Académique Documents
Professionnel Documents
Culture Documents
Thirty-Day Mortality in Patients Undergoing Laparotomy For Small Bowel Obstruction
Transféré par
WadezigTitre original
Copyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
Thirty-Day Mortality in Patients Undergoing Laparotomy For Small Bowel Obstruction
Transféré par
WadezigDroits d'auteur :
Formats disponibles
Original article
Thirty-day mortality in patients undergoing laparotomy for small
bowel obstruction
O. Peacock1 , M. G. Bassett2 , A. Kuryba3 , K. Walker3,4 , E. Davies5 , I. Anderson6 and R. S. Vohra1 ,
on behalf of the National Emergency Laparotomy Audit (NELA) Project Team
1
Trent Oesophago-Gastric Unit, Nottingham City Hospital Campus, Nottingham University Hospitals NHS Trust, Nottingham, 2 NELA Research
Fellow, Royal College of Anaesthetists, 3 Clinical Effectiveness Unit, Royal College of Surgeons of England, and 4 Department of Health Services
Research and Policy, London School of Hygiene and Tropical Medicine, London, 5 Department of Surgery, Royal Lancaster Infirmary, University
Hospitals of Morecambe Bay NHS Foundation Trust, Lancaster, and 6 Colorectal Surgery Department, Salford Royal Hospitals NHS Trust, Salford, UK
Correspondence to: Mr R. S. Vohra, Trent Oesophago-Gastric Unit, Nottingham City Hospital Campus, Nottingham University Hospitals NHS Trust,
Hucknall Road, Nottingham NG5 1PB, UK (e-mail: ravinder.vohra@nuh.nhs.uk; @ravinder_vohra)
Background: Small bowel obstruction (SBO) is a common indication for emergency laparotomy. There
are currently variations in the timing of surgery for patients with SBO and limited evidence on whether
delayed surgery affects outcomes. The aim of this study was to evaluate the impact of time to operation
on 30-day mortality in patients requiring emergency laparotomy for SBO.
Methods: Data were collected from the National Emergency Laparotomy Audit (NELA) on all patients
aged 18 years or older who underwent emergency laparotomy for all forms of SBO between December
2013 and November 2015. The primary outcome measure was 30-day mortality, with date of death
obtained from the Office for National Statistics. Patients were grouped according to the time from
admission to surgery (less than 24 h, 24–72 h and more than 72 h). A multilevel logistic regression model
was used to explore the impact of patient factors, primarily delay to surgery, on 30-day mortality.
Results: Some 9991 patients underwent emergency laparotomy requiring adhesiolysis or small bowel
resection for SBO. The overall mortality rate was 7⋅2 per cent (722 patients). Within each time group,
30-day mortality rates were significantly worse with increasing age, ASA grade, Portsmouth POSSUM
score and level of contamination. Patients undergoing emergency laparotomy more than 72 h after
admission had a significantly higher risk-adjusted 30-day mortality rate (odds ratio 1⋅39, 95 per cent
c.i. 1⋅09 to 1⋅76).
Conclusion: In patients who require an emergency laparotomy with adhesiolysis or resection for SBO, a
delay to surgery of more than 72 h is associated with a higher 30-day postoperative mortality rate.
Presented to the International Surgical Congress of the Association of Surgeons of Great Britain and Ireland (ASGBI),
Glasgow, UK, May 2017, and to the ASGBI Emergency Laparotomy Meeting, Birmingham, UK, November 2017
Paper accepted 2 December 2017
Published online in Wiley Online Library (www.bjs.co.uk). DOI: 10.1002/bjs.10812
Introduction be managed with an observed period of expectant manage-
More than 30 000 patients undergo an emergency laparo- ment for 3–5 days9 , and that 65–80 per cent of patients
tomy each year in National Health Service (NHS) hospi- with adhesive SBO will avoid surgery10 – 14 . However, one
tals in England and Wales1,2 . Acute intestinal obstruction hypothesis is that unnecessary delay of more than 3 days in
is the most common indication, occurring in half of all patients who require surgery may worsen outcomes15 .
patients3 . Surgery is associated with a 30-day mortality rate The National Emergency Laparotomy Audit (NELA)
of 15 per cent1,4 – 6 . Abdominal adhesions following pre- is an ongoing national quality improvement programme
vious surgery account for 60–70 per cent of small bowel describing the processes of care and outcomes of patients
obstruction (SBO)7 , and hernias account for the major- undergoing emergency bowel surgery in NHS hospitals in
ity of other cases8 . Some guidelines suggest that adhesive England and Wales3 . The data set contains preoperative,
SBO with no evidence of peritonitis or strangulation can perioperative and postoperative demographic and outcome
© 2018 BJS Society Ltd BJS
Published by John Wiley & Sons Ltd
O. Peacock, M. G. Bassett, A. Kuryba, K. Walker, E. Davies, I. Anderson and R. S. Vohra
data of more than 40 000 patients who have undergone Emergency laparotomy
emergency laparotomy since December 2013. n =43 574
The aim of this study was to report 30-day mortality in Excluded n =22 616
patients requiring emergency laparotomy for all forms of Elective admission n =3090
Primary indication not obstruction
acute SBO. In particular, the impact of surgical timing (less n = 19526
than 24 h, 24–72 h, or more than 72 h from admission to
Primary indication
surgery) and all-cause 30-day mortality for each group was bowel obstruction
investigated. n =20 958
Excluded (not small bowel
Methods
obstruction) n =10 195
Patients aged 18 years or over requiring an emergency
laparotomy for gastrointestinal surgery in an NHS hospi- Small bowel resection
tal in England and Wales between the 1 December 2013 or adhesiolysis
n =10 763
and 30 November 2015 were identified from the NELA
database. Those requiring an emergency laparotomy dur- Excluded n =772
ing an elective admission were excluded as their manage- Incomplete timings n= 420
Surgery more than 2 weeks
ment is unlikely to be representative of patients requiring after admission n =352
an emergency laparotomy as their index procedure within
an emergency admission. Eligible for final
analysis
Patients were included in the study if the recorded indi- n =9991
cation for surgery was obstruction, and the primary proce-
dure was recorded as small bowel resection or adhesiolysis. Fig. 1 Diagram showing the process of defining patients eligible
At the point of data collection, there was not an option for final analysis
within the NELA database to record an emergency laparo-
tomy performed for SBO. Therefore, patients were consid- perioperative (operative severity, procedure performed,
ered to have undergone an emergency laparotomy for SBO operative approach, intraoperative findings, level of con-
if the primary indication for surgery was obstruction and tamination, blood loss and postoperative destination)
the recorded primary procedure was either a small bowel factors were extracted. The total number of laparotomies
resection or adhesiolysis. All causes of SBO, such as adhe- performed at each hospital was also extracted from the
sions, malignancy and Crohn’s disease, were included in the NELA data set. Time from admission to surgery was
final analysis. defined in three groups: less than 24 h, 24–72 h or more
Time to surgery was calculated by subtracting the time of than 72 h.
admission to hospital from the time of entry into operating
theatre/anaesthetic room. Patients for whom this could not
be calculated were excluded (time of entry before time of Outcome
admission or time of entry not completed). Patients whose The primary outcome measure was (all-cause) 30-day post-
time to surgery was greater than 2 weeks after admission operative mortality in or out of hospital. Date of death
were also excluded as their disease process was assumed to was obtained by linking patient records to the Office for
be different from that of patients undergoing surgery more National Statistics mortality data.
promptly.
