Académique Documents
Professionnel Documents
Culture Documents
GK QA Procedures
Transféré par
Jared MehargDescription originale:
Copyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
GK QA Procedures
Transféré par
Jared MehargDroits d'auteur :
Formats disponibles
PCMH Gamma Knife Center
Physics Quality Control
PROCEDURES
Prepared by H Mota, PhD Updated by C Sibata, PhD
Greenville NC July 2009
DOCUMENT CONTROL TABLE Document Name Program First Version Update #1 Update #2 Update #3 Update #4 Update #5 Update #6 Update #7 Distribution Copies Prepared by Approved by Physics Quality Control: PROCEDURES PCMH Gamma Knife QA 1.0 1.0 - A 1.0-A 1.0 B 1.0 B 1.0 B 1.0 B1 1.0 C RSO RadOnc/Phys Helvecio Mota, PhD Claudio Sibata, PhD 09/30/2005 12/27/2005 11/2006 05/24/2007 12/2007 1/2009 3/2009 07/01/2009 GKC Claudio Sibata, PhD
11/2006 12/2007 01/2009 03/2009 7/1/2009 9/19/2009
no changes Claudio Sibata, PhD no changes Claudio Sibata, PhD no changes Claudio Sibata, PhD treatment variance report updated Claudio Sibata, PhD New Policy for calibration of instruments, TPS QA and GK Patients Plans Backup Claudio Sibata, PhD Policy for LGP Treatment Planning System QA updated Claudio Sibata, PhD
PCMH Gamma Knife Center
Greenville NC
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
Table of Contents
INTRODUCTION 6
SAFETY CHECKS ......................................................................................................................................6 DOSIMETRY CHECKS ...............................................................................................................................7 MATERIAL 9
THE SPHERICAL PHANTOM .....................................................................................................................9 THE FILM HOLDER .................................................................................................................................9 THE ION CHAMBER SYSTEM ..................................................................................................................10 THE RADIATION SURVEY METER ............................................................................................................11 HELMET TEST BOX................................................................................................................................12 OTHER MATERIALS ................................................................................................................................12 SAFETY CHECKS 13
SURVEY METER ....................................................................................................................................13 CONTROL ROOM ...................................................................................................................................13 POWER ON............................................................................................................................................13 INTERCOM AND CAMERA FUNCTIONAL CHECK ....................................................................................13 ALARM TEST.........................................................................................................................................14 EMERGENCY STOP BUTTONS.................................................................................................................15 TREATMENT ROOM ...............................................................................................................................15 EMERGENCY TOOLS ..............................................................................................................................16 COUCH RELEASE HANDLE ....................................................................................................................16 MATTRESS LOCK AND HEIGHT ADJUSTMENT........................................................................................17 POSTING ................................................................................................................................................17 SENSORS OF MOUNTED PATIENT SIDE PROTECTION, HELMET AND ID .................................................18 TEST RUN AND CONSOLE INDICATORS ..................................................................................................18 BEAM STATUS INDICATORS ...................................................................................................................19 ROOM DOOR INTERLOCK ......................................................................................................................19 PERMANENTLY MOUNTED RADIATION MONITOR .................................................................................19 REMOTE RADIATION ALARM INDICATOR ..............................................................................................20 TIMER TERMINATION OF EXPOSURE .....................................................................................................20 TREATMENT PAUSE ...............................................................................................................................20 EMERGENCY COUCH OUT .....................................................................................................................21 APS QA TEST .......................................................................................................................................21 HELMET CHANGER................................................................................................................................24 MEDICAL UPS BATTERY CHECK ..........................................................................................................25 HELMETS CAP SENSOR TEST.................................................................................................................26 HELMETS ID TEST.................................................................................................................................26 HELMET MICROSWITCHES TEST............................................................................................................26 HELMET TRUNNIONS (CENTRICITY) ......................................................................................................28 SITE KIT ................................................................................................................................................29 RADIATION SURVEY: WIPE TEST...........................................................................................................29 RADIATION SURVEY: SOURCES HOUSING (LEAKAGE RADIATION)........................................................29 RADIATION SURVEY: RADIATION LEVELS OUTSIDE THE ROOM.............................................................30 TRAINING: GENERAL RADIATION SAFETY ............................................................................................30
Page 4
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
TRAINING: OPERATIONAL INSTRUCTIONS AND EMERGENCY PROCEDURES FOR PATIENT REMOVAL ....30 DOSIMETRY TESTS 31
GENERAL REMARKS 31 BEAM AXES ALIGNMENT ......................................................................................................................31 DOSIMETRY SPECIFICATIONS .................................................................................................................31 LOCATION OF THE UNIT CENTER POINT ................................................................................................31 DOSE CALIBRATION ..............................................................................................................................32 PRECISION IN DOSE DELIVERY .............................................................................................................32 PERFORMING THE TESTS 33 ACCURACY IN DOSE DELIVERY (UCP COINCIDENCE) ...........................................................................33 PRECISION IN DOSE DELIVERY (DOSE PROFILES) ..................................................................................34 MEASUREMENT OF ABSORBED DOSE RATE ..........................................................................................35 DOSE RATE LINEARITY .........................................................................................................................36 LGP 30 GY CALCULATION ....................................................................................................................37 TIMER ACCURACY ................................................................................................................................37 COUCH MOVEMENT TIME .....................................................................................................................37 OUTPUT FACTORS (HELMET FACTORS) ..................................................................................................38 CLEANING 38
OPERATOR CONSOLE ............................................................................................................................39 CAMERA LENS ......................................................................................................................................39 MONITORS ............................................................................................................................................39 GAMMA KNIFE UNIT .............................................................................................................................40 APPENDICES QUALITY CONTROL CHECK LIST DAILY SPOT CHECK FORM MONTHLY SPOT CHECK FORM ANNUAL CHECK LIST FORM RADIATION SURVEY FORM INSTRUMENTS USED FOR GAMMA KNIFE UNIT CALIBRATION LGP TREATMENT PLANNING SYSTEM QA GK PATIENTS PLANS BACKUP LOG BOOK FORMS (EVENT RECORDS) 41 41 43 44 45 46 47 48 49 50
Page 5
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
TREATMENT VARIANCE REPORTS USEFUL PHONES AND CONTACTS CALIBRATION CERTIFICATES GAMMA KNIFE TECHNICAL DATA EXAMPLE FOR MONTHLY QA EXAMPLE FOR ANNUAL QA LOGIN/PASSWORDS
51 52 53 54 56 59 64
1. Introduction
A quality assurance (QA) program for Gamma Knife must include all aspects of the radiosurgery process: visualization and localization of the target, treatment and dose planning and dose delivery. Therefore, the program should routinely inspect the hardware/ software, and all aspects of the planning and treatment process. That shall cover all safety and dosimetry requirements for all exposures in the stereotactic radiosurgery facility. The quality control (QC) tests described in this document are part of the general QA program for the PCMH Gamma Knife Center. All steps to perform the QC tests are given, including material, frequency, and tolerances. Regarding to frequency of tests, the quality control program is divided in daily, monthly, semi-annual and annual spot checks. The list of test included in the Gamma Knife QC program and corresponding frequency and tolerances is presented in Appendix 6.1 In case of any problem or unusual event during treatment, QC or QA surveys, proper action shall be taken. A logbook is maintained in the control room for events related to the accurate functioning of the gamma knife unit. A special logbook is maintained with treatment variances which may be or not medical events as defined in the Quality Management Program (QMP). Copies of these forms are presented in Appendix 6.10.
Safety checks
Before the patient is ready to be treated, each day items such door interlock, timer, audiovisual systems, emergency-off buttons, console indicators, radiation monitors and table and couch movements must be checked for safety purposes. The safety checks verify conformity of the relevant mechanical, electrical and radiological specifications. Care and maintenance items such as console cleaning and visual inspection are also included in these requirements. It also covers surveys of radioactive leakage and scattering radiation levels, and emergency items.
Page 6
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
The engagement of two microswitches located at the base surface of the helmet indicates the proper positioning of the helmet. To test their sensitivity, a special ring that simulates the helmet docking the central body is provided by the manufacturer. According to AAPM, this test should be performed monthly (cf. Stereotactic Radiosurgery. Radiation Therapy Committee Task Group #42, 1995). Trunnion centricity is checked using the trunnion test tool supplied by the manufacturer. The trunnions are responsible for the accurate placement of a target in the X dimension in manual mode. According AAPM, this procedure is performed monthly. The Automatic Positioning System (APS) is preferably used in all treatments for automatic and accurate placement of a target in all three dimensions (X, Y, and Z). The proper functioning of the APS is verified weekly and after each APS/Trunnion exchange, and every time APS is used. Appendix 6.2 presents a picture of the form used on daily/weekly spot checks.
