Académique Documents
Professionnel Documents
Culture Documents
Ecg 11
Transféré par
drmanoj7882Description originale:
Titre original
Copyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
Ecg 11
Transféré par
drmanoj7882Droits d'auteur :
Formats disponibles
Welcome About Contact Us Disclaimer Store
BODY SYSTEMS HISTORY TAKING OSCE CLINICAL CASES PHARMACOLOGY QUIZ
ADDED OCT 12, 2010, UNDER: CARDIOLOGY
What is Atrial Fibrillation?
Atrial Fibrillation (AF) is the most common cardiac arrythmia and involves the upper two chambers of the hear (atria). In AF the normal electrical impulses of the sino-atrial node are overwhelmed by disorganised impulses arising in the atria or pulmonary veins. This disorganised electrical activity causes uncoordinated contraction of the atria which results in the atria no longer functioning as an effective pump & instead just quivering Some of the impulses from the atria sporadicallty pass through the atrio-ventricular node and result in irregular contraction of the ventricles. Because the atria are no longer effectively pumping, there is an increased risk of developing a thrombus within the atria, which can then pass out of the heart and cause a stroke. As a result atrial fibrillation is a serious medical condition that should treated to prevent serious harm or death of a patient.
Causes
Hypertension Primary Heart Disease coronary artery disease, valve defects, hypertrophic cardiomyopathy Myocardial Infarction Pneumonia Excessive alcohol consumption Hyperthyroidism Carbon Monoxide Poisoning Family History
Signs& Symptoms
Signs
Tachycardia Irregularly Irregular Pulse
Symptoms
Palpitations Syncope Feeling faint SOB Chest Pain Older patients with chronic AF are often asymptomatic
Investigations
Thorough History - onset, duration, associated symptoms Cardiovascular Examination ECG Echocardiogram look for left atrial enlargement & strucural abnormalities Bloods - electrolyte disturbance, renal function, thyroid function (thyrotoxicosis), FBC (anaemia)
Diagnosis
ECG - absent P waves, irregular QRS complexes
Management
Acute Atrial Fibrillation
Treat associated illness Control ventricular rate Verapamil (1st line in acute) Start Anticoagulation Heparin 5000-10,000 units IV . Cardioversion
Chemical Cardioversion Flecainide Electro-Cardioversion Patient must be anti-coagulated if within 48hrs of onset of AF
Chronic Atrial Fibrillation
Rate control Beta-Blocker - Atenolol Ca+ channel blocker Verampimil Cardiac Glycoside Amiodarone Rhythm Control Chemical Cardioversion - Amiodarone Electrical Cardioversion not usually useful in chronic AF as relapse
. Anticoagulation Warfarin
Aim to keep INR between 2-3 Use of warfarin depends upon CHADS score Chads score of >2 means start warfarin unless contraindicated Reduces absolute risk of stroke (1-12%) by 64% Requires regular monitoring & strict control - unpredictable Increased chance of bleeding over aspirin (1.8% vs 0.8%) Not safe in those at risk of falls Good patient education is essential
. Aspirin Chads score of <2 Reduces absolute risk of stroke by 22% No regular monitoring required as predictable Very small chance of bleeding (0.8%)
Prognosis
Double the mortality of those without atrial fibrillation 4 to 5 fold higher risk of stroke than those without fibrillation. Prognosis depends on the patients underlying medical condition. Any atrial arrhythmia can cause a tachycardia-induced cardiomyopathy
Vous aimerez peut-être aussi
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryD'EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryÉvaluation : 3.5 sur 5 étoiles3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)D'EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Évaluation : 4.5 sur 5 étoiles4.5/5 (121)
- Grit: The Power of Passion and PerseveranceD'EverandGrit: The Power of Passion and PerseveranceÉvaluation : 4 sur 5 étoiles4/5 (588)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaD'EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaÉvaluation : 4.5 sur 5 étoiles4.5/5 (266)
- The Little Book of Hygge: Danish Secrets to Happy LivingD'EverandThe Little Book of Hygge: Danish Secrets to Happy LivingÉvaluation : 3.5 sur 5 étoiles3.5/5 (399)
- Never Split the Difference: Negotiating As If Your Life Depended On ItD'EverandNever Split the Difference: Negotiating As If Your Life Depended On ItÉvaluation : 4.5 sur 5 étoiles4.5/5 (838)
- Shoe Dog: A Memoir by the Creator of NikeD'EverandShoe Dog: A Memoir by the Creator of NikeÉvaluation : 4.5 sur 5 étoiles4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerD'EverandThe Emperor of All Maladies: A Biography of CancerÉvaluation : 4.5 sur 5 étoiles4.5/5 (271)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeD'EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeÉvaluation : 4 sur 5 étoiles4/5 (5794)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyD'EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyÉvaluation : 3.5 sur 5 étoiles3.5/5 (2259)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersD'EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersÉvaluation : 4.5 sur 5 étoiles4.5/5 (344)
