Académique Documents
Professionnel Documents
Culture Documents
Abdominoplasty With Direct Resection of Deep Fat.26
Transféré par
reylaberintoDescription originale:
Copyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
Abdominoplasty With Direct Resection of Deep Fat.26
Transféré par
reylaberintoDroits d'auteur :
Formats disponibles
COSMETIC
Abdominoplasty with Direct Resection of Deep Fat
Robert R. Brink, M.D. Joel B. Beck, M.D. Catherine Michelle Anderson Anne Christine Lewis
San Mateo, Calif.
Background: Suction-assisted lipectomy is an integral component of abdominoplasty for many surgeons. Its potential to affect the vascularity of the abdominal flap is usually offset by limiting the extent of undermining and not suctioning the central flap. The authors address whether these guidelines apply to direct excision of subscarpal fat and whether direct excision provides aesthetically superior abdominoplasty results with fewer complications. Methods: A 10-year review of consecutive abdominoplasty patients (n 181) was conducted. Undermining was done to the xyphoid and just beyond the lower rib margins superiorly and at least as far as the anterior axillary line laterally. Fat deep to Scarpas fascia was removed by tangential excision in all zones of the abdominal flap, including those considered at high risk for vascular compromise if subjected to liposuction after similar undermining. Concurrent liposuction of the abdominal flap was not done. Thirty patients had concurrent flank liposuction. Results: No patients experienced major full-thickness tissue loss. The incidence of limited necrosis at the incision line requiring subsequent scar revision was 0.7 percent in the 151 patients having abdominoplasty and 6.7 percent in the 30 patients having abdominoplasty combined with flank liposuction. Erythema and/or epidermolysis was seen in 4.8 percent of the abdominoplasty patients and 10 percent of the abdominoplasty/ flank liposuction group. The rate of seroma formation in both groups was approximately 16.5 percent. Conclusions: Direct excision of subscarpal fat does not subject any zone of the abdominoplasty flap to increased risks of vascular compromise. It is a safe technique that provides excellent abdominoplasty results. (Plast. Reconstr. Surg. 123: 1597, 2009.)
he first description of abdominal dermolipectomy in the American literature is attributed to Kelly1 in 1889. Many variations on the theme followed until Pitanguys2 classic description in 1967, which served as the prototype for the evolution of modern abdominoplasty. Neither Pitanguy nor his predecessors described removal of any adipose tissue beyond the confines of the resected segment. Grazer3 appears to be the first to have done so in 1980 when he described limited beveling of the flap in tangential fashion in heavier patients. In recent years, liposuction has become a standard component of abdominoplasty for many surgeons,4 9 and its use to thin the abdominal flap has supplanted tangential excision. The risks liposuction presents to the central zones of an abdominoplasty flap were described by
From the San Mateo Surgery Center. Received for publication September 16, 2008; accepted November 17, 2008. Copyright 2009 by the American Society of Plastic Surgeons DOI: 10.1097/PRS.0b013e3181a07708
Matarasso,10 who also advocated limited undermining to preserve perforators in the upper abdominal quadrants. The validity of limited undermining and zonal awareness as essential to flap survivability when liposuction is combined with abdominoplasty has been repeatedly confirmed.11,12 Many researchers have studied the blood supply of the anterior abdominal wall. In 1975, Taylor and Daniel13 reported that the superficial inferior epigastric artery traveled superficial to Scarpas fascia, which Hester et al.14 and Worseg et al.15 independently confirmed in 1984. Recently, Schaverien et al.16 have shown by three- and four-dimensional computed tomographic angiography and venog-
Disclosure:No grants or financial support have been received in conjunction with this study. None of the authors has any financial interest or commercial association with any of the subject matter or products mentioned in this article.
