Académique Documents
Professionnel Documents
Culture Documents
Blood Group & Coagulation
Transféré par
KalpeshPatil0 évaluation0% ont trouvé ce document utile (0 vote)
229 vues24 pagesblood groups explained
Copyright
© © All Rights Reserved
Formats disponibles
PPT, PDF, TXT ou lisez en ligne sur Scribd
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentblood groups explained
Droits d'auteur :
© All Rights Reserved
Formats disponibles
Téléchargez comme PPT, PDF, TXT ou lisez en ligne sur Scribd
0 évaluation0% ont trouvé ce document utile (0 vote)
229 vues24 pagesBlood Group & Coagulation
Transféré par
KalpeshPatilblood groups explained
Droits d'auteur :
© All Rights Reserved
Formats disponibles
Téléchargez comme PPT, PDF, TXT ou lisez en ligne sur Scribd
Vous êtes sur la page 1sur 24
ANEMIA
o Iron-Deficiency Anemia (most common)
o Aplastic Anemia - bone marrow does not
produce enough RBC
o Hemorrhagic anemia - due to extreme blood
loss
o Pernicious anemia - B12 deficiency
o Sickle Cell Anemia (genetic)
Sickle Cell Anemia
Genetic disease
Red blood cells become
sickle shape
Cant carry as much
oxygen
RED BLOOD CELL MORPHOLOGY
Sickle cell anemia. Note the sickle shaped
red blood cell.
Thalasemia
Normal hemoglobin is composed of two
chains each of and globin. Thalassemia
patients produce a deficiency of either or
globin, unlike sickle-cell disease which
produces a specific mutant form of globin.
LEUKEMIA
o Type of cancer
o Overproduction of immature white blood
cells
o They take the place of RBCs
o Treatable with bone marrow transplants,
chemothemotherapy, radiation
BLOOD POISONING
SEPTICEMIA
An infection enters the
blood stream, can be
deadly
Treated with antibiotics
THROMBOCYTOPENIA
Low production of
Platelets, Causing
bleeding or bruising
Haemophilia
In general symptoms are internal or external
bleeding episodes, which are called "bleeds
Deficiency in coagulation factor VIII is the
most common cause of haemophilia.
Haemophilia A
Haemophilia B : Deficiency in coagulation
factor IX
Haemophilia C : Deficiency in coagulation
factor XI
Transfusion Reactions
People with Type A blood make
antibodies to Type B RBCs, but
not to Type A
Type B blood has antibodies to
Type A RBCs but not to Type B
Type AB blood doesnt have
antibodies to A or B
Type O has antibodies to both
Type A & B
If different blood types are
mixed, antibodies will cause
mixture to agglutinate
Fig 13.5
13-16
When RBCs carrying one or both antigens are exposed to the
corresponding antibodies, they agglutinate; that is, clump together.
People usually have antibodies against those red cell antigens that
they lack.
Human RBC before (left) and after (right) adding serum
containing anti-A antibodies. The agglutination reaction
reveals the presence of the A antigen on the surface of the
cells.
http://users.rcn.com/jkimball.ma.ultran
et/BiologyPages/B/BloodGroups.html
Illustration of the forward and reverse
grouping reaction patterns of the ABO
groups using a blood group tile
http://www.bh.rmit.edu.au/mls/subjects/abo/resources/genetics1.htm
Transfusion Reactions continued
If blood types don't match,
recipients antibodies
agglutinate donors RBCs
Type O is universal donor
because lacks A & B antigens
Recipients antibodies
wont agglutinate donors
Type O RBCs
Type AB is universal
recipient because doesnt
make anti-A or anti-B
antibodies
Wont agglutinate donors
RBCs
Insert fig. 13.6
13-17
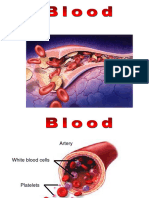
3. Platelets (Thrombocytes)
* Cell fragments bound to megakaryocytes
* Bud Off and are released into the blood
Platelets (thrombocytes)
Are smallest of formed
elements, lack nucleus
Are fragments of
megakaryocytes; amoeboid
Constitute most of mass of
blood clots
Release serotonin to
vasoconstrict & reduce blood
flow to clot area
Secrete growth factors to
maintain integrity of blood
vessel wall
Survive 5-9 days
Function of Platelets
Stop bleeding from a damaged vessel
* Hemostasis
Three Steps involved in Hemostasis
1. Vascular Spasm
2. Formation of a platelet plug
3. Blood coagulation (clotting)
Steps in Hemostasis
Immediate constriction of blood vessel
Vessel walls pressed together become
sticky/adherent to each other
Minimize blood loss
*DAMAGE TO BLOOD VESSEL LEADS TO:
1. Vascular Spasm:
Steps in Hemostasis
a. PLATELETS attach to exposed collagen
b. Aggregation of platelets causes release of
chemical mediators (ADP, Thromboxane A
2
)
c. ADP attracts more platelets
d. Thromboxane A
2
(powerful vasoconstrictor)
* promotes aggregation & more ADP
2. Platelet Plug formation: (figure 11-10)
Leads to formation of platelet plug !