Statistical analysis
Data extraction
Data were analysed using Stata® SE v14.1 statistical soft-
Demographic and preoperative (urgency of surgery, ECG ware (StataCorp, College Station, Texas, USA). The χ2 test
findings, number of operations within the admission, was used to test for differences between categorical demo-
previous cardiac and respiratory history, ASA fitness grade, graphic variables. A multilevel logistic regression model,
and Portsmouth (P) POSSUM16 -predicted mortality), the NELA risk adjustment model, developed by the Clin-
physiological (serum sodium, potassium, urea, creatinine, ical Effectiveness Unit of the Royal College of Surgeons
haemoglobin, white cell count (WCC), lactate, pulse, of England, was used to determine whether there was any
systolic BP and Glasgow Coma Scale (GCS) score) and influence of delay to surgery on postoperative mortality,
© 2018 BJS Society Ltd www.bjs.co.uk BJS
Published by John Wiley & Sons Ltd
Thirty-day mortality after laparotomy for small bowel obstruction
Table 1 Comparison of patient demographics across the different time groups
< 24 h (n = 3112) 24–72 h (n = 3895) > 72 h (n = 2984)
Age (years)
< 65 1182 (38⋅0) 1420 (36⋅5) 1081 (36⋅2)
65–80 1159 (37⋅2) 1472 (37⋅8) 1109 (37⋅2)
> 80 771 (24⋅8) 1003 (25⋅8) 794 (26⋅6)
Sex ratio (M : F) 1417 : 1695 1608 : 2287 1196 : 1788
ASA fitness grade
I 381 (12⋅2) 375 (9⋅6) 239 (8⋅0)
II 1185 (38⋅1) 1638 (42⋅1) 1035 (34⋅7)
III 1082 (34⋅8) 1446 (37⋅1) 1242 (41⋅6)
≥ IV 464 (14⋅9) 436 (11⋅2) 468 (15⋅7)
P-POSSUM score
< 10 2221 (71⋅4) 3013 (77⋅4) 2207 (74⋅0)
10–24⋅9 528 (17⋅0) 542 (13⋅9) 488 (16⋅4)
25–49⋅9 227 (7⋅3) 222 (5⋅7) 193 (6⋅5)
≥ 50 136 (4⋅4) 118 (3⋅0) 96 (3⋅2)
Procedure
Small bowel resection 1660 (53⋅3) 1384 (35⋅5) 1007 (33⋅7)
Adhesiolysis 1452 (46⋅7) 2511 (64⋅5) 1977 (66⋅3)
Approach
Open 2796 (89⋅8) 3465 (89⋅0) 2679 (89⋅8)
Laparoscopic 316 (10⋅2) 430 (11⋅0) 305 (10⋅2)
Findings
Malignancy 126 (4⋅0) 225 (5⋅8) 229 (7⋅7)
No malignancy 2986 (96⋅0) 3670 (94⋅2) 2755 (92⋅3)
Adhesions 1773 (57⋅0) 2953 (75⋅8) 2376 (79⋅6)
No adhesions 1339 (43⋅0) 942 (24⋅2) 608 (20⋅4)
Perforation 259 (8⋅3) 264 (6⋅8) 287 (9⋅6)
No perforation 2853 (91⋅7) 3631 (93⋅2) 2697 (90⋅4)
Contamination
None 2780 (89⋅3) 3534 (90⋅7) 2617 (87⋅7)
Free gas/enteric/pus 332 (10⋅7) 361 (9⋅3) 367 (12⋅3)
Blood loss (ml)
≤ 500 2986 (96⋅0) 3744 (96⋅1) 2841 (95⋅2)
> 500 83 (2⋅7) 102 (2⋅6) 109 (3⋅7)
Missing 43 (1⋅4) 49 (1⋅3) 34 (1⋅1)
Postoperative destination
Ward 1523 (48⋅9) 2004 (51⋅5) 1438 (48⋅2)
Level 2 HDU 926 (29⋅8) 1234 (31⋅7) 1002 (33⋅6)
Level 3 ICU 661 (21⋅2) 654 (16⋅8) 540 (18⋅1)
Died in theatre 2 (0⋅1) 3 (0⋅1) 4 (0⋅1)
ONS 30-day mortality
Alive 2892 (92⋅9) 3659 (93⋅9) 2718 (91⋅1)
Dead 220 (7⋅1) 236 (6⋅1) 266 (8⋅9)
Heart rate (b.p.m.)* 88⋅3 (87, 75–100) 86⋅4 (85, 75–95) 86⋅2 (85, 75–95)
Systolic BP (mmHg)* 131⋅3 (130, 115–145) 131⋅7 (130, 118–145) 131⋅7 (130, 117–145)
Haemoglobin (g/l)* 141⋅5 (143, 128–155) 134⋅5 (135, 121–149) 126 (126, 113–139)
WCC (× 109 /l)* 13⋅1 (12⋅0, 8⋅8–15⋅6) 11⋅5 (10, 7⋅3–13⋅5) 10⋅5 (8⋅7, 6⋅4–12)
Preoperative lactate (mmol/l)* 2⋅2 (1⋅6, 1⋅1–2⋅6) 1⋅7 (1⋅3, 1⋅0–1⋅9) 1⋅4 (1⋅2, 0⋅9–1⋅6)
Sodium (mmol/l)* 136⋅2 (137, 134–139) 136⋅8 (137, 134–140) 137⋅3 (138, 135–140)
Potassium (mmol/l)* 4⋅2 (4⋅2, 3⋅8–4⋅5) 4⋅1 (4⋅1, 3⋅8–4⋅4) 4⋅0 (3⋅9, 3⋅6–4⋅3)
Urea (mmol/l)* 10⋅0 (7⋅3, 5⋅2–11⋅8) 9⋅5 (7⋅1, 4⋅9–11) 8⋅0 (6⋅0, 3⋅9–9⋅2)
Creatinine (mmol/l)* 104⋅0 (83, 66–109) 92⋅9 (77, 62–103) 85⋅1 (69, 55–91)
Values in parentheses are percentages unless indicated otherwise; *values are mean (median, i.q.r.). P-POSSUM, Portsmouth POSSUM; HDU,
high-dependency unit; ONS, Office for National Statistics; b.p.m., beats per minute; WCC, white cell count.
© 2018 BJS Society Ltd www.bjs.co.uk BJS
Published by John Wiley & Sons Ltd
O. Peacock, M. G. Bassett, A. Kuryba, K. Walker, E. Davies, I. Anderson and R. S. Vohra
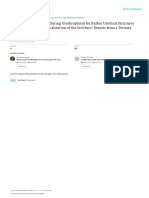
10 was included to account for clustering of 30-day postoper-
9 ative mortality by hospital. The results are reported as odds
30-day mortality (%)
8
7 ratios (ORs) with 95 per cent confidence intervals.
6 Multiple imputation by chained equations with ten
5 imputed data sets was used to account for missing values
4
3 within the patient risk-adjustment variables16,18 . The
2 imputation model included the outcome variable, all vari-
1
0
ables included in the risk-adjustment model, and a number
<24 24–72 >72 of additional variables (NELA year and haemoglobin
Time from admission to surgery (h) level). Rubin’s rules were used to pool the regression
coefficients and estimate their standard errors.
