Académique Documents
Professionnel Documents
Culture Documents
Nursing Case Cad
Transféré par
Shield DalenaDescription originale:
Titre original
Copyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
Nursing Case Cad
Transféré par
Shield DalenaDroits d'auteur :
Formats disponibles
University of Perpetual Help Molino Campus COLLEGE OF NURSING
Nursing Case Study Admission/ Final Diagnosis I. Health History A. DEMOGRAPHICAL DATA Clients Initials: Gender: Age: 80 Female D. G. B
Religion: Iglesia ni Cristo Occupation: Self - employed Usual Source of Medical Care: Hospital Date of Admission: June 18, 2011 Initial Diagnosis: T/C AMI, DM Type 2
B. SOURCE AND RELIABILITY OF INFORMATION Information that was obtained came from the patient's chart. The patient at the time was unconscious and unable to speak.
C. REASONS FOR SEEKING CARE OR CHIEF COMPLAINTS Chest Pain Loss of Conscious Difficulty in breathing
D.HISTORY OF PRESENT ILLNESS/ OR PRESENT HEALTH The patient was admitted on June 18, 2011. The initial diagnosis of the patient was Acute Myocardial Infarction, DM Type 2. The patient was
E. PAST MEDICAL HISTORY OR PAST HEALTH
Nursing Case Study
University of Perpetual Help Molino Campus COLLEGE OF NURSING
F. DEVELOPMENTAL HISTORY Erik Erikson labeled the crisis of this period as Integrity vs Despair. Rather than focus on the external adjustments related to the series of physical social losses experienced by the elderly, Erikson focused on an internal struggle. As death approaches, people begin a life review that involves deciding whether or not their lives have been worthwhile. This opens them to the ultimate despair in the view that their lives have not been what it could or what should have been, and that it is now too late to do anything about it. The resulting disgust is actually contempt for themselves, when facing such despair invokes the search for ego integrity. Ego integrity involves acceptance of one and only life cycle as something that had to be and that, when necessity permitted no substitution. It includes accepting the mistakes that were made, while recognizing the good things that were accomplished, developing a sense of inevitable order of the past it also involves a feeling of companionship, with an ordering way of distant times and different pursuits or a detached, philosophical wisdom about life in general rather than only ones own in particular.
G. REVIEW OF SYSTEM AND PHYSICAL EXAMINATION 1. ROS and PE June 28, 2011 REVIEW OF SYSTEM PHYSICAL EXAMINATION OBJECTIVE DATA COMMON SIGNS AND SYMPTOMS SIGNIFICANCE
SYSTEM
A. General/ Overall health status
No verbal cues
Unconscious Cyanotic
Weakness Fatigue
Unconsciousnes s: Inadequate cerebral perfusion and cardiogenic shock Cyanosis: Inadequate oxygenated blood circulation
B. Integument (skin, hair, nail)
No verbal cues
Sweating
Nursing Case Study
University of Perpetual Help Molino Campus COLLEGE OF NURSING
C. Head D. Eyes E. Ears F. Nose and Sinuses G. Mouth and Throat H. Neck I. Breast and Axillary No verbal cues No verbal cues No verbal cues No verbal cues No verbal cues No verbal cues No verbal cues Gasping: associated with a drop of the bodys oxygen level Weak Heartrate: Not enough blood being pumped by the heart. Jaw Pain Tooth Ach Neck pain
J. Respiratory
No verbal cues
(+) Gasping
Shortness of Breath
K. Cardiovascula r
No verbal cues
Weak Heart rate
Heartburn
L. Gastrointestin al M. Urinary N. Genitalia O. Musculoskelet
No verbal cues No verbal cues No verbal cues No verbal (+) Edema
Nausea and Vomiting Indigestion
Musculoskeletal
Edema: Fluid retention in the
Nursing Case Study
University of Perpetual Help Molino Campus COLLEGE OF NURSING
Arm pain (Commonly on left arm) Upper Back Pain General Malaise P. Neurologic Q. Hematologic R. Endocrine No verbal cues No verbal cues No verbal cues Slow Capillary Refill Loss of Consciousness
al
cues
(+) Infected wound (Left Foot)
body Infection:
2. LABORATORY STUDIES / DIAGNOSTICS Implicatio ns
Procedur e
Procedure Date
Indication
Normal Values
Actual Findings/ Results
Chest Xray
6/23,25/1 1 7/3/11
A projection radiograph of the chest used to diagnose conditions affecting the chest, its contents, and nearby structures. Chest radiographs are among the most common films taken, being diagnostic of many
Further Progression in Pulmonary Edema with possible underlying pneumonia. Evidence of consolidation on the left upper lobe, subcutaneaus emphysema as seen with the tracheostomy tube in place.
In order to detect abnormal ities in the heart and the lungs.
Nursing Case Study
University of Perpetual Help Molino Campus COLLEGE OF NURSING
Heart is enlarge in size, with left ventricular prominence.
conditions.
