
soon after birth because of severe congenital heart The authors received no specific grant from any funding agency
disease and brain anomalies. Almost 50% of cases in the public, commercial, or not-for-profit sectors.
die in the first month, and 90 to 95% of patients do
not survive beyond one year of life. In the absence
of severe cardiac and cerebral malformations, in References
particular the absence of holoprosencephaly, 5 to
10% of patients with trisomy 13 live longer than one 1. Spagnoli C, Kugathasan U, Brittain H, Boyd SG. Epileptic
year.17,18 However, patients with mosaic trisomy 13 spasms and early-onset photosensitive epilepsy in Patau
usually have longer survival and less severe phenotype syndrome: an EEG study. Brain Dev. 2015;37:704-13.
compared to patients with complete trisomy 13. 2. Aypar E, Yildirim MS, Sert A, Ciftci I, Odabas D. A girl with
There have been several cases of long survival in metopic synostosis and trisomy 13 mosaicism: case report and
patients with Patau syndrome, ranging from 3 to 38 review of the literature. Am J Med Genet A. 2011;155A:638-
years old.1,3,10,18,19 Most of these survivors suffered 41.
from severe psychomotor delay, feeding difficulties, 3. Hsu HF, Hou JW. Variable expressivity in Patau syndrome is
profound learning disability, seizures, as well as motor not all related to trisomy 13 mosaicism. Am J Med Genet A.
and mental deficits.1,10,18 The patients who received 2007;143A:1739-48.
intensive treatments survived longer and had better 4. Osborne JP, Lux AL, Edwards SW, Hancock E, Johnson AL,
prognoses.20,21 Although our patient had mosaic Kennedy CR, et al. The underlying etiology of infantile spasms
trisomy 13 syndrome, the control examination at 2 (West syndrome): information from the United Kingdom
years of age showed severe developmental delay and Infantile Spasms Study (UKISS) on contemporary causes
tetraparesia. and their classification. Epilepsia. 2010;51:2168-74.
The spectrum of phenotypic variations in 5. Yamanouchi H, Imataka G, Nakagawa E, Nitta A, Suzuki
mosaic trisomy 13 cases is broad. Therefore, genetic N, Hirao J, et al. An analysis of epilepsy with chromosomal
counseling of expecting parents with prenatally abnormalities. Brain Dev. 2005;27:370-7.
diagnosed mosaic trisomy 13 remains difficult. The 6. Pellock JM, Hrachovy R, Shinnar S, Baram TZ, Bettis D,
majority of physical anomalies tend to be mild and Dlugos DJ, et al. Infantile spasms: a US consensus report.
non-life-threatening. Developmental delays and/or Epilepsia. 2010;51:2175-89.
mental retardation, while being quite common, are 7. Pachajoa H, Meza Escobar LE. Mosaic trisomy 13 and a sacral
not present universally. In all children with Patau appendage. BMJ Case Rep. 2013;31:2013.
syndrome, early developmental intervention and 8. Hino-Fukuyoa N, Haginoyaa K, Iinumaa K, Uematsua M,
continued follow-up is essential for maximizing their Tsuchiyaa S. Neuroepidemiology of West syndrome and early
cognitive skills.10,22 infantile epileptic encephalopathy in Miyagi Prefecture,
Patau syndrome patients are at increased risk Japan. Epilepsy Res. 2009;87:299-301.
of seizures. They may present at an early age with 9. Sanmaneechai O, Sogawa Y, Silver W, Ballaban-Gil
infantile spasms, but the spasms might not be easily K, Moshé SL, Shinnar S. Treatment outcomes of West
controlled with antiepileptic medication.1 This report syndrome in infants with Down syndrome. Pediatr Neurol.
describes the clinical characteristics and prognosis of 2013;48:42-7.
a patient with mosaic trisomy 13 who survived for a 10. Griffith CB, Vance GH, Weaver DD. Phenotypic variability
relatively prolonged period and developed infantile in trisomy 13 mosaicism: two new patients and literature
spasms at an early age that were well-controlled with review. Am J Med Genet A. 2009;149A:1346-58.
anticonvulsants. 11. Palmini A, Halasz P, Scheffer IE, Takahashi Y, Jimenez AP,
Dubeau F, et al. Reflex seizures in patients with malformations
of cortical development and refractory epilepsy. Epilepsia.
Conflict of interest 2005;46:1224-34.
