Académique Documents
Professionnel Documents
Culture Documents
Lower Limb Review
Transféré par
Ryan SilberDescription originale:
Copyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
Lower Limb Review
Transféré par
Ryan SilberDroits d'auteur :
Formats disponibles
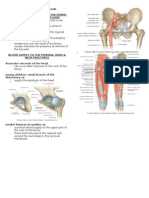
SUPERFICIAL STRUCTURES OF THE LOWER LIMB
Iliotibial tract: Laterally, the fascia lata is thickened to form the iliotibial tract. The iliotibial tract receives the insertions of the tensor fascia lata and gluteus maximus muscles. In the upper part, it has two layers- superficial layer attached to the iliac tubercle (superficial to the Tensor fascia lata), and the deep layer attached to the fibrous capsule of the hip-joint. The two layers fuse below the tensor fascia lata to form a single band down the lateral side of the thigh and is attached to the lateral condyle of the tibia.
Dermatomes:
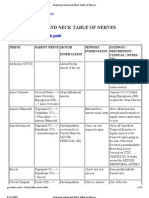
Lower limb Spinal Nerve Dermatomes: L1 = groin (hand in jeans pocket) L2 = lateral thigh S1 = Lateral aspect of the foot, the heel & most of the sole of the foot S2 = median posterior strip of thigh & leg S3 = sitting area of the buttock KNOW IN DETAIL the cleft between the toes, dermatomes and cutaneous nerves of the femoral triangle and the FOOT! (Cutaneous innervation of the hand and the foot are very very important) CUTANEOUS INNERVATION OF THE LOWER LIMB 1. Iliohypogastric nerve: (L1-from lumbar plexus) Supplies the skin of the buttock. 2. Ilioinguinal nerve: (L1-from lumbar plexus) Supplis the skin of the proximal, medial thigh. 3. Genitofemoral nerve: (L1 & L2- from lumbar plexus) Supplis the skin of the proximal, anterior thigh, just inferior to inguinal ligament. 4. Saphenous nerve: (L2,L3 & L4) It is the terminal branch of the femoral nerve. It supplies the skin of the anterior and medial side of the leg and the medial side of the foot except the medial side of the big toe. 5. Sural nerve: It is a branch of the tibial nerve. It Supplies the skin on the posterior and lateral aspects of the leg and lateral side of the foot. 6. Sural communicating nerve: It is a branch of the common peroneal nerve. It Supplies the skin of the posterolateral leg. 7. Superficial peroneal (fibular) nerve: It is a branch of the common peroneal nerve. It supplies the skin of the lower third of the leg and the dorsal part of the foot and medial side of the great toe, except the cleft between the great and 2nd toes. 8. Deep peroneal (fibular) nerve: Is a branch of the common peroneal nerve. It supplies skin on the cleft between the great and 2nd toes. 9. Medial and lateral plantar nerves: are branches of the tibial nerve. They supply the skin of the sole of the foot. The medial plantar nerve supplies medial 3 digits. The lateral plantar nerve supplies lateral 1
digits.
Great saphenous vein:
Extent: It begins on the medial side of the dorsum of the foot by the union of the dorsal vein of the great toe and the medial end of the dorsal venous arch. It ends in the femoral vein about 3 cm. below the inguinal ligament. Course: It ascends in front of (anterior to) the medial malleolus and along the medial side of the leg accompanied by the saphenous nerve. Passes through the saphenous opening (hooks around the falciform margin of the saphenous opening), pierces the cribriform fascia and ends in the femoral vein.
Small saphenous vein
Extent: It begins on the lateral side of the foot from the union of the dorsal vein of the small (little) toe with the lateral end of the dorsal venous arch. It ends by opening to the popliteal vein in the popliteal fossa. Varicose veins: When the superficial veins become abnormally dilated and tortuous (twisted), they are called varicose veins. Most commonly the great saphenous vein is involved. They often cause discomfort. Varicosity may be due to following reasons: a. hereditary weakness of the venous walls b. incompetence of the valves therefore allows the backflow of blood and they dilate c. increased intra-abdominal pressure- in multiple pregnancies or abdominal tumors. d. thrombophlebitis of the deep veins To relieve the condition, the superficial veins and tributaries and/or the incompetent perforator veins are ligated and removed. Vericoses also occur in the testicles Trendelenburgs test I: is performed to test the incompetency of the perforators & superficial veins (trendelenburgs test II is performed for assessing gluteal muscles). Saphenous cutdown : Great saphenous vein is easily be located by making a skin incision anterior to the medial malleolus. This procedure is called saphenous cutdown. This procedure is used for insertion of a canula for prolonged administration of medication in infants and obese persons, or in patients in shock. The saphenous nerve may be cut during this procedure and the patient may complain of pain along the medial border of the foot. Lie in the supine position, raise you leg and empty the vein, tie a bandage arund the saphenous opening. Stand up and after 60 secs the tonicate is removed and in ~ 30 sec the entire leg should fill with blood (competent valves).
Lymphatic drainage of the lower limb: Lymph nodes of the lower limb consist of Inguinal lymph nodes (superficial and deep group) Popliteal lymph nodes Anterior tibial lymph node
FEMORAL TRIANGLE
Boundaries: Laterally - by the Sartorius Medially- by the medial margin of the Adductor longus Base - is directed above and formed by the inguinal ligament (thickening of lower border of ext oblique). Attach to the sup. Ant. Ilic crest and pubic tubercle - mid point of inguinal ligament (between the ant. Sup iliac crest and pubic tubercle) is different from the mid-inguinal point (mid point of line drawn between ant. Sup. Iliac spine and pubic symphysis) Apex - is directed downward and is formed by the crossing of sartorius over the adductor longus. Roof Skin Superficial fascia Superficial inguinal lymph nodes and superficial blood vessels (know the names of the blood vessels found on the roof ie. Exam. Which of these structures is not part of the roof of the triangle) 1. Superficial epigastric 2. Sup. Ext iliac 3. Sup ext pudental arteries Deep fascia Floor - lateral to its medial side by: 1. Iliacus lateral (at this point the iliacus and iliopsoas have united and are now called the liopsoas) 2. Psoas major 3. Pectineus 4. Adductor longus medial boundary (therefore also forms floor) 5. In some cases a small part of the Adductor brevis Contents: 1. A pad of fat 2. Deep Inguinal lymph nodes and the Lymph vessels 3. Femoral artery and its branches- 3 superficial branches (superficial ext.pudendal, superficial epigastric, superficial circumflex iliac) Deep external pudendal A, Profunda femoris A, Muscular branches 4. Femoral vein- it is medial to the femoral artery in the upper part of the triangle, but comes to its posterior aspect near the apex of the triangle. It receives the great saphenous vein and the profunda femoris vein in the triangle.