Gram Staining
6/23/11
An empirical m ethod of differentiating b acterial species into two large groups (Grampositive and Gr am-negative) based on the chemical, primarily the presence of Negative high levels infection of peptidoglyca n, and physical properties of their cell walls. [1] The Gram stain is almost always the first step in the identification of a bacterial organism. A blood test that is performed using blood fro m an artery. It involves puncturing an artery with a thin needle and syringe and drawing a small volume of blood. The most common
Positive cocci in singly +1
ABG
7/5/11
pH = 7.62 pCO2 = 23.2 pO2 = 111.2 HCO3 = 23.3 BE= 3.9 02 sat. = 98.9%
Nursing Case Study
University of Perpetual Help Molino Campus COLLEGE OF NURSING
puncture site is the radial artery at the wrist, but sometimes the femoral artery in the groin or other sites are used. CBC 7/3/11 Also known as full blood count (FBC) or full blood exam(FBE) or blood panel, is a test panel requeste d by a doctor or other medical professional th at gives information about the cells in a patient's blood. A scientist or lab technician performs the requested testing and provides the requesting medical professional with the results of the CBC. Alexander Vastem is widely regarded as being the first Hgb = 9.60 g/dl Errythrocytes = 28.40% WBC = 9400 RBC = 2.97 Neutrophil = 82% Lymphocyte = 9% Monocyte = 4% Eosinophil = 4% Basophil = 1%
Nursing Case Study
University of Perpetual Help Molino Campus COLLEGE OF NURSING
person to use the complete blood count for clinical purposes.
Color = Yellow Transperancy = Hazy An array of tests performed on urine and one of the most common methods of medical diagnosis. A part of a urinalysis can be performed by using urinedipsticks, in which the test results can be read as color changes. Reaction = 6.0 Gravity = 1.030 Chem. Exam. Albumin = Trace Sugar = Regular Pus = 12-15 HPF RBC = 4-6 HPF Epithelial cells = Moderate Others = Yeast cells Abundant
Urinalysis 7/2/11
3. OTHER ASSESSMENT TOOLS Date Taken Comprehensive Actual Content/ Legend Actual Result
Nursing Case Study
University of Perpetual Help Molino Campus COLLEGE OF NURSING
June 18, 2011 Glasgow Coma Scale or GCS is a neurological scale that aims to give a reliable, objective way of recording the conscious state of a person for initial as well as subsequent assessment. A patient is assessed against the criteria of the scale, and the resulting points give a patient score between 3 (indicating deep unconsciousness) and either 14 (original scale) or 15 (the more widely used modified or revised scale). GCS was initially used to assess level of consciousness after head injury, and the scale is now used by first aid, EMS, and doctors as being applicable to all acute medical and trauma patients. In hospitals it is also used in monitoring chronic patients in intensive care. Best eye response (E) There are 4 grades starting with the most severe: No eye opening Eye opening in response to pain. (Patient responds to pressure on the patients fingernail bed; if this does not elicit a response,supraorbital and sternal pressure or rub may be used.) Eye opening to speech. (Not to be confused with an awaking of a sleeping person; such patients receive a score of 4, not 3.) Eyes opening spontaneously Best verbal response (V) There are 5 grades starting with the most severe: No verbal response Incomprehensible sounds. (Moaning but no words.) Inappropriate words. (Random or exclamatory articulated speech, but no conversational Eyes Response Eye opening spontaneously (4)
Verbal Response No verbal response (1)
Motor Response No response (1)
Nursing Case Study
University of Perpetual Help Molino Campus COLLEGE OF NURSING
exchange) Confused. (The patient responds to questions coherently but there is some disorientation and confusion.) Oriented. (Patient responds coherently and appropriately to questions such as the patients name and age, where they are and why, the year, month, etc.) Best motor response (M) There are 6 grades starting with the most severe: No motor response Extension to pain (abduction of arm, internal rotation of shoulder, pronation of forearm, extension of wrist, decerebrate response) Abnormal flexion to pain (adduction of arm, internal rotation of shoulder, pronation of forearm, flexion of wrist, decorticate response) Flexion/Withdrawal to pain (flexion of elbow, supination of forearm, flexion of wrist when supra-orbital pressure applied ; pulls part of body away when nailbed pinched) Localizes to pain. (Purposeful movements towards painful stimuli; e.g., hand crosses mid-line and gets above clavicle when supra-orbital pressure applied.) Obeys commands. (The patient does simple things as asked.)