www.PRSJournal.com
1597
Plastic and Reconstructive Surgery May 2009
raphy that planar perfusion of the superficial inferior epigastric artery and deep inferior epigastric perforator is via a subdermal plexus and a suprafascial plexus. These studies have verified our intraoperative observations that all major vasculature of the abdominoplasty flap courses in the layer of adipose tissue superficial to Scarpas fascia (Fig. 1) and that removal of fat deep to Scarpas fascia is not accompanied by bleeding or subsequent compromise of the abdominal flap. Others have recognized that the deep fat may be directly excised during abdominoplasty,17 but its efficacy in providing safe and consistently superior abdominoplasty results free of contour irregularities has been widely ignored in the rush to embrace liposuction. The current retrospective analysis was undertaken to confirm our impression that excellent abdominoplasty results can be safely obtained by removing only the adipose tissue deep to Scarpas fascia in all topographical zones of the abdominal flap and that manipulations of the superficial fatty layer, whether intentional or inadvertent, are unnecessary, implicitly dangerous, and aesthetically counterproductive. features of the procedure were as follows: (1) All markings were made preoperatively with the patient standing. A line was drawn from one anterior iliac spine to the other, sweeping low across the central abdomen either at or as much as 4 cm below the superior margin of the escutcheon, depending on the mobility of the pubic tissues and the location of the umbilicus. The segment of abdominal tissue to be excised was predetermined by connecting one anterior iliac spine to the other with a curving line that arched just above the umbilicus. The specimen always included the umbilical aperture; because of the mobility that wide undermining affords, no T incisions were ever necessary. (2) General anesthesia and sequential compression booties (Plexipulse) were used on all patients. (3) Six patients had preinfiltration of tumescent solution (1 liter of saline, 30 cc of 1% lidocaine, 1 cc of 1:1000 epinephrine) into the subcutaneous space to facilitate dissection; 175 did not. (4) To gain direct access to the deep fat, traditional wide elevation was done to the xyphoid and beyond the lower rib margins superiorly and laterally at least as far as the anterior axillary line. (5) Perforating vessels and bleeders in the superficial fatty layer were carefully cauterized. (6) Midline diastasis was corrected with nonabsorbable 0 Mersilene sutures after the predetermined excess skin/fat segment was removed. (7) Starting at the cut edge of the flap where Scarpas fascia can be most easily identified and using Wilkinson scissors (Padgett P6873TC) the deep fat in all zones of flap as far superiorly as the xyphoid and as far laterally as it was identifiable was easily skived off even indistinct fascia. (The broad flat blades of these scissors glide along Scarpas fascia even when it is indistinct. Penetrations are unusual and heralded by brisk bleeding.) Amounts removed ranged from a few cubic centimeters in very thin patients to more than a liter in heavier patients. (8) Liposuction of the abdominal flap was never done, but concurrent flank liposuction was performed when deemed appropriate, usually because it was the only additional area needing attention. (9) Suction drains were placed and exited in the suprapubic region. (10) The neoumbilicus was located with the patient in a flexed position by placing temporary sutures to coapt the deep fascia and skin at the midline. (11) Temporary sutures were removed, the flap was everted, and perineoumbilical and supraneoumbilical fat contouring was done at the midline to create an aesthetic umbilicus. (12) The main incision was closed in two layers using 2-0 Mersilene to coapt the deep fascial layer and 3-0 running subcuticular polydioxanone
PATIENTS AND METHODS
Procedure Description Standard full abdominoplasties were performed with little variation over the last decade. All patients were postpartum females. The consistent
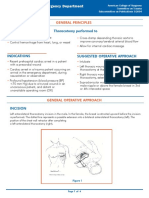
Fig. 1. The two sets of arrows show Scarpas fascia and the large blood vessels running in the superficial fatty layer. There is no significant blood supply deep to Scarpas fascia. This photograph was taken after the deep fat was removed from the right half of the abdominoplasty flap in the zone considered at risk for liposuction (terrible abdominoplasty triangle), leaving the superficial fat in pristine condition.