Fig. 2 All-cause 30-day mortality in the three time groups
Results
after adjusting for patient risk factors. Adjustment was car-
ried out using this model, a multivariable logistic regres- The NELA database contained information for 43 574
sion model based on P-POSSUM variables, that was devel- patients who had an emergency laparotomy for bowel
oped to provide risk-adjusted all-cause 30-day postoper- surgery in 188 NHS hospitals in England and Wales
ative mortality at hospital level17 . This model includes between 1 December 2013 and 30 November 2015
the following variables: age, sex, audit year of procedure, (Fig. 1). Of these, 10 763 (24⋅7 per cent) underwent an
urgency of the surgery, ECG findings, number of opera- emergency laparotomy with adhesiolysis or resection for
tions within the admission, cardiac signs, respiratory his- SBO during the study period. Patients were excluded if
tory, ASA fitness grade, serum sodium, potassium, urea, the time of surgery could not be calculated (either time of
creatinine, haemoglobin, WCC, pulse, systolic BP, GCS, entry to theatre was not completed (419 patients) or time
operative severity, peritoneal soiling, intraoperative blood of entry was before time of admission (1 patient)). Some
loss and presence of malignancy, as well as interactions 352 patients had an emergency laparotomy more than
between age and ASA grade, and age and respiratory his- 2 weeks after admission and were also excluded. Thus,
tory. The model has a C-index of 0⋅863 (95 per cent c.i. during this 2-year interval, 9991 patients were considered
0⋅858 to 0⋅868) and was chosen over P-POSSUM because eligible for final analysis.
of better calibration in patients with a predicted risk of The majority of laparotomies (6879, 68⋅9 per cent) were
death greater than 15 per cent17 . The year of the patient’s performed 24 h or more after admission (Table 1). The
procedure (2013–2014 or 2014–2015) was included as a majority of causes of SBO were adhesion-related (71⋅1 per
variable in the risk-adjustment model to allow for over- cent), and only 5⋅8 per cent were caused by malignancy and
all changes in postoperative mortality over time across all 2⋅9 per cent by inflammatory bowel disease. Mean lactate,
hospitals. For this analysis, a random intercept for hospital WCC and P-POSSUM values were higher in patients who
36
Mean
32 95% limits
99·8% limits
28
30-day mortality (%)
24
20
16
12
0
25 50 75 100 125 150 175 200
No. of operations
Fig. 3 Funnel plot of adjusted 30-day mortality in 188 hospitals that performed ten or more operations for small bowel obstruction
© 2018 BJS Society Ltd www.bjs.co.uk BJS
Published by John Wiley & Sons Ltd
Thirty-day mortality after laparotomy for small bowel obstruction
Table 2 Comparison of patient demographics versus all-cause 30-day mortality within each time group
< 24 h 24–72 h > 72 h
30-day 30-day 30-day
n Deaths mortality (%) P* n Deaths mortality (%) P* n Deaths mortality (%) P*
Overall 3112 220 7⋅1 3895 236 6⋅1 2984 266 8⋅9
Age (years) < 0⋅001 < 0⋅001 < 0⋅001
< 65 1182 23 2⋅0 1420 24 1⋅7 1081 27 2⋅5
65–80 1159 88 7⋅6 1472 91 6⋅2 1109 101 9⋅1
> 80 771 109 14⋅1 1003 121 12⋅1 794 138 17⋅4
Sex 0⋅386 0⋅064 0⋅136
M 1417 94 6⋅6 1608 111 6⋅9 1196 118 9⋅9
F 1695 126 7⋅4 2287 125 5⋅5 1788 148 8⋅3
ASA fitness grade < 0⋅001 < 0⋅001 < 0⋅001
I 381 1 0⋅3 375 2 0⋅5 239 0 0⋅0
II 1185 30 2⋅5 1638 25 1⋅5 1035 29 2⋅8
III 1082 80 7⋅4 1446 98 6⋅8 1242 103 8⋅3
≥ IV 464 109 23⋅5 436 111 25⋅5 468 134 28⋅6
P-POSSUM score < 0⋅001 < 0⋅001 < 0⋅001
< 10 2221 61 2⋅8 3013 81 2⋅7 2207 106 4⋅8
10–24⋅9 528 67 12⋅7 542 62 11⋅4 488 73 15⋅0
25-49⋅9 227 44 19⋅4 222 49 22⋅1 193 50 25⋅9
≥ 50 136 48 35⋅3 118 44 37⋅3 96 37 38⋅5
Procedure < 0⋅001 < 0⋅001 < 0⋅001
Small bowel resection 1660 146 8⋅8 1384 126 9⋅1 1007 124 12⋅3
Adhesiolysis 1452 74 5⋅1 2511 110 4⋅4 1977 142 7⋅2
Approach < 0⋅001 0⋅018 0⋅127
Open 2796 213 7⋅6 3465 221 6⋅4 2679 246 9⋅2
Laparoscopic 316 7 2⋅2 430 15 3⋅5 305 20 6⋅6
Findings
Malignancy 126 14 11⋅1 0⋅071 225 23 10⋅2 0⋅007 229 33 14⋅4 0⋅002
No malignancy 2986 206 6⋅9 3670 213 5⋅8 2755 233 8⋅5
Adhesions 1773 104 5⋅9 0⋅003 2953 160 5⋅4 0⋅003 2376 194 8⋅2 0⋅005
No adhesions 1339 116 8⋅7 942 76 8⋅1 608 72 11⋅8
Perforation 259 25 9⋅7 0⋅090 264 36 13⋅6 < 0⋅001 287 43 15⋅0 < 0⋅001
No perforation 2853 195 6⋅8 3631 200 5⋅5 2697 223 8⋅3
Contamination < 0⋅001 < 0⋅001 < 0⋅001
None 2780 177 6⋅4 3534 182 5⋅2 2617 197 7⋅5
Free gas/enteric/pus 332 43 13⋅0 361 54 15⋅0 367 69 18⋅8
Blood loss (ml) 0⋅099 0⋅001 0⋅002
≤ 500 2986 209 7⋅0 3744 218 5⋅8 2841 244 8⋅6
> 500 83 10 12⋅1 102 15 14⋅7 109 20 18⋅4
Missing 43 1 2⋅3 49 3 6⋅1 34 2 5⋅9
Postoperative destination < 0⋅001 < 0⋅001 < 0⋅001
Ward 1523 39 2⋅6 2004 37 1⋅9 1438 59 4⋅1
Level 2 HDU 926 58 6⋅3 1234 71 5⋅8 1002 86 8⋅6
Level 3 ICU 661 121 18⋅3 654 125 19⋅1 540 118 21⋅9
P-POSSUM, Portsmouth POSSUM; HDU, high-dependency unit. *χ2 test.