12. Ribacoba R, Menendez-Gonzalez M, Hernando I, Salas
None declared. J, Giros ML. Partial trisomy 13q22-qter associated to
Paediatr Indones, Vol. 58, No. 3, May 2018 • 149
Hechmi Ben Hamounda et al.: A case report of West syndrome and mosaic trisomy 13
leukoencephalopathy and late onset generalised epilepsy. Int 18. Fogu G, Maserati E, Cambosu F, Moro MA, Poddie F, Soro G,
Arch Med. 2008;1:5. et al. Patau syndrome with long survival in a case of unusual
13. Auvin S, Hartman AL, Desnous B, Moreau AC, Alberti C, mosaic trisomy 13. Eur J Med Genet. 2008;51:303-14.
Delanoe C, et al. Diagnosis delay in West syndrome: misdiagnosis 19. Imataka G, Hagisawa S, Nitta A, Hirabayashi H, Suzumura
and consequences. Eur J Pediatr. 2012;171:1695-701. H, Arisaka O. Long-term survival of full trisomy 13 in a 14
14. Wheless JW, Gibson PA, Rosbeck KL, Hardin M, O'Dell year old male: a case report. Eur Rev Med Pharmacol Sci.
C, Whittemore V, et al. Infantile spasms (West syndrome): 2016;20:919-22.
update and resources for pediatricians and providers to share 20. Tsukada K, Imataka G, Suzumura H, Arisaka O. Better
with parents. BMC Pediatr. 2012;12:108. prognosis in newborns with trisomy 13 who received intensive
15. Napuri S, LE Gall E, Dulac O, Chaperon J, Riou F. Factors treatments: a retrospective study of 16 patients. Cell Biochem
associated with treatment lag in infantile spasms. Dev Med Biophys. 2012;63:191-8.
Child Neurol. 2010;52:1164-6. 21. Imataka G, Tsuboi Y, Kano Y, Ogino K, Tsuchioka T,
16. Lagae L, Verhelst H, Ceulemans B, De Meirleir L, Nassogne Ohnishi T, et al. Treatment with mild brain hypothermia for
MC, De Borchgrave V, et al. Treatment and long term cardiopulmonary resuscitation after myoclonic seizures in
outcome in West syndrome: the clinical reality. A multicentre infant with robertsonian type of trisomy 13. Eur Rev Med
follow up study. Seizure. 2010;19:159-64. Pharmacol Sci. 2015;19:2852-5.
17. Rasmussen SA, Wong LY, Yang Q, May KM, Friedman JM. 22. Chen CP. Prenatal diagnosis and genetic counseling for
Population-based analyses of mortality in trisomy 13 and mosaic trisomy 13. Taiwan J Obstet Gynecol. 2010;49:13-
trisomy 18. Pediatrics. 2003;111:777-84. 22.
150 • Paediatr Indones, Vol. 58, No. 3, May 2018
Vous aimerez peut-être aussi
- Writing S.O.a.P. Notes 2nd EdDocument191 pagesWriting S.O.a.P. Notes 2nd Edwebst100% (16)
- SyndromesDocument58 pagesSyndromesLGK maorePas encore d'évaluation
- The Terrorist Inside My Husband's Brain PDFDocument5 pagesThe Terrorist Inside My Husband's Brain PDFraymondnomyarPas encore d'évaluation
- SchizophreniaDocument67 pagesSchizophreniaHazirah Mokhtar100% (1)
- Case Study PaediatricsDocument8 pagesCase Study PaediatricsDaudPas encore d'évaluation
- Critical Care Nurse Skills ChecklistDocument4 pagesCritical Care Nurse Skills ChecklistMichael Silva0% (1)
- Reffered PainDocument26 pagesReffered PainHappy Septianto SPas encore d'évaluation
- Evidence Based Assessment of OCDDocument17 pagesEvidence Based Assessment of OCDDanitza YhovannaPas encore d'évaluation
- Guided Prep Pack - Neet Mds 2021-22Document13 pagesGuided Prep Pack - Neet Mds 2021-22Annu SharmaPas encore d'évaluation
- Down Syndrome PDFDocument7 pagesDown Syndrome PDFpaola100% (1)
- Poster Thanaporic Dysplasia KOGI 2018Document1 pagePoster Thanaporic Dysplasia KOGI 2018Yudha GanesaPas encore d'évaluation
