Académique Documents
Professionnel Documents
Culture Documents
Unit 6A
Transféré par
Melanie MaloneyDescription originale:
Copyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
Unit 6A
Transféré par
Melanie MaloneyDroits d'auteur :
Formats disponibles
Unit 6A Ch. 39 P.
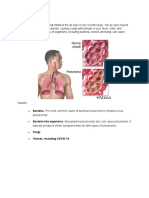
1321 Notes Lower respiratory system function depends on several organ systems: CNS-stimulates and controls breathing Chemoreceptors in brain, aortic arch, carotid bodies which monitor pH and oxygen content of blood. Heart and circulatory system- provide blood supply and gas exchange. Musculoskeletal system- provides intact thorasic cavity capable of expanding and contracting Lungs and bronchial tree- allow air movement and gas exchange. Impaired functioning of any of these systmes effects ventilation and respiration. Tissues become hypoxic with inadequate oxygen to support metabolic activity. Reactive Airway Disease: Asthma and obstructive disorders, air trapping reduces the amount of oxygen available to drive gas exchange. Interstitial Lung Disorders: Affect the ability of the lungs to expand and the work of breathing, again reducing aveolar oxygenation and gas exchange. Pulmonary Vascular Disorders: Affect blood flow to the lungs or a portion of the lungs, reducing gas exchange through their effects on perfusion of the lungs. Respiratory Failure: Is the ultimate consequence of impaired gas exchange. The lungs cannot adequately oxygenate the blood or eliminate carbon dioxide. Neurologic Disorders (head injury, spinal cord trauma or disorders, amyotrophic lateral sclerosis, myasthenia gravis) also can effect gas exchange through their effects on the central or peripheral nervous systems. Aging effects pulmonary ventilation and gas exchange. Number of alveoli decrease, and emphysematious changes (senile emphysema) reduces the surface area for gas excahnge. Alveoli become less elastic, causing increasing air trapping and dead space. For acitve older adults these changes have minimal effects. For those with lung disease age related pulmonary changes increase risk for developing respiratory failure. Reactive Airway Disorders Airways narrow in response to stimulus. Narrowing limits airflow to both into and out of the alveoli. This will increase workload of breathing. And the residual volume of lungs because air is trapped behind narrow airways. Inspired air mixes with abnormally large volume of resudual air, reducing the amount of oxygen available in the alveoli. Decreased aveolar ventilation further reduces oxygen available for exchange. Asthma: Chronic inflammatory disorder of the airways characterized by recurrent episodes of wheezing, breathlessness, chest tightness and coughing. Inflammation causes increased responsiveness of the airways to multiple stimuli. Widespread airflow obstruction. Allergies play strong role in childhood asthma, strong genetic component, environmental factors ; air pollution, occupational hazzards. Respiratoyr viruses rhinovirus and influenza can precipitate asthma attacks. Exercise particularly in cold air and emotional stress. Physiology Review Parasympathetic (cholinergic) stimulation leads to bronchoconstriction, or narrowing of the airways. Sympathetic stimulation through B2 adrenergic receptors causes bronchodilation or expansion of the airways. Slight bronchoconstriction normally predominates. However, when increased airflow is necessary (exercise) the parasympathetic system in inhibited and stimulation of the sympathetic systems causes bronchodilation. Inflammatory mediators (such as histamines) released during an antigen antibody response act directly on bronchial smooth muscle to produce bronchoconstriction. In Asthma the airway is in a persistent state of inflammation. Even when quiet inflammatory cells such as eosinophils , neutrophils, and lymphocytes may be found in airway tissues and edema my be present.