Table 3 Multivariable analysis of unadjusted and adjusted 30-day mortality rates according to stratified time group for operative
intervention
Odds ratio
< 24 h* 24–72 h > 72 h P
Unadjusted 30-day mortality 1⋅00 0⋅85 (0⋅70, 1⋅03) 1⋅29 (1⋅07, 1⋅55) < 0⋅001
NELA risk adjustment model 1⋅00 1⋅02 (0⋅81, 1⋅27) 1⋅38 (1⋅09, 1⋅75) 0⋅007
NELA risk adjustment model + random intercept 1⋅00 1⋅01 (0⋅81, 1⋅27) 1⋅39 (1⋅09, 1⋅76) 0⋅006
Values in parentheses are 95 per cent confidence intervals. All variables adjusted for are outlined in Table 4. *Reference. NELA, National Emergency
Laparotomy Audit.
© 2018 BJS Society Ltd www.bjs.co.uk BJS
Published by John Wiley & Sons Ltd
O. Peacock, M. G. Bassett, A. Kuryba, K. Walker, E. Davies, I. Anderson and R. S. Vohra
Table 4 Logistic regression table for the National Emergency Laparotomy Audit and hospital risk adjustment model for 30-day
mortality
Odds ratio Odds ratio
Time to surgery (h) < 24 1⋅00 (reference) Serum urea (mmol/l) 2 0⋅88 (0⋅45, 1⋅72)
24–72 1⋅02 (0⋅81, 1⋅27) 5 0⋅91 (0⋅74, 1⋅11)
> 72 1⋅39 (1⋅09, 1⋅76) 10 1⋅00 (reference)
Year of surgery 2013–2014 1⋅00 (reference) 20 1⋅17 (1⋅03, 1⋅34)
2014–2015 0⋅82 (0⋅69, 0⋅98) 30 1⋅33 (1⋅05, 1⋅67)
Sex M 1⋅00 (reference) Serum creatinine 40 1⋅24 (0⋅72, 2⋅11)
F 0⋅95 (0⋅79, 1⋅14) (mmol/l) 70 1⋅07 (0⋅84, 1⋅35)
Surgical urgency (h) > 18 1⋅00 (reference) 100 1⋅00 (reference)
6–18 1⋅11 (0⋅83, 1⋅47) 150 0⋅96 (0⋅84, 1⋅09)
2–6 1⋅18 (0⋅89, 1⋅57) 200 0⋅95 (0⋅78, 1⋅15)
<2 1⋅52 (1⋅02, 2⋅25) Serum potassium 3 1⋅06 (0⋅80, 1⋅41)
No. of procedures 1 1⋅00 (reference) (mmol/l) 3⋅5 0⋅99 (0⋅88, 1⋅10)
including this one in 2 1⋅00 (0⋅69, 1⋅46) 4 1⋅00 (reference)
previous 30 days >2 0⋅72 (0⋅19, 2⋅64) 4⋅5 1⋅11 (1⋅03, 1⋅19)
Operative severity Major 1⋅00 (reference) 5 1⋅34 (1⋅13, 1⋅59)
Major+ 1⋅35 (1⋅08, 1⋅68) Pulse rate (b.p.m.) 60 0⋅58 (0⋅44, 0⋅76)
ECG findings No abnormalities 1⋅00 (reference) 70 0⋅71 (0⋅61, 0⋅82)
AF rate 60–90 b.p.m. 1⋅18 (0⋅86, 1⋅64) 90 1⋅00 (reference)
AF rate > 90 b.p.m. or 1⋅01 (0⋅82, 1⋅25) 120 1⋅48 (1⋅23, 1⋅77)
abnormal
Cardiac signs/chest X-ray No cardiac failure 1⋅00 (reference) 140 1⋅75 (1⋅14, 2⋅70)
appearance Antihypertensive therapy 1⋅25 (1⋅02, 1⋅54) Age (years) 50 0⋅26 (0⋅14, 0⋅44)
Borderline cardiomegaly 1⋅63 (1⋅20, 2⋅22) ASA grade I or II 60 0⋅48 (0⋅38, 0⋅59)
Cardiomegaly 1⋅48 (0⋅88, 2⋅48) 70 1⋅00 (reference)
GCS score 13–15 1⋅00 (reference) 80 2⋅34 (1⋅88, 2⋅92)
9–12 2⋅86 (1⋅30, 6⋅28) 90 6⋅14 (3⋅51, 10⋅74)
3–8 3⋅71 (1⋅83, 7⋅53) Age (years) 50 0⋅31 (0⋅19, 0⋅52)
Presence of malignancy None 1⋅00 (reference) ASA grade III 60 0⋅57 (0⋅47, 0⋅69)
Primary 1⋅74 (1⋅06, 2⋅85) 70 1⋅00 (reference)
Nodal metastases 2⋅18 (1⋅22, 3⋅89) 80 1⋅70 (1⋅48, 1⋅95)
Distant 3⋅64 (2⋅51, 5⋅28) 90 2⋅78 (1⋅96, 3⋅95)
Peritoneal soiling None 1⋅00 (reference) Age (years) 50 0⋅62 (0⋅48, 0⋅81)
Serous fluid 1⋅10 (0⋅91, 1⋅34) ASA grade IV 60 0⋅75 (0⋅67, 0⋅84)
Localized pus 1⋅14 (0⋅69, 1⋅90) 70 1⋅00 (reference)
Free bowel content, pus or 2⋅06 (1⋅58, 2⋅70) 80 1⋅70 (1⋅48, 1⋅95)
blood
Blood loss (ml) < 100 1⋅00 (reference) 90 2⋅78 (1⋅96, 3⋅95)
101–500 1⋅20 (0⋅99, 1⋅44) Age (years) 50 0⋅62 (0⋅48, 0⋅81)
501–999 1⋅88 (1⋅20, 2⋅94) ASA grade V 60 0⋅75 (0⋅67, 0⋅84)
≥ 1000 2⋅64 (1⋅14, 6⋅12) 70 1⋅00 (reference)
Serum sodium (mmol/l) 125 1⋅19 (0⋅89, 1⋅59) 80 3⋅48 (1⋅50, 8⋅12)
130 1⋅13 (0⋅90, 1⋅42) 90 31⋅25 (3⋅03, 321⋅88)
140 1⋅00 (reference) Respiratory history None 1⋅00 (reference)
150 2⋅30 (1⋅06, 5⋅01) ASA grade I or II Mild dyspnoea 2⋅15 (1⋅22, 3⋅79)
Systolic BP (mmHg) 80 1⋅74 (1⋅35, 2⋅25) Limiting and at rest 6⋅75 (3⋅14, 14⋅48)
100 1⋅24 (1⋅13, 1⋅37) Respiratory history None 1⋅00 (reference)
120 1⋅00 (reference) ASA grade III Mild dyspnoea 1⋅35 (0⋅99, 1⋅83)
150 0⋅91 (0⋅80, 1⋅03) Limiting and at rest 2⋅02 (1⋅45, 2⋅80)
180 1⋅08 (0⋅74, 1⋅59) Respiratory history None 1⋅00 (reference)
Serum WCC (× 109 /l) 5 0⋅96 (0⋅86, 1⋅08) ASA grade IV Mild dyspnoea 1⋅60 (1⋅10, 2⋅35)
10 1⋅00 (reference) Limiting and at rest 2⋅17 (1⋅54, 3⋅05)
20 1⋅03 (0⋅89, 1⋅18) Respiratory history None 1⋅00 (reference)
30 0⋅99 (0⋅68, 1⋅44) ASA grade V Mild dyspnoea 0⋅83 (0⋅11, 6⋅25)
40 0⋅91 (0⋅39, 2⋅09) Limiting and at rest 5⋅09 (1⋅00, 25⋅79)
Values in parentheses are 95 per cent confidence intervals. AF, atrial fibrillation; b.p.m., beats per minute; GCS, Glasgow Coma Scale; WCC, white cell
count.