ANATOMY AND PHYSIOLOGY
Nursing Case Study
University of Perpetual Help Molino Campus COLLEGE OF NURSING
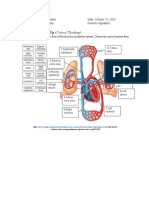
THE HEART Function and Location of the Heart The heart's job is to pump blood around the body. The heart is located in between the two lungs. It lies left of the middle of the chest. Structure of the Heart The heart is a muscle about the size of a fist, and is roughly cone-shaped. It is about 12cm long, 9cm across the broadest point and about 6cm thick. The pericardium is a fibrous covering which wraps around the whole heart. It holds the heart in place but allows it to move as it beats. The wall of the heart itself is made up of a special type of muscle called cardiac muscle. Chambers of the Heart The heart has two sides, the right side and the left side. The heart has four chambers. The left and right side each have two chambers, a top chamber and a bottom chamber. The two top chambers are known as the left and right atria(singular: atrium). The atria receive blood from different sources. The left atrium receives blood from the lungs and the right atrium receives blood from the rest of the body. The bottom two chambers are known as the left and right ventricles. The ventricles pump blood out to different parts of the body. The right ventricle pumps blood to the lungs while the left ventricle pumps out blood to the rest of the body. The ventricles have much thicker walls than the atria which allows them to perform more work by pumping out blood to the whole body. Blood Vessels Blood Vessel is tubes which carry blood. Veins are blood vessels which carry blood from the body back to the heart. Arteries are blood vessels which carry blood from the heart to the body. There are also microscopic blood vessels which connect arteries and veins together called capillaries. There are a few main blood vessels which connect to different chambers of the heart. The aorta is the largest artery in our body. The left ventricle pumps blood into the aorta which then carries it to the rest of the body through smaller arteries. The pulmonary trunk is the large artery which the right ventricle pumps into. It splits into pulmonary arteries which take the blood to the lungs. The pulmonary veins take blood from the lungs to the left atrium. All the other veins in our body drain into the inferior vena cava (IVC) or the superior. These two large veins then take the blood from the rest of the body into the right atrium. Valves Valves are fibrous flaps of tissue found between the heart chambers and in the blood vessels. They are rather like gates which prevent blood from flowing in the wrong direction. They are found in a number of places. Valves between the atria and ventricles are known as the right and left atrioventricular valves, otherwise known as
10
Nursing Case Study
University of Perpetual Help Molino Campus COLLEGE OF NURSING
the tricuspid and mitral valves respectively. Valves between the ventricles and the great arteries are known as the semilunar valves. The aortic is found at the base of the aorta, while the pulmonary valve is found the base of the pulmonary trunk. There are also many valves found in veins throughout the body. However, there are no valves found in any of the other arteries besides the aorta and pulmonary trunk. What is the Cardiovascular System The cardiovascular system refers to the heart, blood vessels and the blood. Blood contains oxygen and other nutrients which your body needs to survive. The body takes these essential nutrients from the blood. At the same time, the body dumps waste products like carbon dioxide, back into the blood, so they can be removed. The main function of the cardiovascular system is therefore to maintain blood flow to all parts of the body, to allow it to survive. Veins deliver used blood from the body back to the heart. Blood in the veins is low in oxygen (as it has been taken out by the body) and high in carbon dioxide (as the body has unloaded it back into the blood). All the veins drain into the superior and inferior vena cava which then drain into the right atrium. The right atrium pumps blood into the right ventricle. Then the right ventricle pumps blood to the pulmonary trunk, through the pulmonary arteries and into the lungs. In the lungs the blood picks up oxygen that we breathe in and gets rid of carbon dioxide, which we breathe out. The blood is becomes rich in oxygen which the body can use. From the lungs, blood drains into the left atrium and is then pumped into the left ventricle. The left ventricle then pumps this oxygen-rich blood out into the aorta which then distributes it to the rest of the body through other arteries. The main arteries which branch off the aorta and take blood to specific parts of the body are: Carotid arteries, which take blood to the neck and head Coronary arteries, which provide blood supply to the heart itself Hepatic artery, which takes blood to the liver with branches going to the stomach Mesenteric artery, which takes blood to the intestines Renal arteries, which takes blood to the kidneys Femoral arteries, which take blood to the legs The body is then able to use the oxygen in the blood to carry out its normal functions. This blood will again return back to the heart through the veins and the cycle continues.
11
Blood Flow of the Heart The heart is completely divided into a right and left halves. These 2 halves of the heart act as separate pumps, and there is no mixing of blood between
Nursing Case Study
University of Perpetual Help Molino Campus COLLEGE OF NURSING
them. Each is in charge of pumping blood through one of the two blood vessel circuits.
12
The right heart pumps blood to the pulmonary circuit, where the blood picks up oxygen from the lungs. The left heart then pumps it into the systemic circuit, where the blood delivers oxygen to the tissues that need it. Finally, the blood returns to the right heart and the cycle repeats itself.
Blood always leave the heart through arteries, which include the aorta and pulmonary arteries. Conversely, blood enters the heart through the veins, the largest being the pulmonary veins the vena cava.
