Académique Documents
Professionnel Documents
Culture Documents
Chapter 34CongestiveHeartFailure
Transféré par
V_RN0 évaluation0% ont trouvé ce document utile (0 vote)
29 vues49 pageschf
Copyright
© Attribution Non-Commercial (BY-NC)
Formats disponibles
PPT, PDF, TXT ou lisez en ligne sur Scribd
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentchf
Droits d'auteur :
Attribution Non-Commercial (BY-NC)
Formats disponibles
Téléchargez comme PPT, PDF, TXT ou lisez en ligne sur Scribd
0 évaluation0% ont trouvé ce document utile (0 vote)
29 vues49 pagesChapter 34CongestiveHeartFailure
Transféré par
V_RNchf
Droits d'auteur :
Attribution Non-Commercial (BY-NC)
Formats disponibles
Téléchargez comme PPT, PDF, TXT ou lisez en ligne sur Scribd
Vous êtes sur la page 1sur 49
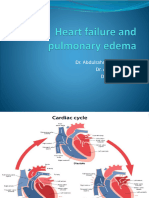
Congestive Heart Failure
(relates to Chapter 34, Nursing Management: Heart Failure and Cardiomyopathy, in the textbook)
Congestive Heart Failure
Definition
An abnormal condition involving impaired cardiac pumping CHF is not a disease but a syndrome Associated with long-standing hypertension and coronary artery disease (CAD)
Congestive Heart Failure
Definition
Heart is unable to pump adequate amount of blood to meet metabolic needs Affects about 5 million people in the United States The most common reason for hospitalization in adults older than 65
Congestive Heart Failure
Etiology and Pathophysiology
Risk factors CAD Age Hypertension Obesity
Congestive Heart Failure
Etiology and Pathophysiology
Risk factors Cigarette smoking Diabetes mellitus High cholesterol African American descent
Congestive Heart Failure
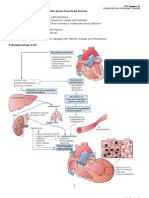
Etiology and Pathophysiology
May be caused by any interference with normal mechanisms regulating cardiac output (CO)
Congestive Heart Failure
Etiology and Pathophysiology
CO depends on: Preload Afterload Myocardial contractility Heart rate Metabolic state
Congestive Heart Failure
Etiology and Pathophysiology
Pathology of ventricular failure Systolic failure Most common cause of CHF Left ventricle (LV) loses ability to generate enough pressure to eject blood forward
Congestive Heart Failure
Etiology and Pathophysiology
Pathology of ventricular failure Systolic failure Hallmark is a in LV ejection fraction
Congestive Heart Failure
Etiology and Pathophysiology
Pathology of ventricular failure Diastolic failure Impaired ability of the ventricles to fill during diastole Usually the result of LV hypertrophy
Congestive Heart Failure
Etiology and Pathophysiology
Pathology of ventricular failure Diastolic failure Pulmonary congestion Normal ejection fraction
Congestive Heart Failure
Etiology and Pathophysiology
Pathology of ventricular failure Mixed systolic and diastolic failure Seen in dilated cardiomyopathy Biventricular failure Patient has extremely poor ejection fractions
Congestive Heart Failure
Etiology and Pathophysiology
Compensatory mechanisms Ventricular dilation Ventricular hypertrophy Increased SNS stimulation Neurohormonal responses
Congestive Heart Failure
Types of Congestive Heart Failure
One-sided failure eventually leads to biventricular failure
Congestive Heart Failure
Types of Congestive Heart Failure
Left-sided failure Most common form Blood backs up through the left atrium into the pulmonary veins Pulmonary congestion and edema
Congestive Heart Failure
Types of Congestive Heart Failure
Left-sided failure Most common cause: HTN Cardiomyopathy Rheumatic heart disease CAD
Left-Sided Heart Failure
Fig. 34-1
Congestive Heart Failure
Types of Congestive Heart Failure