Figure 11-10
(+) Feedback promotes formation of platelet Plug !
Final Step in Hemostasis
a. Transformation of blood from liquid to solid
b. Clot reinforces the plug
c. Multiple cascade steps in clot formation
d. Fibrinogen (plasma protein) Fibrin
Thrombin
3. Blood Coagulation (clot formation):
Clotting Cascade
Figure 11-11
Thrombin in Hemostasis
Factor X
Clotting Cascade
Participation of 12 different clotting factors
(plasma glycoproteins)
Factors are designated by a roman numeral
Cascade of proteolytic reactions
Intrinsic pathway / Extrinsic pathway
Common Pathway leading to the formation
of a fibrin clot !
inactive
active
Hageman factor (XII)
CLOT !
X
Clotting Cascade
Intrinsic Pathway:
Stops bleeding within (internal) a cut vessel
Foreign Substance (ie: in contact with test
tube)
Factor XII (Hageman Factor)
Extrinsic pathway:
Clots blood that has escaped into tissues
Requires tissue factors external to blood
Factor III (Tissue Thromboplastin)
Vous aimerez peut-être aussi
- Circulatory SystemDocument49 pagesCirculatory SystemBrent ValdespinaPas encore d'évaluation
- Decipher Your Labwork - CBC: Functional MedicineD'EverandDecipher Your Labwork - CBC: Functional MedicineÉvaluation : 1 sur 5 étoiles1/5 (1)
- L15 - Blood - CMDocument32 pagesL15 - Blood - CMAleandra LettPas encore d'évaluation
- UNIT 1 Blood Part 2 of 2: (7th Edition)Document10 pagesUNIT 1 Blood Part 2 of 2: (7th Edition)Yasir SidiqPas encore d'évaluation
- Blood Typing: A, B, AB and O Blood TypesDocument15 pagesBlood Typing: A, B, AB and O Blood TypesWidjaya HS TeacherPas encore d'évaluation
- Lab 4Document47 pagesLab 4202310446Pas encore d'évaluation
- Lecture On Blood Groups, Transfusion, RH Incompatibility by Dr. RoomiDocument41 pagesLecture On Blood Groups, Transfusion, RH Incompatibility by Dr. RoomiMudassar Roomi100% (1)
- BloodDocument7 pagesBloodphoebe.gillePas encore d'évaluation
- BMS 201 (Lab) : Blood Grouping and Transfusion: Noha Nooh Lasheen Associate Professor of PhysiologyDocument25 pagesBMS 201 (Lab) : Blood Grouping and Transfusion: Noha Nooh Lasheen Associate Professor of PhysiologyRowaa SamehPas encore d'évaluation
- Blood Lectures 2 2017Document41 pagesBlood Lectures 2 2017Philip Abayomi VincentPas encore d'évaluation
- Blood Lectures 2014 PIO 205Document84 pagesBlood Lectures 2014 PIO 205Philip Abayomi VincentPas encore d'évaluation
- Lec - 5-BloodDocument35 pagesLec - 5-BloodEntesarPas encore d'évaluation
- Blood TypingDocument44 pagesBlood Typingjguevara-mendozaPas encore d'évaluation
- Differential Percentage Count On Your Blood Smear, The Absolute Differential Counts Can Be DeterminedDocument19 pagesDifferential Percentage Count On Your Blood Smear, The Absolute Differential Counts Can Be DeterminedrayeviePas encore d'évaluation
- Blood Group and Transfusion ReactionDocument15 pagesBlood Group and Transfusion ReactionAhmad KhanPas encore d'évaluation
- Blood and LymphaticDocument4 pagesBlood and LymphaticCKPas encore d'évaluation
- Blood Groups: Dr. Kenan GumustekinDocument43 pagesBlood Groups: Dr. Kenan Gumustekinsyed nomanshahPas encore d'évaluation