5. Femoral nerve it lies lateral to the femoral artery and outside the femoral sheath. It soon divides into its branches. 6. Femoral branch of the genitorfemoral nerve. It descends close to the femoral artery. 7. Femoral sheath- it encloses the femoral vessels and the femoral canal
FEMORAL SHEATH
It does not enclose the femoral nerve. femoral nerve lies deep to fascia iliacus and therefore does not get covered by the sheath. The anterior wall of the sheath is formed by the downward prolongation of the fascia transversalis of the abdomen, in front of the femoral vessels. The posterior wall of the sheath is formed by the downward prolongation of the fascia iliaca behind the femoral vessels. The interior of the sheath is divided into 3 compartments by two anteroposterior septa that stretch between its anterior and posterior walls. The lateral compartment contains the femoral artery and the femoral branch of the genitofemoral N (lateral to the artery). The middle compartment contains the femoral vein The medial and smallest compartment is named the femoral canal, and contains some lymphatic vessels and a lymph gland (Cloquets lymph node is a deep inguinal lymph node). Femoral canal- It is conical and measures about 1.25 cm. in length.Its base is directed upward and open to the abdomen and named the femoral ring (upper end of the femoral canal). It is closed by the femoral septum. Its lower end extends to the level of the saphenous opening Femoral hernia can occur through the femoral ring into the femoral canal. The direction of course of the femoral hernia is downwards through the femoral canal, then forwards through the saphenous opening, and finally upwards and laterally (U-shape). Organs such as the intestine may pertrude into femoral ring. Usually, herniation will be confined to femoral sheath but sometimes it can go inferiorly and pass through the saphenous opening and lie right under the skin. There can be a strangulation of the herniated structure and the blood supply is lost leading to necrosis of the organ It can be reduced by following in reverse order. While releasing strangulation of the femoral hernia, the lacunar ligament is incised. Before incising the lacurnar ligament for enlarging the femoral ring, care should be taken to avoid injury to the accessory obturator artery (not always there called a common variation), which may run along its concave free margin. May lead to severe bleeding. This artery is a branch of the inferior epigastric artery which comes from the external iliac artery
ADDUCTOR CANAL
Boundaries: Anterolaterally - by the Vastus medialis Posteriorly - by the Adductor longus in the upper half
Adductor magnus in the lower half. At the junction of the middle and lower of the thigh, there is an opening in (in the adductor magnus) for the femoral vessels Roof formed by 1. A fibrous sheet which extends from the Vastus medialis, across the femoral Vessels to the Adductor longus and magnus. 2. Sartorius muscle lying on the aponeurosis 3. Subsartorial plexus of nerves lies on the fibrous roof. The subsartorial plexus is formed by branches froma) medial cutaneous N of the thigh. b) saphenous N c) obturator N Contents 1. Femoral artery 2. Femoral vein 3. Saphenous nerve branch of the femoral nerve, 4. Nerve to the Vastus medialis branch of femoral nerve
Muscle sartorius
Action flexes, abducts, laterally rotates thigh; flexes and medially rotates leg at knee Also, slight flexion of the thigh Chief flexor of the thigh. When the thigh is fixed, it flexes the trunk on the thigh as in sitting up. It is a postural muscle same as iliacus
Nerve Supply femoral nerve
iliacus
femoral nerve
psoas major
Ventral rami of the L2 & L3 (roots of the lumbar plexus (L1-L4))
pectineus
flexes and adducts thigh
femoral nerve Some times by obturator or accessory obturator nerves
rectus femoris
extension of leg Assists on flexion of the thigh (Note: observe its origin) extension of leg extension of leg extension of leg Pulls up the synovial membrane during extension of the knee joint prevents crushing of synovial membrane during extension Abduction and medial rotation of the thigh. Steadies the tibia on the femur while standing
femoral nerve
vastus lateralis vastus medialis vastus intermedius Articularis genu
femoral nerve (L2-L4) femoral nerve femoral nerve Femoral nerve
Tensor fascia lata
Superior gluteal nerve (from sacral plexus)
Femoral artery:
It is the direct continuation of the external iliac artery. It begins immediately behind the inguinal ligament at the mid-inguinal point (midpoint between the anterior superior iliac spine and the symphysis pubis). This is where you feel for the pulse of the artery Termination: It ends at the junction of the middle with the lower third of the thigh, where it passes through an opening in the Adductor magnus to become the popliteal artery. Know relations to femoral artery and nerve and that is is covered in a femoral sheath Relations: In the femoral triangle: The first 4 cm. of the vessel is enclosed, together with the femoral vein, in a fibrous sheaththe femoral sheath. The femoral artery lies in the lateral compartment of the femoral sheath along with the femoral branch of the genitofemoral nerve. In the femoral triangle, the artery is superficial. In front of it are the skin and superficial fascia, the superficial inguinal lymph glands, the superficial circumflex iliac vessels, fascia lata and the anterior wall of the femoral sheath.
Laterally: 1.The femoral branch of the genitofemoral nerve 2. The femoral nerve & its branches (Femoral nerve lies outside the femoral sheath) Posterior: Behind the artery are -1. Posterior wall of the femoral sheath (Bed) 2. Psoas major tendon 3. Pectineus 4. Adductor longus. 5. Fibrous Capsule of the hip joint 6. Femoral vein (in the lower part) The artery is separated from the capsule of the hip-joint by the tendon of the Psoas major Medially: The femoral vein NOTE:(femoral vein lies on the medial side of the upper part of the artery, but is behind (posterior to-) the femoral artery in the lower part of the femoral triangle).
The profunda femoris artery
Branches: In femoral triangle, gives off 2 branches Medial Circumflex Femoral- arises from the medial side. It anastomoses with the inferior gluteal, lateral femoral circumflex, and first perforating arteries (cruciate anastomosis). The acetabular branch of the medial circumflex femoral artery supplies hip joint. Lateral Circumflex Femoral A- arises from the lateral side of the profunda, It takes part in the cruciate anastomosis on the back of the thigh.
Lumbar Plexus
Root value- L1, L2, L3, L4. It is located in the posterior abdominal wall within the psoas major muscle. The branches of the lumbar plexus are: Iliohypogastric- L.1 (lateral) Ilioinguinal- L.1 (lateral) Genitofemoral- L. 1, 2 (anterior) Lateral cutaneous nerve of the thigh- L 2, 3 (lateral) Femoral - L 2, 3, 4 (Dorsal divisions of the ventral rami) (lateral) Obturator - L 2, 3, 4. (Ventral divisions of the ventral rami) (medial) Accessory obturator - L 3, 4 (Ventral divisions of the ventral rami)
Femoral Nerve
Root value (Origin) from the lumbar plexus, Dorsal divisions of the ventral rami of L2, L3, L4. Origin is in the posterior wall of the abdominal cavity within the psoas major muscle. It emerges from the muscle at the lower part of its lateral border. In the femoral triangle, it lies lateral to the femoral vessels and outside the femoral sheath. It soon splits into an anterior and a posterior division. Branches I. Within the abdomen
1. Small branches to the Iliacus 2. A branch to the upper part of the femoral artery 3. Nerve to pectineus it crosses behind the femoral sheath to reach the muscle. KNOW that it innervates the iliacus and pectineus in the pelvis B. Branches from the posterior division of the femoral nerve (mainly muscular) 1. Saphenous nerve only cutaneous nerve from this division. Runs lateral to femoral artery and then medial to artery through adductor canal. Does not go through adductor hiatus but pierced through roof of canal and goes medial to knee joint and ends at the ball of the great toe (first metatarsal joint) (Know saphenous nerve in detail*** It is the longest cutaneous nerve in the body 2. Branches to the quadriceps femoris muscles (Rectus femoris, Vastus lateralis, Vastus intermedius, Vastus medialis). o The branch supplying the rectus femoris gives an articular branch to the hip joint o The branch supplying the vastus intermedius gives an articular branch to the knee joint 3. Articular branch (goes to joint) to the medial side of the knee joint - comes from the nerve from the vastus medialis Saphenous Nerve It is the largest cutaneous branch of the femoral nerve. In the lower part of the femoral triangle and upper part of the adductor canal it lies lateral to the femoral artery. Then it crosses in front of the artery from lateral to medial side. In the lower part of the adductor canal it lies medial to the artery as far as the opening in the lower part of the Adductor magnus. It pierces the deep fascia and accompanies the saphenous artery. In the leg, it accompanies the great saphenous vein to the front of the medial malleolus and then runs forward on the medial border of the foot, and is distributed to the skin on the medial side of the foot, as far as the ball of the great toe.