- Congenital Toxoplasmosis Associated With Severe Intracerebral Calcification and West SyndromeDocument3 pagesCongenital Toxoplasmosis Associated With Severe Intracerebral Calcification and West SyndromeDevina Rossita HapsariPas encore d'évaluation
- Thanatoporic Dysplasia FIXDocument7 pagesThanatoporic Dysplasia FIXYudha GanesaPas encore d'évaluation
- Neuroradiological Findings of Trisomy 13 in A Rare Long-Term SurvivorDocument3 pagesNeuroradiological Findings of Trisomy 13 in A Rare Long-Term Survivorchristian roblesPas encore d'évaluation
- Patau SindromDocument4 pagesPatau SindromOgnjen IvkovićPas encore d'évaluation
- FTPDocument2 pagesFTPDesta FransiscaPas encore d'évaluation
- 2479 ArticleDocument5 pages2479 Articleclbenitez52Pas encore d'évaluation
- 1 s2.0 S0738081X14002375 MainDocument13 pages1 s2.0 S0738081X14002375 Mainmarisa araujoPas encore d'évaluation
- Fragile X Syndrome (Martin-Bell Syndrome)Document6 pagesFragile X Syndrome (Martin-Bell Syndrome)yudhi kurniawanPas encore d'évaluation
- Triple X Syndrome With A Rare Finding: Cleft Palate: Case ReportDocument3 pagesTriple X Syndrome With A Rare Finding: Cleft Palate: Case ReportDewi JayantiPas encore d'évaluation
- Reyes - Unit 2 (Part 2)Document4 pagesReyes - Unit 2 (Part 2)Justine Ericca ReyesPas encore d'évaluation
- Evidence For The Oocyte Mosaicism Selection Model On The Origin of Patau Syndrome (Trisomy 13)Document7 pagesEvidence For The Oocyte Mosaicism Selection Model On The Origin of Patau Syndrome (Trisomy 13)christian roblesPas encore d'évaluation
- Prevalence of Prader-Willi Syndrome Among Infants With Hypotonia-2014Document4 pagesPrevalence of Prader-Willi Syndrome Among Infants With Hypotonia-2014nikos.alexandrPas encore d'évaluation
- Brain TumorsDocument12 pagesBrain Tumors36Kushal saNdHuPas encore d'évaluation
- Sindrom PatauDocument12 pagesSindrom PatauIoana PaulaPas encore d'évaluation
- Potter'S Syndrome: A Study of 15 Patients: Original ArticleDocument4 pagesPotter'S Syndrome: A Study of 15 Patients: Original ArticleyanuarizkaPas encore d'évaluation
- Discussion: Aspiration DisplayedDocument4 pagesDiscussion: Aspiration DisplayedmartinPas encore d'évaluation
- Tsukada 2012Document8 pagesTsukada 2012jijiPas encore d'évaluation
- SRM College of PhysiotherapyDocument24 pagesSRM College of PhysiotherapyPONMATHI P FACULTY OF PHYSIOTHERAPYPas encore d'évaluation
- Chen Et Al 2007 Prader Willi Syndrome An Update and Review For The Primary PediatricianDocument12 pagesChen Et Al 2007 Prader Willi Syndrome An Update and Review For The Primary Pediatricianvcnflga08Pas encore d'évaluation
- Phenotypic Analysis of A Case of "3MC Syndrome" With Review of LiteratureDocument3 pagesPhenotypic Analysis of A Case of "3MC Syndrome" With Review of LiteratureBOHR International Journal of Current Research in Optometry and Ophthalmology (BIJCROO)Pas encore d'évaluation
- Orphanet Journal of Rare Diseases: Jacobsen SyndromeDocument10 pagesOrphanet Journal of Rare Diseases: Jacobsen SyndromeMuhammad RezaPas encore d'évaluation
- Trisomy 13Document9 pagesTrisomy 13caldylanPas encore d'évaluation
- Medip, IJCP-1422 CDocument3 pagesMedip, IJCP-1422 CdsagemaverickPas encore d'évaluation
- 46 Onankpa EtalDocument3 pages46 Onankpa EtaleditorijmrhsPas encore d'évaluation
- Noonan Syndrome (Am Fam Physician. 2014 PDFDocument7 pagesNoonan Syndrome (Am Fam Physician. 2014 PDFKhalila DiantiPas encore d'évaluation
- HoloprosencephalyDocument4 pagesHoloprosencephalynskhldPas encore d'évaluation