Dosimetry checks
The dosimetry tests are performed to verify the LGK specifications regarding radiation dose delivery. It can be classified in three steps: Geometric accuracy in dose delivery. To verify the location of the mechanical Unit Center Point (UCP) and the radiological isocenter of the treatment unit. Precision in dose delivery (beam alignment). To compare measured and calculated spatial distributions of relative radiation dose within a volume surrounding the UCP; i.e., beam profiles verification. Measurement of Absorbed Dose Rate at the UCP.
Radiation/mechanical isocenter coincidence is checked by irradiation of a film in a specially designed tool. The mechanical/radiation isocenter tool is basically a light-tight aluminum film cassette, containing a small piece of film. At the center of the cassette, a pin is used to pierce a tiny hole on the film which indicates the mechanical isocenter of the machine. Dose profiles are measured using film dosimetry on acceptance and annually, and after source change. The timer constancy, linearity and accuracy are checked over the range of clinical use using an ionization chamber coupled with an electrometer. A spread of the electrometer readings of a constant time setting determines the constancy and reproducibility of the timer and the dosimetric system. The transit "On-Off" error calculation (!) is based on the same method used in a teletherapy machine, where ! = [nR2-R1] / n[R1-R2] (see Chapter 4). The radiation output of the machine is measured using with a NIST-traceable ion chamber placed at the center of an 80 mm radius sphere of tissue equivalent material (polystyrene) which is positioned at the focus of the 18mm collimator. The dose output measured for the gamma knife is referred to the dose to water. The percent discrepancy between the measured output and the anticipated output should be within 3%. This measured dose is stored in the Leksell GammaPlan. Measurements are done with the others helmets to verify the relative helmet factors also referred as output factors. Since ion chamber cannot measure adequately 4 and 8 mm beam, this is verified using diodes or thermoluminescent dosimeters (TLD) or film dosimetry. The procedure is repeated annually.
Page 7
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
Couch movement time is the interval time during which the patient may be exposed to radiation in the case where treatment is interrupted right after it is initiated. When the treatment is interrupted, the couch moves the patient out of the unit, and the shielding door closes completely. The couch travel time is adjusted to the minimum, typically within 30-40 sec. This test is performed monthly. Furthermore, the treatment planning aspects of quality assurance should include the computer output check and decay correction in the Leksell GammaPlan. This procedure is performed monthly.
Page 8
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
2. Material
The following material/devices are necessary to carry out the Gamma Knife QC tests: Spherical Phantom, with different cassettes for film, ion chamber, diode and TLD measurements Film Holder, specially designed by Elekta to verify the geometric accuracy Films (radiochromic and/or Kodak EDR2) Film scanner Densitometer (optional) Ion chamber system calibrated for TG21 protocol (and long low noise coaxial cable) Thermometer Barometer Timer or chronometer Radiation survey meter (large volume or pressurized ionization chamber) Thermo luminescent detectors (TLD) and reader (optional) Diode or similar detectors (optional) and corresponding electrometer Adjustment Ring and Allen key Helmet test box Helmet trunnions test tool APS test tool 0.1 mm shims (4 pieces) QA forms (and MS Excel spreadsheet and computer) Pencil (white) to mark film orientation Lab scintillation detector (to measure low radioactivity samples)
The Spherical Phantom
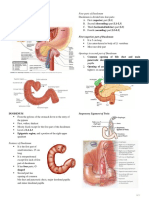
The shape and size of the dosimetry phantom for Gamma Knife simulates the head of an adult patient. It is a solid plastic sphere of 16 cm diameter made of polystyrene. According to Elekta, the absorbed dose measured at the center of the phantom is underestimated by approximately 1% as compared to water. The phantom is divided into two hemi-spheres between which a cassette can be inserted. The hemi-spheres and the cassette are held together by four plastic holders (See next Fig). Two of these holders are provided with an axis allowing the phantom to be aligned in the helmet by means of the trunnions. When both trunnions are locked at 100.0, the center of the phantom coincides with the UCP if the helmet is in the treatment position. Depending on how these four pieces are arranged, the phantom can be aligned in two mutually perpendicular orientations. One of different cassettes can be inserted into the sphere. The cassettes allow film dosimetry, diode, TLD and small ionization chamber respectively. The cassettes are 10 mm thick. A hole was especially drilled in one of the rounded corners of the cassette so the measurement point of the chamber coincides with the center of the cassette (phantom). These corners are the only parts of the cassette that are accessible when it is inserted in the spherical phantom. Similar hole was drilled in the diode cassette.
The Film Holder
Page 9
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
This tool is required when the geometrical location of the radiation focus or UCP is to be determined with sufficient accuracy. This cylindrical film [see (5) next Fig] holder is accurately machined and is made of aluminum. The Film Holder contains a small space where a film can be placed and a sharp, springloaded needle. The film holder is aligned and fixed in the 4 mm helmet by means of the trunnions, so that the position of the needle tip exactly coincides with the mechanically defined UCP (both trunnions locked at 100.0). A small piece of film placed in position in the holder is pierced by the needle just prior to exposure. The geometrical relationship between the mechanical defined location of the UCP may thus be compared with the location of the radiologically defined UCP.
Elekta phantom, cassettes, and holders
The ion chamber system
The small volume (0.007 cm3) ion chamber Exradin A16 was selected for the absolute dosimetry. The dosimetry protocol recommended for Gamma Knife is the AAPM-TG21, since the geometry of calibration in the Gamma Knife can not meet the criteria of the AAPM-TG51. The ionization chamber is calibrated in terms of Nk (and Nx). The electrometer is a CMNC model 206. Both ion chamber and electrometer are calibrated at the ADCL of University of Wisconsin (see copy in Appendix 6.12) every two years.
Page 10
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
Characteristics of the Exradin A16 ion chamber
The radiation survey meter
The Victoreen 451P is the preferred survey meter because it is a 300 cm3 pressurized air ionization chamber (8 atmospheres), providing enhanced sensitivity (!R) and improved energy response to measure gamma and x-ray radiation. It is calibrated for 137Cs by the Global Calibration Laboratory - Ohio (see copy in Appendix 6.12) every year.
Page 11
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
Helmet Test Box
The helmet test box allows us to check the operation of the helmet microswitches and the helmet cap sensor and to check the helmet identity by means of three sets of indicators and a table.
(1) (2) (3) (4)
Helmet microswitches check indicators Helmet ID indicators Helmet cap check indicator Helmet ID table
Other materials
The thermometer available in the GK center is the Digital Hart Scientific model 1521. The barometer is the Digital Nova Lynx. The timer is a Digital Cole-Palmer. These are calibrated instruments. Copy of the calibration certicates are attached in Appendix 6.12. The original documents are kept in a designated binder in the console room.
Page 12
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
3. Safety Checks
Survey Meter
Type: visual inspection Periodicity: Every day
The radiation survey meter shall be operational and calibrated, and readily available at the Gamma Knife Center. Backup batteries (2 " 9V) should be kept close to the survey meter.
Control Room
Type: visual inspection Periodicity: Every day
Verify that the control console and the electric cabinet have all parts and no unusual changes have occurred. The Uninterrupted Power Supply (UPS) green light on the cabinet should be on. The Gamma Knife operating procedure should be in the control room.
Power ON
Type: console test Periodicity: Every day
1. Insert the key into the Power keyswitch (1) and turn it to the ON (!) position.
2. Verify that the Control Unit and the Safety System on the electric cabinet is powered (green LED). 3. On the console enter the user/password login as operator (OP/OP).
Intercom and Camera Functional Check
Type: visual inspection Periodicity: Every day
Check the function of the intercom and camera system (1 Elekta and 1 or 2 additional). The patient microphone and room speakers can be checked using the FM stereo.
Page 13
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
The console microphone can be check by knocking on it using a pencil while pushing the TALK button. Note: The Elekta camera image is shown on the Samsung monitor on the left. Push twice the source button to get the audio/video signal from the camera.
Alarm Test
Type: console test Periodicity: Every day
In the control panel initiate the alarm test from the Select TEST FUNCTION dialog; 1 Click the ALARM TEST button.