MUSCLES OF THE MEDIAL SIDE OF THE THIGH
Muscle adductor longus Action adducts thigh and assists in lateral rotation adducts thigh and assists in lateral rotation Nerve Supply obturator nerve (Ant. Division)
adductor brevis
obturator nerve (Ant. Division)
adductor magnus
Adductor part-inferior ramus of pubis; ramus of ischium (ischiopubic ramus) Hamstring part- ischial tuberosity
Adductor part- gluteal tuberosity, linea aspera, medial supracondylar line. Hamstring partadductor tubercle of femur
Adducts thigh and assists in lateral rotation. Hamstring part extends thigh
Adductor partobturator nerve (Post. Division) Hamstring parttibial part of sciatic nerve
Openings in the adductor magnus- (5 osseoaponeurotic openings): At the insertion of the adductor magnus, there is a series of osseoaponeurotic openings, formed by tendinous arches attached to the bone. The upper four openings are small, and give passage to the perforating branches of the profunda femoris artery. The lowest is of large size (hiatus magnus), and transmits the femoral vessels to the popliteal fossa.
The Obturator Nerve
The anterior division descends in front of the Obturator externus and the Adductor brevis The posterior division pierces the anterior part of the Obturator externus, and supplies this muscle. It then passes behind the Adductor brevis on the front of the Adductor magnus.
LEG ANTERIOR COMPARTMENT OF THE LEG AND DORSUM OF THE FOOT
Structures passing deep to the superior extensor retinaculum are- (KNOW THE ARRANGMENT!) From medial to lateral: Tibialis anterior Extensor hallucis longus Anterior tibial artery (& vein) Anterior tibial nerve (deep peroneal N). Extensor digitorum longus Peroneus tertius
MUSCLES OF THE ANTERIOR COMPARTMENT OF THE LEG AND DORSUM OF THE FOOT
KNOW THE JOINTS THAT THESE MUSCLES ACT ON! Muscle Action tibialis anterior Extends (dorsiflexion) the foot at ankle; Nerve Supply deep peroneal nerve
extensor digitorum longus
peroneus tertius extensor hallucis longus extensor digitorum brevis extensor hallucis brevis (is the medial most part of the extensor digitorum brevis)
inverts foot at subtalar joint helps to maintain the medial longitudinal arch of foot (SUBTALAR JOINT) extends the lateral 4 toes; dorsiflexes (extends) foot at the ankle. Flexes all the joints that it crosses which are many dorsiflexes (extends) foot; everts foot at subtalar joint
(anterior tibial N) Innervates cleft between 1st and 2nd toe deep peroneal nerve (anterior tibial N)
deep peroneal nerve (anterior tibial N) extends big toe; dorsiflexes foot; inverts foot at subtalar deep peroneal nerve joint (anterior tibial N) Extend the 2nd, 3rd, & 4th toes at the deep peroneal nerve metatarsophalangeal joints. (anterior tibial N) extends big toe deep peroneal nerve (anterior tibial N)
Anterior Tibial Artery
it becomes the dorsalis pedis artery
Dorsalis Pedis Artery
It is the continuation of the anterior tibial artery. Extent: From the midpoint of the front of the ankle joint it runs forwards in the dorsum of the foot to the proximal part of the first intermetatarsal space. Termination: It dips between the two heads of the 1st dorsal interosseous and joins the lateral plantar artery to complete the plantar arch. The pulse is felt On its medial side is the tendon of the Extensor hallucis longus On its lateral side, the first tendon of the Extensor digitorum longus, and the termination of the deep The arcuate artery Clinical: pulsations of the dorsalis pedis artery can be easily felt.
Deep Peroneal Nerve
Foot drop:
Common peroneal nerve is in danger of injury because of its superficial position (neck of fibula). Injury leads to paralysis of all the dorsiflexors and evertors of the foot (muscles of the anterior and lateral compartments) resulting in foot drop. The toes drag on the foot while walking. Cutaneous sensibility is lost in the
anterolateral aspect of the leg and dorsum of the foot excepting the outer and inner border of the foot (supplied by the sural and saphenous nerves respectively). MAY BE DUE TO FRACTURE OF THE FEMUR!!!!
LATERAL COMPARTMENT OF THE LEG
Lateral compartment of the leg consists of the two evertors of the foot- Peroneus longus and Peroneus brevis. ALL PERONIAL MUSCLES EVERT THE FOOT BUT ONLY THE LONGUS AND BREVIS ARE SUPPLIED BY THE SUPERFICIAL PERONIAL NERVE (IE. NOT THE TERTIOUS DEEP PERONIAL NERVE) KNOW WHICH JOINTS THEY ACT ON! Muscle peroneus longus peroneus brevis Action Nerve Supply superficial peroneal (musculocutaneous) nerve
everts foot at subtalar joint. Plantar flexes (flexes) foot. supports lateral longitudinal arch (sling)and transverse arch (bow string) of foot everts foot superficial peroneal nerve at subtalar joint. plantar flexes (flexes) foot. Holds up lateral (musculocutaneous nerve) longitudinal arch
Superficial Peroneal Nerve
It supplies Peroneus longus Peroneus brevis Skin of the dorsal surfaces of all the toes except the cleft between the 1st and 2nd toes
(supplied by the deep peroneal nerve), and the lateral side of the little toe (supplied by the sural nerve) MUSCLES OF THE POSTERIOR COMPARTMENT OF THE LEG
Soleus is the peripheral heart (calf pump) Two heads of the gastrocnemius and the soleus are together called Triceps surae
Superficial Group
Muscle Insertion Action Nerve Supply
gastrocnemius
Middle of the posterior surface of calcaneum via tendocalcaneus Plantaris (short muscle Middle of the posterior with long slender surface of calcaneum via tendon) tendocalcaneus Soleus (Bulky muscle) Middle of the posterior surface of calcaneum via tendocalcaneus
plantar flexes (flexes) foot at the ankle; raises heel during walking; flexes knee plantar flexes foot; flexes knee
tibial nerve
tibial nerve
with gastrocnemius, a powerful plantar tibial nerve & flexor of ankle; steadies leg on foot; main posterior tibial propulsive force in walking and running nerve
Deep Group
Popliteus Intracapsular, but Becomes extracapsular Key muscle which unlocks extrasynovial; and inserted into the the knee (flexes) at the beginning Popliteal groove on triangular area above the of the flexion; draws the lateral the lateral surface of soleal line on the meniscus backwards and prevents the lateral condyle of posterior surface of the it from getting crushed during femur, lateral tibia flexion of the knee meniscus of the knee joint flexes distal tibial nerve phalanges of lateral (posterior tibial) four toes; plantar flexes foot; supports lateral longitudinal arch of foot flexes distal phalanx tibial of big toe; plantar nerve(posterior flexes foot; supports tibial) medial longitudinal arch of foot Lateral of posterior (enters 4th layer of the plantar flexes foot; inverts foot surface of tibia sole) tuberosity of (powerful) at subtalar joint. below soleal line; navicular bone mainly, supports medial longitudinal arch posterior surface of and to all the tarsal of foot fibula and bones except the Talus interosseous membrane tibial nerve ( nerve to popliteus winds around its lower border & supplies its anterior surface)
flexor digitorum longus
flexor hallucis longus
tibialis posterior
tibial nerve (posterior tibial)
Posterior Tibial Artery
Termination: It ends under cover of the flexor retinaculum, midway between the medial malleolus and medial tubercle of the calcaneum by dividing into medial and lateral plantar arteries. Relations Behind the medial malleolus, the tendons, blood vessels, and nerve are arranged, under cover of the flexor retinaculum in the following order from the medial to the lateral side: (1) Tibialis posterior (medial) (2) Flexor digitorum longus, (3) Posterior tibial artery, with a vein on either side of it (4) Tibial nerve (5) Flexor hallucis longus. (lateral) **MUST KNOW THIS ARRANGMENT*** (TOM DICK AND VERY NERVOUS HARRY) Note that bleow the medial melleolus you feel for the Posterior Tibial Pulse
Posterior tibial nerve
Root Value? it divides into two branches- medial and lateral plantar nerves.