- Common Dysmorphic Syndromes in The NICUDocument12 pagesCommon Dysmorphic Syndromes in The NICUDaniel PuertasPas encore d'évaluation
- Symmetrical Thalamic Lesions in The Newborn: A Case SeriesDocument8 pagesSymmetrical Thalamic Lesions in The Newborn: A Case SeriesValentina RusuPas encore d'évaluation
- Fragile X SyndromeDocument2 pagesFragile X SyndromeadamPas encore d'évaluation
- Santos Et Al 2011. Hearing Loss and Airway Problems in Children With MucopolysaccharidosesDocument7 pagesSantos Et Al 2011. Hearing Loss and Airway Problems in Children With MucopolysaccharidosesBoPas encore d'évaluation
- Seminar: Christine Léauté-Labrèze, John I Harper, Peter H HoegerDocument10 pagesSeminar: Christine Léauté-Labrèze, John I Harper, Peter H HoegerMayaSuyataPas encore d'évaluation
- Caso de EncefalitisDocument4 pagesCaso de EncefalitisJonathan CuevaPas encore d'évaluation
- Cog NTDocument11 pagesCog NTFabiolaQuijaitePas encore d'évaluation
- CebocephalyDocument12 pagesCebocephalyUser AbPas encore d'évaluation
- Davis 2003Document9 pagesDavis 2003Apotik ApotekPas encore d'évaluation
- Failure To ThriveDocument3 pagesFailure To ThrivefernandoPas encore d'évaluation
- Journal of Oral Biology and Craniofacial Research: N.M. Al-Namnam, F. Hariri, M.K. Thong, Z.A. Rahman TDocument3 pagesJournal of Oral Biology and Craniofacial Research: N.M. Al-Namnam, F. Hariri, M.K. Thong, Z.A. Rahman TPrima AndisetyantoPas encore d'évaluation
- Chapter 31 Neuroblastoma - 2012 - Pediatric Surgery Seventh Edition 70856Document18 pagesChapter 31 Neuroblastoma - 2012 - Pediatric Surgery Seventh Edition 70856valeria falceanuPas encore d'évaluation
- CPDocument10 pagesCPAnonymous vnv6QFPas encore d'évaluation
- 8 PDFDocument10 pages8 PDFYusmiatiPas encore d'évaluation
- Clinical Ophthalmology: Clinical Presentation and Management of Congenital PtosisDocument25 pagesClinical Ophthalmology: Clinical Presentation and Management of Congenital PtosisEnjelinmariesca KaruriPas encore d'évaluation
- Very Severe Spinal Muscular Atrophy (Type 0) : A Report of Three CasesDocument4 pagesVery Severe Spinal Muscular Atrophy (Type 0) : A Report of Three CasesRafaela Queiroz MascarenhasPas encore d'évaluation
- MedulloblastomaDocument17 pagesMedulloblastomabrown_chocolate87643Pas encore d'évaluation
- Van Wyck GrumbachDocument2 pagesVan Wyck Grumbachwanwan_adongPas encore d'évaluation
- Intacranial Complications of Chronic Suppurative Otitis Media, Ottico-Antral TypeDocument4 pagesIntacranial Complications of Chronic Suppurative Otitis Media, Ottico-Antral TypeRio OktabyantoroPas encore d'évaluation
- Prenatal Diagnosis of Cleft Lip and Cleft Lip Palate Case ReportDocument5 pagesPrenatal Diagnosis of Cleft Lip and Cleft Lip Palate Case ReportManjirou SanoPas encore d'évaluation
- MedBack CPDocument5 pagesMedBack CPJulia Rei Eroles IlaganPas encore d'évaluation
- Thanatophoric Dysplasia, An Enigmatic Dilemma: A Case ReportDocument3 pagesThanatophoric Dysplasia, An Enigmatic Dilemma: A Case ReportRioPas encore d'évaluation
- Jurnal 2Document10 pagesJurnal 2lomba Panah Dies UnsriPas encore d'évaluation
- 81 179 1 SMDocument5 pages81 179 1 SMconcozPas encore d'évaluation
- Pituitary Tumour Apoplexy Within Prolactinomas in Children A More Aggressive ConditionDocument6 pagesPituitary Tumour Apoplexy Within Prolactinomas in Children A More Aggressive ConditionTony Miguel Saba SabaPas encore d'évaluation
- 104 FullDocument5 pages104 FullSamPas encore d'évaluation