© 2018 BJS Society Ltd www.bjs.co.uk BJS
Published by John Wiley & Sons Ltd
Thirty-day mortality after laparotomy for small bowel obstruction
had surgery less than 24 h after admission, and a higher Discussion
proportion of small bowel resections was also performed
in this group. This study of the NELA database of emergency laparo-
The overall 30-day mortality rate was 7⋅2 per cent (722 tomy for all forms of SBO has shown that the timing of
of the 9991 patients). The unadjusted 30-day mortality rate laparotomy is an independent predictor of all-cause 30-day
in the group of patients with inaccuracies of data entry for mortality. Within each time group studied, increasing
surgical timing (420 of 10 763 patients, 3⋅9 per cent) was mortality was associated with increasing age, ASA grade,
5⋅7 per cent. P-POSSUM score, level of contamination and whether a
Despite patients treated within 24 h being the small bowel resection was required as expected. Patients
highest-risk group, their unadjusted 30-day mortality who had surgery within 24 h represent a different cohort
rate was only slightly higher than that in patients treated of SBO, presenting with signs of strangulation or periton-
in 24–72 h; the rate in the group of patients treated more ism (or a cause of SBO unlikely to settle with conservative
than 72 h after admission was substantially higher (Fig. 2). management), as noted by the greater proportion requir-
The adjusted 30-day mortality rate by hospital perform- ing a small bowel resection and higher mean lactate, WCC
ing ten or more laparotomies for SBO did not demonstrate and P-POSSUM values in this group. Patients who had an
any greater variation between hospitals than would be operation more than 72 h after hospital admission had a 39
expected by chance alone (Fig. 3). Of the 188 hospitals per cent higher mortality risk than those who had surgery
compared, nine (4⋅8 per cent) would be expected to fall less than 24 h from admission, after adjustment for patient
outside the inner funnel limits by chance alone, and only demographics and physiological factors (OR 1⋅39, 95 per
six (3⋅2 per cent) were observed. There were no outlying cent c.i. 1⋅09 to 1⋅76). This increase in mortality was not
hospitals. linked to hospital factors.
The unadjusted all-cause 30-day mortality rate was Previous studies have focused on patients with adhesive
significantly worse with increasing age, ASA grade, SBO. In the present study, all forms of SBO requiring adhe-
P-POSSUM score, level of contamination, requirement siolysis or small bowel resection were included. Although
for small bowel resection and postoperative level of care this produces a heterogeneous group, it is more represen-
within each time group (Table 2). When most variables tative of actual clinical practice for SBO. There are several
were considered, 30-day mortality was generally higher in other limitations to this study, which must be considered.
the group that had surgery more than 72 h after admission. This was a retrospective observational study, and the ret-
rospective nature probably accounts for the large number
Multilevel logistic regression model of patients with missing values (11⋅4 per cent) within the
data set that were accounted for using multiple imputation
Comparison of unadjusted 30-day mortality rates in the
groups of patients having surgery less than 24 h, 24–72 h by chained equations to address the issue of bias. NELA
and more than 72 h after admission demonstrated a sig- is reliant on data entry from multiple sources, and this is
nificant increase in mortality proportional to the time another reason for the high number of missing variables.
taken to perform the operation (P < 0⋅001) (Table 3). Using The database included data only for patients who required
patient demographic, surgical and physiological variables an emergency operative intervention for SBO (with adhe-
in the NELA data set (Table 4), the NELA risk adjust- siolysis or small bowel resection), not for those with SBO
ment model was used to derive the risk-adjusted hospital that settled with conservative management or required
30-day mortality rates for each time group (Table 3). There another form of operative intervention. The study was not
were 1138 patients (11⋅4 per cent) missing one or more designed to evaluate which patients actually required an
risk-adjustment variables that were accounted for by multi- operation for SBO. The proportion of patients who were
ple imputation using chained equations with ten imputed turned down for surgery because of fitness or patient choice
data sets. is unknown. It is also possible that surgical delay reflects a
There was strong statistical evidence of a difference reluctance to intervene surgically with regard to particular
in 30-day mortality between the time groups (Table 3). patient or institutional factors, which cannot be captured
There was little difference in the adjusted 30-day mor- by this database. However, the database collects a com-
tality between patients having surgery less than 24 h after prehensive list of patient variables, enabling risk-adjusted
admission for SBO and those in the 24–72 h group, but outcomes and comparison of the study groups to reduce
mortality was substantially higher when the operation was selection bias. The prospective National Audit of Small
done more than 72 h after admission (OR 1⋅39, 95 per cent Bowel Obstruction (NASBO)3 may address some of the
c.i. 1⋅09 to 1⋅76; P = 0⋅006). limitations of this study.
© 2018 BJS Society Ltd www.bjs.co.uk BJS
Published by John Wiley & Sons Ltd
O. Peacock, M. G. Bassett, A. Kuryba, K. Walker, E. Davies, I. Anderson and R. S. Vohra
Currently, there are no UK guidelines for the manage- Surgeons National Surgical Quality Improvement Program
ment of SBO. The World Society of Emergency Surgery database. J Am Coll Surg 2012; 215: 503–511.
has produced guidelines9 for the management of adhesive 7 Parker MC, Ellis H, Moran BJ, Thompson JN, Wilson MS,
SBO, which advocate, in the absence of signs of strangu- Menzies D et al. Postoperative adhesions: ten-year follow-up
of 12 584 patients undergoing lower abdominal surgery. Dis
lation or peritonism, a period of non-operative manage-
Colon Rectum 2001; 44: 822–829.
ment for up to 72 h. However, there are variations in this
8 Markogiannakis H, Messaris E, Dardamanis D, Pararas N,
suggested non-operative management period, with other Tzertzemelis D, Giannopoulos P et al. Acute mechanical
guidelines and studies advocating up to 5 days for adhesive bowel obstruction: clinical presentation, etiology,
SBO19,20 . In contrast, Teixeira and colleagues15 demon- management and outcome. World J Gastroenterol 2007; 13:
strated that patients with adhesive SBO whose operation 432−437.
was delayed by 24 h or more after admission had signifi- 9 Di Saverio S, Coccolini F, Galati M, Smerieri N, Biffl WL,
cantly higher risk-adjusted mortality than patients who had Ansaloni L et al. Bologna guidelines for diagnosis and
early (at less than 24 h) surgical intervention. management of adhesive small bowel obstruction (ASBO):
2013 update of the evidence-based guidelines from the
World Society of Emergency Surgery ASBO Working
Acknowledgements
Group. World J Emerg Surg 2013; 8: 42.
10 Seror D, Feigin E, Szold A, Allweis TM, Carmon M, Nissan
O.P. and M.G.B. are joint first authors of this publication.
S et al. How conservatively can postoperative small bowel
The authors thank all the members of the NELA project
obstruction be treated? Am J Surg 1993; 165: 121–125.
team who prepared the first- and second-year NELA 11 Tanaka S, Yamamoto T, Kubota D, Matsuyama M, Uenishi
reports for their contribution to this study: D. Cromwell, T, Kubo S et al. Predictive factors for surgical indication in
N. Eugene, M. Grocott, C. Johnston, J. Lourtie, R. adhesive small bowel obstruction. Am J Surg 2008; 196:
Moonesinghe, D. Murray, D. Papadimitriou, C. Peden, T. 23–27.