Right-sided failure Backward flow to the right atrium and venous circulation Results from diseased right ventricle
Congestive Heart Failure
Types of Congestive Heart Failure
Right-sided failure Venous congestion Peripheral edema Hepatomegaly Splenomegaly Jugular venous distension
Congestive Heart Failure
Types of Congestive Heart Failure
Right-sided failure Primary cause is left-sided failure Cor pulmonale RV dilation and hypertrophy caused by pulmonary pathology
Acute Congestive Heart Failure
Clinical Manifestations
Pulmonary edema Agitation Pale or cyanotic Cold, clammy skin Severe dyspnea Tachypnea
Pulmonary Edema
Fig. 34-2
Chronic Congestive Heart Failure
Clinical Manifestations
Fatigue Dyspnea Paroxysmal nocturnal dyspnea (PND) Tachycardia Edema Nocturia
Chronic Congestive Heart Failure
Clinical Manifestations
Behavioral changes Restlessness, confusion, attention span Chest pain Weight changes Skin changes Dusky appearance
Congestive Heart Failure
Complications
Pleural effusion Arrhythmias Left ventricular thrombus Hepatomegaly
Congestive Heart Failure
Classification
Based on the persons tolerance to physical activity Class 1: No limitation of physical activity Class 2: Slight limitation
Congestive Heart Failure
Classification
Based on the persons tolerance to physical activity Class 3: Marked limitation Class 4: Inability to carry on any physical activity without discomfort
Congestive Heart Failure
Diagnostic Studies
Primary goal is to determine underlying cause Physical exam Chest x-ray ECG Hemodynamic assessment
Congestive Heart Failure
Diagnostic Studies
Primary goal is to determine underlying cause Echocardiogram Stress testing Cardiac catheterization Ejection fraction (EF)
Acute Congestive Heart Failure
Nursing and Collaborative Management
Primary goal is to improve LV function by: Decreasing intravascular volume Decreasing venous return Decreasing afterload
Acute Congestive Heart Failure
Nursing and Collaborative Management
Primary goal is to improve LV function by: Improving gas exchange and oxygenation Improving cardiac function Reducing anxiety
Acute Congestive Heart Failure
Nursing and Collaborative Management
Decreasing intravascular volume Improves LV function by reducing venous return Loop diuretic: drug of choice
Acute Congestive Heart Failure
Nursing and Collaborative Management
Decreasing venous return (preload) Reduces the amount of volume returned to the LV during diastole High Fowlers position
Acute Congestive Heart Failure
Nursing and Collaborative Management
Decreasing afterload Decreases pulmonary congestion IV nitroprusside (Nipride) nesiritide (Natrecor)
Acute Congestive Heart Failure
Nursing and Collaborative Management
Improving gas exchange and oxygenation Decreases pulmonary congestion IV nitroprusside (Nipride) nesiritide (Natrecor)
Acute Congestive Heart Failure
Nursing and Collaborative Management
Improving cardiac function Digitalis Newer inotropics Dobutamine Hemodynamic monitoring
Acute Congestive Heart Failure
Nursing and Collaborative Management
Reducing anxiety Morphine IV inotropic drugs Vasodilators ACE inhibitors
Chronic Congestive Heart Failure
Collaborative Care
Treat underlying cause Maximize CO Alleviate symptoms
Chronic Congestive Heart Failure
Collaborative Care
Oxygen treatment Rest Biventricular pacing Cardiac transplantation
Chronic Congestive Heart Failure
Drug Therapy
ACE inhibitors Diuretics Inotropic drugs Vasodilators -Adrenergic blockers
Chronic Congestive Heart Failure
Nutritional Therapy
Fluid restrictions not commonly prescribed Sodium restriction 2 g sodium diet Daily weights Same time each day Wearing same type of clothing