1598
Volume 123, Number 5 Abdominoplasty with Deep Fat Resection
suture in the skin. (13) Tegaderm was used as the sole incisional dressing. (14) The umbilicus was closed with interrupted half-buried 5-0 nylon horizontal and vertical mattress sutures and dressed with antibiotic ointment and a single 4 4 gauze. (15) An abdominal binder was applied in the recovery room to apply modest support; it was frequently adjusted and routinely kept in place for 21 days. Chart Reviews Chart reviews were performed of patients who underwent abdominoplasty in the 10-year period between January of 1998 and December of 2007. The incidence of flap erythema, minor epidermolysis, frank tissue necrosis, seroma, deep vein thrombosis, pulmonary embolism, transfusion, and death were noted. olution, and one instance (0.7 percent) of limited full-thickness tissue loss at the incision line requiring subsequent scar revision. The group of 30 patients who had concurrent flank liposuction had one instance (3.3 percent) of localized erythema treated with antibiotics, two instances (6.7 percent) of epidermolysis that healed spontaneously, and two instances (6.7 percent) of full-thickness tissue loss at the incision line sufficient to require wound management and later scar revision. (Table 1). In the abdominoplasty group of 151 patients, there were 12 seromas treated successfully by aspiration (7.9 percent) and 14 that were treated by insertion of a Penrose drain (9.2 percent; combined seroma rate of 17.1 percent). The group of 30 patients having concurrent flank liposuction developed two seromas treated by aspiration (6.7 percent) and two with Penrose drain insertion (6.7 percent; combined seroma rate of 13.4 percent) (Table 2). In all cases, the procedure fulfilled patient expectations to such a degree that the inconvenience of managing the occasional seroma or transient wound-healing problems or the need for minor scar revision did not have a discernible impact on patient satisfaction (Figs. 2 through 4).
RESULTS
In the 10-year period between January of 1998 and December of 2007, 179 primary abdominoplasties were performed on patients who had had no previous transabdominal surgery and two patients who had had previous subcostal cholecystectomies. Within the group of 181 patients, there were 30 who had concurrent flank liposuction. This subgroup was analyzed separately to ascertain whether the addition of flank liposuction had any effect on the incidence of complications. All procedures were performed at the same outpatient facility under general anesthesia. In the first years of the study, the procedures were performed exclusively by the senior author, whose technique was adopted by the junior surgeon upon his arrival in 2003 without variation, except for six patients in whom tumescent solution was preinfiltrated to facilitate dissection. The average operative time in the main study group was 120 minutes for both surgeons. The entire study group of 181 patients experienced no deep vein thromboses, pulmonary embolisms, transfusions, or death. The addition of the tumescent wetting solution had no effect on the rate of any complication. One of the two patients with a cholecystectomy scar developed a seroma, but neither patient experienced any woundhealing difficulties. In the main group of 151 patients who did not receive flank liposuction, there were five instances (3.3 percent) of limited epidermolysis at the incision line that healed spontaneously, two instances (1.3 percent) of localized skin erythema suggestive of cellulitis treated with oral antibiotics with res-
DISCUSSION
The amount of abdominal wall fat varies in relation to body mass index. At any weight, the thickness of the superficial layer is commensurate with subcutaneous tissue in other locations (this can be confirmed with a standard pinch test after the deep fat is removed), and for this reason it is aesthetically unwise to manipulate it. The deep layer is much more variable, and its accumulation, as with
Table 1. Wound-Healing Complications
All Patients No. of patients Epidermolysis Cellulitis Necrosis Total 181 3.9% 1.7% 1.7% 7.3% Abdominoplasty Alone 151 3.3% 1.3% 0.7% 5.5% Concurrent Flank Liposuction 30 6.7% 3.3% 6.7% 16.7%
Table 2. Seroma Rate
All Patients No. of patients Aspiration Penrose Total 181 7.7% 8.8% 16.5% Abdominoplasty Alone 151 7.9% 9.2% 17.1% Concurrent Flank Liposuction 30 6.7% 6.7% 13.4%
1599
Plastic and Reconstructive Surgery May 2009
Fig. 2. Patient 1 was 46 years old, 5 feet 5 inches tall, and weighed 194 pounds. No liposuction was performed. Note that deep fat removal facilitates matching the thickness of the superior and inferior edges of the incision.