2 Observe that the following indicators are functioning at the control panel: System Error Alarm Emergency Alarm (including audible alarm). Also, yellow light mounted on the wall should flash. 3 You may press the ALARM MUTE button to check that the audible alarm is silenced. It will resume after two minutes if the test is not terminated within this time. 4 A dialog to confirm operation of the alarms opens. Click YES to confirm correct operation of the alarms. Click NO if the alarms did not function correctly. If you click NO the treatment session terminates. Note: The treatment cannot start until the system has passed the alarm test and the test run. Alarm test can also be used to reset system error in the MCU (Main Control Unit, also known as system computer). Click YES to run the alarm test.
Page 14
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
Emergency Stop Buttons
Type: console test Periodicity: Every day
The emergency stop button is used when there is a risk of injury to patient or operator or risk of damage to the LGK unit due to movement of the couch or shielding doors.
1. Press the EMERGENCY STOP button on the console and observe: The emergency alarm buzzer sounds, the emergency alarm indicators on the control panel and the treatment view monitor flash and the message Emergency Stop Activated is displayed in the system information field. The couch and radiation shielding doors hold their positions until the emergency stop is released. 2. Repeat the procedure with the two EMERGENCY STOP buttons (with identical functionality) located in the treatment room. This test can be performed also by pressing the emergency buttons without any radiation/ treatment sequence. The alarms will sound/flash.
Treatment Room
Type: visual inspection Periodicity: Every day
Verify that the no unusual changes have occurred. Particular attention should be given to the helmets. By sliding the hands over the collimators make sure that there is no misplacing of the collimators. All helmet trolleys should be secured. Check also the storage cabinet to verify that nothing is missing.
Page 15
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
Emergency Tools
Type: visual inspection Periodicity: Every day
Normally, the couch is moved out of the treatment position when the emergency COUCH OUT button is pressed, or can be pulled out manually. If both of these methods fail, the patient can be released by use of the APS/Trunnion Special Release Tool Check that these tools are present, undamaged and easily accessible: Long Allen Key (1) Spade Tool (2) APS Special Release Tool (3) Ratchet Handle (4) (used for manually closing the shielding doors)
Couch Release Handle
Type: mechanical test 1. Pull the couch release handle. Periodicity: Weekly
2. Pull the couch to verify that it is released. 3. Push back the couch release handle into locking position. 4. Pull the couch to verify that it is locked.
Page 16
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
Perform a function check and ensure that the handle is properly pushed back after the test.
Mattress Lock and Height Adjustment
Type: test Periodicity: Every day
1. 2. 3. 4. 5.
Press the MATTRESS LOCK button (1) to lock the sliding mattress. Try to slide the mattress it should not move. Press the MATTRESS UNLOCK button to unlock the sliding mattress. Try to slide the mattress it should now move. Pres (7) UP and DOWN buttons and verify that the mattress height adjustment functions well.
Posting
Type: visual inspection Periodicity: Every day
Check if the NRC/State notice to employees, Safety Instructions and license are post in the operating room. Also check that the two-sided Emergency Procedures placard is displayed in an appropriate place, clearly visible, and free from damage, including the diagram of the high level zone.
Page 17
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
Sensors of Mounted Patient Side Protection, Helmet and ID
Type: test Periodicity: Every day
1. Open the helmet changer cover and press and hold the CARRIER RELEASE button to unlock the helmet carrier and push the helmet carrier a few inches along the telescopic rails; 2. Remove the cap from the rear of the helmet; 3. Remove the side protection from the couch; 4. On the control console try a TIMER RUN for 1 min selecting the correct collimator and pressing the START key. A message should inform that the system is not ready to start. Helmet cap not mounted; Helmet changer not fully out; Patient protection not mounted. 5. Cancel treatment and try another Timer Run selecting a wrong collimator. After clicking OK, a message should inform that a wrong collimator was selected planned/actual. 6. Repeat the step above for the other collimators.
Test Run and Console Indicators
Type: console/system test Periodicity: Every day
The Test Run allows checking that the treatment session will be performed correctly. Note: To perform the Test Run a collimator helmet must be installed on the treatment couch. It may be convenient to mount the helmet which will be used for the first treatment run.
Page 18
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
Initiate the Test Run from the Select Test Function dialog and Click the Test Run button.
The Treatment View dialog opens. You can use it during the Test Run to observe: the target position; the current position; the couch in / couch out indications; the shielding doors open/close indications; and the beam status indicators and the independent radiation monitors (see below). Observe the progress of the test treatment in the Elapsed Time and % of Time fields. Note that 12 seconds (0.20 minute) before the completion of the shot, the attention signal sounds. When the treatment time has elapsed the couch moves fully out of the radiation unit. Note: If the APS is present and activated in the System Configuration, the Test Run will include APS coordinate checks using manual control. The Perform Checks dialog box will open on the monitor. Press the space bar on the keyboard to enlarge the APS View. The coordinates of two runs shall be verified inside the room using the NEXT and CONFIRM buttons.
Beam Status Indicators
Type: visual inspection Periodicity: Every day
Any time while the unit shielding door is open, verify the RADIATION ON box above the room door and the TREATMENT and the radiation symbol at the console are lightened up.
Room Door Interlock
Type: visual inspection Periodicity: Every day
During test runs, verify if treatment stop sequence is initiated when trying to open the room door. The emergency alarms accompanied by a warning buzz are immediately activated. The door interlock can also be checked by trying to start the radiation while the door is open. A message on the monitor will say that the system is not ready to start because the treatment room door is open.
Permanently Mounted Radiation Monitor
Type: visual inspection with beam on Periodicity: Every day
Inside the GK room there is a radiation detector (Geiger) Primalarm (Nuclear Associate) to provide independent continuous monitoring of the condition of RADIATION ON. The red light alarm is activated when the radiation level at detector position reaches 2.5 mR/h. The system is connected to a small UPS battery to allow operation in case of electrical power
Page 19
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
failure in the building. This detector should be readily visible when the operator enters the room. The check consists in verify if the alarm lights when the GK shielding door is opened. The video camera is useful to verify the red light blinking. The battery system should also be verified by unplugging the wall outlet power supply and verifying that the green light stays on.
Remote Radiation Alarm Indicator
Type: visual inspection with beam on Periodicity: Every day
The radiation detector inside the room is connected to a remote indicator in the control room allowing the operator get the radiation alert signal before enter the room. The red light should blink while the GK shielding door remains open.
Timer Termination of Exposure
Type: console/system test Periodicity: Every day
The exposure (helmet docked) will end after the time selected has been elapsed. Confirm that couch starts moving out immediately after this exposure time. Note: The timer accuracy is verified during Monthly Checks.
Treatment Pause
Type: console test Periodicity: Every day
A treatment pause sequence can be initiated at any time and is sometimes initiated automatically by the control system. A treatment pause moves the couch out to the fully withdrawn position and closes the radiation shielding doors. Activate a treatment pause by pressing the PAUSE button on the control panel.
7. Note: If the remaining time of the current step is less than 4 seconds the initiation of pause is delayed the time needed to complete the step. If the treatment pause sequence fails, press the Couch Out button on the control panel.
Page 20
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
Emergency Couch Out
Type: console test Periodicity: Every day
If a treatment pause is activated but fails, the COUCH OUt button is used to move the patient out of the treatment position as quickly as possible. The COUCH OUT button can be used even if the control unit is non-operational but it will not operate if the EMERGENCY STOP is activated. Press and hold the COUCH OUT button until the shielding doors are closed.
The console indicate a SYSTEM ERROR ALARM. Once the cause of the alarm has been cleared, the interlocking can be reset by clicking the appropriate button in the Configuration dialog.
APS QA Test
Type: test Periodicity: Weekly and after each APS/Trunnion exchange. Today if APS is used
This is a functional test of the APS. The readings do not indicate the overall accuracy of the system. Configure APS mode on the System Configuration dialog, selected from the Special Functions dialog.
Wait until all leds are green in the APS module on the Electric Cabinet. Initiate the QA TestRun from the Select Test Function dialog.
Page 21
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
If the test is not performed after APS/Trunnion exchange, the QA-Test dialog will appear before each run.
If you want to continue without performing the test, click YES. If you want to perform the test, or do not want to continue, click NO to return to the Select Activity dialog. The QA test includes two helmet test positions reached by a number of automatic movements of the APS system and a number of manually controlled movements in the vicinity of the helmet scales. Automatic movement can be selected whenever the AUTOMATIC OK is shown in the Treatment View dialog.
To set the movement in automatic mode press the CONFIRM button while keeping the NEXT button pressed on the APS manual control. Be sure that no objects obstruct the movement of the APS. To stop the automatic movement, use the manual control and press one or both safety switches and CANCEL at the same time
Page 22
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
Note: The Enlarged View can be used for the treatment view monitors. Toggle between the Enlarged View and Normal View by use of the Space key
Performing the Test
1. Start the QA Test and select RUN 1=QA-TEST RUN from the Treatment View dialog.
Note: RUN 2=TRANSPORT POS is the APS transport position used for servicing purposes only and to fit the APS units with holder properly into the transport cases. 2. Follow the instructions in the APS status window. Use the manual control and automatic movement to move the APS to the docking position as prompted. 3. Dock the test tool to the APS.