- BloodDocument80 pagesBloodHem Chandra ShahPas encore d'évaluation
- Abo Group.Document33 pagesAbo Group.R.KABILANPas encore d'évaluation
- BloodDocument6 pagesBloodslmylwkaaPas encore d'évaluation
- Ch11 CardiovascularSystemDocument152 pagesCh11 CardiovascularSystemJaneen FarolaPas encore d'évaluation
- The CARDIOVASCULAR SYSTEM Part 1.kjspDocument11 pagesThe CARDIOVASCULAR SYSTEM Part 1.kjspKleindyn Joy PeraltaPas encore d'évaluation
- Blood TransfusionDocument1 pageBlood Transfusion6qhx62pr42Pas encore d'évaluation
- Maintenance of The Body: Chapter 1: BloodDocument45 pagesMaintenance of The Body: Chapter 1: Blooddania mauriyanaPas encore d'évaluation
- Chapter 1 - Blood RP PDFDocument55 pagesChapter 1 - Blood RP PDFpizzaPas encore d'évaluation
- RBC DisordersDocument49 pagesRBC DisordersGeraldine AgpesPas encore d'évaluation
- Unit 2-Blood Guided NotesDocument5 pagesUnit 2-Blood Guided NotesJeanette IrambonaPas encore d'évaluation
- 1 Transfusion1 PDFDocument7 pages1 Transfusion1 PDFVatha NaPas encore d'évaluation
- Blood Groups: 1 PhysiologyDocument36 pagesBlood Groups: 1 PhysiologyAkash JaatPas encore d'évaluation
- Human Physiology From Cells To Systems 8th Edition Lauralee Sherwood Solutions ManualDocument9 pagesHuman Physiology From Cells To Systems 8th Edition Lauralee Sherwood Solutions Manuallagantrongcnswd100% (30)
- Blood: Joanna Gwen F. FabreroDocument28 pagesBlood: Joanna Gwen F. FabreroAlan PeterPas encore d'évaluation
- 6 - HemoglobinopathiesDocument55 pages6 - HemoglobinopathiesSara BakerPas encore d'évaluation
- Basic Hematologic TestsDocument9 pagesBasic Hematologic TestsdtimtimanPas encore d'évaluation
- Blood & Immunity WorksheetDocument7 pagesBlood & Immunity WorksheetBrenna CrowePas encore d'évaluation
- RBC DISORDERS StudentsDocument84 pagesRBC DISORDERS Studentskimberly abianPas encore d'évaluation
- Blood TransfusionDocument30 pagesBlood TransfusionshantikimbaPas encore d'évaluation
- Blood Group SerologyDocument89 pagesBlood Group SerologynelsonlaizerPas encore d'évaluation
- A and P II Blood 3Document26 pagesA and P II Blood 3ashPas encore d'évaluation
- Anatomy Final Exam Notes PDFDocument45 pagesAnatomy Final Exam Notes PDFLydia LalalandPas encore d'évaluation
- المحاضرة 4Document5 pagesالمحاضرة 4Shi no MePas encore d'évaluation
- Blood Anatomy and PhysiologyDocument28 pagesBlood Anatomy and PhysiologyPORTRAIT OF A NURSEPas encore d'évaluation
- 9 Anatomy 2021 BloodDocument32 pages9 Anatomy 2021 BloodDanica DaniotPas encore d'évaluation
- Blood GroopsDocument32 pagesBlood GroopsAbbas AliPas encore d'évaluation
- The Circulatory System: Components of Blood and Lymph (Detail Study)Document11 pagesThe Circulatory System: Components of Blood and Lymph (Detail Study)Parardha DharPas encore d'évaluation
- Human BloodDocument40 pagesHuman Bloodjetes67387Pas encore d'évaluation
- CVS - BloodDocument30 pagesCVS - BloodQuimson KennethPas encore d'évaluation
- Bio310 Summary 1-5Document22 pagesBio310 Summary 1-5Syafiqah ArdillaPas encore d'évaluation