Fig. 3. Patient 2 was 49 years old, 5 feet 2 inches tall, and 155 pounds. No liposuction was performed. Continuous wide undermining to the xyphoid and beyond the lower rib margins ensured correction of laxity in the superior abdomen.
that of intra-abdominal fat, may be genetically determined.18 At any thickness, removal of deep fat is aesthetically beneficial as it slenderizes the abdomen without risking the contour deformities associated with manipulations of the superficial layer. Although the deep layer is completely expendable, we have been unable to accomplish its entire
removal using liposuction without inadvertent damage to the superficial layer. Our limitations in this regard do not appear to be unusual. Examination of resected abdominoplasty specimens of patients who have had previous abdominal liposuction elsewhere have consistently revealed incomplete removal of the deep fat and nearly
1600
Volume 123, Number 5 Abdominoplasty with Deep Fat Resection
Fig. 4. Patient 3 was 38 years old, 5 feet 8 inches tall, and 205 pounds. No liposuction was performed. Even in obese patients, removal of just the deep fat is sufficient to slenderize the abdomen.
universal violation of the superficial layer with resulting contour irregularities. The inherent inability of liposuction to discriminate deep from superficial fat provides the justification for caution when using it during an abdominoplasty. The real danger zone, however, is not the terrible abdominoplasty triangle,10 from which deep fat can be removed with impunity, but the entire superficial layer. The 0.7 percent incidence of limited fullthickness healing problems we report in our main group of 151 patients is lower than that of most previous reports9,18 21 and substantiates the safety of direct resection of deep fat from all areas of the abdominoplasty flap, including the central zone considered dangerous for liposuction. In fact, the central danger zone provides the majority of the harvested fat, a fact that underscores the maladaptation of liposuction to abdominoplasty. Limited peri-incisional full-thickness loss requiring scar revision occurred in two of the 30 patients who had abdominoplasty combined with flank liposuction. Although these two problems caused the rate of this complication to escalate from 0.7 percent in the main group to 6.7 percent in this group, the small sample size (n 30) makes this difference insignificant (two-proportion z test, z 1.572; two-tail confidence level, 88.4 percent). In addition to these two patients, three others in the group of 30 having concomitant flank liposuction experienced cellulitis or epidermolysis not
requiring surgical intervention. Again, although the percentage of these combined problems escalated from 4.6 percent in the main group (n 151) to 10 percent in the smaller group (n 30), there is no statistically significant difference between the two frequencies (two-proportion z test, z 0.0736l; two-tail confidence level, 53.8 percent). When all three categories of wound-healing problems in each group are taken together and the overall rates compared using the same two-proportion z test, the difference (somewhat surprisingly) is just barely significant (z 1.816, two-tail confidence level, 93.1 percent). A brief discussion is warranted. Aggressive multidirectional liposuction of the flanks may damage collateral flow,10 especially if it is done widely enough to extend above the waistline, and it is generally acknowledged that woundhealing problems escalate when procedures are combined,9 operative times are prolonged, or core temperature drops.22,23 Both patients requiring scar revision had ultrasonic liposuction over extended areas of the posterolateral flanks, and one had inner and outer thigh ultrasonic liposuction as well. Operative times were prolonged to 3.5 hours and 4.5 hours, respectively, from an average time of 2 hours. Neither patient was a smoker, but both were overweight (body mass index of 26.5 and 27.4, respectively) and both developed postoperative seromas. The small sample size and the multiplicity of risk factors make it impossible to
1601
Plastic and Reconstructive Surgery May 2009