4. Use the manual control to move the QA test tool to the first test position. As the tip of the tool reaches the face of the helmet it should align with the engraved marks on the helmet
Page 23
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
The longer mark is the reference mark and the other marks are 0.5 and 1.0 mm marks. The reading should be 0 0.5 mm. This confirms the operation of the APS in the X and Y axis. The spring loaded tip of the tool is pressed against the face of the helmet. Read the scale on top of the tool. The reading should be 0 0.5 mm. This confirms the operation of the APS in the Z axis. Note: If any reading is outside the range, do not use the APS until it has been inspected by Elekta service representative. 5. Use the manual control to move the QA test tool to the second test position. 6. Confirm the operation of the APS in each axis as described in step 4 above. 7. Use the manual control to move out the QA test tool from the second test position. 8. The APS QA Test is complete when the APS status window indicates movement to the first treatment position. 9. Click CANCEL (on the treatment view monitor) to finish the QA test. You are prompted to accept or reject the test follow the instructions on the screen. 10. Undock the test tool. Note: Park Position. To remove the APS units or before changing helmets a special parking position must be reached with the APS units and the APS Used check box in the Configuration dialog must have been selected. 1 On the Couch/APS Manual Control, press NEXT + CANCEL during 3 seconds. The APS is now ready to move to the predefined parking position. 2 To initiate automatic movement to the parking position press and hold NEXT and then press and hold CONFIRM. You may release the buttons after the APS starts moving. You can stop the automatic movement by pressing CANCEL at anytime. Do not reconfigure or shut off the APS during the automatic movement.
Helmet Changer
Type: test Periodicity: Weekly
Perform a visual check daily and test the function weekly by performing a helmet installation on the helmet support.
Page 24
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
Medical UPS Battery Check
Type: test Battery Type: Dry lead. Expected Battery Life: More than 5 years. The state of the rechargeable batteries in the electrical cabinet shall be tested by the following procedure. The test should only be performed at the end of the working day or if LGK is not scheduled to be used. 1. Insert the key into the Power keyswitch (1) and turn it to the on (!) position. Periodicity: Monthly
2. Open the door of the electrical cabinet. 3. Perform a test run. 4. Switch off the input button (2) of the UPS unit. The indicating lamp (3) goes out.
Page 25
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
The chargers are now turned off and the system is powered from the batteries as indicated by the indicator lamps of the Test Unit section on the UPS. 5. Let the input button be switched off for 20 minutes. The output voltage is measured over that period of time and if it falls below a preset level, a System Error Alarm is generated. 6. If an alarm is generated contact your Elekta service representative to arrange for the batteries to be exchanged. If no alarm is generated, the batteries are in satisfactory condition. 7. After 20 minutes, switch on the input button (2) of the UPS unit. The indicating lamp (3) turns on. If the UPS batteries have been used to power the system during a power failure they should be left to charge for a minimum period of one hour when the power supply is restored before the LGK is used again.
Helmets Cap Sensor Test
Type: test with test box Periodicity: Monthly
1. Connect the test box to the helmet connectors as shown. The check is made with the helmet on the helmet trolley by using the adjustment ring and the helmet test box (5) Helmet cap sensor (6) Adjustment ring (7) Helmet test box (with J1 and J2 connectors)
2. If the helmet cap sensor is working the Helmet cap indicator will illuminate when the helmet cap is mounted. 3. If the indicator illuminates but the sensor had failed to operate, adjust the position of the sensor. 4. If the indicator doesnt illuminate or if the sensor still doesnt operate after adjustment contact Elekta service representative.
Helmets ID Test
Type: test with test box Periodicity: Monthly
1. Check the helmet ID indicated by the Helmet ID indicators against those shown in the table on the helmet test box. 2. If the helmet ID is incorrect or if no indicators illuminate contact Elekta service representative.
Helmet Microswitches Test
Type: test with test box Periodicity: Monthly
Page 26
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
The adjustment of the helmet microswitches must be checked monthly, or if the Treatment Pause (stop sequence) is initiated due to helmet connector problems, or if the system indicates that adjustment is necessary. The check is made with the helmet on the helmet trolley by using the adjustment ring and the test box. 1. Position the ring with the UP notice facing the floor and opposite to the connectors side. (Reference toward the UP position of the helmet when mounted in the couch).
2. Check which of the Helmet in position indicators on the test box are illuminated and take the appropriate action as follows: If one or both red indicators is illuminated, adjust the microswitches. If both green indicators are illuminated, place shims (0.1 mm) at each corner (4 piece in total) between the adjustment ring and the flat surface beside the microswitch. Both red indicators should now be illuminated. If the red indicators dont illuminate, adjust the Microswitches. 3. Using the special key wrench provided, loosen the recessed nut of the microswitch.
4. Use an Allen key to adjust the screw of the microswitch up or down as required. 5. Tighten the recessed nut using the special key wrench.
Page 27
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
6. 7. 8. 9.
Repeat the microswitch check. Make further adjustments as necessary until both microswitches are set correctly. Remove the adjustment ring and disconnect the test box. Perform a test run to verify correct operation of the microswitches.
Helmet Trunnions (centricity)
Type: test Periodicity: Monthly
The helmet trunnions must be checked at monthly intervals while in regular use, at installation and at any time that damage is suspected, for instance if they are dropped or struck. CAUTION Extreme care must be taken whenever handling the trunnions as they may be damaged if dropped or if struck by a hard or heavy object. The helmet trunnion test is performed with the helmet mounted on the helmet supports using the helmet trunnion test tool.
1. If mounted, remove the gamma angle slices from the trunnions. 2. Attach the helmet test tool (1) to the helmet by tightening the four screws on the ends of the test tool arms into the corresponding holes in the helmet. 3. Push the trunnions inwards so that they are brought into contact with the test tool.
4. Secure the trunnions.
Page 28
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
5. Check the X-coordinate against the vernier scale for both trunnions. The readings shall be 100 0.1 mm. 6. Try to rotate the bushings (2). If the bushings can be rotated, the trunnions have passed the test. If the bushings cannot be rotated, stop all further treatment sessions and contact your Elekta service representative. Note: Alternatively, the helmet trunnion test can be performed with the helmet mounted on the helmet changer in its outer position.
Site Kit
Type: Visual Inspection Periodicity: Annually
A Site Kit containing a number of spare parts is included in the delivery of the LGK unit.
Check the contents of the Site Kit and, if needed, order spare parts from your Elekta service representative.
Radiation Survey: Wipe Test
Type: measurement Frequency: Semi-Annual
This test is to exclude radioactive material outside the encapsulation of the sources. Despite the improbability of such leakage, preventive testing is seen as necessary because of the potentially detrimental consequences of cobalt-60 contamination of parts of the LGK. This could lead to the spread of radioactive material to patients, personnel and the public. 1. Wipe the outer surface of each collimator helmet with a small piece of soft tissue moistened with alcohol. 2. Place the tissue in a shielded well counter; sensitive to detect 5 nCi. 3. Monitor the tissue for a specified time (normally 50 s). The measured activity should be less than 5 nCi. Records of the test should be kept and maintained for inspection by the Agency.
Radiation Survey: Sources Housing (Leakage Radiation)
Type: measurement Frequency: Annual and After Changes
Page 29
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
Using a calibrated survey meter (Victoreen 451P) measure the dose rate at several points 1 meter surrounding the gamma knife unit source housing, with the shielding door closed. A special form for this measurement is presented in the Appendix 6.5. The maximum and average radiation levels at 1 meter from the surface of unit housing in the CLOSED position shall not exceed 100 !Sv/h (10 mR/h) and 20 !Sv/h (2 mR/h) respectively.
Radiation Survey: Radiation Levels outside the Room
Type: measurement Frequency: Annual and After Changes
Using a calibrated survey meter (Victoreen 451P) measure the dose rate at several points at 30 cm adjacent to the gamma stereotactic radiosurgery room with the shielding door OPEN. The survey shall be performed with a phantom in the focus beam of radiation. A special form for this measurement is presented in the Appendix 6.5. The radiation levels in restricted areas shall not exceed the occupational limits established by the State Regulatory Agency (15A NCAC 11 .1604). The levels in unrestricted areas shall not exceed the limit to member of the public (15A NCAC 11 .1611).