Chronic Congestive Heart Failure
Nursing Management Nursing Assessment
Past health history Medications Functional health problems Cold, diaphoretic skin
Chronic Congestive Heart Failure
Nursing Management Nursing Assessment
Tachypnea Tachycardia Crackles Abdominal distension Restlessness
Chronic Congestive Heart Failure
Nursing Management Nursing Diagnoses
Activity intolerance Excess fluid volume Disturbed sleep pattern Impaired gas exchange Anxiety
Chronic Congestive Heart Failure
Nursing Management Planning
Overall goals: Peripheral edema Shortness of breath Exercise tolerance Drug compliance No complications
Chronic Congestive Heart Failure
Nursing Management Nursing Implementation
Acute intervention Establishment of quality of life goals Symptom management Conservation of physical/emotional energy Support systems
Chronic Congestive Heart Failure
Nursing Management Nursing Implementation
Ambulatory and home care Teaching Psychologic changes Exercise-saving behaviors Medications
Chronic Congestive Heart Failure
Nursing Management Nursing Implementation
Evaluation Respiratory status Sleep Fluid balance
Chronic Congestive Heart Failure
Nursing Management Nursing Implementation
Evaluation Activity tolerance Anxiety control Knowledge: disease process
Vous aimerez peut-être aussi
- Reverse and Prevent Heart Disease: Natural Ways to Stop and Prevent Heart Disease, Using Plant-Based Oil-Free Diets (Cure Congestive Heart Failure)D'EverandReverse and Prevent Heart Disease: Natural Ways to Stop and Prevent Heart Disease, Using Plant-Based Oil-Free Diets (Cure Congestive Heart Failure)Pas encore d'évaluation
- Congestive Heart FailureDocument43 pagesCongestive Heart FailuresudersonPas encore d'évaluation
- Systolic Heart FailureDocument66 pagesSystolic Heart FailureFerinaTarizaIIPas encore d'évaluation
- Congestive Heart FailureDocument44 pagesCongestive Heart FailureAmelia LubisPas encore d'évaluation
- Heart Failure 1Document50 pagesHeart Failure 1dhiraj parmar100% (1)
- Heart FailureDocument4 pagesHeart FailureDane WrightPas encore d'évaluation
- Session 24 Heart FailureDocument15 pagesSession 24 Heart Failuredreampurpose97Pas encore d'évaluation
- Heart Failure: Scott Kaba MatafwaliDocument25 pagesHeart Failure: Scott Kaba MatafwaliAngetile KasangaPas encore d'évaluation
- Congestive Cardiac Failure GuideDocument47 pagesCongestive Cardiac Failure GuideRajesh Sharma100% (1)
- CARDIOVASCULAR DISEASES: SIGNS, SYMPTOMS AND TREATMENT OF HEART FAILUREDocument27 pagesCARDIOVASCULAR DISEASES: SIGNS, SYMPTOMS AND TREATMENT OF HEART FAILURESanthoshi Sadhanaa SankarPas encore d'évaluation
- Heart FailureDocument108 pagesHeart FailureDeasy Rizka Rahmawati100% (1)
- Cardiogenic Shock ManagementDocument66 pagesCardiogenic Shock ManagementdrkurniatiPas encore d'évaluation
- Heart Failure PDFDocument25 pagesHeart Failure PDFDewMaL HealthPas encore d'évaluation
- CHF 1Document36 pagesCHF 1Ashwin Raghav SankarPas encore d'évaluation
- Cardio-Vascular Disease: HypertensionDocument74 pagesCardio-Vascular Disease: HypertensionLijoPas encore d'évaluation
- Heartfailurepptsam 170511135108Document48 pagesHeartfailurepptsam 170511135108enam professorPas encore d'évaluation
- CONGESTIVE CARDIAC FAILURE AnjuDocument32 pagesCONGESTIVE CARDIAC FAILURE Anjuanju rachel josePas encore d'évaluation
- Cardiovascular Disorders: BY: Maximin A. Pomperada, RN, MANDocument65 pagesCardiovascular Disorders: BY: Maximin A. Pomperada, RN, MANRellie Castro100% (1)
- Heart Failure: Zelalem T., MD Yr III Resident, PediatricsDocument65 pagesHeart Failure: Zelalem T., MD Yr III Resident, PediatricsChalie MequanentPas encore d'évaluation