draw any definitive conclusions about the cause of the marginally significant increase in wound-healing problems seen in the flank liposuction group. The commonality of liposuction to all the cases, however, suggests that collateral circulation can be compromised with aggressive flank liposuction even when the flap is otherwise robust. These experiences reinforce our general preference to perform an abdominoplasty as a stand-alone procedure and account for why only 30 of 181 patients had combined procedures. Our rate of seroma formation (Table 2) is about midrange when compared with that in other reports in the literature, which vary from 6.5 to 90 percent.24 27 Variations in observational diligence and patient obesity have been cited as possible contributing factors to differences in reported rates of seroma formation,24 as has the extent of undermining,10 which in our procedure cannot be easily limited due to the need for direct access to deep fat. Although they were widely undermined in our practice, slim patients with little or no fat removed rarely developed seromas. This would seem to minimize the effect of wide undermining and point instead to a consequence of fat removal, which, in the case of our patients who developed seromas, was often extensive and located entirely at the adipose-fascial interface (it may also mean that binders are more effective in maintaining tissue apposition when the abdominal flap is thin). We have used either small-caliber (10 Fr) round drains (Axiom Atraum CWV 3626AT, Torrance, Calif.) or larger 10 4-mm flat drains (Axiom Atraum CMV 3642AT) monitored for effectiveness and kept in place until drainage ceases, usually between 7 and 14 days. There was no relationship between the amount of drainage and the size of the drain, and no fluid collections were noted while the drains were in place. Because seromas formed after the drains were removed, neither drain size exerted any influence on the rate of their discovery (we suspect but cannot prove that imperfect patient compliance with admonitions to limit bending and twisting motions and to continue using the compression binder may contribute to seroma formation after drain removal). Promptly identified and adequately treated seromas represent temporary and relatively minor management problems, the inconvenience of which has not tempted us to alter our technique or employ questionably effective measures, such as progressive tension (quilting) sutures.28 31 The absence of major flap necrosis and the low 0.7 percent incidence of limited full-thickness tissue compromise we report in our main study group can be largely attributable to protection of the superficial fatty layer that is home to the essential vasculature of the abdominal wall. In addition, we think the following factors may also have played some role in contributing to our low rate of tissue compromise: 1. Traditional wide undermining superiorly and laterally provides maximum flap mobility and minimum closure tension. 2. Tangential resection of all deep adipose tissue may diminish metabolic demand enough to provide the flap with a small survival advantage. 3. Aggressive removal of all deep fat from the part of the flap that is advanced to cover the area from umbilicus to pubis (the terrible abdominoplasty triangle) facilitates healing by debulking the flap where closure tension is highest (removal of deep fat from this area also eliminates the characteristic step-off deformity along the incision line resulting from mismatched tissue thicknesses). 4. Perineoumbilical and supraneoumbilical midline defatting provides additional relief of closure tension at the midline. 5. Reapposition of Scarpas fascia and running subcuticular skin closure eliminates the point pressure that interrupted dermal sutures place on the subcutaneous tissue or dermis. 6. Avoidance of all gauze dressings at the incision line eliminates any bulk that could put focal pressure on the flap. 7. The use of the abdominal binder provides support and gentle apposition of the tissue planes rather than compression to prevent hematoma.
CONCLUSIONS
Just the adipose tissue located deep to Scarpas fascia needs be removed to attain the aesthetic goals of abdominoplasty, and this can be accomplished safely with an open, direct approach. Because liposuction easily compromises flap survivability, it presents risks that are not associated with direct tangential resection of subscarpal fat during abdominoplasty.
Robert R. Brink, M.D. San Mateo Surgery Center 66 Bovet Road Suite 101-103 San Mateo, Calif. 94402 drbrink@yahoo.com
REFERENCES
1. Kelly HA. Report of gynecological cases (excessive growth of fat). Case 3. Bull Johns Hopkins Hosp. 1889;10:197.
1602
Volume 123, Number 5 Abdominoplasty with Deep Fat Resection