MUSCLES OF THE GLUTEAL REGION
Muscle gluteus maximus Origin Outer surface of ilium- from the posterior gluteal line and the area behind. From sacrum, coccyx, sacrotuberous ligament Insertion Most fibers to the iliotibial tract, some fibers to the gluteal tuberosity of femur (very important to know for exams) Action Chief extensor at the hip joint. Extends and laterally rotates thigh at hip; through iliotibial tract it extends knee joint and steadies the femur on tibia in standing (assists in rising from sitting position or in climbing stairs) Nerve Supply inferior gluteal nerve (L5,S1,S2)
gluteus medius
gluteus minimus
tensor fascia lata
piriformis
superior gemellus obturator internus inferior gemellus obturator externus quadratus femoris
Abducts and medially rotates the thigh at hip; tilts pelvis when walking. Keeps pelvis level when opposite leg is raised during walking therefore, when they are paralyzed, unsupported (leg off ground) side will sag. LOOK UP TRENDELENBERGH TEST II test competency of the sup. Gluteal nerve abducts and medially rotates the thigh at hip; keeps pelvis level when opposite leg is raised Abduction and medial rotation of the thigh. Steadies the femur on tibia in standing. Assists gluteus maximus in extending knee joint Lateral rotator of thigh. Abduct the thigh when the thigh is flexed. Steadies femoral head in acetabulum lateral rotator of thigh
superior gluteal nerve (L4,L5,S1)
superior gluteal nerve
superior gluteal nerve
Ventral rami of sacral nerves S1 and S2 Nerve to obturator internus (L5,S1,S2) Nerve to obturator internus (L5,S1,S2) Nerve to quadratus femoris (L4,L5,S1) obturator nerve posterior division Nerve to quadratus femoris(L4,L5,S1)
lateral rotator of thigh
lateral rotator of thigh Lateral rotator of thigh. steadies the head of femur in acetabulum lateral rotator of thigh
(STRUCTURES DEEP TO THE GLUTEUS MAXIMUS) Communication between the pelvis and the gluteal region is done via the greater sciatic foramen
The piriformis muscle is the key to this region. Superior gluteal vessels and nerve emerge above the piriformis. All other structures are below the piriformis. 1. Bony structures- Greater trochanter, Ischial tuberosity, Ischial spine 2. Bursae- trochanteric bursa, Ischial bursa, gluteofemoral bursa 3. Ligaments- Sacrotuberous ligament, Sacrospinous ligament 4. Muscles1) Gluteus medius 2) Gluteus minimus *Glutei medius and minimus abduct the hip joint and prevent adduction of the thigh when the body weight is on the same leg. 3) Piriformis key because many structures pass above and below EXAM What structures pass above and below piriformis Above superior gluteal nerve and vessels Below PIN structures (pudendal nerve, internal pudendal artery, nerve to obturator internus) - inferior gluteal nerve - sciatic nerve - posterior cutaneous nerve of the thigh (passes posterior or superficial to the sciatic nerve) - nerve to quadratus femoris
4) Superior gemellus another key muscle because many structures that pass above and below piriformis 5) Obturator internus 6) Inferior gemellus 7) Quadratus femoris 8) Upper part of adductor magnus 9) Origin of hamstrings 5. NervesNerve emerging above the piriformis: 1) Superior gluteal nerve Nerves those emerge inferior to piriformis 1) Sciatic nerve (L4, 5, S1, 2, 3) lies between the ischial tuberosity and the greater trochanter. Its "safe" side for gluteal injection is the lateral side where it has no branches. It may divide in this region into the common peroneal (L4, 5, S1, 2) and the tibial (L4, 5, S1, 2, 3) nerves. 2) Nerve to quadratus femoris 3) Posterior cutaneous nerve of the thigh 4) Inferior gluteal nerve. 5) Pudendal nerve (S2, 3, 4) 6) Nerve to obturator internus (L5, S1, 2)
6. Blood vessels 1. Superior gluteal artery & vein branch of the posterior division of the internal iliac artery 2. Inferior gluteal artery & vein branch of the anterior division of the internal iliac artery 3. Internal pudendal vessels branch of the anterior division of the internal iliac artery 4. Cruciate anastomosis 5. Trochanteric anastomosis Clinical correlations: Clinical correlation of the superior gluteal nerve: Trendelenburg sign: (II) This test is performed to assess the functions of the gluteus medius and minimus muscles. ). During normal walking, the gluteus medius and minimus contract first on one side, then on the other side (contract alternately). When they contract, they raise the pelvis on the unsupported (opposite) side. This permits the leg to be raised off the ground before taking a forward step. Normally the gluteus medius and minimus contract on the supported side as soon as the contralateral foot leaves the floor, preventing tipping of the pelvis to the unsupported side. When a person who has suffered a lesion of the superior gluteal nerve is asked to stand on one leg, the pelvis on the unsupported side drops (sags), indicating that the gluteus medius and minimus muscles on the supported side are weak or non-functional. The patient exhibits a dipping or lurching gait. This is referred clinically as positive trendelenburg test. It can also result due to fracture of the greater trochanter or dislocation of the hip joint. Piriformis syndrome: Compression of the sciatic nerve by the piriformis muscle. In 50% of the cases, case histories indicate trauma to the buttock associated with hypertrophy & spasm of the piriformis. Skaters, cyclists who excessively use the gluteal muscles, and women are more likely to develop this syndrome. In 12% of individuals common peroneal division of sciatic nerve passes through piriformis and may be compressed. Intragluteal Injections: Gluteal region is a common site for intramuscular injections because the muscles are thick and large. The needle pierces skin, fascia, and the 3 gluteal muscles. Injected substances are absorbed into the intramuscular veins. Injections into the buttock are safe only in the superolateral quadrant of the buttock well away from the sciatic nerve. It can be given superior to a line extending from the PSIS to the superior border of the greater traochanter. Everyone giving injections into this region must be aware of the danger of hitting the sciatic nerve. With respect to sciatic nerve, the lateral side of the buttock is the side of safety and medial side is the side of danger. Sciatica: pain along the sciatic nerveis a relatively common form of low back pain and leg pain. This pain along the sciatic nerve can be caused when a root of the sciatic nerve is pinched or irritated (referred as radiculopathy). Sciatica is usually caused by pressure on the sciatic nerve from a herniated disc (also referred to as a ruptured disc, pinched nerve, slipped disk, etc.). For some people, the pain from sciatica can be severe and debilitating. Tibial component of Sciatic (or can also say the sciatic) supplies all the hamstring muscles, except the short head of the biceps femoris which is the peronial
MUSCLES OF THE POSTERIOR COMPARTMENT OF THE THIGH
Muscle biceps femoris, long head biceps femoris, short head Action flexes and laterally rotates leg when knee is flexed, extends thigh(when starting to walk) Same as above Nerve Supply tibial part of sciatic nerve common peroneal part of sciatic nerve tibial part of sciatic nerve tibial part of sciatic tibial part of sciatic N
semitendinosus flexes and medially rotates leg; extends thigh at the hip semimembranosus flexes and medially rotates leg; extends thigh at the hip adductor magnus (hamstring extends thigh part)
The Sciatic Nerve
Branches: It does not supply any structure in the gluteal region. The articular branches supply the hip-joint The muscular branches From the tibial component: to the hamstring muscles1. Long head of Biceps femoris 2. Semitendinosus 3. Semimembranosus 4. Adductor magnus (ischial part) o From the common peroneal part: Short head of the biceps femoris Sciatic Nerve Clinical correlation: 1. Sciatica: Pressure or irritation of the roots of the sciatic nerve causes shooting pain along the course of the sciatic nerve on the back of the thigh. In sciatica, anaesthetic drug is injected into the nerve midway between the greater trochanter and ischial tuberosity to relieve the pain. 3. The sciatic nerve may be injured in posterior dislocation of the hip joint. If the injury is complete, all the hamstring muscles and the muscles below the knee joint are paralysed. It results in Foot drop. Further, all cutaneous sensations below the knee are lost except the medial side of the lower part of the leg and medial border of the foot as far as the ball of the great toe (area supplied by the saphenous nerve).