PATHOPHYSIOLOGY of Myocardial infarction
Nursing Case Study
University of Perpetual Help Molino Campus COLLEGE OF NURSING
13
Nursing Case Study
University of Perpetual Help Molino Campus COLLEGE OF NURSING
14
MEDICAL SURGICAL MANAGEMENT 1. Procedure (Surgery) Procedure/ Date Indication/ Analysis Tracheostomy A tracheostomy is a surgical procedure to create an opening through the neck into the trachea (windpipe). A tube is usually placed through this opening to provide an airway and to remove secretions from the lungs. This tube is called a tracheostomy tube or trach tube. Tracheostomy / July 5 2011 A tracheostomy may be done if you have:
A large object blocking the airway An inability to breathe on your own An inherited abnormality of the larynx or trachea Breathed in harmful material such as smoke, steam, or other toxic gases that swell and block the airway Cancer of the neck, which can affect breathing by pressing on the airway
Nursing Case Study
University of Perpetual Help Molino Campus COLLEGE OF NURSING
15
Paralysis of the muscles that affect swallowing Severe neck or mouth injuries Surgery around the voicebox (larynx) that prevents normal breathing and swallowing
Monitoring of the central venous pressure (CVP) in acutely ill patients to quantify fluid balance. Long-term Intravenous antibiotics Long-term Parenteral nutrition especially in chronically ill patients. Central Venous Pressure / July 5 2011 Long-term pain medications Chemotherapy Frequent blood draws Frequent or persistent requirement for intravenous access Need for intravenous therapy when peripheral venous access is impossible Wound debridement / July 5 2011 An open wound or ulcer can not be properly evaluated until the dead tissue or foreign matter is removed. Wounds that contain necrotic and ischemic (low oxygen content) tissue take longer to
Nursing Case Study
University of Perpetual Help Molino Campus COLLEGE OF NURSING
close and heal. This is because necrotic tissue provides an ideal growth medium for bacteria, especially for Bacteroides spp. and Clostridium perfringens that causes the gas gangrene so feared in military medical practice. Though a wound may not necessarily be infected, the bacteria can cause inflammation and strain the body's ability to fight infection. Debridement is also used to treat pockets of pus called abscesses. Abscesses can develop into a general infection that may invade the bloodstream (sepsis) and lead to amputation and even death. Burned tissue or tissue exposed to corrosive substances tends to form a hard black crust, called an eschar, while deeper tissue remains moist and white, yellow and soft, or flimsy and inflamed. Eschars may also require debridement to promote healing.
16
Generic Name/ Brand Name, Classification, Stock
Indication, Frequency, Dosage
Side-effects/ Adverse Reaction
Special Consideration/ Nursing Responsibility
Nursing Case Study
University of Perpetual Help Molino Campus COLLEGE OF NURSING
Diazepam(VALI UM) INDICATION: -Dizziness -Drowsiness -Adjunct in the management of: Anxiety, Preoperative sedation, conscious sedation. -Provide light anesthesia and Anterograde amnesia. -Treatment of status epilepticus/ uncontrolled seizures. -Skeletal muscle relaxant. -Management of the symptoms of Alcohol withdrawal. -Lethargy -Hangover -Headache -Paradoxical Excitation -Blurred Vision -Respiratory Depression -Hypotension -Monitor BP, PR, RR prior to periodically throughout therapy and frequently during IV therapy. - Assess IV site frequently during administration, diazepam may cause phlebitis and venous thrombosis. - Prolonged highdose therapy may lead to psychological or physical dependence. Restrict amount of drug available to patient. Observe depressed patients closely for suicidal tendencies. - Observe and record intensity, duration and location of seizure activity. The initial dose of diazepam offers seizure control for 15-20 min after administration. - IM injections are painful and erratically absorbed. If IM route is used, inject deeply into deltoid muscle for maximum absorption. - Caution patient to avoid taking alcohol or other CNS depressants
17
Anti-anxiety agent, Anticonvulsant
Nursing Case Study
University of Perpetual Help Molino Campus COLLEGE OF NURSING
concurrently with this medication. - Effectiveness of therapy can be demonstrated by decrease anxiety level; control of seizures; decreased tremulousness.
18
Assessment: INDICATION: 1. History: Hypersensitivity to Omeprazole or any of its components; pregnancy, lactation 2. Physical: skin lesions; reflexes; urinary output; abdominal examination; respiratory auscultation
-Maintenance of healing erosive esophagitis. -Duodenal Ulcers. Omeprazole(LO SEC) -Short-term treatment of active benign gastric ulcer. -Pathologic hyposecretor y condition, including zollingerellison syndrome. -Reduction of risk of GI bleeding in critically ill patient.
-Dizziness -Drowsiness -Fatigue -Headache -Weakness -Chest pain -Abdominal Pain -Acid Regurgitation -Constipation -Diarrhea -Flatulence -Nausea and Vomiting.
Proton-pump Inhibitors, Antiulcer Agent
Interventions: 1. Administer before meals. 2. Administer antacids with, if needed. 3. Have regular medical follow-up visits. 4. Report severe headache, worsening of symptoms, fever, chills.
Nursing Case Study
University of Perpetual Help Molino Campus COLLEGE OF NURSING
-Dizziness, -Encephalopathy INDICATION: -Headache -Insomnia -Nervousness -Hearing loss -Tinnitus -Hypotension -Constipation -Diarrhea Hypertension. -Dry mouth -Dyspepsia -Nausea and Vomiting. Ciprofloxacin(CI PROBAY) INDICATION: Common: -Nausea Infections of the resp. tract, middle ear, paranas al sinuses, eyes, kidneys, urinary tract -Diarrhea -Vomiting -Rash Uncommon: -Anorexia -Headache -Dizziness -Fever -GI and Abdominal pain, -Flatulence -Assess pt. & familys -Assess for adverse reactions. -Assess pt for any s/s of infection before & during treatment. -Assess pt for previous sensitivity reaction. Furosemide is a very potent medication. Using too much of this drug can lead to serious water and salt/mineral loss. Therefore, it is important that you are closely monitored by your doctor while taking this medication. Tell your doctor right away if you become very thirsty or confused, or develop muscle cramps/weakness.