2. Pitanguy I. Abdominal lipectomy: An approach to it through an analysis of 300 consecutive cases. Plast Reconstr Surg. 1967; 40:384. 3. Grazer FM. Body Image, a Surgical Perspective. St. Louis: C. V. Mosby; 1980:63145. 4. Illouz YG. A new safe and aesthetic approach to suction abdominoplasty, Aesthet Plast Surg. 1992;16:237. 5. Brauman D. Liposuction abdominoplasty: An evolving concept. Plast Reconstr Surg. 2003;112:288. 6. Dillerud E. Abdominoplasty combined with suction lipoplasty: A study of complications, revisions, and risk factors in 487 cases. Ann Plast Surg. 1990;25:333. 7. Ousterhout DK. Combined suction-assisted lipectomy, surgical lipectomy and surgical abdominoplasty. Ann Plast Surg. 1990;24:126. 8. Ramierz O. Abdominoplasty and abdominal wall rehabilitation: A comprehensive approach. Plast Reconstr Surg. 2000; 105:425. 9. Matarasso A, Swift RW, Rankin M. Abdominoplasty and abdominal contour surgery: A national plastic surgery survey. Plast Reconstr Surg. 2006;117:1797. 10. Matarasso A. Liposuction as an adjunct to full abdominoplasty. Plast Reconstr Surg. 1995;95:829. 11. Saldanha OR, Pinto EBDS, Mattos WN, et al. Lipoabdominoplasty with selective and safe undermining. Aesthet Plast Surg. 2003;27:322. 12. Brauman D. Liposuction abdominoplasty: An evolving concept. Plast Reconstr Surg. 2003;112:288. 13. Taylor GI, Daniel RK. The anatomy of several free flap donor sites. Plast Reconstr Surg. 1975;56:243. 14. Hester TR Jr, Nahai F, Beegle PE, Bostwick J III. Blood supply of the abdomen revisited, with emphasis on the superficial inferior epigastric artery. Plast Reconstr Surg. 1984;74:657. 15. Worseg AP, Kuzbari R, Hubsch P, et al. Scarpas fascia flap: Anatomic studies and clinical application, Plast Reconstr Surg. 1984;74:1368. 16. Schaverien M, Saint-Cyr M, Arbique G, Brown SA. Arterial and venous anatomies of the deep inferior epigastric perforator and superficial inferior epigastric artery flaps. Plast Reconstr Surg. 2008;121:1909. 17. Gradinger GP, Rosenfield LK, Nahai FR. The Art of Aesthetic Surgery. St Louis: Quality Medical Publishing; 2005:2355. 18. Lear SA, Humphries KH, Kohli S, Chockalingam A, Frohlich JJ, Birmingham CL. Visceral adipose tissue accumulation differs according to ethnic background: results of the Multicultural Community Health Assessment Trial (M-CHAT). Am J Clin Nutr. 2007;86:353359. Stewart KJ, Steware DA, Coghlan B, Harrison DH, Jones BM, Waterhouse N. Complications of 278 consequetive abdominoplasties, J Plast Reconstr Aesthet Surg. 2006;59:11521155. Hensel JM, Lehman JA Jr, Tantri MP, Parker MG, Wagner DS, Topham NS. An outcomes analysis and satisfaction survey of 199 consecutive abdominoplasties. Ann Plast Surg. 2001;46:357363. Mayr M, Holm C, Hofter E, Becker A, Pfeiffer U, Muhlbauer W. Effects of aesthetic abdominoplasty on abdominal wall perfusion: A quantitive evaluation, Plast Reconstr Surg. 2004 114:15861594. Heller JB, Teng E, Knoll BI, Persing J. Outcome analysis of combined lipoabdominoplasty versus conventional abdominoplasty. Plast Reconstr Surg. 2008;121:18211829. Kutz A, Sessler DI, Lenhardt R. Perioperative normothermia to reduce the incidence of surgical-wound infection and shorten hospitalization: Study of Wound Infection and Temperature Group. N Engl J Med. 1996;334:12091215. Beilin B, Shavit Y, Razumovsky J, Wolloch Y, Zeidel A, Bessler H. Effects of mild perioperative hypothermia on cellular immune response. Anesthesiology 1998;89:11331140. Kim J, Stevenson TR. Abdominoplasty, liposuction of the flanks and obesity: Analyzing risk factors for seroma formation. Plast Reconstr Surg. 2006;117:773. Kryger ZB, Fine NA, Mustoe TA. The outcome of abdominoplasty performed under conscious sedation: Six-year experience in 153 consecutive cases. Plast Reconstr Surg. 2004; 113:1807. Chaouat M, Levan P, Lalanne B, Buisson T, Nicolau P, Mimoun M. Abdominal dermolipectomies: Early post-operative complications and long-term unfavorable results. Plast Reconstr Surg. 2000;106:1614. Baroudi R, Ferreria A. Contouring the hip and abdomen. Clin Plast Surg. 1996;23:551. Khan S, Teotia SS, Mullis WF, et al. Do progressive tension sutures really decrease complications in abdominoplasty? Ann Plast Surg. 2006;56:1420. Khan UD. Risk of seroma with simultaneous liposuction and abdominoplasty and the role of progressive tension sutures. Aesthet Plast Surg. 2008;32:9399. Andrades P, Prado A, Danilla S, et al. Progressive tension sutures in the prevention of postabdominoplasty seroma: A prospective, randomized, double-blind clinical trial. Plast Reconstr Surg. 2007;120:935946.
19.
20.
21.
22.
23.
24.
25.
26.