- Heart FailureDocument44 pagesHeart FailureSalman Habeeb100% (6)
- Heart Failure: Living With A Hurting HeartDocument44 pagesHeart Failure: Living With A Hurting HeartWyz ClassPas encore d'évaluation
- Left Ventricular FailureDocument17 pagesLeft Ventricular Failurenisha24100% (1)
- Hypertension For EMS ProvidersDocument35 pagesHypertension For EMS ProvidersPaulhotvw67100% (5)
- Heart FailureDocument28 pagesHeart FailureStella CooKeyPas encore d'évaluation
- Kuliah Pakar HF FKUMMDocument46 pagesKuliah Pakar HF FKUMMOkta Dwi Kusuma AyuPas encore d'évaluation
- Hypertension Clinical GuideDocument74 pagesHypertension Clinical GuideNoman MunirPas encore d'évaluation
- DR - Sfeir Principles+of+Cardiac+SurgeryDocument91 pagesDR - Sfeir Principles+of+Cardiac+SurgeryFrida AtallahPas encore d'évaluation
- Congestive Heart FailureDocument43 pagesCongestive Heart Failure568563100% (1)
- DocumentDocument10 pagesDocumentMulhma AlharbiPas encore d'évaluation
- Heart FailureDocument94 pagesHeart FailureAnusha Verghese100% (1)
- Congestive Cardiac Failure by NeetaDocument26 pagesCongestive Cardiac Failure by NeetaNeeta AnandaPas encore d'évaluation
- Heart Failure PAED 604 2023 VileshDocument34 pagesHeart Failure PAED 604 2023 VileshAvneelPas encore d'évaluation
- Heart Failure: DR Edial SanifDocument45 pagesHeart Failure: DR Edial SanifiikPas encore d'évaluation
- Cardiac Heart Failure Guide: Causes, Symptoms & Nursing CareDocument43 pagesCardiac Heart Failure Guide: Causes, Symptoms & Nursing CareCindy DeliaPas encore d'évaluation
- Pharmacotherapy - Heart Failure - Dr. Mohammed KamalDocument62 pagesPharmacotherapy - Heart Failure - Dr. Mohammed KamalMohammed KamalPas encore d'évaluation
- CHFDocument35 pagesCHFMarione GimenezPas encore d'évaluation
- Project Based Learning 2 Year 2021 Title: Heart DiseasesDocument19 pagesProject Based Learning 2 Year 2021 Title: Heart DiseasesADAM BIN MUHIDIN MoePas encore d'évaluation
- Heart Disease Causes, Symptoms & TreatmentDocument42 pagesHeart Disease Causes, Symptoms & TreatmentMuhammad ShahzadPas encore d'évaluation
- Ischemic Heart DiseaseDocument56 pagesIschemic Heart DiseaseSMART PHARMACY By BRIJESHPas encore d'évaluation
- 1 Heart FailureDocument49 pages1 Heart FailureDammaqsaa W BiyyanaaPas encore d'évaluation
- Pharmacotherapy of heart failureDocument79 pagesPharmacotherapy of heart failureAbera JamboPas encore d'évaluation
- Cardiovascular Diseases.Document35 pagesCardiovascular Diseases.Shimmering MoonPas encore d'évaluation
- Heart Failure NewDocument40 pagesHeart Failure NewRoshani sharmaPas encore d'évaluation
- Cardiomyopathy & Lvad: Presenter: Ms Elby JohnDocument43 pagesCardiomyopathy & Lvad: Presenter: Ms Elby JohnajishPas encore d'évaluation
- Right-Sided Heart FailureDocument4 pagesRight-Sided Heart FailureKhalid Mahmud ArifinPas encore d'évaluation
- Shock in Children Lecture NewDocument41 pagesShock in Children Lecture NewDky HartonoPas encore d'évaluation
- Heart Failure and Pulmonary EdemaDocument60 pagesHeart Failure and Pulmonary EdemaYosra —Pas encore d'évaluation
- Cardiomyopathy: Mrs. D. Melba Sahaya Sweety M.SC Nursing GimsarDocument55 pagesCardiomyopathy: Mrs. D. Melba Sahaya Sweety M.SC Nursing GimsarD. Melba S.S ChinnaPas encore d'évaluation
- Myocardial Infarction Case Analysis: Symptoms, Causes, Diagnosis (MIDocument76 pagesMyocardial Infarction Case Analysis: Symptoms, Causes, Diagnosis (MIIpePas encore d'évaluation
- Cardiac FailureDocument19 pagesCardiac FailureBat ManPas encore d'évaluation
- Heart FailureDocument28 pagesHeart FailureaparnaPas encore d'évaluation