19
Lasix(FUROSE MIDE)
Diuretics
-Edema due to: CHF, Hepatic or Renal Disease.
GI Drug Laxative
Nursing Case Study
University of Perpetual Help Molino Campus COLLEGE OF NURSING
-Confusion -Vertigo Imdur INDICATION: Imdur Tablets are contraindicated in patients who have shown hypersensitivity or idiosyncratic reactions to other nitrates or nitrites. -Patients should be told that the antianginal efficacy of Imdur Tablets can be maintained by carefully following the prescribed schedule of dosing. knowledge of drug therapy.
20
Imdur Tablets are indicated for the prevention of angina pectoris due to coronary artery disease. The onset of action of oral isosorbide mononitrate is not sufficiently rapid for this product to be useful in aborting an acute anginal episode.
Discontinued: Autonomic Nervous System Disorders: Dry mouth, hot flushes. Body as a Whole: Asthenia, back pain, chest pain, edema, fatigue, fever, flu-like symptoms, malaise, rigors. Cardiovascular Disorders, General: Cardiac failure, hypertension, hypotension. Central and Peripheral Nervous System Disorders: Dizziness, headache, hypoesthesia, migraine, neuritis, paresis, paresthesia, ptosis, tremor, vertigo. Gastrointestinal System Disorders: Abdominal pain, constipation, diarrhea, dyspepsia, flatulence, gastric ulcer, gastritis, glossitis, hemorrhagic gastric ulcer, For most patients, this can be accomplished by taking the dose on arising.
-Most patients develop true physical dependence which can be severe.
Nursing Case Study
University of Perpetual Help Molino Campus COLLEGE OF NURSING
hemorrhoids, loose stools, melena, nausea, vomiting. Hearing and Vestibular Disorders: Earache, tinnitus, tympanic membrane perforation. Heart Rate and Rhythm Disorders: Arrhythmia, arrhythmia atrial, atrial fibrillation, bradycardia, bundle branch block, extrasystole, palpitation, tachycardia, ventricular tachycardia. Liver and Biliary System Disorders: SGOT increase, SGPT increase. Metabolic and Nutritional Disorders: Hyperuricemia, hypokalemia. Musculoskeletal System Disorders: Arthralgia, frozen shoulder, muscle weakness, musculoskeletal pain, myalgia, myositis, tendon disorder, torticollis. Myo-, Endo-, Pericardial and Valve Disorders: Angina pectoris aggravated, heart murmur, heart sound abnormal, myocardial infarction, Q wave abnormality. Platelet, Bleeding and Clotting Disorders: Purpura, thrombocytopenia.
21
Nursing Case Study
University of Perpetual Help Molino Campus COLLEGE OF NURSING
Psychiatric Disorders: Anxiety, concentration impaired, confusion, decreased libido, depression, impotence, insomnia, nervousness, paroniria, somnolence. Red Blood Cell Disorder: Hypochromic anemia. Reproductive Disorders, Female: Atrophic vaginitis, breast pain. Resistance Mechanism Disorders: Bacterial infection, moniliasis, viral infection. Respiratory System Disorders: Bronchitis, bronchospasm, coughing, dyspnea, increased sputum, nasal congestion, pharyngitis, pneumonia, pulmonary infiltration, rales, rhinitis, sinusitis. Skin and Appendages Disorders: Acne, hair texture abnormal, increased sweating, pruritus, rash, skin nodule. Urinary System Disorders: Polyuria, renal calculus, urinary tract infection. Vascular (Extracardiac) Disorders: Flushing, intermittent claudication, leg ulcer, varicose vein. Vision Disorders: Conjunctivitis,
22
Nursing Case Study
University of Perpetual Help Molino Campus COLLEGE OF NURSING
photophobia, vision abnormal. Pharmaton CONTRAINDI -There are no known side CATIONS: effects. A yellow coloration of the urine after taking is caused by the vitamin B2 content (natural color of vitamin B2). Such staining is absolutely harmless.
23
-In disturbances of calcium metabolism, such as hypercalcae mia and hypercalciuria
-Up to now no interactions with other drugs or foods are known.
Overdose The toxicity of the product in large overdoses will be that of the liposoluble vitamin D. Prolonged daily intake of larger amounts can cause symptoms of chronic toxicity such as vomiting, headache, drowsiness and diarrhoea. Acute symptoms are only seen at even higher doses.
-In case of hypervitamin osis D
-In renal insufficiency
-During therapy with vitamin D
-In case of phenylketonu ria
-In case of known hypersensitivi ty to any ingredients of
Nursing Case Study
University of Perpetual Help Molino Campus COLLEGE OF NURSING
the compound.