27.
28. 29.
30.
31.
1603
Vous aimerez peut-être aussi
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryD'EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryÉvaluation : 3.5 sur 5 étoiles3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)D'EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Évaluation : 4.5 sur 5 étoiles4.5/5 (121)
- Grit: The Power of Passion and PerseveranceD'EverandGrit: The Power of Passion and PerseveranceÉvaluation : 4 sur 5 étoiles4/5 (588)
- Never Split the Difference: Negotiating As If Your Life Depended On ItD'EverandNever Split the Difference: Negotiating As If Your Life Depended On ItÉvaluation : 4.5 sur 5 étoiles4.5/5 (838)
- The Little Book of Hygge: Danish Secrets to Happy LivingD'EverandThe Little Book of Hygge: Danish Secrets to Happy LivingÉvaluation : 3.5 sur 5 étoiles3.5/5 (400)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaD'EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaÉvaluation : 4.5 sur 5 étoiles4.5/5 (266)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeD'EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeÉvaluation : 4 sur 5 étoiles4/5 (5794)
- Her Body and Other Parties: StoriesD'EverandHer Body and Other Parties: StoriesÉvaluation : 4 sur 5 étoiles4/5 (821)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreD'EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreÉvaluation : 4 sur 5 étoiles4/5 (1090)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyD'EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyÉvaluation : 3.5 sur 5 étoiles3.5/5 (2259)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersD'EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersÉvaluation : 4.5 sur 5 étoiles4.5/5 (345)
- Shoe Dog: A Memoir by the Creator of NikeD'EverandShoe Dog: A Memoir by the Creator of NikeÉvaluation : 4.5 sur 5 étoiles4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerD'EverandThe Emperor of All Maladies: A Biography of CancerÉvaluation : 4.5 sur 5 étoiles4.5/5 (271)
- Team of Rivals: The Political Genius of Abraham LincolnD'EverandTeam of Rivals: The Political Genius of Abraham LincolnÉvaluation : 4.5 sur 5 étoiles4.5/5 (234)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceD'EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceÉvaluation : 4 sur 5 étoiles4/5 (895)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureD'EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureÉvaluation : 4.5 sur 5 étoiles4.5/5 (474)
- Blast Injuries & Gunshot WoundsDocument93 pagesBlast Injuries & Gunshot WoundsdocpreetiPas encore d'évaluation
- On Fire: The (Burning) Case for a Green New DealD'EverandOn Fire: The (Burning) Case for a Green New DealÉvaluation : 4 sur 5 étoiles4/5 (74)
- The Yellow House: A Memoir (2019 National Book Award Winner)D'EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Évaluation : 4 sur 5 étoiles4/5 (98)
- The Unwinding: An Inner History of the New AmericaD'EverandThe Unwinding: An Inner History of the New AmericaÉvaluation : 4 sur 5 étoiles4/5 (45)
- NAVLE Study Strategies Zuku ReviewDocument60 pagesNAVLE Study Strategies Zuku ReviewMohamed Omar90% (10)
- The Diet Solution Metabolic Typing TestDocument10 pagesThe Diet Solution Metabolic Typing TestkarnizsdjuroPas encore d'évaluation
- Avian Anatomy 1Document50 pagesAvian Anatomy 1Le KhaiPas encore d'évaluation
- Using Master Tung's Gallbladder Points For Diseases of The Head and NeckDocument2 pagesUsing Master Tung's Gallbladder Points For Diseases of The Head and NeckTrần Hồ Thạnh Phú100% (1)
- Refractory MigraineDocument495 pagesRefractory MigraineSuresh Srinivas100% (1)
- Mentz1993 Lipomarcacion PDFDocument4 pagesMentz1993 Lipomarcacion PDFreylaberintoPas encore d'évaluation