Poulton, M. Cripps, S. Drake and M. Oliver. 12 Jeong WK, Lim SB, Choi HS, Jeong SY. Conservative
NELA was commissioned by the Healthcare Quality management of adhesive small bowel obstructions in
Improvement Partnership (HQIP) and funded by NHS patients previously operated on for primary colorectal
England and the Welsh Government. cancer. J Gastrointest Surg 2008; 12: 926–932.
Disclosure: The authors declare no conflict of interest. 13 Cox MR, Gunn IF, Eastman MC, Hunt RF, Heinz AW.
The safety and duration of non-operative treatment for
adhesive small bowel obstruction. Aust N Z J Surg 1993; 63:
References
367–371.
1 Symons NR, Moorthy K, Almoudaris AM, Bottle A, Aylin P, 14 Miller G, Boman J, Shrier I, Gordon PH. Natural history of
Vincent CA et al. Mortality in high-risk emergency general patients with adhesive small bowel obstruction. Br J Surg
surgical admissions. Br J Surg 2013; 100: 1318–1325. 2000; 87: 1240–1247.
2 Shapter SL, Paul MJ, White SM. Incidence and estimated 15 Teixeira PG, Karamanos E, Talving P, Inaba K, Lam L,
annual cost of emergency laparotomy in England: is there a Demetriades D. Early operation is associated with a survival
major funding shortfall? Anaesthesia 2012; 67: 474–478. benefit for patients with adhesive bowel obstruction. Ann
3 National Audit of Small Bowel Obstruction (NASBO). Surg 2013; 258: 459–465.
NASBO Protocol V14; 2017. http://www.nasbo.org.uk/wp- 16 Copeland GP, Jones D, Walters M. POSSUM: a scoring
content/uploads/2017/01/NASBOv14.pdf [accessed 11 system for surgical audit. Br J Surg 1991; 78: 355–360.
April 2016]. 17 National Emergency Laparotomy Audit (NELA). NELA
4 Saunders DI, Murray D, Pichel AC, Varley S, Peden CJ. Technical Document; 2016. http://www.nela.org.uk/reports
Variations in mortality after emergency laparotomy: the first [accessed 11 April 2017].
report of the UK Emergency Laparotomy Network. Br J 18 White IR, Royston P, Wood AM. Multiple imputation using
Anaesth 2012; 109: 368–375. chained equations: issues and guidance for practice. Stat Med
5 Vester-Andersen M, Lundstrom LH, Moller MH, Waldau 2011; 30: 377–399.
T, Rosenberg J, Moller AM. Mortality and postoperative 19 Diaz JJ, Jr., Bokhari F, Mowery NT, Acosta JA, Block EF,
care pathways after emergency gastrointestinal surgery in Bromberg WJ et al. Guidelines for management of small
2904 patients: a population-based cohort study. Br J Anaesth bowel obstruction. J Trauma 2008; 64: 1651−1664.
2014; 112: 860–870. 20 Schraufnagel D, Rajaee S, Millham FH. How many sunsets?
6 Al-Temimi MH, Griffee M, Enniss TM, Preston R, Vargo Timing of surgery in adhesive small bowel obstruction: a
D, Overton S et al. When is death inevitable after study of the Nationwide Inpatient Sample. J Trauma Acute
emergency laparotomy? Analysis of the American College of Care Surg 2012; 74: 181–187.
© 2018 BJS Society Ltd www.bjs.co.uk BJS
Published by John Wiley & Sons Ltd
Vous aimerez peut-être aussi
- Pancreatitis AgudaDocument6 pagesPancreatitis AgudaElias Emmanuel JaimePas encore d'évaluation
- Colorectal Disease - 2022 - Clausen - Incidence and Clinical Predictors of 30 Day Emergency Readmission After ColorectalDocument12 pagesColorectal Disease - 2022 - Clausen - Incidence and Clinical Predictors of 30 Day Emergency Readmission After ColorectalArtémis BowstringPas encore d'évaluation
- Acute Intestinal ObstructionDocument9 pagesAcute Intestinal ObstructionRoxana ElenaPas encore d'évaluation
- Pancreatic ®stula After Pancreatic Head ResectionDocument7 pagesPancreatic ®stula After Pancreatic Head ResectionNicolas RuizPas encore d'évaluation
- 1 Bjs 10662Document8 pages1 Bjs 10662Vu Duy KienPas encore d'évaluation
- Apendisitis MRM 3Document8 pagesApendisitis MRM 3siti solikhaPas encore d'évaluation
- Liver A BSC DrainDocument8 pagesLiver A BSC DrainAngelica AmesquitaPas encore d'évaluation
- Management of Suspected Anastomotic Leak After Bariatric Laparoscopic Roux-en-Y Gastric BypassDocument7 pagesManagement of Suspected Anastomotic Leak After Bariatric Laparoscopic Roux-en-Y Gastric BypassJOTACEPas encore d'évaluation
- Timing of Endoscopy For Acute Upper Gastrointestinal Bleeding: A Territory-Wide Cohort StudyDocument7 pagesTiming of Endoscopy For Acute Upper Gastrointestinal Bleeding: A Territory-Wide Cohort StudyFaisal BaigPas encore d'évaluation
- 1 s2.0 S0140673623013119 MainDocument10 pages1 s2.0 S0140673623013119 MainpipeudeaPas encore d'évaluation
- Comparison of Laparoscopic vs. Open Surgery For Rectal CancerDocument7 pagesComparison of Laparoscopic vs. Open Surgery For Rectal Cancermohammed askarPas encore d'évaluation
- Laparoscopic Appendectomy For Complicated Appendicitis - An Evaluation of Postoperative Factors.Document5 pagesLaparoscopic Appendectomy For Complicated Appendicitis - An Evaluation of Postoperative Factors.Juan Carlos SantamariaPas encore d'évaluation
- dubois2010Document7 pagesdubois2010mia widiastutiPas encore d'évaluation
- Tecnica de Clips Nefrectomia ParcialDocument8 pagesTecnica de Clips Nefrectomia ParcialAlfredo BalcázarPas encore d'évaluation
- Isj-5899 oDocument5 pagesIsj-5899 oAbhiram MundlePas encore d'évaluation
- Laparoscopic Appendectomy PostoperativeDocument6 pagesLaparoscopic Appendectomy PostoperativeDamal An NasherPas encore d'évaluation
- Article LCA Mars 2023Document10 pagesArticle LCA Mars 2023Côme JaubertPas encore d'évaluation
- Art07 PDFDocument6 pagesArt07 PDFadan2010Pas encore d'évaluation
- Complicated AppendicitisDocument4 pagesComplicated AppendicitisMedardo ApoloPas encore d'évaluation
- Laparoscopic Versus Open Cystogastrostomy For Pancreatic Pseudocysts A Comparative StudyDocument4 pagesLaparoscopic Versus Open Cystogastrostomy For Pancreatic Pseudocysts A Comparative StudyInternational Journal of Innovative Science and Research TechnologyPas encore d'évaluation
- Analysis of Recurrent Urethral Strictures Due To Iatrogenic Urethral TraumaDocument6 pagesAnalysis of Recurrent Urethral Strictures Due To Iatrogenic Urethral TraumaNur Syamsiah MPas encore d'évaluation