Training: General Radiation Safety
Type: visual inspection of records Frequency: Annual
The RSO is responsible for providing an annual radiation safety workshop for personnel assigned to Gamma Knife Center including administrators, campus police officers, students and housekeepers.
Training: Operational Instructions and Emergency Procedures for Patient Removal
Type: visual inspection of records Frequency: Annual
Emergency procedures for patient removal shall be practiced at intervals not exceeding 12 month and records of these exercises shall be kept for review by the Agency. During the annual QMP review, verify if the training records at the PCMH Gamma Knife Center are in compliance with this regulatory requirement.
Page 30
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
4. Dosimetry Tests
4.1.General remarks
Beam Axes Alignment
All 201 gamma radiation emitting sources are hemispherically distributed around the patients head when it is in the treatment position. The radiation emitted by the sources is collimated to narrow beams. The axes of all these 201 beams are directed towards a common focus at the center of the treatment unit. A beam axis is defined as the line between the center of a radiation source and a mechanically determined point centered in the treatment unit, the so called Unit Center Point (UCP). The deviations in alignment between the axes, i.e. the smallest distance between the axes alignment is of critical importance as it affects the combined spatial dose distribution from all beams. The tolerance is defined for the most critical situation, which is the 4-mm collimator helmet. The APS and the trunnions of the helmet provide mechanical means to accurately align a predetermined point within the coordinate system of the frame to the UCP. The uncertainty in target alignment to the UCP introduced by the trunnions is of systematic nature. The tolerance (accuracy) of this alignment is specified to be 0.5 mm, including the uncertainty in the experimental method to measure it. This geometrical specification complies well with the accuracy with which a target point can be localized by means of the best presently available imaging techniques.
Dosimetry specifications
At present no national or international specifications exist which deal specifically with the dosimetry in connection with the narrow beams used in radiosurgery. Thus it was practical to apply suitable parts of the dosimetric specifications that already exist for external beam radiotherapy. The International Commission on Radiological Measurements and Units (ICRU) defined and specified the acceptable degree of uncertainty in the determination of the absorbed radiation dose when using photon beams. The maximum acceptable uncertainty in monitor calibration is 3 %. This should also be the aim in radiosurgery. This specification is only required for specified reference conditions. For other situations it may be difficult to reach this goal. The smallest beams do not have lateral electron equilibrium and suitable detectors that provide both the necessary spatial resolution and high dosimetric accuracy are either very hard to come by or simply do not exist. Thus for non-reference conditions, a maximum acceptable uncertainty of 5% should be the aim.
Location of the Unit Center Point
It is imperative to know how accurately the radiation dose is delivered geometrically to a pre-determined point in the stereotactic space. For that purpose the location of the point of dose rate maximum in the non attenuated radiation field (UCP) is compared with the location of the UCP mechanically determined by means of the trunnions. (Leksell Gamma Knife accuracy).
Page 31
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
Two different methods are applied. One is based on film dosimetry and is performed after the unit has been installed in the clinic but prior to the first treatment; that is during the acceptance procedure period. The results of this test should be recorded as a reference for future measurements. The location of the radiation focus is designed to be tide firmly fixed. Thus, once the exact location of the radiation focus is established (Method 1), new measurements can be made at long time intervals or when the radiation sources of the unit have been moved. The Leksell coordinate frame is positioned and immobilized by steel trunnions which are very rigid. Nevertheless, accidental damage to the trunnions may cause geometrical errors in the positioning of the target point to the UCP. A mechanical test of the trunnions is therefore necessary (Method 2) described previously as Trunnions Centricity Check. The Method 1 as described in this section is referred as Accuracy in Dose Delivery. After exposure, the location of a narrow hole pierced through the exposed film, is compared with the location of the center of the density distribution. By combining the results of measurements in three perpendicular directions, the distance between the UCP (mechanically defined) and the target point (radiologically defined) are determined. Within methodological errors this distance defines the accuracy at which a predetermined point can be aligned in the unit. Two films that are rotated 90 around the xaxis are required, i.e. one x-z - film and one x-y - film.
Dose Calibration
Radiophysical characteristics of LGK are pre-stored in LGP in relative terms. This practical solution can be justified by the consistency of these radiophysical characteristics. The only exception is the absolute dose rate of the unplugged 18 mm collimator helmet, as measured at the center of the 16 cm spherical phantom. The dose rate and the date of its measurement are required so that the treatment time, corrected for source decay, can be calculated by LGP for each shot (irradiation). Note: Leksell GammaPlan normally calculates the treatment time at dose maximum. As the point at which the ionization chamber measures the dose rate is the UCP, the dose rate must be calculated at the same location, that is X=Y=Z=100. The dose rate maximum for the 18 mm collimator helmet is approximately located at X=Y=100, Z=97 and is approximately 1.6 % higher than the dose rate at UCP.
Precision in Dose Delivery
The dose distribution at and around the UCP must be investigated. The strength of each radiation source, its exact alignment in relation to the collimator system, the tolerances to which the collimators are manufactured as well as their exact alignment, affect the dose distribution not only in time but also in space. Very high dose gradients exist in the radiation field to be measured. Film dosimetry with radiochromic films is recommended because of good spatial resolution and very low energy dependence. If the dose distribution from one single beam is to be measured in Leksell Gamma Knife, the other 200 beams must be blocked. The transmission through each of the tungsten plugs
Page 32
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
used to blocked beams in Leksell Gamma Knife is only 0.3 to 0.4 % of the open beam. However, the combined dose contribution from the transmission of 200 plugs is more than 50 % of the dose measured at the center of the single beam and must be subtracted from the dose delivered by a single open beam. Therefore, for the purpose of tests in the clinic, only the dose distribution resulting from >50 beams should be measured. The transmission is then <1 % of dose maximum. The beam channels of Leksell Gamma Knife are manufactured to such narrow tolerances that the radiophysical characteristics of all beams of the same helmet size may be considered as identical. It is therefore sufficient to store the characteristics of one single beam of each helmet size as data for the purpose of dose planning. The stored data was measured in an experimental setup, exactly simulating one beam channel of LGK. The experimental data has also been compared with data resulting from Monte Carlo calculations.
4.2.Performing the Tests
Accuracy in Dose Delivery (UCP coincidence)
Type: measurement Required material Film holder and phantom holder (see page 8) Film, type GrafChromicTM film (MD55, EBT or HS) Pencil to mark film orientation Film scanner Frequency: Annual
Procedure 1. 2. 3. 4. 5. 6. 7. Cut two pieces of films 25 mm x 25 mm in size. Carefully mark the orientation of the film plane at the periphery of the film (x-y and x-z). Place the x-y unexposed film in the film holder as marked and lock (tape) its cover. Mount the 4 mm collimator helmet on the Leksell Gamma Knife. Lock one of the trunnions at 100.0 and leave the second trunnion unlocked. Insert the film holder between the trunnions and lock the second trunnion at 100.0. Rotate the film holder so that the film plane is vertically oriented. Prevent the film holder from rotation by locking it. 8. Pierce the film with the needle of the film holder (a clicking sound must be heard). The film (film holder) must from now on remain in the same position, until the film is exposed. 9. Calculate the exposure time required to deliver a dose given in the column 3 of the table in the next section, depending on the film type, to the center of the spherical phantom. 10. Expose the film in the film holder for the time calculated above. 11. Verify that the exposed film contains a narrow hole. 12. Save the exposed film in a paper envelope. 13. Place the x-z film in the film holder. 14. Repeat step 1 through step 12 but with the film plane oriented horizontally. Acceptable Result
Page 33
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
The tolerance for this measurement is specified to be 0.5 mm. In all units tested so far, this distance has been found to be between 0.1 mm and 0.3 mm including experimental errors.