- Blood Types A B O Ab: Reynaldo Cus 2CDocument6 pagesBlood Types A B O Ab: Reynaldo Cus 2CVirgilio CusPas encore d'évaluation
- ABO Compatibilities For Transfusion Therapy: Donor RecipientDocument6 pagesABO Compatibilities For Transfusion Therapy: Donor RecipientDexie James Ventenilla DizonPas encore d'évaluation
- Blood Composition and Functions: Indian Institute of Technology PatnaDocument41 pagesBlood Composition and Functions: Indian Institute of Technology PatnaHritik KumarPas encore d'évaluation
- Blood - A Fluid Tissue That Circulates Throughout The Body, Via The Arteries and Veins, Providing A VehicleDocument7 pagesBlood - A Fluid Tissue That Circulates Throughout The Body, Via The Arteries and Veins, Providing A VehicleArnie Jude CaridoPas encore d'évaluation
- Blood Transfusion FinalDocument107 pagesBlood Transfusion Finalsanthiyasandy100% (11)
- Anaphy Midterm Notes (The Blood Summary)Document4 pagesAnaphy Midterm Notes (The Blood Summary)Zosia Sage100% (1)
- 09 ThalassemiaDocument43 pages09 Thalassemiaمحمد علي حريج / مسائيPas encore d'évaluation
- Hematology Tests - G I SVDocument49 pagesHematology Tests - G I SVSV. Trần Hữu ThắngPas encore d'évaluation
- Blood GroupDocument13 pagesBlood GroupShanJishmaPas encore d'évaluation
- BloodDocument17 pagesBloodtallaeryllePas encore d'évaluation
- Blood Physiology-Lecture 4Document54 pagesBlood Physiology-Lecture 4alfaristurkiPas encore d'évaluation
- CHAPTER 1.1 Blood PDFDocument25 pagesCHAPTER 1.1 Blood PDFMuhammad Irfan AmiruddinPas encore d'évaluation
- What Makes Methanol (PKa 15.54) A Stronger Acid Than Water (PKa 15Document4 pagesWhat Makes Methanol (PKa 15.54) A Stronger Acid Than Water (PKa 15KalpeshPatilPas encore d'évaluation
- Short Communications: Limiiits, (V, M, AxDocument2 pagesShort Communications: Limiiits, (V, M, AxKalpeshPatilPas encore d'évaluation
- Nadi Diagnosis TechniquesDocument7 pagesNadi Diagnosis TechniquesKalpeshPatilPas encore d'évaluation
- Mental Stress Evaluation Using Heart Rate Variability AnalysisDocument7 pagesMental Stress Evaluation Using Heart Rate Variability AnalysisKalpeshPatilPas encore d'évaluation
- Led Control by Matlab and Massage Display On LCD Serial Communication and Pic 16f877aDocument13 pagesLed Control by Matlab and Massage Display On LCD Serial Communication and Pic 16f877aKalpeshPatilPas encore d'évaluation
- Desire of Ages Chapter-33Document3 pagesDesire of Ages Chapter-33Iekzkad Realvilla100% (1)
- Jordana Wagner Leadership Inventory Outcome 2Document22 pagesJordana Wagner Leadership Inventory Outcome 2api-664984112Pas encore d'évaluation
- Capgras SyndromeDocument4 pagesCapgras Syndromeapi-459379591Pas encore d'évaluation
- Survey Results Central Zone First LinkDocument807 pagesSurvey Results Central Zone First LinkCrystal Nicca ArellanoPas encore d'évaluation
- Introduction To Political ScienceDocument18 pagesIntroduction To Political Sciencecyrene cayananPas encore d'évaluation
- Esse 3600Document15 pagesEsse 3600api-324911878100% (1)
- ScientistsDocument65 pagesScientistsmohamed.zakaPas encore d'évaluation