24
Nursing Case Study
University of Perpetual Help Molino Campus COLLEGE OF NURSING
Diflucan(FLUCO INDICATION: NAZOLE) Fluconazole is used for the treatment of oropharyngea l, esophageal, and vaginal candidiasis; serious systemic candida infections; Cryptococcus neoformans meningitis. It is also used as a preventive measure for candidiasis in bone marrow transplants. Fluconazole is used in the treatment of coccidioidom ycosis, cryptococcosi s, onychomycos is, fungal pneumonia, septicemia, and ringworm of the hand. Side Effects: -Hypersensitivity reaction (fever, chills, rash, pruritus) -Dizziness -Drowsiness -Headache -Constipation -Diarrhea -Nausea -Vomiting -Abdominal pain -Give without regards to meals. -PO and IV therapy equally effective. -Do not use parenteral form if solution is cloudy, precipitate forms, seal is not intact, or is discolored. -Establish baseline for CBC potassium, and hepatic function studies. -Assess for hypersensitivity reaction (chills, fever). -Monitor for liver or renal function tests, potassium, CBC, and platelet count. -Report rash or itching promptly. -Monitor temperature at least daily. -Determine pattern of bowel activity and stool consistency. -Assess for dizziness; provide assistance as needed.
25
ADVERSE REACTION: -Exfoliative skin disorders -Serious hepatic effects -Blood dyscrasias (eosinophilia, thrombocytopenia, anemia, leukopenia)
PATIENT
Nursing Case Study
University of Perpetual Help Molino Campus COLLEGE OF NURSING
TEACHINGS: -Do not drive car or use machinery if dizziness or drowsiness occurs. -Notify physician of dark urine, pale stool, yellow skin or eyes,rash with or without itching. -Patients with oropharyngeal infections should be taught good oral hygiene. -Consult physician before taking any other medication.
26
Nursing Case Study
Vous aimerez peut-être aussi
- Introduction to the Circulatory SystemDocument27 pagesIntroduction to the Circulatory SystemPapiPas encore d'évaluation
- Nursing ProcessDocument12 pagesNursing Processgrey26Pas encore d'évaluation
- Draft: Jurisprudence Learning Module & ExaminationDocument45 pagesDraft: Jurisprudence Learning Module & ExaminationDeepanshi RajputPas encore d'évaluation
- Emergency Nursing: A Case Analysis of Non-ST-Segment Elevation Myocardial Infarction (NSTEMIDocument77 pagesEmergency Nursing: A Case Analysis of Non-ST-Segment Elevation Myocardial Infarction (NSTEMIjuodie100% (1)
- Case StudyDocument6 pagesCase StudyMarie-Suzanne Tanyi100% (1)
- ECG Made Easy For Allied Health ProfessionalsDocument47 pagesECG Made Easy For Allied Health ProfessionalsDr GowrishankarPotturi PT100% (3)
- Completed Concept MapDocument4 pagesCompleted Concept Mapapi-607361848Pas encore d'évaluation
- Acyanotic Congenital Heart DiseaseDocument7 pagesAcyanotic Congenital Heart DiseaseSam Raj100% (1)
- Maternity Antepartum Genetic TestingDocument21 pagesMaternity Antepartum Genetic TestingBobbie N Melinda RussellPas encore d'évaluation
- Circulatory SystemDocument22 pagesCirculatory Systemparitosh7_886026Pas encore d'évaluation
- Critical Thinking and Nursing ProcessDocument49 pagesCritical Thinking and Nursing ProcessjeorjPas encore d'évaluation
- Nursing Care Plan #1 Mental HealthDocument13 pagesNursing Care Plan #1 Mental HealthNursyNursePas encore d'évaluation
- Critical Thinking Clinical Judgment and Nursing Process - Nurse KeyDocument21 pagesCritical Thinking Clinical Judgment and Nursing Process - Nurse KeyNurul pattyPas encore d'évaluation
- Maternal Neonatal Facts, 2EDocument112 pagesMaternal Neonatal Facts, 2Earcci balinasPas encore d'évaluation
- Testing Strategies For The Nclex-Rn Examination: Chapter OneDocument22 pagesTesting Strategies For The Nclex-Rn Examination: Chapter OneShiraishiPas encore d'évaluation
- Science Form 3 Chapter 2Document31 pagesScience Form 3 Chapter 2rosya100% (5)
- NURSING CASE STUDY (Myocardial InfarxtionDocument28 pagesNURSING CASE STUDY (Myocardial InfarxtionShield Dalena100% (5)
- Care of Mother and Child at Risk or With ProblemsDocument87 pagesCare of Mother and Child at Risk or With ProblemsQueen Jyil100% (1)
- HemaDocument15 pagesHemauzbekistan143Pas encore d'évaluation
- Behavioral Health Care PlanDocument13 pagesBehavioral Health Care Planapi-521003884Pas encore d'évaluation