- Ref 15Document9 pagesRef 15Tiago BaraPas encore d'évaluation
- Stroke and Cerebrovascular Disease in ChildhoodD'EverandStroke and Cerebrovascular Disease in ChildhoodVijeya GanesanPas encore d'évaluation
- Pediatric JournalDocument5 pagesPediatric Journalmichael halimPas encore d'évaluation
- JurdingDocument6 pagesJurdingsiti hazard aldinaPas encore d'évaluation
- Menstrual Cycle Patterns of Indonesian Adolescents PDFDocument5 pagesMenstrual Cycle Patterns of Indonesian Adolescents PDFKopi BotolPas encore d'évaluation
- Menstrual Cycle Patterns of Indonesian Adolescents PDFDocument5 pagesMenstrual Cycle Patterns of Indonesian Adolescents PDFKopi BotolPas encore d'évaluation
- Correlation Between Non-Exclusive Breastfeeding and Low Birth Weight To Stunting in ChildrenDocument5 pagesCorrelation Between Non-Exclusive Breastfeeding and Low Birth Weight To Stunting in ChildrenAnonymous hETtEBkk7Pas encore d'évaluation
- APAC Comarision of Registration Guidelines 2014 PDFDocument54 pagesAPAC Comarision of Registration Guidelines 2014 PDFAnu PariyarathPas encore d'évaluation
- 7 Essential Steps of CPRDocument2 pages7 Essential Steps of CPRBea YmsnPas encore d'évaluation
- IMA Monthly Report Form JulyDocument4 pagesIMA Monthly Report Form JulyInternetStudioPas encore d'évaluation
- 811 2Document16 pages811 2almightyx10Pas encore d'évaluation
- Danish Mask StudyDocument1 pageDanish Mask StudyJuana AtkinsPas encore d'évaluation
- Perioperative Nursing: Lecturer: Mr. Renato D. Lacanilao, RN, MANDocument27 pagesPerioperative Nursing: Lecturer: Mr. Renato D. Lacanilao, RN, MANJmarie Brillantes PopiocoPas encore d'évaluation
- Case Study 5 (Respiratory) - COPDDocument6 pagesCase Study 5 (Respiratory) - COPDSamantha AquinoPas encore d'évaluation
- Senior CapstoneDocument6 pagesSenior Capstoneapi-313278667Pas encore d'évaluation
- Rog Final MDDocument5 pagesRog Final MDSaiPas encore d'évaluation
- Cover LetterDocument1 pageCover Letterapi-400385739Pas encore d'évaluation
- MestastaseDocument10 pagesMestastaseCahyono YudiantoPas encore d'évaluation
- Marijuana and EpilepsyDocument17 pagesMarijuana and EpilepsyOmar AntabliPas encore d'évaluation
- Https Cghs - Nic.in Reports View Hospital - JSPDocument36 pagesHttps Cghs - Nic.in Reports View Hospital - JSPRTI ActivistPas encore d'évaluation
- MEdication ErrorsDocument6 pagesMEdication ErrorsBeaCeePas encore d'évaluation
- MHC PDFDocument2 pagesMHC PDFYuvarani AruchamyPas encore d'évaluation
- Revitears Study 2Document16 pagesRevitears Study 2office.hospimedPas encore d'évaluation
- Perineal Urethrostomy PUDocument2 pagesPerineal Urethrostomy PUclara FPas encore d'évaluation
- Introduction To Anaesthesia: Fatiş Altındaş Department of AnesthesiologyDocument26 pagesIntroduction To Anaesthesia: Fatiş Altındaş Department of AnesthesiologymochkurniawanPas encore d'évaluation
- Biology Investigatory Project: The Study of Effects of Antibiotics On Micro-OrganismsDocument9 pagesBiology Investigatory Project: The Study of Effects of Antibiotics On Micro-OrganismsSamanwitha SharmaPas encore d'évaluation
- Toxicity Review Natural ProductsDocument5 pagesToxicity Review Natural Productsamino12451Pas encore d'évaluation
- Obgyn Physician Assistant 1Document3 pagesObgyn Physician Assistant 1api-558916281Pas encore d'évaluation
- Ginjal Polikistik PDFDocument15 pagesGinjal Polikistik PDFAgunkRestuMaulanaPas encore d'évaluation
- Bell 2015Document5 pagesBell 2015Afien MuktiPas encore d'évaluation