- Sayyid Jamal Al-Din Muhammad B. Safdar Al-Afghani (1838-1897)Document8 pagesSayyid Jamal Al-Din Muhammad B. Safdar Al-Afghani (1838-1897)Itslee NxPas encore d'évaluation
- Tugas 3Document20 pagesTugas 3dellaayuPas encore d'évaluation
- Social Awareness CompetencyDocument30 pagesSocial Awareness CompetencyudaykumarPas encore d'évaluation
- Statistical MethodsDocument4 pagesStatistical MethodsYra Louisse Taroma100% (1)
- Physics - TRIAL S1, STPM 2022 - CoverDocument1 pagePhysics - TRIAL S1, STPM 2022 - CoverbenPas encore d'évaluation
- LittorinidaeDocument358 pagesLittorinidaeSyarif Prasetyo AdyutaPas encore d'évaluation
- Sophia Vyzoviti - Super SurfacesDocument73 pagesSophia Vyzoviti - Super SurfacesOptickall Rmx100% (1)
- Seismic Response of Elevated Liquid Storage Steel Tanks Isolated by VCFPS at Top of Tower Under Near-Fault Ground MotionsDocument6 pagesSeismic Response of Elevated Liquid Storage Steel Tanks Isolated by VCFPS at Top of Tower Under Near-Fault Ground MotionsciscoPas encore d'évaluation
- E 05-03-2022 Power Interruption Schedule FullDocument22 pagesE 05-03-2022 Power Interruption Schedule FullAda Derana100% (2)
- Data Science Online Workshop Data Science vs. Data AnalyticsDocument1 pageData Science Online Workshop Data Science vs. Data AnalyticsGaurav VarshneyPas encore d'évaluation
- Lets Install Cisco ISEDocument8 pagesLets Install Cisco ISESimon GarciaPas encore d'évaluation
- Public Service Media in The Networked Society Ripe 2017 PDFDocument270 pagesPublic Service Media in The Networked Society Ripe 2017 PDFTriszt Tviszt KapitányPas encore d'évaluation
- Concrete Design Using PROKONDocument114 pagesConcrete Design Using PROKONHesham Mohamed100% (2)
- 7cc003 Assignment DetailsDocument3 pages7cc003 Assignment Detailsgeek 6489Pas encore d'évaluation
- Faith-Based Organisational Development (OD) With Churches in MalawiDocument10 pagesFaith-Based Organisational Development (OD) With Churches in MalawiTransbugoyPas encore d'évaluation
- Capstone Report FormatDocument11 pagesCapstone Report FormatAnkush PalPas encore d'évaluation
- Cum in Mouth ScriptsDocument10 pagesCum in Mouth Scriptsdeudaerlvincent72Pas encore d'évaluation
- Far Eastern University-Institute of Nursing In-House NursingDocument25 pagesFar Eastern University-Institute of Nursing In-House Nursingjonasdelacruz1111Pas encore d'évaluation
- Ad1 MCQDocument11 pagesAd1 MCQYashwanth Srinivasa100% (1)
- Rubrics For Field Trip 1 Reflective DiaryDocument2 pagesRubrics For Field Trip 1 Reflective DiarycrystalPas encore d'évaluation
- Summar Training Report HRTC TRAINING REPORTDocument43 pagesSummar Training Report HRTC TRAINING REPORTPankaj ChauhanPas encore d'évaluation
- Quadrotor UAV For Wind Profile Characterization: Moyano Cano, JavierDocument85 pagesQuadrotor UAV For Wind Profile Characterization: Moyano Cano, JavierJuan SebastianPas encore d'évaluation
- Toward A Design Theory of Problem SolvingDocument24 pagesToward A Design Theory of Problem SolvingThiago GonzagaPas encore d'évaluation