Attack Triggers: inhalation of allergens such as pollen, animal dander, household dust, tobacco, irritant gases ( sulfer dioxide, nitrogen dioxide and ozone) second hand smoke, chemicals. Viral respiratory infections are common internal stimulus for asthma attacks. Asprin, and other nonsteroidal antiinflamatory drugs. Sulfites (in wine, beer, fresh fruit and salads) and beta-blockers. As a result hypoxemia develops. Hypoxemia and increase lung volume due to tapping stimulat the respiratory rate. Hyperventilation causes the Paco2 to fall, leading to respiratory alkalosis. Summary: In an acute attack, inflammatory mediators are released from sensitized airways followed by activation of inflammatory cells. These events lead to bronchoconstriction, airway edema, and impaired mucociliary clearance. Airway narrowing limits airflow and increases the work of breathing; trapped air mixes with inhaled air , impairing gas exchange. Manifestations chest tightness Cough dyspnea wheezing tachypnea and tachycardia anxiety and apprehension
Vous aimerez peut-être aussi
- Shoe Dog: A Memoir by the Creator of NikeD'EverandShoe Dog: A Memoir by the Creator of NikeÉvaluation : 4.5 sur 5 étoiles4.5/5 (537)
- Never Split the Difference: Negotiating As If Your Life Depended On ItD'EverandNever Split the Difference: Negotiating As If Your Life Depended On ItÉvaluation : 4.5 sur 5 étoiles4.5/5 (838)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureD'EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureÉvaluation : 4.5 sur 5 étoiles4.5/5 (474)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeD'EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeÉvaluation : 4 sur 5 étoiles4/5 (5782)
- Grit: The Power of Passion and PerseveranceD'EverandGrit: The Power of Passion and PerseveranceÉvaluation : 4 sur 5 étoiles4/5 (587)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceD'EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceÉvaluation : 4 sur 5 étoiles4/5 (890)
- The Yellow House: A Memoir (2019 National Book Award Winner)D'EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Évaluation : 4 sur 5 étoiles4/5 (98)
- On Fire: The (Burning) Case for a Green New DealD'EverandOn Fire: The (Burning) Case for a Green New DealÉvaluation : 4 sur 5 étoiles4/5 (72)
- The Little Book of Hygge: Danish Secrets to Happy LivingD'EverandThe Little Book of Hygge: Danish Secrets to Happy LivingÉvaluation : 3.5 sur 5 étoiles3.5/5 (399)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryD'EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryÉvaluation : 3.5 sur 5 étoiles3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnD'EverandTeam of Rivals: The Political Genius of Abraham LincolnÉvaluation : 4.5 sur 5 étoiles4.5/5 (234)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaD'EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaÉvaluation : 4.5 sur 5 étoiles4.5/5 (265)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersD'EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersÉvaluation : 4.5 sur 5 étoiles4.5/5 (344)
- The Emperor of All Maladies: A Biography of CancerD'EverandThe Emperor of All Maladies: A Biography of CancerÉvaluation : 4.5 sur 5 étoiles4.5/5 (271)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyD'EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyÉvaluation : 3.5 sur 5 étoiles3.5/5 (2219)
- The Unwinding: An Inner History of the New AmericaD'EverandThe Unwinding: An Inner History of the New AmericaÉvaluation : 4 sur 5 étoiles4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreD'EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreÉvaluation : 4 sur 5 étoiles4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)D'EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Évaluation : 4.5 sur 5 étoiles4.5/5 (119)