POPLITEAL FOSSA
Boundaries Above and laterally: Biceps femoris Above and medially: Semitendinous and Semimembranosus Below and laterally: Lateral head of the Gastrocnemius and Plantaris Below and medially: Medial head of the Gastrocnemius Floor: Popliteal surface of the femur
Oblique popliteal ligament of the knee-joint Upper end of the tibia Fascia covering the Popliteus Popliteus Roof: Skin, superficial fascia, deep fascia (popliteal fascia) Contents A pad of fat Popliteal lymph nodes (2-3) Popliteal artery and its 5 genicular branches Popliteal vein Terminal part of the short saphenous vein Tibial nerve Common peroneal nerve Lower part of the posterior cutaneous nerve of the thigh Articular branch from the obturator nerve The tibial nerve descends through the middle of the fossa, lying under the deep fascia and crossing the vessels posteriorly from the lateral to the medial side. (THIS IS THE MOST ANTERIOR STRUCTURE NVA) The popliteal vein separates the popliteal artery from the tibial nerve through out its course in the popliteal fossa.
Popliteal artery
It ends at the lower border of the Popliteus by dividing into anterior and posterior tibial arteries.
Common Peroneal Nerve
It descends obliquely along the lateral side of the popliteal fossa to the head of the fibula, close to the medial margin of the Biceps femoris muscle. It lies between the tendon of the Biceps femoris and lateral head of the Gastrocnemius muscle, winds around the neck of the fibula, between the Peroneus longus and the bone,. It ends by dividing under cover of the peroneus longus into the superficial and deep peroneal nerves. HIP JOINT Bones taking part: Cup like acetabulum of the hip bone and the round head of the femur Within the acetabulum there is a horse-shoe shaped lunate surface covered with articular cartilage. Lower part of the cup is non-articular and called acetabular fossa (filled with fat). Iliofemoral ligament- It is the strongest ligament in the body. It lies on the anterior surface of the fibrous capsule. It is inverted Y shaped. It is attached above to the anterior inferior iliac spine and below to the intertrochanteric line of femur.
Pubofemoral ligament- It lies anteroinferior to the hip joint. It is attached above to the pubic crest and below blends with the iliofemoral ligament. Ischiofemoral ligament: It lies posteroinferior to the fibrous capsule. It is attached superiorly to the ischium behind the acetabulum and inferiorly it blends with the fibrous capsule. Movements of the hip joint: The movements of the hip joint are: Flexion, extension, abduction, adduction, lateral rotation, medial rotation, and circumduction Note that when the foot is off the ground (eg. walking), the thigh is free to move on the trunk. When the foot is on the ground (from sitting position to the standing position or bending forward to pick up an object) the trunk can be made to move on a fixed thigh. Flexion- Iliopsoas, sartorius, tensor fascia lata, rectus femoris, pectineus Extension- chiefly by the gluteus maximus muscle with help by the hamstrings Abduction- Gluteus medius, gluteus minimus, tensor fascia lata Adduction- by the adductors longus, brevis, magnus and the gracilis, pectineus, obturator externus Medial rotation- by anterior part of the gluteus minimus and medius and tensor fascia lata muscles Lateral rotation- by gluteus maximus, quadratus femoris, piriformis, obturator internus and externus, superior and inferior gemelli. KNOW ABOUT POST. DISLOCATION OF THE HIP JOINT!