- Thursday Nov 3rd - BayehDocument12 pagesThursday Nov 3rd - BayehFatima MaazPas encore d'évaluation
- Chap.30 Complications From Heart Disease WordDocument6 pagesChap.30 Complications From Heart Disease WordcaisakiPas encore d'évaluation
- Heart Failure: Classification, Risk Factors and Clinical FeaturesDocument28 pagesHeart Failure: Classification, Risk Factors and Clinical FeaturesfredyPas encore d'évaluation
- Congestive Cardiac FailureDocument49 pagesCongestive Cardiac FailureHampson MalekanoPas encore d'évaluation
- CARDIOVASCULAR DISORDERS GUIDEDocument112 pagesCARDIOVASCULAR DISORDERS GUIDEAleey ShahPas encore d'évaluation
- NSC 314 Group 3-1Document80 pagesNSC 314 Group 3-1Agboola SeyiPas encore d'évaluation
- Coronary Artery Disease: By. Saiha AlinaDocument19 pagesCoronary Artery Disease: By. Saiha AlinasaihaPas encore d'évaluation
- HTN and CHFDocument29 pagesHTN and CHFkiflomPas encore d'évaluation
- A NCM 103 Lecture 2013Document80 pagesA NCM 103 Lecture 2013V_RNPas encore d'évaluation
- NCM 106Document13 pagesNCM 106V_RNPas encore d'évaluation
- Gluco MetersDocument7 pagesGluco MetersV_RNPas encore d'évaluation
- A SepsisDocument5 pagesA SepsisV_RNPas encore d'évaluation
- Physiology of RespirationDocument10 pagesPhysiology of RespirationV_RNPas encore d'évaluation
- Bed MakingDocument8 pagesBed MakingV_RN100% (1)
- CatheterizationDocument14 pagesCatheterizationV_RNPas encore d'évaluation
- Safety&SecurityDocument22 pagesSafety&SecurityV_RNPas encore d'évaluation
- Nursing as an Art - Care, Culture and Self-AwarenessDocument1 pageNursing as an Art - Care, Culture and Self-AwarenessV_RNPas encore d'évaluation
- Neurologic Disorders - NCM 102 LecturesDocument12 pagesNeurologic Disorders - NCM 102 LecturesBernard100% (4)
- Lancing DeviceDocument12 pagesLancing DeviceV_RNPas encore d'évaluation
- ShockDocument84 pagesShockV_RNPas encore d'évaluation
- HaemodialysisDocument98 pagesHaemodialysisKo Zin100% (1)
- 6th Central Pay Commission Salary CalculatorDocument15 pages6th Central Pay Commission Salary Calculatorrakhonde100% (436)
- 6th Central Pay Commission Salary CalculatorDocument15 pages6th Central Pay Commission Salary Calculatorrakhonde100% (436)
- Cardiovascular AssessmentDocument69 pagesCardiovascular AssessmentV_RNPas encore d'évaluation
- 2571central Venous PressureDocument39 pages2571central Venous PressureV_RN100% (1)
- Chapter 35arrhythmiasDocument116 pagesChapter 35arrhythmiasV_RNPas encore d'évaluation
- Hand WashingDocument3 pagesHand WashingV_RNPas encore d'évaluation
- Incorporating Florence Nightingale PDFDocument7 pagesIncorporating Florence Nightingale PDFV_RNPas encore d'évaluation
- Nursing Informatics Lecture2010Document354 pagesNursing Informatics Lecture2010V_RN100% (5)
- Assessing Neurologic Function and Gerontologic ConsiderationsDocument23 pagesAssessing Neurologic Function and Gerontologic ConsiderationsV_RNPas encore d'évaluation
- Homeostasis, Stress and Adaptation - Ppt2aDocument154 pagesHomeostasis, Stress and Adaptation - Ppt2aV_RN100% (2)
- Assessment of Respiratiory FunctionDocument12 pagesAssessment of Respiratiory FunctionV_RNPas encore d'évaluation
- Assessment of Respiratiory FunctionDocument12 pagesAssessment of Respiratiory FunctionV_RNPas encore d'évaluation
- Copd 2011Document82 pagesCopd 2011V_RNPas encore d'évaluation
- Activity and ExerciseDocument67 pagesActivity and Exercisenursereview100% (3)
- Incorporating Florence Nightingale PDFDocument7 pagesIncorporating Florence Nightingale PDFV_RNPas encore d'évaluation
- DirectingDocument67 pagesDirectingV_RNPas encore d'évaluation
- Hopkins Status ReportDocument56 pagesHopkins Status ReportJeffrey GillespiePas encore d'évaluation