- Her Body and Other Parties: StoriesD'EverandHer Body and Other Parties: StoriesÉvaluation : 4 sur 5 étoiles4/5 (821)
- Manajemen Trauma ThoraksDocument62 pagesManajemen Trauma ThoraksqweqweqwPas encore d'évaluation
- Vent Web HandoutDocument41 pagesVent Web Handoutwaqas_xsPas encore d'évaluation
- Chronic Obstructive Pulmonary Disease: Olivia Faye J Listanco IM Resident January 21, 2016Document52 pagesChronic Obstructive Pulmonary Disease: Olivia Faye J Listanco IM Resident January 21, 2016FayeListancoPas encore d'évaluation
- Respiratory Distress in ChildrenDocument16 pagesRespiratory Distress in ChildrenNanda WibowoPas encore d'évaluation
- Competency Appraisal II Respiratory ExamDocument5 pagesCompetency Appraisal II Respiratory ExampauchanmnlPas encore d'évaluation
- Volume Controlled VentilationDocument7 pagesVolume Controlled VentilationVijay GadagiPas encore d'évaluation
- Deresuscitation ARDSDocument28 pagesDeresuscitation ARDSSudaryadiPas encore d'évaluation
- Pulmonary Function TestDocument39 pagesPulmonary Function TestLuqman AlwiPas encore d'évaluation
- MS-SL Prelims FirstsemDocument17 pagesMS-SL Prelims Firstsemmcdonald 1234Pas encore d'évaluation
- Chapter 66 1Document20 pagesChapter 66 1isapatrick8126Pas encore d'évaluation
- Interstitial Lung Disease GuideDocument40 pagesInterstitial Lung Disease GuideMalueth AnguiPas encore d'évaluation
- Basics Mechanical VentilationDocument51 pagesBasics Mechanical VentilationademPas encore d'évaluation
- Bacteria. The Most Common Cause of Bacterial Pneumonia Is StreptococcusDocument4 pagesBacteria. The Most Common Cause of Bacterial Pneumonia Is StreptococcusLouise OpinaPas encore d'évaluation
- Daftar Pustaka-Wps OfficeDocument2 pagesDaftar Pustaka-Wps OfficeRezha July prakosoPas encore d'évaluation
- Mechanical Ventilation Troubleshooting Skill Respiratory Therapy COVID 19 Toolkit - 070420Document8 pagesMechanical Ventilation Troubleshooting Skill Respiratory Therapy COVID 19 Toolkit - 070420Sirgut TesfayePas encore d'évaluation
- NV8 BrochureDocument2 pagesNV8 BrochureJhon DaltonPas encore d'évaluation
- Pts PTR Rev 4.1.21Document4 pagesPts PTR Rev 4.1.21M JainPas encore d'évaluation
- Asthma COPD Overlap Syndrome - ACOSDocument59 pagesAsthma COPD Overlap Syndrome - ACOSdrmaqsoodaliPas encore d'évaluation
- Chest CT Signs in Pulmonary Disease PDFDocument19 pagesChest CT Signs in Pulmonary Disease PDFpvs5155Pas encore d'évaluation
- Nursing Care Plan: Interaction Immediate Cause Goal: Effectivenes SDocument6 pagesNursing Care Plan: Interaction Immediate Cause Goal: Effectivenes SCatherine Kaye Marquez RoxasPas encore d'évaluation
- Case Study 1 COPDDocument5 pagesCase Study 1 COPDRenee RoSePas encore d'évaluation
- Pneumothorax, Bullae, BlebsDocument45 pagesPneumothorax, Bullae, Blebsrobel derejePas encore d'évaluation
- Drugs Acting On Respiratory SystemDocument3 pagesDrugs Acting On Respiratory SystemAlyssa Audrey CaoagasPas encore d'évaluation
- Autopeep Paul Pepe Jhon MariniDocument5 pagesAutopeep Paul Pepe Jhon MariniRenatoPas encore d'évaluation
- Pulmonary Medicine 1Document28 pagesPulmonary Medicine 1Gloria JaisonPas encore d'évaluation
- FDA Approved ListDocument25 pagesFDA Approved ListAli UnitedHospitalPas encore d'évaluation
- Chapter 01Document7 pagesChapter 01Robert Kerwick100% (5)
- AntitussivesDocument3 pagesAntitussivesChristineDeniseBernardoPas encore d'évaluation
- Vyntus-Family BR EN PDFDocument7 pagesVyntus-Family BR EN PDFLajoskaPas encore d'évaluation
- Physiology of Mechanical VentilationDocument12 pagesPhysiology of Mechanical VentilationCarlos ZepedaPas encore d'évaluation