KNEE JOINT
Ligaments of the knee joint: 1. Fibrous capsule 2. Ligamentum patellae 3. Tibial collateral ligament (Medial collateral ligament) 4. Fibular collateral ligament (Lateral collateral ligament) 5. Oblique popliteal ligament 6. Anterior cruciate ligament 7. Posterior cruciate ligament 8. Medial meniscus (medial semilunar cartilage) 9. Lateral meniscus (lateral semilunar cartilage) Ligamentum patellae: It is the anterior ligament of the knee joint. It is the distal part of the tendon of the quadriceps femoris muscle. It extends from the apex of the patella to the upper half of the tuberosity of tibia. Medial and lateral patellar retinacula are expansions from the vastus medialis and lateralis on either side of the ligamentum patellae. Cruciate ligaments join the femur and tibia in the center of the knee joint. They are called cruciate because they cross each other like letter X. They are named anterior and posterior by their attachments to the tibia. They are intracapsular (situated within the capsule), but extrasynovial. (like the popliteal tendon). They provide stability to the knee joint. Anterior cruciate ligament (I.D. - Picture): It is attached below to the anterior part of the intercondylar area
between the attachments of the anterior horns of the medial and lateral menisci. It passes superiorly, posteriorly and laterally to be attached to the medial surface of the lateral condyle of the femur. It becomes taut when the knee is fully extended. It prevents posterior displacement of the femur on the tibia. Posterior cruciate ligament (I.D. - Picture): It is the stronger of the two. It is attached to the posterior intercondylar area of the tibia behind the attachments of the lateral and medial menisci. It passes upwards and forwards medial to the anterior cruciate ligament and is attached to the lateral surface of the medial condyle of the femur. It becomes taut during flexion of the knee joint. It prevents anterior displacement of the femur on the tibia. It is the main stabilizing factor for the femur when walking downhill. Medial meniscus (medial semilunar cartilage): is C shaped. Its outer border is thick, convex and attached to the fibrous capsule. Its inner border is thin, concave and free. Its anterior horn (end) is attached to the anterior intercondylar area of the tibia, anterior to the attachment of the ACL. Its posterior horn (end) is attached to the posterior intercondylar area, anterior to the attachment of the PCL. Its outer margin is firmly attached to the tibial collateral ligament. Lateral meniscus (lateral semilunar cartilage): It is nearly circular, smaller and more freely movable than the medial meniscus. Its anterior horn is attached to the anterior intercondylar area, behind the attachment of the ACL. The posterior horn is attached to the intercondylar area behind the intercondylar tubercle, in front of the posterior horn of the medial meniscus. The convex outer border of the lateral meniscus is not attached to the fibular collateral ligament. The tendon of the popliteus muscle separates the lateral meniscus from the fibular collateral ligament. Few fibers of the popliteus muscle take origin from the lateral meniscus. The popliteus muscle pulls the lateral meniscus posteriorly during flexion and hence, prevents it from being crushed. UNHAPPY TRIAD 3 structures that are commonly injured in the knee joint 1) medial collateral ligament 2) medial meniscus 3) ant. Cruciate ligament (ie. Torn ACL) Bursae around the knee: (Clinical Question) There are as many as 12-15 bursae around the knee. Some of them communicate with the joint cavity. Can be independent or an extension of the synovial cavity of the joint. 1. Suprapatellar bursa- deep to the quadriceps tendon- Communicates with the joint cavity. Articularis genu gets attached to this bursa. EXAM QUESTION if get stabbed in lower ant leg, what bursa is likely to get inflamed musct know position of bursa to dtermine this 2. Prepatellar bursa- between patella and skin normally inflamed in maids due to kneeling and moping the floor (Called HOUSMAIDS KNEE/BURSITIS) 3. Subcutaneous (or superficial) infrapatellar bursa- between the skin and tuberosity of tibia (When inflamed called CLERGYMANS KNEE) 4. Deep infrapatellar bursa- between ligamentum patellae and tibia, can communicate with capsul of knee joint ***LOCKING OF THE KNEE OR SCREW HOME MOVEMENT In the last stage of extension of the knee, the thigh (femur) is rotated medially or the leg (tibia) is rotated laterally and the joint is said to be screwed into home and locked.
With the foot on the ground, it is the femur that moves on the stationary tibia. The medial rotation of femur which occurs as part of the final stage of extension of the knee is called Locking. With the foot off the ground, extension is associated with lateral rotation of tibia on stationary femur. ***UNLOCKING OF THE KNEE Flexion of the knee from the fully extended position: This movement is the reverse of the locking movement. While flexing the knee (from the fully extended position), the joint has to be unlocked by a reverse rotation and this is done by the popliteus muscle. Hence, Popliteus is called unlocking muscle (know this !!!!!). When the foot is on the ground, femur is made to rotate laterally by the popliteus.
ANKLE JOINT Talocrural joint
Bones: Proximally 1. Distal articular surface of the tibia and its medial malleolus 2. Lateral malleolus of the fibula 3. Inferior transverse tibiofibular ligament Distally- Trochlea of the talus 2. Medial ligament: (deltoid ligament) Is strong. It is triangular in shape. Its apex is attached to the medial malleolus. It fans out distally and gets attached to the 1) talus, 2) calcaneus and 3) navicular bones. The deltoid ligament stabilizes the ankle joint during eversion and prevents subluxation (partial dislocation) of the joint. 3. Lateral ligament: It is weaker than the medial ligament. It is composed of 3 parts- anterior talofibular ligament, posterior talofibular ligament and the calcaneofibular ligament. Lateral and medial ligament strengthens the sides of the joint Movements: Dorsiflexion and plantar flexion. Dorsiflexion- by the muscles in the anterior compartment of the leg (Tibialis anterior, Extensor hallucis longus, Extensor digitorum longus, Peroneus tertius) Plantarflexion- by the muscles in the posterior compartment of the leg (soleus, gastrocnemius, tibialis posterior, flexor hallucis longus, flexor digitorum longus)
PLANTAR APONEUROSIS
It is the thickened central part of the deep fascia of the sole of the foot. It is triangular in shape. Its functions are1. holds the parts of the foot together 2. protects the plantar surface from injury 3. supports the longitudinal arch of the foot
Posterior end (apex) is attached to the medial tubercle of the calcaneum. Base (anterior end) is divided into 5 slips- one to each toe that split to enclose the digital tendons. From the sides of the plantar aponeurosis, vertical septa extend deeply to form 3 compartments of the sole of the foot- medial, central and lateral compartment. Deep to the plantar aponeurosis are the muscles (arranged in 4 layers), blood vessels and nerves of the sole of the foot. Clinical correlation: Plantar fasciitis - Straining and inflammation of the plantar aponeurosis causing severe pain and tenderness of the sole of the foot. Can occur in runners with inappropriate shoes. Calcaneal spur Repeated attacks of plantar fasciitis produce ossification in the posterior attachment of the plantar aponeurosis. This is called calcaneal spur. The condition is heel spur syndrome.
MUSCLES OF THE SOLE OF THE FOOT
First Layer abductor hallucis flexor digitorum brevis (I.D.) Flexes, abducts big toe (hallux). medial plantar Supports medial N longitudinal arch Flexes lateral four medial plantar toes. Supports N medial and lateral longitudinal arches Flexes, abducts 5th lateral plantar N toe. Supports lateral longitudinal arch
abductor digiti minimi
Second Layer tendons from flexor digitorum longus and flexor hallicus longus are found in this layer Between first and second layer you see the passage of the neuromuscular bundle consisting of the medial and lateral plantar artery and nerves Lateral flexor digitorum margin of aids flexor digitorum longus accessorius the tendon tendon to flex lateral four lateral plantar (quadratus of flexor toes (helps to straighten the nerve plantae) ON digitorum direction of the pull) EXAM longus Lumbricals (4 in Tendons of flexor dorsal extends toes at interphalangeal 1st lumbricalnumber) digitorum longus (1st- digital joints; flex metatarso medial plantar N; single head expansion phalangeal joints (prevents (unipennate), from (extensor buckling of the toes in walking 2nd, 3rd, & 4th-
medial side of the expansion) and running) tendon of Fl.Dig.L. of lateral going to the 2nd toe. Rest four toes of the lumbricals arise (middle each by two heads and (bipennate) from terminal adjacent sides of the phalanx) tendons going to the 2nd, 3rd, 4th, and 5th toes
deep branch of the lateral plantar N
Medial plantar artery
It is the smaller of the 2 terminal branches of the posterior tibial artery. It begins under cover of the flexor retinaculum. It passes forward along the medial side of the foot. It runs between the 1st and 2nd layers of the sole of the foot. It lies medial to the medial plantar nerve. At the base of the first metatarsal bone, it passes along the medial border of the first toe, anastomosing with the first dorsal metatarsal artery. Lateral plantar artery It is the larger of the 2 terminal branches of the posterior tibial artery. It begins deep to the flexor retinaculum. It passes obliquely laterally between the 1st and 2nd layers of the sole of the foot, to the base of the fifth metatarsal bone. It then turns medially to the interval between the bases of the first and second metatarsal bones between the 3rd and the 4th layers, where it unites with the deep plantar branch of the dorsalis pedis artery, thus completing the plantar arch.