- Team of Rivals: The Political Genius of Abraham LincolnD'EverandTeam of Rivals: The Political Genius of Abraham LincolnÉvaluation : 4.5 sur 5 étoiles4.5/5 (234)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreD'EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreÉvaluation : 4 sur 5 étoiles4/5 (1090)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceD'EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceÉvaluation : 4 sur 5 étoiles4/5 (895)
- Her Body and Other Parties: StoriesD'EverandHer Body and Other Parties: StoriesÉvaluation : 4 sur 5 étoiles4/5 (821)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureD'EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureÉvaluation : 4.5 sur 5 étoiles4.5/5 (474)
- The Unwinding: An Inner History of the New AmericaD'EverandThe Unwinding: An Inner History of the New AmericaÉvaluation : 4 sur 5 étoiles4/5 (45)
- EKG Interpretation NursingDocument14 pagesEKG Interpretation NursingTanya ViarsPas encore d'évaluation
- The Yellow House: A Memoir (2019 National Book Award Winner)D'EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Évaluation : 4 sur 5 étoiles4/5 (98)
- On Fire: The (Burning) Case for a Green New DealD'EverandOn Fire: The (Burning) Case for a Green New DealÉvaluation : 4 sur 5 étoiles4/5 (73)
- 14 Clauss Pediatric Echocardiography PDFDocument159 pages14 Clauss Pediatric Echocardiography PDFSergiu NiculitaPas encore d'évaluation
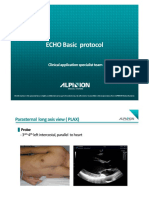
- Echo Basic Protocol (ENG)Document15 pagesEcho Basic Protocol (ENG)stoicea_katalinPas encore d'évaluation
- Samson Notes 2014Document345 pagesSamson Notes 2014Hamza Ahmed100% (1)
- Approach Cyanosis FinalDocument31 pagesApproach Cyanosis Finalsuheena.CPas encore d'évaluation
- Fphys 07 00653 PDFDocument10 pagesFphys 07 00653 PDFvirnaPas encore d'évaluation
- Arrhythmia (Irregular Heartbeats) Symptoms, Types, and TreatmentDocument5 pagesArrhythmia (Irregular Heartbeats) Symptoms, Types, and TreatmentCyberMeow100% (1)
- Cardio PDFDocument94 pagesCardio PDFSalwaPas encore d'évaluation
- Sudden Cardiac Death IRELANDDocument8 pagesSudden Cardiac Death IRELANDDusan OrescaninPas encore d'évaluation
- EkgppDocument93 pagesEkgppLindsay WishmierPas encore d'évaluation
- Stress-Induced (Takotsubo) CardiomyopathyDocument13 pagesStress-Induced (Takotsubo) CardiomyopathyAdrian GeambasuPas encore d'évaluation
- BIOLOGY INVESTIGATORY PROJECT - Cardiovascular Diseases - Coronary Artery Disease PDFDocument50 pagesBIOLOGY INVESTIGATORY PROJECT - Cardiovascular Diseases - Coronary Artery Disease PDFlskumar100% (1)
- Cor Pulmonale: Peter Celec P Ete Rcelec at GM Ail. Com W W W. Imbm. SKDocument108 pagesCor Pulmonale: Peter Celec P Ete Rcelec at GM Ail. Com W W W. Imbm. SKAppry M SilabanPas encore d'évaluation
- Erythema Marginatum Chorea: Migratory Polyarthritis Cardiac Involvement Subcutaneous NodulesDocument27 pagesErythema Marginatum Chorea: Migratory Polyarthritis Cardiac Involvement Subcutaneous NodulesMisbah KaleemPas encore d'évaluation
- C. Miller Fisher: Stroke in The 20th Century: Louis R. CaplanDocument2 pagesC. Miller Fisher: Stroke in The 20th Century: Louis R. CaplanBetro SetopPas encore d'évaluation
- Congestive Heart Failure: Mulualem W.MD Dmu, Department of Internal Medicine For Ho StudentsDocument27 pagesCongestive Heart Failure: Mulualem W.MD Dmu, Department of Internal Medicine For Ho Studentsmuluneh birhanePas encore d'évaluation
- Ashp - Midyear PosterDocument1 pageAshp - Midyear Posterapi-611918048Pas encore d'évaluation
- Test About Circulatory SystemDocument5 pagesTest About Circulatory SystemThảo VânPas encore d'évaluation
- Cardiac MonitorDocument3 pagesCardiac MonitorShameera M. KamlianPas encore d'évaluation
- NSG 6001 Final Exam 1 - Question and AnswersDocument49 pagesNSG 6001 Final Exam 1 - Question and AnswersDAVIDPas encore d'évaluation
- BCU 2022 First Announcement RevDocument14 pagesBCU 2022 First Announcement RevAnggar KingStyle100% (1)
- Cardio Nancy Test BankDocument36 pagesCardio Nancy Test BankNoavilPas encore d'évaluation
- SOMBILLO Scenario 1 ANGINADocument2 pagesSOMBILLO Scenario 1 ANGINAKarla SombilloPas encore d'évaluation
- Classification of Congenital Heart DiseaseDocument1 pageClassification of Congenital Heart DiseaseClaudia SanchezPas encore d'évaluation
- Mrcp-PACES 2023 - Sequence - CVSDocument2 pagesMrcp-PACES 2023 - Sequence - CVSvaranasidineshPas encore d'évaluation
- Syncope 12Document19 pagesSyncope 12miss ramaPas encore d'évaluation
- Hypertrophic Cardiomyopathy: One in Every 500 PeopleDocument12 pagesHypertrophic Cardiomyopathy: One in Every 500 PeoplevishwanathPas encore d'évaluation
- Crochetage' Sign On ECG in Secundum ASDDocument2 pagesCrochetage' Sign On ECG in Secundum ASDAishah Shalimar PutriPas encore d'évaluation
- Alcapa FinalDocument22 pagesAlcapa FinalCardiacCareCenterMCHPas encore d'évaluation