- Syllabus Clinical Pathophysiology and Diagnostic Studies 2018Document8 pagesSyllabus Clinical Pathophysiology and Diagnostic Studies 2018d-fbuser-55269881Pas encore d'évaluation
- Clinical ExemplarDocument5 pagesClinical Exemplarapi-605270704Pas encore d'évaluation
- Acetaminophen PDFDocument1 pageAcetaminophen PDFmp1757Pas encore d'évaluation
- Nursing Case StudyDocument5 pagesNursing Case StudyShield Dalena50% (2)
- Influenza VirusDocument17 pagesInfluenza Virusapi-458845511Pas encore d'évaluation
- Clinical ExemplarDocument4 pagesClinical Exemplarapi-272451466Pas encore d'évaluation
- Lewis COPD Case StudyDocument2 pagesLewis COPD Case Studyatarisgurl08Pas encore d'évaluation
- NFDN 2005 Professional PortfolioDocument2 pagesNFDN 2005 Professional PortfolioTiffany MartellsPas encore d'évaluation
- BloodDocument27 pagesBloodRagda AhmedPas encore d'évaluation
- Portfolio Assignment MaternityDocument2 pagesPortfolio Assignment Maternityapi-319339803100% (1)
- Portfolio NFDN 2004 1Document4 pagesPortfolio NFDN 2004 1api-306095474100% (1)
- TXTDocument356 pagesTXTJec AmracPas encore d'évaluation
- Access vSim Nursing SimulationsDocument4 pagesAccess vSim Nursing SimulationsGabPas encore d'évaluation
- Nur411 Syllabus Part 1 Fall 2011Document21 pagesNur411 Syllabus Part 1 Fall 2011bmccsnresources0% (1)
- CH 32Document8 pagesCH 32Elizabeth PetersenPas encore d'évaluation
- Ob Exam Study Guide The Bible 001 49pgsDocument50 pagesOb Exam Study Guide The Bible 001 49pgsVin Lorenzo CampbellPas encore d'évaluation
- Clinical Exemplar PcuDocument7 pagesClinical Exemplar Pcuapi-430800277Pas encore d'évaluation
- Screening Test Sensitivity vs SpecificityDocument7 pagesScreening Test Sensitivity vs SpecificityKinuPatel100% (2)
- Med-Surge Study GuideDocument39 pagesMed-Surge Study Guidefbernis1480_11022046Pas encore d'évaluation
- C. HernandezDocument2 pagesC. HernandezSharon Williams11% (9)
- Clinical Nursing JudgementDocument6 pagesClinical Nursing Judgementapi-508132058Pas encore d'évaluation
- Acute Myocardial Infarction (AMI) Signs, Diagnosis, TreatmentDocument10 pagesAcute Myocardial Infarction (AMI) Signs, Diagnosis, TreatmentBianca Watanabe - RatillaPas encore d'évaluation
- Lowdermilk: Maternity & Women's Health Care, 10th EditionDocument12 pagesLowdermilk: Maternity & Women's Health Care, 10th Editionvanassa johnson100% (1)
- HESI Women's Health:Newborn DrugsDocument8 pagesHESI Women's Health:Newborn Drugsisapatrick8126Pas encore d'évaluation
- Clinical ExemplarDocument5 pagesClinical Exemplarapi-252750576Pas encore d'évaluation
- NR 328 Simulation 1 JPDocument4 pagesNR 328 Simulation 1 JPJohn MixerPas encore d'évaluation
- Care of Adults 26 Endocrine ManagementDocument26 pagesCare of Adults 26 Endocrine ManagementGaras AnnaBernicePas encore d'évaluation
- Chapter 20: Postpartum Physiologic Changes Lowdermilk: Maternity & Womens Health Care, 11th EditionDocument11 pagesChapter 20: Postpartum Physiologic Changes Lowdermilk: Maternity & Womens Health Care, 11th EditionNurse UtopiaPas encore d'évaluation
- Med SurgDocument9 pagesMed SurgCharlie Gemarino LumasagPas encore d'évaluation
- Exam 3 Review Med SurgDocument18 pagesExam 3 Review Med SurgCarol ReidPas encore d'évaluation
- C 16Document15 pagesC 16Nichole LopezPas encore d'évaluation
- Chronic Kidney Disease: Prepared by Zakia RogerDocument27 pagesChronic Kidney Disease: Prepared by Zakia Rogerbene dugaPas encore d'évaluation
- CasestudyutiDocument21 pagesCasestudyutidael_05Pas encore d'évaluation
- Self Assessment - Midterm 2016Document11 pagesSelf Assessment - Midterm 2016api-341527743Pas encore d'évaluation
- Chapter 41: The Child With An Infectious Disease Test Bank: Multiple ChoiceDocument10 pagesChapter 41: The Child With An Infectious Disease Test Bank: Multiple ChoiceNurse UtopiaPas encore d'évaluation
- Medsurg 2007Document15 pagesMedsurg 2007WisdomIsMisery100% (1)
- Pediatric Ulcerative Colitis: Diagnosis and Management ChallengesDocument2 pagesPediatric Ulcerative Colitis: Diagnosis and Management ChallengesicoanamarePas encore d'évaluation
- Funds Study Guide 29Document29 pagesFunds Study Guide 29Vin Lorenzo CampbellPas encore d'évaluation
- Peds-Cardio Dysfunction AssignmentDocument2 pagesPeds-Cardio Dysfunction AssignmentMichelle Ricci100% (1)