Medial plantar nerve
It is the larger of the two terminal divisions of the posterior tibial nerve BRANCHES (1) Muscular - Abductor hallucis Flexor digitorum brevis Flexor hallucis brevis (by a branch from proper digital to the great toe) 1st Lumbrical (by the 1st common digital nerve) (2) Cutaneous - to the skin on the medial half of the sole of the foot. (3) Articular to the tarsal and metatarsal joints (4) Proper digital nerve to the medial side of the great toe called proper cuz it supplies on 1 toe (the big or great toe that is) (5) Three common digital nerves. called common because they supply two toes each
Each common digital nerve splits into two proper digital nerves which supply the skin of the medial 3 toes. The distribution of these digital nerves is similar to those of the median nerve in the hand.
The first common digital nerve supplies the 1st Lumbrical.
Lateral Plantar Nerve
Superficial branchMuscular Flexor digiti minimi brevis 3rd plantar interosseous 4th dorsal interosseous Cutaneous- Skin of the lateral 1 toes. Deep branch supplies: Lateral 3 lumbricals First 2 plantar interossei First 3 dorsal interossei Adductor hallucis Medial longitudinal arch: It is formed by calcaneus, the talus, the navicular, the three cuneiforms, and the 1st, 2nd, & 3rd metatarsals. The head of the talus is the key stone of the medial longitudinal arch. Tibialis anterior and peroneus longus help to maintain this arch. It is strengthened by the tibialis posterior and plantar aponeurosis Lateral longitudinal arch: It is formed by calcaneus, the cuboid, and the 4th and 5th metatarsals. It is much flatter.
Vous aimerez peut-être aussi
- Lower LimbDocument6 pagesLower LimbYusri Arif100% (1)
- Lower Limb Anatomy TablesDocument8 pagesLower Limb Anatomy Tableskep1313Pas encore d'évaluation
- Table of Joints in Lower LimbDocument5 pagesTable of Joints in Lower LimbVijay Pradeep100% (3)
- Anatomy Lower LimbDocument43 pagesAnatomy Lower LimbYasif Abbas100% (2)
- Muscle Origin Insertion Innervation Action: (Branch of The Brachial Plexus)Document58 pagesMuscle Origin Insertion Innervation Action: (Branch of The Brachial Plexus)sdfs sdfdPas encore d'évaluation
- Clinical Notes of Lower LimbDocument5 pagesClinical Notes of Lower Limbbeia21100% (1)
- Popliteal Fossa: Dr.P.Sasikala, Assistant Professor of AnatomyDocument18 pagesPopliteal Fossa: Dr.P.Sasikala, Assistant Professor of AnatomySasikala Mohan100% (1)
- Lower Limb McqsDocument55 pagesLower Limb McqsKeshav NagpalPas encore d'évaluation
- MCQ of UpperDocument17 pagesMCQ of Upperد.مهاجر في أرض اللهPas encore d'évaluation
- Gluteal RegionDocument34 pagesGluteal Regionlion2chPas encore d'évaluation
- Anatomy Ofthe Upper ArmDocument37 pagesAnatomy Ofthe Upper ArmBenjamin JonathanPas encore d'évaluation
- Anatomy Upper Limb Q Bank MCQ 1Document10 pagesAnatomy Upper Limb Q Bank MCQ 1oofjd100% (1)
- Back Anatomy TableDocument7 pagesBack Anatomy TableJeffrey XiePas encore d'évaluation
- 30 SEQs of Lower Limb Anatomy by DR RoomiDocument2 pages30 SEQs of Lower Limb Anatomy by DR RoomiMudassar Roomi50% (2)
- Teach Yourself Upper LimbDocument44 pagesTeach Yourself Upper LimbSambili Tonny100% (2)
- Lower LimbDocument53 pagesLower LimbRupesh M DasPas encore d'évaluation
- Anatomy MCQ - Lower Limb PDFDocument30 pagesAnatomy MCQ - Lower Limb PDFnonPas encore d'évaluation
- Upper and Lower Limb Anatomy QuestionsDocument8 pagesUpper and Lower Limb Anatomy QuestionsAnon AnonPas encore d'évaluation
- Lower Limbs MCQs Section 1 TitleDocument148 pagesLower Limbs MCQs Section 1 TitleCaim ZPas encore d'évaluation
- Upper Extremity Circulation and NervesDocument35 pagesUpper Extremity Circulation and NervesMarie100% (1)
- 07 Upper Limb FinalDocument50 pages07 Upper Limb FinalRavishan De AlwisPas encore d'évaluation
- Mcqs in Upper Limb: DR - Khalid MiladDocument10 pagesMcqs in Upper Limb: DR - Khalid MiladOzgan SüleymanPas encore d'évaluation
- Upper Limb MCQsDocument12 pagesUpper Limb MCQstafi66Pas encore d'évaluation
- Abdomen Test QuestionsDocument20 pagesAbdomen Test QuestionsRuth AlooPas encore d'évaluation
- Upper Limb Solved MCQs (Set-1)Document6 pagesUpper Limb Solved MCQs (Set-1)Fawad KtkPas encore d'évaluation
- Quiz Low Limb 2019-DikonversiDocument9 pagesQuiz Low Limb 2019-DikonversiwillysvdPas encore d'évaluation
- MCQ Lower Limb G4Document14 pagesMCQ Lower Limb G4Sajjad HaiderPas encore d'évaluation
- Lower Limb Nerves and MusclesDocument24 pagesLower Limb Nerves and MusclesLola KhatimPas encore d'évaluation
- Osteology of The Upper Limb LectureDocument40 pagesOsteology of The Upper Limb LectureFavour OnyeaboPas encore d'évaluation
- Lower LimbDocument122 pagesLower LimbHiruzaminPas encore d'évaluation
- Lower Limb MCQ FinalDocument7 pagesLower Limb MCQ FinalTofunmi AdegokePas encore d'évaluation
- (PPT) Anatomy 2.5 Lower Limbs - Blood and Nerve Supply - Dr. Tan PDFDocument110 pages(PPT) Anatomy 2.5 Lower Limbs - Blood and Nerve Supply - Dr. Tan PDFPreeti Joan BuxaniPas encore d'évaluation
- Lowerlimbtestquestions 140901100930 Phpapp02Document33 pagesLowerlimbtestquestions 140901100930 Phpapp02Zohaib ShahjehanPas encore d'évaluation
- Blood Vessels of Upper LimbDocument23 pagesBlood Vessels of Upper Limbkhalid_shinasPas encore d'évaluation
- Circumflex Scapular: Dorsum of Thoracodorsal: Latissmus DorsiDocument4 pagesCircumflex Scapular: Dorsum of Thoracodorsal: Latissmus Dorsispeedy.catPas encore d'évaluation
- Anatomy - Head and Neck Table of NervesDocument11 pagesAnatomy - Head and Neck Table of NervesIke Ononiwu100% (3)
- Joints of The Lower LimbDocument35 pagesJoints of The Lower LimbISLAMIC STATUS ZONEPas encore d'évaluation
- Snell Lower LimbDocument44 pagesSnell Lower LimbBen100% (3)
- Vector - and Rodent-Borne Diseases in Europe and North America 2gfshDocument411 pagesVector - and Rodent-Borne Diseases in Europe and North America 2gfshRhyan ArfanPas encore d'évaluation