Precision in Dose Delivery (dose profiles)
Type: measurement Required material Spherical phantom with film cassette Film, type GrafChromicTM film (MD55, EBT or HS) Pencil to mark film orientation Film scanner Frequency: Annual
Procedure Eight films are required for the measurements of the dose profiles, two for each collimator helmet. 1. Cut eight pieces of the 2.5"x 2.5" films. Make sure to mark the side and orientation of each piece before cutting. 2. Mark the films indicating the stereotactic axes (x-y and x-z) at the periphery of the film. 3. Tape the film, in the correct orientation, at the inner surface of the film cassette of the special phantom. Use minimal tape to limit the contamination of the cassette walls by glue. 4. Align and lock the phantom with the film cassette in the 4 mm helmet by setting both trunnions at 100.0. Ensure that the film is correctly oriented. 5. Expose the film to a suitable dose depending on the type of film used (e.g. column 5 in the table below). 6. Save the exposed film in an opaque envelope. 7. Repeat step 1 through step 6 with the same collimator helmet but with the new film oriented perpendicularly in relation to the first exposure. 8. Repeat step 1 through step 7 with the remaining three collimator helmets. 9. A number of new films, of the same size or smaller (e.g. 1.5x1.5) as in step 1 above, are required for the film calibration procedure. 10. All exposures for the film calibration are made in the 18 mm helmet and with the film plane oriented vertically (X-Y plane of the frame when the " angle is 90). 11. Expose a number of films to e.g. the following doses:
Film Type used MD55 HS EBT
Dose, in Gy, for film number 1 15 2.5 0.2 2 30 5 0.5 3 45 10 1 4 60 15 1.5 5 90 20 2 6 120 30 3 7 150 35 4
12. Keep one film unexposed to determine the background density. 13. Save the films in an opaque envelope.
Page 34
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
14. Scan the calibration films in the same film orientation as marked in step 1. Save the files to be analyzed using imageJ or equivalent software. 15. Repeat step 14 for the profile films to obtain the reading profiles along the stereotactic main coordinate axes of the frame. 16. Convert the profiles to relative dose profiles and compare with those calculated provided by Elekta (since the LGP does not permit export calculated data). Notes: Avoid exposing the films to unnecessary light since they are sensitive to UV from fluorescent light and sunlight. Remember that films after being exposed goes through the process of post-exposure optical density growth. They should be scanned at the same time, preferably next day. Acceptable Result The experimental and calculated dose distributions normalized to the dose at UCP are compared by determining the distance from the UCP to the 50 % isodose. The measured distance must agree within 1 mm with that of the corresponding calculated profile. The data should be stored as reference for future measurements.
Measurement of Absorbed Dose Rate
Type: measurement Required material Spherical phantom with IC cassette Small sized and calibrated ionization chamber (A16) Electrometer (nC range; CNMC 206) Barometer Thermometer Timer (optional) MonthlyCheck.xls spreadsheet Frequency: Monthly Check
Procedure If the timer of the LGK are used then the measurement must be corrected for the dose received during the movement into the treatment position and out from this position. 1. Connect the ionization camber in the GK Room the electrometer in the Control Room. 2. Turn on the electrometer at least 10 minutes prior starting the measurements. 3. Align the spherical phantom with the IC cassette between the trunnions in the unplugged 18 mm helmet so that the face of the cassette is vertically orientated. Both trunnions must read 100.0 0.1. 4. Insert the chamber. The measuring point of the chamber should now coincide with the UCP; i.e. at X = Y = Z = 100.0 0.2. 5. Initiate a few-minutes Timer Run and expose the chamber to charge the stray capacities of connectors and long cable. 6. Measure the charge during exposure of 1 minute runs. Repeat 3 times and calculate the average (!1). If the measurements are not stable, repeat 10 times. 7. Measure the charge for a 4 min run (R4)
Page 35
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
8. Measure the local pressure (in mBar) and measure the temperature inside the IC cavity on the cassette/phantom (in oC). 9. The transit error # in minutes is given by
10. The corrected reading for 1 min will be given by M= /(1+ #)
11. Make the required corrections for temperature and air pressure:
12. The absorbed dose rate (Gy/min) in water is calculated using the TG-21 protocol: Dwater = 3.749 " M " CTP where 3.749 is the TG21 factor obtained as described in the document Absolute Dosimetry for the PCMH Gamma Knife Center. (note: 3.7799 was obtained on Feb 2005) 13. Use the Excel spreadsheet MonthlyCheck.xls(see Appendix 6.3) to obtain the dose rate and compare todays data with the decayed calibration data. 14. Use LGP to calculate the time for a reference treatment (phantom) of 30 Gy and compare with the decayed calibration data. Notes: The transit time error is a parameter necessary for the QA. However, there are two other ways to measure the dose rate without obtaining the transit time error. 1. Take the readings of two and one minute. The reading rate is obtained by the difference between these two readings. 2. Use an external timer (e.g. timer in the electrometer, if available) and measure the dose integrated in a given time interval after docking the helmet and before undock the helmet. Acceptable Result The constancy with the four 1 min measurement (max/min 1)"100 should be less than 2%. The transit error should be less than 0.05 min. The measured dose rate should not deviate by more than 1 % from LGP. Change the dose rate stored in LGP immediately if the deviation is more than 3 %. Change also if the average deviation of three consecutive measurements is in the range 1 % $ R $ 3 %.
Dose Rate Linearity
Type: measurement Required material As previous test Procedure
Page 36
Frequency: Monthly Check
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
Following the dose rate measurement obtain the IC reading for 10 and 15 minutes runs. Divide the readings by Run Time + !. Using the four corrected reading (1, 4, 10 and 15 min) calculate the linearity index as (max/min 100) "100. Acceptable Result The linearity index should be less than 2%.
LGP 30 Gy Calculation
Type: LGP calculation Required material LGP Procedure Obtain a LGP time for a 30 Gy dose delivered to the Elekta Phantom normalized at the UCP and calculate the dose rate. Calculate the decayed dose rate from the dose rate at the commissioning. Obtain the percent difference. Acceptable Result The percent difference should be less than 2%. Frequency: Monthly Check
Timer Accuracy
Type: measurement Required material Calibrated timer Frequency: Monthly Check
Procedure Following the dose rate measurement for 15 minutes runs, measure the elapsed time the helmet stay docked in the treatment position. Acceptable Result The time should be accurate better than 6 sec in 15 min.
Couch Movement Time
Type: measurement Required material Timer/Chronometer
Page 37
Frequency: Monthly Check
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
Procedure Using PAUSE button interrupt the exposure any time after it is initiated. Using the timer or chronometer measure the .time interval from the interruption until the shielding door is completely closed. Acceptable Result The timer should be within 30 to 40 seconds.
Output Factors (helmet factors)
Type: measurement Required material Diode detector Compatible electrometer Elekta phantom with diode cassette Frequency: Annual Check
Procedure 1. Position the diode cassette in the Elekta Phantom in such way that the diode cavity will be horizontal and left side in the positive quadrant. 2. Measure the reading rates in the same way as the ion chamber for the 4 helmets 3. Calculate the output factors relative to the reading obtained for the 18 mm helmet and compare with the LGP data (0.87, 0.956, 0.984 and 1.000 for 4, 8, 14 and 18mm, respectively). Acceptable Result The factors should not differ more than 2% from LGP data.
5. Cleaning
Some cleaning after inspection should be performed monthly. Before cleaning any part of the system, shut down the electrical power to the system. Turn the Power keyswitch (1) to the off ( ) position.
Page 38
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
Operator Console
Clean the external casing of the control panel, mouse and keyboard with a soft, damp, lintfree cloth.
Camera Lens
Clean the camera lens (Elekta) in accordance with the manufacturers recommendations.
Monitors
Clean the monitors in accordance with the manufacturers recommendations. To maintain the monitors in good condition, clean the exterior at regular intervals with a soft, damp, lint-free cloth.
CAUTION Do not apply a spray cleaner, wax or compressed air directly to the casing of the monitors. Do not apply an alcohol-based cleaner to the monitor casing. Do not use abrasive substances or strong solvents such as thinners or benzine to clean the monitors. To avoid the risk of spillage do not place liquids or solvents on top of, or in close proximity to, the monitors. Failure to observe these precautions may result in damage to the casing and/ or screen of the monitors.
Page 39
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
Gamma Knife Unit
Clean all parts, especially on their upper surfaces, by wiping them with a damp cloth soaked in a mild detergent and then drying thoroughly. After cleaning, lubricate the following parts with the Molycote grease supplied with the unit: the guide rail on the helmet trolley. the bushings at the helmet support for the helmet guide pins.