- Cirocchi2017 PDFDocument18 pagesCirocchi2017 PDFAndres TamePas encore d'évaluation
- New England Journal Medicine: The ofDocument12 pagesNew England Journal Medicine: The ofFarizka Dwinda HPas encore d'évaluation
- EASY TrialDocument8 pagesEASY TrialDpxeir PapanikolaouPas encore d'évaluation
- Comparison of Perioperative Outcomes Between Laparoscopic and Open Approach For PancreatoduodenectomyDocument9 pagesComparison of Perioperative Outcomes Between Laparoscopic and Open Approach For PancreatoduodenectomyVu Duy KienPas encore d'évaluation
- SurgicalTipsandTricksDuringUrethroplastyforBulbarUrethralStricturesFocusingonAccurateLocalisationoftheStricture ResultsfromaTertiaryCentreDocument8 pagesSurgicalTipsandTricksDuringUrethroplastyforBulbarUrethralStricturesFocusingonAccurateLocalisationoftheStricture ResultsfromaTertiaryCentreTomek RPas encore d'évaluation
- Journal Medicine: The New EnglandDocument7 pagesJournal Medicine: The New England'Muhamad Rofiq Anwar'Pas encore d'évaluation
- Role of Laparoscopic Cholecystectomy in The Early Management of Acute Gallbladder DiseaseDocument6 pagesRole of Laparoscopic Cholecystectomy in The Early Management of Acute Gallbladder DiseaseHoracio ChaconPas encore d'évaluation
- Comparative Analysis of Clinical Outcomes of Open Appendectomy and Laparoscopic AppendectomyDocument6 pagesComparative Analysis of Clinical Outcomes of Open Appendectomy and Laparoscopic AppendectomyIJRASETPublicationsPas encore d'évaluation
- farach2014Document5 pagesfarach2014mia widiastutiPas encore d'évaluation
- Stapled Rectal Mucosectomy vs. Close HemorrhoidectomyDocument9 pagesStapled Rectal Mucosectomy vs. Close HemorrhoidectomyNadllely Garcia ZapataPas encore d'évaluation
- Impact of Postoperative Morbidity On Long-Term Survival After OesophagectomyDocument10 pagesImpact of Postoperative Morbidity On Long-Term Survival After OesophagectomyPutri PadmosuwarnoPas encore d'évaluation
- Protocol oDocument8 pagesProtocol oCynthia ChávezPas encore d'évaluation
- A Prospective Treatment Protocol For Outpatient Laparoscopic Appendectomy For Acute AppendicitisDocument5 pagesA Prospective Treatment Protocol For Outpatient Laparoscopic Appendectomy For Acute AppendicitisBenjamin PaulinPas encore d'évaluation
- 65 Stenoza GDDDocument7 pages65 Stenoza GDDGabriela MilitaruPas encore d'évaluation
- Complications of Enterocystoplastycase SeriesDocument5 pagesComplications of Enterocystoplastycase SeriesIJAR JOURNALPas encore d'évaluation
- Measure BUN Creat urine leakageDocument4 pagesMeasure BUN Creat urine leakagerendi wibowoPas encore d'évaluation
- Time From Admission To Initiation of Surgery For Source Control Is A Critical Determinant of Survival in Patients With Gastrointestinal Perforation With Associated Septic ShockDocument10 pagesTime From Admission To Initiation of Surgery For Source Control Is A Critical Determinant of Survival in Patients With Gastrointestinal Perforation With Associated Septic ShockSANDRA MILENA GUTIERREZ CAÑASPas encore d'évaluation
- Oesophagal PerfDocument7 pagesOesophagal PerfShiva KumarPas encore d'évaluation
- 1-s2.0-S2667008923000253-mainDocument4 pages1-s2.0-S2667008923000253-mainal malikPas encore d'évaluation
- Cutaneous Needle Aspirations in Liver DiseaseDocument6 pagesCutaneous Needle Aspirations in Liver DiseaseRhian BrimblePas encore d'évaluation
- Ahbps-24-44 Appendicitis After Liver Transplantation JournalDocument8 pagesAhbps-24-44 Appendicitis After Liver Transplantation JournalIndah JamtaniPas encore d'évaluation
- Serosal Appendicitis: Incidence, Causes and Clinical SignificanceDocument3 pagesSerosal Appendicitis: Incidence, Causes and Clinical SignificancenaufalrosarPas encore d'évaluation
- Management of Acute Upper Gastrointestinal Bleeding: Urgent Versus Early EndosDocument5 pagesManagement of Acute Upper Gastrointestinal Bleeding: Urgent Versus Early EndosCarolina Ormaza GiraldoPas encore d'évaluation
- Management of Acute Upper Gastrointestinal Bleeding: Urgent Versus Early EndosDocument5 pagesManagement of Acute Upper Gastrointestinal Bleeding: Urgent Versus Early EndossamuelPas encore d'évaluation
- qt5kh1c39r NosplashDocument12 pagesqt5kh1c39r NosplashSusiePas encore d'évaluation
- Gastro Graf inDocument12 pagesGastro Graf inquileutePas encore d'évaluation
- Corto y Largo PlazoDocument6 pagesCorto y Largo PlazoElard Paredes MacedoPas encore d'évaluation
- Downloaded From Uva-Dare, The Institutional Repository of The University of Amsterdam (Uva)Document15 pagesDownloaded From Uva-Dare, The Institutional Repository of The University of Amsterdam (Uva)Pra YudhaPas encore d'évaluation
- Articles: BackgroundDocument12 pagesArticles: BackgroundJoshua BensonPas encore d'évaluation
- 268 2011 Article 1088 PDFDocument6 pages268 2011 Article 1088 PDFIoel Tovar TrovaPas encore d'évaluation
- IMU Learning Outcome: Psychomotor SkillsDocument11 pagesIMU Learning Outcome: Psychomotor SkillsRameshPas encore d'évaluation
- Early Laparoscopic Cholecystectomy Benefits in Acute CholecystitisDocument4 pagesEarly Laparoscopic Cholecystectomy Benefits in Acute CholecystitisalifandoPas encore d'évaluation
- Pattern of Acute Intestinal Obstruction: Is There A Change in The Underlying Etiology?Document4 pagesPattern of Acute Intestinal Obstruction: Is There A Change in The Underlying Etiology?neildamiPas encore d'évaluation
- General Surgery: Ruptured Liver Abscess: A Novel Surgical TechniqueDocument3 pagesGeneral Surgery: Ruptured Liver Abscess: A Novel Surgical TechniqueRahul SinghPas encore d'évaluation
- APENDICITISDocument9 pagesAPENDICITISAtziri LoeraPas encore d'évaluation
- Laparoscopic Cholecystectomy:An Experience of 200 Cases: Original ArticleDocument4 pagesLaparoscopic Cholecystectomy:An Experience of 200 Cases: Original ArticleAndrei GheorghitaPas encore d'évaluation