- AnatomyDocument11 pagesAnatomyoddone_outPas encore d'évaluation
- Upper Limb-MCQ With AnswersDocument20 pagesUpper Limb-MCQ With AnswersMatt McCannPas encore d'évaluation
- Wrist and Hand ComplexDocument6 pagesWrist and Hand ComplexAlyssa Mae CamposanoPas encore d'évaluation
- Wiki Abdomen Mcqs ExplainedDocument9 pagesWiki Abdomen Mcqs Explainedchemptnk100% (2)
- Conduct of Normal Labor and DeliveryDocument29 pagesConduct of Normal Labor and DeliveryEzekiel ArtetaPas encore d'évaluation
- Upper Limb - Clinical AnatomyDocument19 pagesUpper Limb - Clinical AnatomyewijayapalaPas encore d'évaluation
- Bone TissueDocument66 pagesBone TissueFunikawati Baldiyah100% (1)
- Lumbar Plexus (Grays Anatomy)Document12 pagesLumbar Plexus (Grays Anatomy)Joemar ReveloPas encore d'évaluation
- Sheep FactsDocument50 pagesSheep FactsMoises Calastravo100% (1)
- Blue Boxes Lower LimbDocument4 pagesBlue Boxes Lower LimbZllison Mae Teodoro MangabatPas encore d'évaluation
- Popliteal Fossa: By: Dr. Sana KashifDocument18 pagesPopliteal Fossa: By: Dr. Sana KashifUSAMA AHMEDPas encore d'évaluation
- Study Sheet - Gross Anatomy Lower - ExtremityDocument12 pagesStudy Sheet - Gross Anatomy Lower - ExtremityMuhammad BilalPas encore d'évaluation
- Fractures and Dislocations of the Upper LimbDocument27 pagesFractures and Dislocations of the Upper LimbAlapati Vinod KumarPas encore d'évaluation
- Joints of Lower LimbDocument7 pagesJoints of Lower LimbjsdlzjPas encore d'évaluation
- Upper Limb MCQ AnswersDocument3 pagesUpper Limb MCQ AnswerschiPas encore d'évaluation
- SCALP: (Keith L Moore)Document5 pagesSCALP: (Keith L Moore)rajtanniruPas encore d'évaluation
- Anatomy - Upper LimbDocument72 pagesAnatomy - Upper LimbAiman ArifinPas encore d'évaluation
- Anatomy Questions Hip and ThighDocument11 pagesAnatomy Questions Hip and Thighmohamed mowafeyPas encore d'évaluation
- Anatomy 250Document50 pagesAnatomy 250Abdul MusawerPas encore d'évaluation
- Pelvis and PerineumDocument5 pagesPelvis and PerineumSarah Sy-SantosPas encore d'évaluation
- Lower Limb - Clinical AnatomyDocument18 pagesLower Limb - Clinical Anatomyewijayapala100% (2)
- The Osteology of The Lower LimbDocument4 pagesThe Osteology of The Lower LimbAldi PrawidyaPas encore d'évaluation
- 15 PharynxDocument9 pages15 Pharynxapi-3757921Pas encore d'évaluation
- Upper Limb Bones and MusclesDocument119 pagesUpper Limb Bones and MusclesNuhu Bankwhot100% (1)
- Finding An Apartment Project: Background - Answer These Questions in Complete SentencesDocument4 pagesFinding An Apartment Project: Background - Answer These Questions in Complete Sentencesapi-288310744Pas encore d'évaluation
- Patriarchal Blessing Scripture FormatDocument2 pagesPatriarchal Blessing Scripture FormatBret Richard JohnsonPas encore d'évaluation
- RAISE ORGANIC HOG ReviewerDocument4 pagesRAISE ORGANIC HOG Reviewermarkdaveasaytuno2Pas encore d'évaluation
- Many Different Uses For YL Lavender OilDocument8 pagesMany Different Uses For YL Lavender OilLena WolfePas encore d'évaluation
- GET17Report FinalDocument56 pagesGET17Report Finalmnn164Pas encore d'évaluation
- Pathophysiology of Postpartum Hemorrhage and Third Stage of LaborDocument7 pagesPathophysiology of Postpartum Hemorrhage and Third Stage of Labornouval_iqbalPas encore d'évaluation
- Circulation in Humans ExplainedDocument2 pagesCirculation in Humans ExplainedKliemmah PeltierPas encore d'évaluation
- Thoracic WallDocument12 pagesThoracic WallZainab NaffeePas encore d'évaluation
- Body Fluid Electrolytes Acid Base BalanceDocument2 pagesBody Fluid Electrolytes Acid Base BalanceMarzanul Islam AnikPas encore d'évaluation
- Motor Neurone Disease and HomoeopathyDocument8 pagesMotor Neurone Disease and HomoeopathyDr. Rajneesh Kumar Sharma MD HomPas encore d'évaluation
- Principles of Spine Trauma and Spinal Deformities PDFDocument34 pagesPrinciples of Spine Trauma and Spinal Deformities PDFVirlan Vasile CatalinPas encore d'évaluation
- CH 11Document18 pagesCH 11dazaikun22032003Pas encore d'évaluation
- Jurnal LepraDocument20 pagesJurnal LepraCalvin AffendyPas encore d'évaluation
- The Sclera PDFDocument334 pagesThe Sclera PDFMaría Soledad Romero LópezPas encore d'évaluation
- امتحان تجريبي للصف الحادي عشر -فترة رابعة-ورقة ثانيةDocument5 pagesامتحان تجريبي للصف الحادي عشر -فترة رابعة-ورقة ثانيةshehabedenPas encore d'évaluation
- Grade 9 Sex Ed - Youtube LinksDocument16 pagesGrade 9 Sex Ed - Youtube Linksapi-204719782Pas encore d'évaluation
- Word Frequency - Based On 450 Million Word COCA CorpusDocument89 pagesWord Frequency - Based On 450 Million Word COCA Corpusjoelson100% (2)
- February 17, 2017 Strathmore TimesDocument24 pagesFebruary 17, 2017 Strathmore TimesStrathmore TimesPas encore d'évaluation
- Routine Immunization - Details - For 4th August MetingDocument57 pagesRoutine Immunization - Details - For 4th August Metingjalanayush777Pas encore d'évaluation
- Scoliosis: Review of Diagnosis and Treatment: Janusz Popko, Michał Kwiatkowski, Monika GałczykDocument5 pagesScoliosis: Review of Diagnosis and Treatment: Janusz Popko, Michał Kwiatkowski, Monika Gałczykandi dirhanPas encore d'évaluation
- Serology NewDocument116 pagesSerology NewFarlogyPas encore d'évaluation
- Diverticular Disease 2Document5 pagesDiverticular Disease 2karl abiaadPas encore d'évaluation
- SCIENCE FORM 2 (Chapter 1) NOTESDocument41 pagesSCIENCE FORM 2 (Chapter 1) NOTESRamanath Ram100% (1)
- 5090 - w22 - QP - 12 Biology O-Level PypDocument20 pages5090 - w22 - QP - 12 Biology O-Level Pypmuiz phiPas encore d'évaluation
- Alveolar Osteitis A Comprehensive Review ofDocument10 pagesAlveolar Osteitis A Comprehensive Review ofFakhrul ImamPas encore d'évaluation
- Chiari CaseDocument27 pagesChiari CaseShaurya AgarwalPas encore d'évaluation