Page 40
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
6. Appendices
6.1.Quality Control Check List
Page Safety Checks Survey Meter Control Room Power ON Intercom and Cameras Alarm Test Emergency Stop Buttons Treatment Room Emergency Tools Couch Release Handle Mattress Lock and Height Adjustment Posting Mounted Sensors Test Run Beam Status Indicators Room Door Interlock Permanently Mounted Rad.Monitor Remote Radiation Alarm Indicator Timer Termination of Exposure Treatment Pause Emergency Couch Out APS QA Test Helmet Changer Medical UPS Battery Check Helmets Cap Sensor Test Helmets ID test Helmet Microswitches Test Helmet Trunnions (centricity) Site Kit Wipe Test Leakage Radiation Room Shielding Survey Training Records
Dosimetry and Geometry Accuracy Tests
Daily X X X X X X X X
Week
Month
Semi Annual
Annual
Tolerance
Pass / cal Pass Pass Pass Pass Pass Pass Pass
11 11 11 11 12 13 13 14 14 15 15 16 16 17 17 17 18 18 18 19 19 22 23 24 24 24 26 25\7 27 27 28 28 31 32 32
X X X X X X X X X X X X X X X X X X X X X X X X X X X
Pass Pass Pass Pass Pass Pass Pass Pass /cal Pass Pass Pass Pass 0.5 mm Pass Pass Pass Pass 0.1 mm 0.1 mm Pass < 0.005 !Ci 10 mR/h NCAC limits Pass
Accuracy in Dose Delivery (UCP) Precision in Dose Delivery (profiles) Transit Error
0.5 mm 1mm - 0.05 min
Page 41
PCMH Gamma Knife Center
Absorbed Dose Rate (output) Timer Linearity (dose rate linearity) Timer Accuracy LGP 30 Gy Calculation Couch Movement Time Output Factors (helmet factors)
Cleaning
Physics Quality Control PROCEDURES
33 35 35 35 36 36 37 37 37 38 X X X X X X X X X
Last Update # Version
07/01/09 1.0 - C
3% 2% 6s /15min 2% 30 40s 2% -
Operator Console Camera Lens Monitors Gamma Knife Unit
Page 42
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
6.2.Daily Spot Check Form
Picture of the form used for week/daily spot checks. The template file is maintained in the Radiation Oncology Department Pirate Drive (mount a drive with the following information // radoncp/physics) The file is kept under the Physics/Gammaknife folder.
Page 43
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
6.3.Monthly Spot Check Form
Picture of the monthly spot checks form. MonthlyCheck.xls is a MS Excel spreadsheet that manages all calculation and checks. The measured data are entered in the green cells. The template file is maintained in the Radiation Oncology Department Pirate Drive (mount a drive with the following information //radoncp/physics) The file is kept under the Physics/ Gammaknife folder. Note: The data in yellow and green cells are generic examples.
Page 44
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
6.4.Annual Check List Form
Interval: Not to exceed one year Procedure: 1. Do all procedures for the monthly spot check. 2. Measure the relative helmet factors and verify them in kula.txt. 3. Irradiate film for all helmets in axial, coronal and sagittal aspects. 4. Irradiate film for Mechanical Isocenter /Radiation Isocenter Coincidence. 5. Evaluate all films.
Page 45
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
6.5.Radiation Survey Form
The template file is maintained in the Radiation Oncology Department Pirate Drive (mount a drive with the following information //radoncp/physics) The file is kept under the Physics/ Gammaknife folder.
Page 46
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
6.6.Instruments Used for Gamma Knife Unit Calibration
Introduction The dosimetry system for Gamma Knife Stereotactic Radiosurgery shall be initially established via initial beam specification and calibration and shall be maintained thereafter through monthly and annual checks and calibrations. Protocols for the calibration follow procedures currently published by the AAPM. An independent check of the machine output shall be performed annually to verify that the treatment unit calibration is consistent with national standards. This document specifies the policy adopted by the PCMH Gamma Knife Center to verify and maintain the calibration of the instrumentation used for dosimetry. Procedure The following instruments are used: A A16 Exradin ionization chamber, serial number XAA052131, calibrated on 9/5/2007 B CNMC 206 electrometer, serial number 10508155, calibrated on 8/29/2007 C Digital Barometer/Altimeter Nova Lynx, serial number 908342-W1, calibrated on 5/12/2005. D Hart Scientific Thermometer 1521 serial number A58222, calibrated on 4/25/2008. E Survey meters: Bicron Surveyor 2000 serial number A887U, calibrated on 11/2008 and Fluke Biomedical 451P-RYR serial number 2395, calibrated on 9/2/2008. A The ionization chamber is calibrated at an ADCL with 2-year frequency or every time it is suspected that there is a malfunction. The physicist should determine such situation via intercomparison with similar calibrated ionization chamber. B The electrometer is calibrated at an ADCL with 2-year frequency or every time it is suspected that there is a malfunction. The physicist should determine such situation via intercomparison with another calibrated electrometer. C The barometer shall be verified against the air pressure reported by the NOAA National Oceanic and Atmospheric Administration for the PGV airport corrected for the altitude of 52 feet in a monthly basis. Another calibration of the barometer will be done when discrepancy between the comparisons is over 2%. D - The thermometer is intercompared every year by the medical physicist or every time it is suspected that there is an equipment malfunction. E The survey meters are sent for calibration by the PCMH Radiation Safety Department every year. Record Keeping The calibration certificates and the records of verifications and intercomparisons will be maintained at the Gamma Knife Operation room.
Page 47
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
6.7.LGP Treatment Planning System QA
Introduction The LGP Treatment Planning System QA will consist of daily (on the day of the procedure), monthly and annual or upgrade checks. Procedure Daily 1. Check the date of calibration, dose rate and output factors used in the patient plan. Last version is 8.3.1. The calibration date is 9/30/2005 and the dose rate is 3.582 Gy/min. The output factors are 0.870, 0.956, 0.984 and 1.000 for 4, 8, 14 and 18 mm collimators respectively. Decay the dose rate by hand calculation/spreadsheet to todays date and compare with plan. Sign to confirm the decayed calculation by the current dose rate value. Monthly 1. After monthly calibration, compare the dose rate measured with decayed from plan, patient: Phantom Dosimetry. Open the patient file in LGP, go to plans and copy a new plan for today treatment. 2. Print out the plan, check calibration date, output factors and decayed output. Check the treatment time and fill the monthly form. 3. Save the plan printout with the Monthly form in the Monthly and Annual QA log binder. See example in Appendix. Annual or Upgrade 1. After upgrade or after annual calibration, certified the data in LGP and print out the Install Test patient. 2. To certify the data you need to log in as an administrator. 3. Open patient: Test Install. Copy a new plan for todays treatment. Use snapshop workspace. Put cross hair at the lesion (posterior lesion) slice 91 and zoom into the lesion. Take a snapshot. Go to measurements, get volumes for the matrix, skull and tu. Also get, DVH for all three volumes. Printout protocol, snapshot and measurements. Compare with values in the annexed document.
Page 48
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
6.8. GK Patients Plans Backup
Introduction The GK Patient Plans Backup will be done every month (around the 1st of the month). Procedure There are two separate external hard disks. They are used alternatively for redundancy. 1. 2. 3. 4. 5. Log in into Leksell Gamma Plan as an administrator Log in again as an administrator Select storage tab Press backup button Restore of backups is only done by the Elekta engineer.
Users List: administrator Admin default Admin lgp planner motah Admin root physics phys planner planner sibata Admin physicist phys
Page 49
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
6.9.Log Book Forms (Event Records)
Page 50
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
6.10.Treatment Variance Reports
PCMH Gamma Knife Center
TREATMENT VARIANCE REPORT
Patient Name: Diagnosis: Treatment Variance description: MR#: Date of treatment:
Please attach pictures if needed
Immediate action taken (if any):
Event classification
Medical Event?
" Yes
" No
Expected Clinical Outcome:
Remedial Actions / Prevention:
Additional Notes:
Name Radiation Oncologist Medical Physicist Neurosurgeon
Signature
Date:
Page 51
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
6.11.Useful Phones and Contacts
Elekta service representative 1-800-3354 Site number US131125/001 James Wooder: 757-676.5238 James.wooder@elekta.com
Page 52
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
6.12.Calibration Certificates
See corresponding binder Next calibration of electrometer/ionization chamber is September 2009.