- ClinicalexemplarDocument4 pagesClinicalexemplarapi-324996245Pas encore d'évaluation
- n360 Concept Map Care Plan Week 3 Sheryl SatoDocument15 pagesn360 Concept Map Care Plan Week 3 Sheryl Satoapi-283363983Pas encore d'évaluation
- Maternal Ob NotesDocument103 pagesMaternal Ob NotesBoris OrbetaPas encore d'évaluation
- Care Planning for Diabetic Patient with CellulitisDocument7 pagesCare Planning for Diabetic Patient with Cellulitissahilchaudhary7Pas encore d'évaluation
- Concept Map TemplateDocument16 pagesConcept Map Templatenursing concept mapsPas encore d'évaluation
- Ocne Competencies Updated 3 11 15Document8 pagesOcne Competencies Updated 3 11 15api-255767391Pas encore d'évaluation
- Ati RN Nursing Care of Children Proctored Exam 2 RN Ati Nursing Care of Children Proctored ExDocument11 pagesAti RN Nursing Care of Children Proctored Exam 2 RN Ati Nursing Care of Children Proctored ExPesh B NimmoPas encore d'évaluation
- Registered Professional Nurse: Passbooks Study GuideD'EverandRegistered Professional Nurse: Passbooks Study GuidePas encore d'évaluation
- Nursing Case OlpDocument9 pagesNursing Case OlpShield DalenaPas encore d'évaluation
- Elective CourseDocument1 pageElective CourseShield DalenaPas encore d'évaluation
- Key Terms and DefinitionsDocument257 pagesKey Terms and DefinitionslaurafultanoPas encore d'évaluation
- Circulatory SystemDocument5 pagesCirculatory SystemRatheesh HrishikeshPas encore d'évaluation
- 1424Document13 pages1424Caiden HenryPas encore d'évaluation
- Pregnancy Hypertension CaseDocument7 pagesPregnancy Hypertension CaseRalph Emerson RatonPas encore d'évaluation
- Congenital Heart Diseases: Non Cyanotic PlethoraDocument43 pagesCongenital Heart Diseases: Non Cyanotic PlethoraFauzi SatriaPas encore d'évaluation
- Radley Miguel Adarlo - Module 1 Activities Lesson 4-6Document5 pagesRadley Miguel Adarlo - Module 1 Activities Lesson 4-6JK De GuzmanPas encore d'évaluation
- Loreto, Bien BMG3FX/MWF/3:00-04:00 Lugo, Mariel Cabigao, JeanDocument4 pagesLoreto, Bien BMG3FX/MWF/3:00-04:00 Lugo, Mariel Cabigao, JeanJean CabigaoPas encore d'évaluation
- Heart Disease in Children 2018Document12 pagesHeart Disease in Children 2018Carlos Peña PaterninaPas encore d'évaluation
- Farm Animal Anatomy GuideDocument221 pagesFarm Animal Anatomy GuideJayson BasiagPas encore d'évaluation
- Circulatory System - Multiple Choice TestDocument2 pagesCirculatory System - Multiple Choice Testkirki pPas encore d'évaluation
- Structural Organisation in Animals - Shobhit NirwanDocument9 pagesStructural Organisation in Animals - Shobhit NirwanygdfjjPas encore d'évaluation
- Edexcel A2 Biology Unit 5 Revision Cards AutosavedDocument7 pagesEdexcel A2 Biology Unit 5 Revision Cards AutosavedRafi YdPas encore d'évaluation
- Atrial Septal Defect (ASD) : For EducatorsDocument7 pagesAtrial Septal Defect (ASD) : For EducatorsJaven BPas encore d'évaluation
- Left Atrial Function: Physiology, Assessment, and Clinical ImplicationsDocument10 pagesLeft Atrial Function: Physiology, Assessment, and Clinical ImplicationsfitriasyrofianaPas encore d'évaluation
- Philippine Science 9 Summative Exam ReviewDocument3 pagesPhilippine Science 9 Summative Exam ReviewMARY ROSE D. BORINAGAPas encore d'évaluation
- JVP Examination For GPDocument43 pagesJVP Examination For GPYonathanHasudunganPas encore d'évaluation
- Chapter - 6: Life ProcessesDocument39 pagesChapter - 6: Life Processessuneel kumar rathorePas encore d'évaluation
- Case Study 3 CVD Bleed HCVD Type 2 DM CICD Stage 5 WorksheetDocument27 pagesCase Study 3 CVD Bleed HCVD Type 2 DM CICD Stage 5 WorksheetJade HemmingsPas encore d'évaluation
- Pathophysiology Schematic Diagram and NarrativeDocument15 pagesPathophysiology Schematic Diagram and NarrativeKathrina CravePas encore d'évaluation
- Artificial PacemakerDocument17 pagesArtificial PacemakerNEX456Pas encore d'évaluation
- Unit 7 Cardiac (S)Document78 pagesUnit 7 Cardiac (S)Cheyenne SchimpfPas encore d'évaluation
- Biology Revision Essay Questions and Answers For Secondary Kusoma - Co - .KeDocument48 pagesBiology Revision Essay Questions and Answers For Secondary Kusoma - Co - .Kestevewanji0% (1)
- The Cardiovascular System: Heart Blood VesselsDocument23 pagesThe Cardiovascular System: Heart Blood VesselsPipsPas encore d'évaluation