- Anesthesia For The Older PatientsDocument40 pagesAnesthesia For The Older PatientsRAHUL SUTHARPas encore d'évaluation
- A Manual Veterinary Therapeutics and Pharmacology 1000843791 PDFDocument597 pagesA Manual Veterinary Therapeutics and Pharmacology 1000843791 PDFNasir KhanPas encore d'évaluation
- Physical Changes with Aging: A Guide to Normal SenescenceDocument53 pagesPhysical Changes with Aging: A Guide to Normal SenescenceRohit SejwalPas encore d'évaluation
- Principle of Animal Physiology (Christopher D. Moyes, Patricia Schulte) Principle ofDocument763 pagesPrinciple of Animal Physiology (Christopher D. Moyes, Patricia Schulte) Principle ofKing Amv86% (7)
- AMC BLS Training TeamDocument6 pagesAMC BLS Training TeamRajasekhar BandiPas encore d'évaluation
- P5 Science SA2 2019 ACS Exam PapersDocument42 pagesP5 Science SA2 2019 ACS Exam PapersAsvinnaah kumarPas encore d'évaluation
- 54 MCQs on Cardiac PhysiologyDocument22 pages54 MCQs on Cardiac PhysiologyShahabuddin Shaikh0% (1)
- 7th Grade Natural Science Reinforcement WorksheetDocument3 pages7th Grade Natural Science Reinforcement WorksheetnataliaPas encore d'évaluation
- Complete Physical, Mental and Social Well-BeingDocument44 pagesComplete Physical, Mental and Social Well-BeingBasil Francis Alajid77% (13)
- 1 Fetal CirculationDocument21 pages1 Fetal Circulationdr_mohanad100% (1)
- Tortora 13e Glossary 2012Document30 pagesTortora 13e Glossary 2012Shweta KhannaPas encore d'évaluation
- Body Fluids and CirculationDocument5 pagesBody Fluids and CirculationSheehan MathurPas encore d'évaluation
- Surgery ReviewDocument12 pagesSurgery ReviewJo AnnePas encore d'évaluation
- Obstructive Sleep Apnea - Pulmo LectureDocument16 pagesObstructive Sleep Apnea - Pulmo LecturemandrakesMD0% (1)
- Mrs. Maria Eloisa Lim Chu Gungon: When You Reach Age 75 When You Reach Age 75 If The Insured Passes Away at Age 75Document11 pagesMrs. Maria Eloisa Lim Chu Gungon: When You Reach Age 75 When You Reach Age 75 If The Insured Passes Away at Age 75John Philip TiongcoPas encore d'évaluation
- Explore the Human Body with Fun Lesson PlansDocument13 pagesExplore the Human Body with Fun Lesson Planschongty19841613Pas encore d'évaluation
- ECG Lecture: Waveforms, Leads and ApplicationsDocument21 pagesECG Lecture: Waveforms, Leads and ApplicationsSalah Salah 201-901-341Pas encore d'évaluation
- Walking For A Healthy Heart: How To Prevent Heart Failure? What Is Heart Failure?Document1 pageWalking For A Healthy Heart: How To Prevent Heart Failure? What Is Heart Failure?Karla SombilloPas encore d'évaluation
- Ecocardiografia 5 Cortes YagelDocument3 pagesEcocardiografia 5 Cortes YagelMaria Alejandra Guzmán Quijada100% (1)
- CMS 251 Unit 1 Cardiovascular SystemDocument114 pagesCMS 251 Unit 1 Cardiovascular SystemAmon RicoPas encore d'évaluation
- DORVDocument5 pagesDORVkelly christyPas encore d'évaluation
- Dilated CardiomyopathyDocument6 pagesDilated CardiomyopathyMuthuswamyPas encore d'évaluation
- Kuliah 16 Cor PulmonaleDocument41 pagesKuliah 16 Cor PulmonalecaturwiraPas encore d'évaluation
- KUHS B.SC Nursing 1st Year Physiology Important Question BankDocument10 pagesKUHS B.SC Nursing 1st Year Physiology Important Question BankShabir Khan100% (1)
- Delivered.: ConfidenceDocument7 pagesDelivered.: ConfidenceMed AkrimPas encore d'évaluation
- Heart Block TypesDocument4 pagesHeart Block TypesKurl JamoraPas encore d'évaluation
- 038 Health In1 PDFDocument281 pages038 Health In1 PDFbhatchinmay7100% (1)
- Edan Im8 Specs SheetDocument15 pagesEdan Im8 Specs SheetGoutham RevuruPas encore d'évaluation