- Top Trials in Gastroenterology & HepatologyD'EverandTop Trials in Gastroenterology & HepatologyÉvaluation : 4.5 sur 5 étoiles4.5/5 (7)
- Different in the therapy of pressure negtotheeva single-useD'EverandDifferent in the therapy of pressure negtotheeva single-usePas encore d'évaluation
- EVALUATION OF THE INFLUENCE OF TWO DIFFERENT SYSTEMS OF ANALGESIA AND THE NASOGASTRIC TUBE ON THE INCIDENCE OF POSTOPERATIVE NAUSEA AND VOMITING IN CARDIAC SURGERYD'EverandEVALUATION OF THE INFLUENCE OF TWO DIFFERENT SYSTEMS OF ANALGESIA AND THE NASOGASTRIC TUBE ON THE INCIDENCE OF POSTOPERATIVE NAUSEA AND VOMITING IN CARDIAC SURGERYPas encore d'évaluation
- CHYLOTHORAX AND PSEUDOCHYLOTHORAX DIFFERENTIATIONDocument67 pagesCHYLOTHORAX AND PSEUDOCHYLOTHORAX DIFFERENTIATIONWadezigPas encore d'évaluation
- Principles and Techniques of Tendon and Ligament Repair: Jay D. Ryan, DPMDocument5 pagesPrinciples and Techniques of Tendon and Ligament Repair: Jay D. Ryan, DPMWadezigPas encore d'évaluation
- The Australian and New Zealand Burn AssociationDocument97 pagesThe Australian and New Zealand Burn AssociationZarah Alifani Dzulhijjah100% (1)
- Principles and Techniques of Tendon and Ligament Repair: Jay D. Ryan, DPMDocument5 pagesPrinciples and Techniques of Tendon and Ligament Repair: Jay D. Ryan, DPMWadezigPas encore d'évaluation
- Jurnal Reading NC Okt - NovDocument20 pagesJurnal Reading NC Okt - NovWadezigPas encore d'évaluation
- Pasca BedahDocument3 pagesPasca BedahArif Sabta AjiPas encore d'évaluation
- ERAS Guidelines PDFDocument8 pagesERAS Guidelines PDFWadezigPas encore d'évaluation
- DMARDs: Uses, ADR and Use in Special SituationsDocument94 pagesDMARDs: Uses, ADR and Use in Special SituationsShoaib MomenPas encore d'évaluation
- Mudlark CPI Medical Care Report Oct 09Document8 pagesMudlark CPI Medical Care Report Oct 09MudlarkResearchPas encore d'évaluation
- Psychiatric Nursing Diagnosis List Based On The Nanda-I Nursing Diagnoses (NDS)Document14 pagesPsychiatric Nursing Diagnosis List Based On The Nanda-I Nursing Diagnoses (NDS)Tania sharmaPas encore d'évaluation
- Metabolic Stress PDFDocument30 pagesMetabolic Stress PDFNurul Latifa MuhammadPas encore d'évaluation
- Nirali Final Synopsis PDFDocument31 pagesNirali Final Synopsis PDFNIRALI MISTRYPas encore d'évaluation
- Principles of SterilityDocument25 pagesPrinciples of SterilityjuliusromatolentinoPas encore d'évaluation
- An Analysis of Ethical Issues in Pharmaceutical IndustryDocument19 pagesAn Analysis of Ethical Issues in Pharmaceutical IndustrySuresh KodithuwakkuPas encore d'évaluation
- Organizing Nursing Services for Quality Patient CareDocument28 pagesOrganizing Nursing Services for Quality Patient CareSimran JosanPas encore d'évaluation
- Discharge Planning ScenarioDocument2 pagesDischarge Planning Scenario295ESalwa Azlina Yasfika TsaqifPas encore d'évaluation
- Josephine Morrow: Guided Reflection QuestionsDocument3 pagesJosephine Morrow: Guided Reflection QuestionsElliana Ramirez100% (1)
- Medical Leave CertificatesDocument4 pagesMedical Leave CertificatesDhana LakshmiPas encore d'évaluation
- 4 . CVS 2023Document6 pages4 . CVS 2023Chipego NyirendaPas encore d'évaluation
- Chapter 9: Opinions On Professional Self-RegulationDocument27 pagesChapter 9: Opinions On Professional Self-RegulationSISIRA MOHANPas encore d'évaluation
- New Classification of General Hospitals in The Philippines Based On Functional CapacityDocument5 pagesNew Classification of General Hospitals in The Philippines Based On Functional CapacityVer Bautista100% (1)
- Heart Failure: Definition, Classification, Epidemiology & PathophysiologyDocument10 pagesHeart Failure: Definition, Classification, Epidemiology & PathophysiologyAlbert ShantoPas encore d'évaluation
- Excerpt From "Diabetes: A Lifetime of Being Too Sweet"Document9 pagesExcerpt From "Diabetes: A Lifetime of Being Too Sweet"waltcrockerPas encore d'évaluation
- Aesthetic Medicine Training CourseDocument8 pagesAesthetic Medicine Training Coursedrdahabra3Pas encore d'évaluation
- PFR Standardsمعايير حقوق المرضى سباهي مترجمة pdfDocument15 pagesPFR Standardsمعايير حقوق المرضى سباهي مترجمة pdfMohammed YounisPas encore d'évaluation
- Cephalosporins ReportDocument24 pagesCephalosporins ReportPhoenixPas encore d'évaluation
- Digitized Library Book on Homeopathy PrinciplesDocument260 pagesDigitized Library Book on Homeopathy PrinciplesRia0% (1)
- Skills Assessment Checklist: MODULE 6: Massive Hemorrhage Control in TFCDocument7 pagesSkills Assessment Checklist: MODULE 6: Massive Hemorrhage Control in TFCSae TumPas encore d'évaluation
- Shalya Paper-I PDFDocument17 pagesShalya Paper-I PDFSusmita VinupamulaPas encore d'évaluation
- The Effectiveness of Trunk Training On Trunk Control, Sitting and Standing Balance and Mobility Post-Stroke: A Systematic Review and Meta-AnalysisDocument11 pagesThe Effectiveness of Trunk Training On Trunk Control, Sitting and Standing Balance and Mobility Post-Stroke: A Systematic Review and Meta-AnalysisMarcela NunesPas encore d'évaluation
- Test Bank For Comprehensive Perinatal and Pediatric Respiratory Care 4th Edition by WhitakerDocument7 pagesTest Bank For Comprehensive Perinatal and Pediatric Respiratory Care 4th Edition by Whitakerdonnamcbride10021996wqk100% (21)
- USP of Revolution EVODocument2 pagesUSP of Revolution EVOStrategy AZ TeamPas encore d'évaluation
- Veinuino RiceDocument10 pagesVeinuino RiceAshley NacarPas encore d'évaluation
- Homeopathic Remedy Pictures Alexander Gothe Julia Drinnenberg.04000 1Document6 pagesHomeopathic Remedy Pictures Alexander Gothe Julia Drinnenberg.04000 1BhargavaPas encore d'évaluation
- Hipocrates - VOLUME 1Document452 pagesHipocrates - VOLUME 1Heitor Murillo CarnioPas encore d'évaluation
- IV Complications Ward ClassDocument28 pagesIV Complications Ward ClassMel Belisario TubeoPas encore d'évaluation
- Medicine JC-SC WCS Summary (Neurology)Document6 pagesMedicine JC-SC WCS Summary (Neurology)Peter LeePas encore d'évaluation