- General Principles: Thoracotomy Performed ToDocument4 pagesGeneral Principles: Thoracotomy Performed ToreylaberintoPas encore d'évaluation
- Complicaciones Blefaro EsteticaDocument15 pagesComplicaciones Blefaro EsteticareylaberintoPas encore d'évaluation
- A Classification and Algorithm For Treatment of Breast PtosisDocument9 pagesA Classification and Algorithm For Treatment of Breast PtosisreylaberintoPas encore d'évaluation
- Treatment of Early Childhood Caries A Case Report 2 1Document6 pagesTreatment of Early Childhood Caries A Case Report 2 1SuciPas encore d'évaluation
- Ventilation: Kinematics and Kinetics.: Thorax Structure and FunctionDocument52 pagesVentilation: Kinematics and Kinetics.: Thorax Structure and FunctionAlejandra RomeroPas encore d'évaluation
- Stroke Signs and Symptoms - CDC - GovDocument2 pagesStroke Signs and Symptoms - CDC - Govjeanne_mbPas encore d'évaluation
- Portal Vein Thrombosis, Risk Factors, Clinical Presentation, and TreatmentDocument6 pagesPortal Vein Thrombosis, Risk Factors, Clinical Presentation, and TreatmentAdiPas encore d'évaluation
- Urinary System and Disorders IntroductionDocument23 pagesUrinary System and Disorders IntroductionHananya ManroePas encore d'évaluation
- Objectives: Terms of Use Privacy Policy Notice AccessibilityDocument16 pagesObjectives: Terms of Use Privacy Policy Notice AccessibilityJuan Sebas OspinaPas encore d'évaluation
- RITM LeprosyDocument3 pagesRITM LeprosyDanielle Vince CapunoPas encore d'évaluation
- Clinical Presentation of Abdominal TuberculosisDocument4 pagesClinical Presentation of Abdominal TuberculosisRizky AmaliahPas encore d'évaluation
- The Chemical Composition and Pharmaceutical Effect of Celosia Cristata A Review On Nutritional AspectDocument6 pagesThe Chemical Composition and Pharmaceutical Effect of Celosia Cristata A Review On Nutritional AspectInternational Journal of Innovative Science and Research TechnologyPas encore d'évaluation
- Journal Neuropediatri PDFDocument8 pagesJournal Neuropediatri PDFHalimah PramudiyantiPas encore d'évaluation
- Fisiologi Hati Dan Kandung EmpeduDocument24 pagesFisiologi Hati Dan Kandung EmpeduMusmul AlqorubPas encore d'évaluation
- Situation Analysis of Children in Timor-LesteDocument194 pagesSituation Analysis of Children in Timor-LesteBunga P.Pas encore d'évaluation
- ToradolDocument2 pagesToradolAdrianne Bazo100% (1)
- 27 Auramine Staining FinDocument11 pages27 Auramine Staining FinRahmat Sayyid ZharfanPas encore d'évaluation
- Complete Cardiology Revision Part 3 - B107b8e3 0692 4e9c 80a0 90c4dbd98754Document59 pagesComplete Cardiology Revision Part 3 - B107b8e3 0692 4e9c 80a0 90c4dbd98754KumarPas encore d'évaluation
- DEV2011 2018 Practical Week 8 DRAFT REPORT PDFDocument1 pageDEV2011 2018 Practical Week 8 DRAFT REPORT PDFAreesha FatimaPas encore d'évaluation
- Cuscuta AssignmentDocument12 pagesCuscuta AssignmentAshfaq Hussain KharalPas encore d'évaluation
- Halosil Hospitals Sell Sheet 060817Document2 pagesHalosil Hospitals Sell Sheet 060817duna tarimaPas encore d'évaluation
- SIgE Conjugate 02.17Document4 pagesSIgE Conjugate 02.17Clodagh WhelanPas encore d'évaluation
- Job Description Occupational Health and Safety SpecialistsDocument3 pagesJob Description Occupational Health and Safety SpecialistsMala MinniePas encore d'évaluation
- Newborn Buried Alive:: Transgender'S RevengeDocument16 pagesNewborn Buried Alive:: Transgender'S RevengeAbhishekh GuptaPas encore d'évaluation
- Artificial IntelligenceDocument27 pagesArtificial IntelligenceMd HassanPas encore d'évaluation
- Aids ProjectDocument7 pagesAids Projectapi-270625016Pas encore d'évaluation
- Top 10 Differential Diagnoses in Family Medicine - CoughDocument2 pagesTop 10 Differential Diagnoses in Family Medicine - CoughTiza OyonPas encore d'évaluation