Page 53
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
6.13.Gamma Knife Technical Data
Physical Data Overall length, including cover Overall width, including cover Overall height, including cover Total weight (approximate) Maximum load on couch Radio-physical Data Total cobalt-60 activity at loading (approx.) Number of radiation sources Radiation dose rate at focal point at loading Accuracy Data APS positioning accuracy Mechanical isocenter radius Helmet positioning accuracy Treatment timer APS Range of Movement APS x axis APS y axis APS z axis (normal) APS z axis (high docking position) Batteries There are two UPS units containing batteries; one in the electrical cabinet (called Medical UPS) and one in the computer cabinet (called Office UPS). The UPS in the electrical cabinet contains rechargeable, dry lead, maintenance-free batteries. The UPS in the computer cabinet contains rechargeable, dry lead, maintenance-free batteries. The mouse operates with two AAA / LR03 1.5 volt alkaline type batteries. 59.0 to 141.0 mm 40 to 160 mm 58 to 142 mm -11 to 77 mm < 0.2 mm < 0.3 mm < 0.1 mm < 0.2 % < 6,600 Curie (< 2.44 x 1014 Bq) 201 > 3 Gy min-1 4.64 m 2.00 m 1.94 m 20,000 kg 180 kg
Page 54
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
Page 55
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
6.14.Example for Monthly QA
Page 56
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
Page 57
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
Page 58
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
6.15.Example for Annual QA
Page 59
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
Page 60
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
Page 61
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
Page 62
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
Page 63
PCMH Gamma Knife Center
Physics Quality Control PROCEDURES
Last Update # Version
07/01/09 1.0 - C
Login/Passwords
Gamma Knife console: OP/OP GammaPlan: lgp/elekta or planner/planner Administrator: administrator/administrator root/3l3kta
Page 64
Vous aimerez peut-être aussi
- Exam 3 Study GuideDocument10 pagesExam 3 Study GuideJared MehargPas encore d'évaluation
- Common Derivatives IntegralsDocument4 pagesCommon Derivatives Integralsapi-243574449Pas encore d'évaluation
- Calculus Based PhysicsDocument267 pagesCalculus Based PhysicsSAMEER ALI KHANPas encore d'évaluation
- Karzmark Primer On Linear AcceleratorsDocument56 pagesKarzmark Primer On Linear AcceleratorsJared Meharg100% (3)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeD'EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeÉvaluation : 4 sur 5 étoiles4/5 (5794)
- Shoe Dog: A Memoir by the Creator of NikeD'EverandShoe Dog: A Memoir by the Creator of NikeÉvaluation : 4.5 sur 5 étoiles4.5/5 (537)
- The Yellow House: A Memoir (2019 National Book Award Winner)D'EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Évaluation : 4 sur 5 étoiles4/5 (98)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceD'EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceÉvaluation : 4 sur 5 étoiles4/5 (895)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersD'EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersÉvaluation : 4.5 sur 5 étoiles4.5/5 (344)
- The Little Book of Hygge: Danish Secrets to Happy LivingD'EverandThe Little Book of Hygge: Danish Secrets to Happy LivingÉvaluation : 3.5 sur 5 étoiles3.5/5 (399)
- Grit: The Power of Passion and PerseveranceD'EverandGrit: The Power of Passion and PerseveranceÉvaluation : 4 sur 5 étoiles4/5 (588)
- The Emperor of All Maladies: A Biography of CancerD'EverandThe Emperor of All Maladies: A Biography of CancerÉvaluation : 4.5 sur 5 étoiles4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaD'EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaÉvaluation : 4.5 sur 5 étoiles4.5/5 (266)
- Never Split the Difference: Negotiating As If Your Life Depended On ItD'EverandNever Split the Difference: Negotiating As If Your Life Depended On ItÉvaluation : 4.5 sur 5 étoiles4.5/5 (838)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryD'EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryÉvaluation : 3.5 sur 5 étoiles3.5/5 (231)
- On Fire: The (Burning) Case for a Green New DealD'EverandOn Fire: The (Burning) Case for a Green New DealÉvaluation : 4 sur 5 étoiles4/5 (73)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureD'EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureÉvaluation : 4.5 sur 5 étoiles4.5/5 (474)
- Team of Rivals: The Political Genius of Abraham LincolnD'EverandTeam of Rivals: The Political Genius of Abraham LincolnÉvaluation : 4.5 sur 5 étoiles4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyD'EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyÉvaluation : 3.5 sur 5 étoiles3.5/5 (2259)
- The Unwinding: An Inner History of the New AmericaD'EverandThe Unwinding: An Inner History of the New AmericaÉvaluation : 4 sur 5 étoiles4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreD'EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreÉvaluation : 4 sur 5 étoiles4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)D'EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Évaluation : 4.5 sur 5 étoiles4.5/5 (121)
- Her Body and Other Parties: StoriesD'EverandHer Body and Other Parties: StoriesÉvaluation : 4 sur 5 étoiles4/5 (821)
- The Hybrid Denture1Document9 pagesThe Hybrid Denture1SitiKhadijah100% (1)
- Ebook Selective Anatomy Prep Manual For Undergraduates Vol 1 2E PDF Full Chapter PDFDocument67 pagesEbook Selective Anatomy Prep Manual For Undergraduates Vol 1 2E PDF Full Chapter PDFcharles.brewer536100% (25)
- Revision Tables - 270820162807Document105 pagesRevision Tables - 270820162807flickers xxxPas encore d'évaluation
- 01 Introductory PgyDocument76 pages01 Introductory Pgygbsreg gbsregPas encore d'évaluation
- Scotchcast PDFDocument311 pagesScotchcast PDFSaadPas encore d'évaluation
- Studer Surgical - Images - of - Ileal - ConduitDocument11 pagesStuder Surgical - Images - of - Ileal - ConduitTomek RPas encore d'évaluation
- The Urinary SystemDocument46 pagesThe Urinary SystemWeb AredomPas encore d'évaluation
- Bipolar Forceps 3-3 - 8in CrvreuseDocument4 pagesBipolar Forceps 3-3 - 8in CrvreuseSalma El MamouniPas encore d'évaluation
- CPT PCM NHSNDocument307 pagesCPT PCM NHSNYrvon RafaPas encore d'évaluation
- AscitesDocument32 pagesAscitesIsaac MwangiPas encore d'évaluation
- Acls AtpDocument44 pagesAcls AtpDeborah Anasthasia PakpahanPas encore d'évaluation
- How To Increase Breast SizeDocument7 pagesHow To Increase Breast SizeAndrewJonathanPas encore d'évaluation
- اخطاء سامح دوز (@USEM BOT)Document3 pagesاخطاء سامح دوز (@USEM BOT)Nona Al-shaibaniPas encore d'évaluation
- JAAOS - Volume 05 - Issue 02 March 1997Document60 pagesJAAOS - Volume 05 - Issue 02 March 1997kenthepaPas encore d'évaluation
- KKPMT IV B ICD 9 Female GenitaliaDocument31 pagesKKPMT IV B ICD 9 Female GenitaliaAldy SetyawanPas encore d'évaluation
- Tim Gilbert and Nicola Rudge Chief of Medicine 1 Service and Chief PharmacistDocument39 pagesTim Gilbert and Nicola Rudge Chief of Medicine 1 Service and Chief PharmacistjellyjohnPas encore d'évaluation
- SuccinylcholineDocument2 pagesSuccinylcholineSalma KarimahPas encore d'évaluation
- serdevASMS1 4 2014Document25 pagesserdevASMS1 4 2014Doctores Duarte BarrosPas encore d'évaluation
- Fortisian 5 MBDocument44 pagesFortisian 5 MBBadass BitchPas encore d'évaluation
- Cardiovascular SystemDocument6 pagesCardiovascular SystemNashreen QtqtPas encore d'évaluation
- (Gross A) Lower Extremities, Thorax, and Lungs Practicals Reviewer (Gabasan) (Lab)Document75 pages(Gross A) Lower Extremities, Thorax, and Lungs Practicals Reviewer (Gabasan) (Lab)Kristine Nicole UbanaPas encore d'évaluation
- RENAP 2009 Training SchedulesDocument3 pagesRENAP 2009 Training SchedulesNoel100% (4)
- What Is Extracorporeal Cardiopulmonary Resuscitation?: Federico Pappalardo, Andrea MontisciDocument5 pagesWhat Is Extracorporeal Cardiopulmonary Resuscitation?: Federico Pappalardo, Andrea MontisciPrajogo KusumaPas encore d'évaluation
- Policies and Procedures For Ambulance ServiceDocument3 pagesPolicies and Procedures For Ambulance ServiceLymberth Benalla100% (1)
- A Narrative Review of The Management of Nasal Foreign Bodies in Children in General PracticeDocument8 pagesA Narrative Review of The Management of Nasal Foreign Bodies in Children in General PracticeLennon Ponta-oyPas encore d'évaluation
- Duodenum AnatomyDocument3 pagesDuodenum AnatomyAce Acapulco100% (1)
- 812-Article Text-2928-1-10-20191129 (PMR)Document6 pages812-Article Text-2928-1-10-20191129 (PMR)Azza SintaPas encore d'évaluation
- Oper Ations Management Case Study On ShouldiceDocument11 pagesOper Ations Management Case Study On Shouldicegauarv_sharma100% (1)
- JurnalDocument60 pagesJurnalHumairah AnandaPas encore d'évaluation
- Eyehance MTFDocument6 pagesEyehance MTFanandprasad244Pas encore d'évaluation